In this issue of American Family Physician, the series of One-Pagers1–3 from the Robert Graham Center offer evidence that a primary care workforce crisis may once again be taking shape. The 1990s saw alignment of public policy and funding efforts to increase the primary care workforce, and indeed family medicine training capacity grew by 34 percent.4 U.S. medical students responded, and the primary care physician workforce increased, but the growth of the subspecialist workforce still outstripped that of primary care physicians. Since 1997, U.S. medical school graduate matches in family medicine and general internal medicine programs have fallen by nearly 50 percent. Despite the disproportionate growth of subspecialties, U.S. primary care physicians still provide most of the care to most patients for most conditions most of the time.
Recent efforts to frame physician workforce policies focus on demand-based models (as opposed to need-based models) and suggest that as Americans' affluence rises, there will be a hue and cry for more subspecialty services. These proposals also suggest that primary care functions will be in less demand and that providers other than physicians will assume these functions.4–6 It is important to recognize that what the market will bear may not be what the population can bear when it comes to health care. The U.S. health system's failure to adopt a primary care focus results in poorer health outcomes for all Americans compared with our nation's industrialized peers, and at a much greater cost. Starfield and colleagues have compared the United States with other developed countries and found that the United States ranked lowest in its primary care functions and lowest in health care outcomes, but highest in health care spending (Figures 1 and 2).7–10
FIGURE 1.
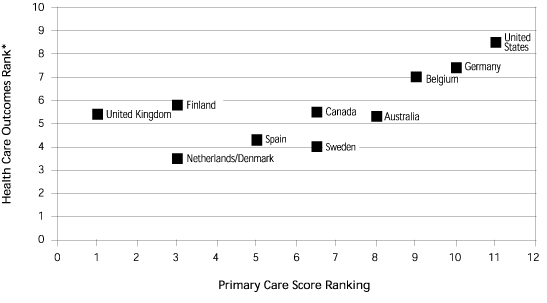
Primary care versus outcome indicators (rank 1 is best, rank 12 is worst).
*--Rank is based on patient satisfaction, expenditures per person, 14 health indicators, and medications per person.
FIGURE 2.
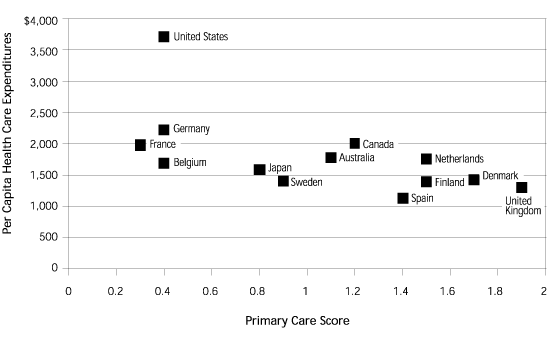
Health care expenditures versus primary care score.
More than two decades of accumulated evidence reveals that having a primary care–based health system matters. People and countries with adequate access to primary care realize a number of health and economic benefits, including the following:
Evidence of Effectiveness
Evidence of Efficiency
Evidence of Equity
The United States leads the world in many ways: militarily, economically, and in health care spending. Health care spending of $1.7 trillion per year should be sufficient to place the United States in the lead in health and health care outcomes. However, we find ourselves behind nearly all of our nation's industrialized peers with regard to health outcomes. We face another primary care workforce crisis that is compounded by increased diversion of medical school graduates into subspecialties. We appear to lack the political will to reorient our system to primary care and to provide coverage and access to health care for all Americans.
The policy options for reorienting our health care system to primary care have been on the table for more than a decade24 and include the following:
- Reimbursement that facilitates and rewards continuous, patient-centered, comprehensive, compassionate, and coordinated care; reimbursement that reflects the special challenges of primary care, fostering patient-focused continuity and maximizing quality and safety; and reimbursement that promotes team practice and offers patients the expertise and training of each member rather than having them compete to fill the same roles
- Developing and supporting information systems and decision-support tools that help primary care physicians and their patients improve the quality of primary health care and to know when it is time to involve subspecialists
- Using state licensing laws, population health needs assessments, and funding to shape an appropriate workforce
- Explicit subsidies for training programs that produce primary care physicians
- Expansion of loan forgiveness for primary care physicians
- Adequate support for practice-based research and primary care health services research
- Measuring and rewarding effective care, especially preventive care services
- Supporting better connections between primary health care, public health, mental health, and subspecialty services
Failure to find the will to change is a path to increasingly poor outcomes, escalating costs, and the dismantling of primary care infrastructures that will take decades to rebuild. There appears to be some resurgence of optimism, or at least urgency, for offering health care coverage for everyone in the United States.25,26 If this latest effort develops momentum among the public and policy makers, it may offer an opportunity to develop a health care system that is more appropriately oriented to primary care, and that supports the needed workforce to deliver its promise. Family physicians must become engaged in working through their own organizations, collaborating with other professional primary care organizations, and working with consumer groups to educate the public and policy makers about the need for immediate action.

