
Am Fam Physician. 2003;68(12):2413-2418
Fractures of the toe are one of the most common lower extremity fractures diagnosed by family physicians. Toe fractures most frequently are caused by a crushing injury or axial force such as stubbing a toe. Joint hyperextension and stress fractures are less common. Most patients have point tenderness at the fracture site or pain with gentle axial loading of the digit. Anteroposterior and oblique radiographs generally are most useful for identifying fractures, determining displacement, and evaluating adjacent phalanges and digits. Referral is indicated in patients with circulatory compromise, open fractures, significant soft tissue injury, fracture-dislocations, displaced intra-articular fractures, or fractures of the first toe that are unstable or involve more than 25 percent of the joint surface. Most children with fractures of the physis should be referred, but children with selected nondisplaced Salter-Harris types I and II fractures may be treated by family physicians. Stable, nondisplaced toe fractures should be treated with buddy taping and a rigid-sole shoe to limit joint movement. Displaced fractures of the lesser toes should be treated with reduction and buddy taping. Patients with displaced fractures of the first toe often require referral for stabilization of the reduction.
Toe fractures are one of the most common fractures diagnosed by primary care physicians. In one rural family practice,1 toe fractures comprised 8 percent of 295 fractures diagnosed; in an Air Force family practice residency program,2 they made up 9 percent of 624 fractures treated. Published studies suggest that family physicians can manage most toe fractures with good results.1,2
Anatomy
The first toe has only two phalanges; the second through the fifth toes generally have three, but the fifth toe sometimes can have only two (Figure 1). Flexor and extensor tendons insert at the proximal portions of the middle and distal phalanges. These tendons may avulse small fragments of bone from the phalanges; they also can be injured when a toe is fractured. Abductor, interosseus, and adductor muscles insert at the proximal aspects of each proximal phalanx. The pull of these muscles occasionally exacerbates fracture displacement. Sesamoid bones generally are present within flexor tendons in the first toe (Figure 1, top) and are found less commonly in the flexor tendons of other toes. In children, a physis (i.e., cartilaginous growth center) is present in the proximal part of each phalanx (Figure 2).
Differential Diagnosis
The same mechanisms that produce toe fractures may cause a ligament sprain, contusion, dislocation, tendon injury, or other soft tissue injury. Radiographs often are required to distinguish these injuries from toe fractures. Stress fractures can occur in toes. They typically involve the medial base of the proximal phalanx and usually occur in athletes. Stress fractures have a more insidious onset and may not be visible on radiographs for the first two to four weeks after the injury.
History and Physical Findings
Most toe fractures are caused by an axial force (e.g., a stubbed toe) or a crushing injury (e.g., from a falling object). Joint hyperextension, a less common mechanism, may cause spiral or avulsion fractures. Common presenting symptoms include bruising, swelling, and throbbing pain that worsens with a dependent position, although this type of pain also may occur with an isolated subungual hematoma. Although tendon injuries may accompany a toe fracture, they are uncommon.
Physical examination should include assessment of capillary refill; delayed capillary refill may indicate circulatory compromise. The skin should be inspected for open wounds or significant injury that may lead to skin necrosis. The nail should be inspected for subungual hematomas and other nail injuries. Deformity of the digit should be noted; most displaced fractures and dislocations present with visible deformity. Nondisplaced fractures usually are less apparent; however, most patients with toe fractures have point tenderness over the fracture site. The localized tenderness of a contusion may mimic the point tenderness of a fracture. Application of a gentle axial loading force distal to the injury (i.e., compressing the distal phalanx toward the foot) may distinguish contusions from fractures. If this maneuver produces sharp pain in a more proximal phalanx, it suggests a fracture in that phalanx.
Radiographic Findings
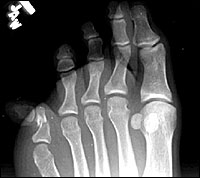
Radiographic studies of a toe should include anteroposterior, lateral, and oblique views (Figure 1). A combination of anteroposterior and lateral views may be best to rule out displacement. However, overlying shadows often make the lateral view difficult to interpret (Figure 1, center). In many cases, anteroposterior and oblique views are the most easily interpreted (Figure 1, top and bottom).
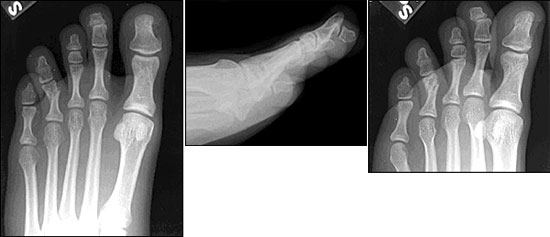
Fractures of the lesser toes are four times as common as fractures of the first toe.3 Most toe fractures are nondisplaced or minimally displaced. Comminution is common, especially with fractures of the distal phalanx. Displaced spiral fractures generally display shortening or rotation, whereas displaced transverse fractures may display angulation. In children, toe fractures may involve the physis (Figure 2).
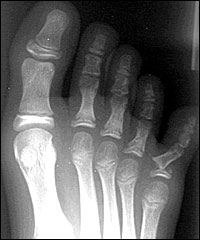
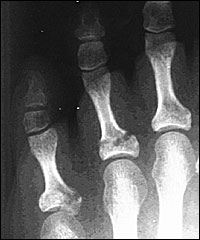
Fractures of multiple phalanges are common (Figure 3). Therefore, phalanges and digits adjacent to the fracture must be examined carefully; joint surfaces also must be examined for intra-articular fractures (Figure 3). Patients with intra-articular fractures are more likely to develop long-term complications.
Indications for Referral
Patients with circulatory compromise require emergency referral. Toe fractures of this type are rare unless there is an open injury or a high-force crushing or shearing injury. Patients with open toe fractures or fractures with overlying skin necrosis are at high risk for osteomyelitis. If there is a break in the skin near the fracture site, the wound should be examined carefully. If the wound communicates with the fracture site, the patient should be referred. In some practice sites, family physicians manage open toe fractures; a discussion about the management of this type of injury can be found elsewhere.3,4 Patients also may require referral because of delayed complications such as osteomyelitis from open fractures, persistent pain after healing, and malunion.
FRACTURES OF THE FIRST TOE
Because of the first toe's role in weight bearing, balance, and pedal motion, fractures of this toe require referral much more often than other toe fractures. Deformity, decreased range of motion, and degenerative joint disease in this toe can impair a patient's functional ability.
Referral is recommended for patients with first-toe fracture-dislocations, displaced intra-articular fractures, and unstable displaced fractures (i.e., fractures that spontaneously displace when traction is released following reduction). Referral also is recommended for children with first-toe fractures involving the physis.4 These injuries may require internal fixation.
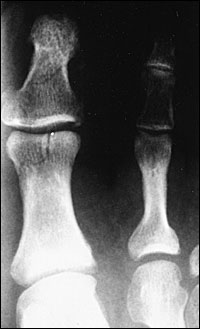
Referral should be strongly considered for patients with nondisplaced intra-articular fractures involving more than 25 percent of the joint surface (Figure 4).4 These fractures may lose their position during follow-up. Even if the fragments remain nondisplaced, significant degenerative joint disease may develop.4
Referral also should be considered for patients with other displaced first-toe fractures, unless the physician is comfortable with their management.
FRACTURES OF THE LESSER TOES
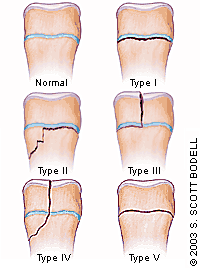
Although referral rarely is required for patients with fractures of the lesser toes, referral is recommended for patients with open fractures, fracture-dislocations (Figure 5), displaced intra-articular fractures, and fractures that are difficult to reduce. Referral is recommended for children with fractures involving the physis, except nondisplaced Salter-Harris type I and type II fractures (Figure 6).4
Patients with unstable fractures and nondisplaced, intra-articular fractures of the lesser toes that involve more than 25 percent of the joint surface (Figure 3) usually do not require referral and can be managed using the methods described in this article.
Treatment
STABLE, NONDISPLACED FRACTURES
Patients with closed, stable, nondisplaced fractures can be treated with splinting and a rigid-sole shoe to prevent joint movement. To enhance comfort, some patients prefer to cut out the part of the shoe that overlies the fractured toe. A walking cast with a toe platform may be necessary in active children and in patients with potentially unstable fractures of the first toe.
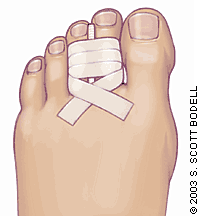
The preferred splinting technique is to buddy tape the affected toe to an adjacent toe (Figure 7).4 Treatment should continue until point tenderness is resolved, usually at least three weeks (four weeks for fractures of the first toe). Taping may be necessary for up to six weeks if healing is slow or pain persists.
To control pain and swelling, patients should apply ice and elevate the affected foot for the first few days after the injury. Patients should limit icing to 20 minutes per hour so that soft tissues will not be injured. Non-narcotic analgesics usually provide adequate pain relief. Narcotic analgesics may be necessary in patients with first-toe fractures, multiple fractures, or fractures requiring reduction.
If an acute subungual hematoma is present (less than 24 hours old), decompression may relieve pain substantially. Despite theoretic risks of converting the injury to an open fracture, decompression is recommended by most experts.5 Toenails should not be removed because they act as an external splint in patients with fractures of the distal phalanx.
After the splint is discontinued, the patient should begin gentle range-of-motion (ROM) exercises with the goal of achieving the same ROM as the same toe on the opposite foot. Follow-up radiographs may be taken three to six weeks after the injury, but they generally do not influence treatment and probably are not necessary in nondisplaced toe fractures.
DISPLACED FRACTURES OF LESSER TOES
After anesthetizing the toe with ice or a digital block, the physician holds the tip of the toe, applies longitudinal traction, and manipulates the bone fragments into proper position. In most cases, this is done by simply adjusting the direction of traction to correct any shortening, rotation, or malalignment. To unlock fragments, it may be necessary to exaggerate the deformity slightly as traction is applied or to manipulate the fragments with one hand while the other maintains traction. Following reduction, the nail bed of the fractured toe should lie in the same plane as the nail bed of the corresponding toe on the opposite foot. If it does not, rotational deformity should be suspected. Unless it is fairly subtle, rotational deformity should be corrected by further manipulation.
The reduced fracture is splinted with buddy taping. Fracture position ideally will be maintained when traction is released, but in some cases the reduction can be held only with buddy taping. Referral is indicated if buddy taping cannot maintain adequate reduction.
DISPLACED FRACTURES OF THE FIRST TOE
Displaced fractures of the first toe generally are managed similarly to displaced fractures of the lesser toes. To minimize the possibility of future disability, the position of the bone fragments after reduction should be as close to anatomic as possible. If the reduction is unstable (i.e., the position is not maintained after traction is released), splinting should not be used to hold the reduction, and referral is indicated.
To check proper alignment, radiographs should be taken immediately after reduction and again seven to 10 days after the injury (three to five days in children).4 In patients with potentially unstable or intra-articular fractures of the first toe, follow-up radiographs should be taken weekly for two or three weeks to monitor fracture position. At the conclusion of treatment, radiographs should be repeated to document healing.
Complications
A common complication of toe fractures is persistent pain and a decreased tolerance for activity. Pain that persists longer than a few months may indicate malunion, which may limit a patient's future activities significantly. Toe fractures, especially intra-articular fractures, can result in degenerative joint disease, and osteomyelitis is a potential complication of open fractures.