A 46-year-old woman presented for her annual well-woman examination and Papanicolaou smear. She had no complaints, except for occasional itchiness associated with skin lesions (see accompanying figure) that were symmetrically present in both axillae.
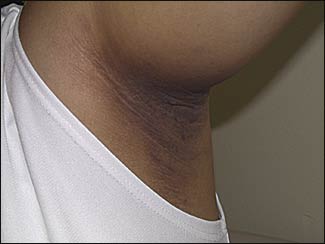
On further questioning, she revealed that she had always been overweight and had multiple family members with type 2 diabetes. She had not recently changed bathing soap, deodorant, or laundry detergent brands. She also denied having myalgias, arthralgias, or other rashes.
On examination, she was obese, with some hair growth on her upper lip. Skin examination revealed velvety, hyperpigmented lesions in the axillae. Thyroid examination was normal. Laboratory results showed a borderline elevated blood glucose level and normal complete blood count.
Question
Based on the patient's history and physical examination, which one of the following is the correct diagnosis?
A. Cutaneous lupus.
B. Acanthosis nigricans.
C. Contact dermatitis.
D. Superficial spreading melanoma.
E. Erythrasma.
Discussion
The correct answer is B: acanthosis nigricans. The lesion seen in the figure is called acanthosis nigricans. Acanthosis nigricans is a nonspecific skin change most commonly found in flexural areas such as the axillae, beltline, or the nuchal fold. It is associated with insulin resistance, most commonly caused by obesity. When the lesion is seen in a patient without apparent diabetes or obesity, evaluation for other causes should be pursued, such as hypothyroidism, gastrointestinal malignancy, or other causes of insulin resistance (e.g., polycystic ovary syndrome, rare lipodystrophies).
Melanoma is in the differential of any pigmented skin lesion; however, the large size and symmetric location of these axillary lesions would greatly decrease suspicion of melanoma.
Chronic skin exposure to an irritant or allergen may lead to lichenification and hyperpigmentation, but contact dermatitis is less likely to be the cause of this patient's lesions because no topical exposure is recalled and no new deodorant, soap, or detergent has been used.
Systemic lupus erythematosus has been associated with acanthosis nigricans, especially in black women. However, this patient has no other signs suggestive of this disease. Lupus is less likely, given the lack of myalgias or arthralgias and a completely normal blood count.
Erythrasma is a bacterial infection caused by Corynebacterium minutissimum. While it is most commonly seen in the groin area, it also may involve the axillae. The brown or brick-red color may appear similar to acanthosis nigricans, but there is no velvety thickening of the skin with erythrasma. This skin infection usually responds rapidly to oral or topical antibiotics, whereas acanthosis nigricans would be unaffected.
Weight loss and control of blood glucose levels may improve acanthosis nigricans caused by obesity and insulin resistance. Topical retinoic acid or oral isotretinoin (Accutane) has been prescribed for cosmetic improvement, with variable reports of success.1 Additionally, topical alphahydroxy acid solutions may be useful for softening the lesions.1

