Although local anesthesia usually is used in surgical procedures, field or nerve blocks can provide more effective anesthesia in some situations. In a field block, local anesthetic is infiltrated around the border of the surgical field, leaving the operative area undisturbed. In field blocks, epinephrine may be added to the anesthetic to enhance vasoconstriction and prolong the duration of anesthesia. In a nerve block, anesthetic is injected directly adjacent to the nerve supplying the surgical field. A review of regional anatomy and the location of nerves and other important structures is essential before administering the injection. Systemic toxicity is rare with regional anesthesia and can be prevented by using the smallest dose possible and aspirating before the injection. Supraorbital, supratrochlear, infraorbital, and mental nerve blocks can provide adequate anesthesia in procedures on parts of the face. Field block also may be considered when operating on the ear or lips.
Effective anesthesia is a prerequisite for any surgical procedure. Most family physicians use local anesthesia because of its ease of administration, safety, and efficacy. However, large doses may be required for some procedures, and other anesthetic techniques may be considered in certain clinical situations. Part I of this two-part article focuses on regional anesthetic options for surgeries of the head and neck.
Comparison of Anesthesia Options
For laceration repair, topical anesthesia may be as effective as local infiltration and usually causes no discomfort, making it especially useful in children.1,2 For procedures on intact skin in children, one commonly used topical agent is EMLA cream (eutectic mixture of local anesthetics), a combination of 2.5 percent lidocaine and 2.5 percent prilocaine. EMLA has proven benefits but is limited by its delayed onset of action (one to two hours after application).3,4
The field block anesthetizes the nerves supplying the skin in the operative field. Local anesthetic solution is infiltrated around the border of the surgical field. Anesthesia from a field block lasts longer than that from local infiltration,5 and it does not cause swelling in the surgical field or obscure local anatomy.2
TABLE 1 Uses for Regional Anesthesia in the Office Setting
| Abscess incision and drainage |
| Closed reduction of fractures and dislocations |
| Foreign body removal |
| Ingrown toenail excision |
| Paronychia drainage |
| Subcutaneous cyst removal |
| Suturing |
| Topically before procedures such as nasolaryngoscopy, esophagogastroduodenoscopy |
| Wound debridement |
Regional anesthesia is particularly useful when larger areas must be anesthetized; in these cases, local infiltration would require large doses of anesthetic (Table 1). In a nerve block, anesthetic is injected into the extra-neural or paraneural spaces, providing complete anesthesia in the region supplied by that nerve, distal to the site of injection.6 Blunt bevel (B bevel) needles, which have an increased bevel angle (45 degrees) and blunter tip, may minimize nerve trauma.7 Patients usually are adequately anesthetized within10 to 20 minutes of the injection, and nerve blocks require relatively small amounts of anesthetic solution. Anesthesia begins with sympathetic blockade, which causes peripheral vasodilatation. Patients then experience a loss of pain, temperature sensation, proprioception, and touch and pressure sensation; motor paralysis is the final stage.3
TABLE 2 Reasons to Avoid Use of Regional Anesthesia
| Allergy to anesthetic agent |
| Infection at injection site |
| Poor patient acceptance or cooperation |
| Physician's lack of familiarity with nerve block |
| Coagulopathy |
Information from reference 8.
The key to successful regional anesthesia is familiarity with the local anatomy of the nerve and its associated landmarks. To help avoid injecting anesthetic into the nerve, the patient is told to signal if any paresthesia is felt in the region of needle insertion. Some physicians think paresthesia helps localize the nerve; however, this technique may increase the risk for residual neuropathy.5 Sharp, severe pain on injection signals intraneural injection; the needle should be withdrawn before additional anesthetic is injected. Communicating with the patient and minimizing sedation adds another element of safety. Regional anesthesia can be used in almost any situation where local anesthesia is not suitable, but certain higher risk situations should be avoided (Table 2).8
TABLE 3 Potential Systemic Toxicity with Regional Anesthesia
| Central nervous system |
| Lightheadedness, tinnitus, metallic taste, visual disturbances, numbness of the tongue and lips (rarely progressing to muscle twitching), loss of consciousness, seizures, and coma. |
| Cardiovascular system |
| Decreased ventricular contractility, decreased conduction, and loss of vasomotor tone. |
Local toxicity with regional anesthesia is rare.3,9 Most cases of systemic toxicity involve central nervous system or cardiovascular compromise resulting from intravascular injection or an overdose of the anesthetic (Table 3). These complications can be prevented by using the smallest effective dose of anesthetic and aspirating before the injection. Bupivacaine (Marcaine) use has been associated with higher rates of cardiac complications.10 In pregnant patients, local anesthetics given in large doses may be absorbed and transferred to the fetus; high fetal concentrations of anesthetics can lead to adverse effects.11 Cervical blocks, for example, usually should be avoided in pregnant patients.
Preparation
Before regional anesthesia is given, the procedure, risks, and potential complications are explained to the patient, and consent is obtained. No special preparation is necessary for topical anesthesia. A review of regional anatomy and the location of nerves and other important structures also are essential before the injection.
When infiltrating anesthesia is used, the anesthetic solution is drawn into a syringe with a large-bore needle (e.g., 18 gauge). Lidocaine (Xylocaine) is the most commonly used local anesthetic because of its rapid onset of action and adequate duration. However, many other agents are available (Table 4).9,12 A 1 percent or 2 percent lidocaine solution is used in local infiltration and field blocks; in nerve blocks, the concentration usually is limited to 1 percent. Epinephrine (1:100,000 to 1:200,000 dilution) may be added to anesthetic solutions in local infiltrations and field blocks to enhance vasoconstriction, which decreases systemic absorption and prolongs the duration of anesthesia.4,13 However, this technique is not used in nerve blocks because many nerves run immediately adjacent to arterial vessels; inadvertent intravascular injection could cause ischemia. Epinephrine administration also should be avoided near the terminal arterial branches in the digits, tip of the nose, ear lobes, or tip of the penis.2,3
Sodium bicarbonate may be added to neutralize the acidic local anesthetic and to reduce the burning sensation associated with anesthetic administration.14,15 The usual mixture is a 1:10 dilution (1 mL of sodium bicarbonate added to 10 mL of 1 percent lidocaine). Buffering lidocaine may cause the agent to slowly lose its effectiveness; therefore, it is recommended that the solution be used within one week of mixing.
The area to be anesthetized is cleaned with povidoneiodine solution before the anesthetic is injected. Small-gauge needles (e.g., 25 to 30 gauge) are used to reduce patient discomfort. Stretching the skin at the injection site may decrease discomfort.
TABLE 4 Commonly Used Local Anesthetic Agents
| Agent | Drug class | Concentration (%) | Onset | Duration* | Maximum dose (mg per kg) |
|---|---|---|---|---|---|
| Lidocaine (Xylocaine) | Amide | 1 | Rapid | 30 to 60 minutes | 4 |
| Mepivacaine (Carbocaine) | Amide | 1 | Moderate | 45 minutes to 1.5 hours | 4 |
| Bupivacaine (Marcaine) | Amide | 0.25 | Slow | 2 to 4 hours | 3 |
| Procaine (Novocain) | Ester | 1.0 to 2.0 | Slow | 15 to 60 minutes | 7 |
| Tetracaine (Pontocaine) | Ester | 0.25 | Slow | 2 to 3 hours | 1.5 |
| Chloroprocaine (Nesacaine) | Ester | 2 | Slow | 30 minutes | 6 to 7 |
*—Duration is increased in local anesthetics that contain epinephrine.
Topical Anesthesia
A combination of lidocaine, epinephrine, and tetracaine (Pontocaine) may be used for repair of skin lacerations.16 A cotton-tipped applicator or cotton ball soaked in the mixture is applied and held in place for 20 to 30 minutes. This procedure is contraindicated in areas supplied by end-arteries (e.g., pinna, nose, penis, and digits). For procedures on intact skin, EMLA is applied and covered with an occlusive dressing such as Tegaderm. The anesthetic must be left in contact with the skin for one to two hours before beginning the procedure; reapplication for at least 30 to 60 minutes may be necessary. Anesthetic sprays may be used on mucous membranes. The anesthetic is sprayed for 15 to 30 seconds and may be repeated to achieve adequate anesthesia.
Local Infiltration
Local infiltration is used when anesthesia is required in small areas (e.g., for repair of minor lacerations, skin biopsies). The anesthetic solution is infiltrated to the deep dermis, where the sensory plexus supplying the skin begins to branch. The amount of solution used depends on the area that needs to be infiltrated; however, extensive local infiltration is not recommended.
FIGURE 1. Field block.
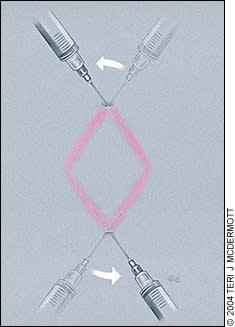
FIGURE 2.
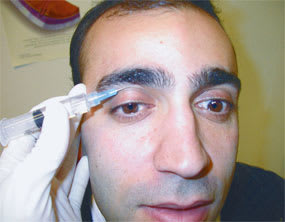
Supraorbital nerve block.
FIGURE 3.
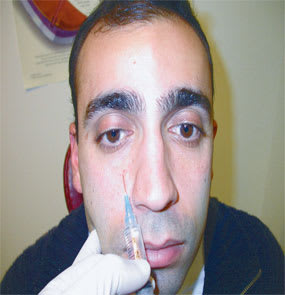
Infraorbital nerve block.
FIGURE 4.
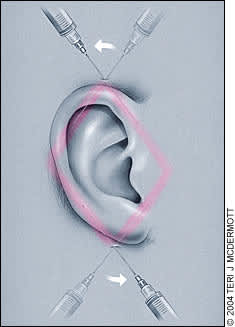
Ear block.
Field Block
In the field block, anesthetic is infiltrated to the subcutaneous area surrounding the operative field. The needle is inserted at two points, and anesthetic solution is injected along four lines (walls) that surround the area to be anesthetized (Figure 1). The shape of the anesthetic field can be modified by changing the number and direction of the anesthetic walls.
Forehead Block
The forehead is supplied by the supraorbital and supratrochlear nerves. The supraorbital nerve emerges from the supraorbital foramen, which can be palpated along the upper border of the orbit, approximately 2.5 cm lateral to the midline of the face. The supratrochlear nerve exits along the upper border of the orbit, approximately 1 cm medial to the supraorbital foramen (Figure 2).
The supraorbital nerve is blocked by inserting the needle toward the foramen and injecting 2 to 3 mL of 1 percent lidocaine. Injection directly into the foramen should be avoided to decrease the risk of nerve damage. To block the supratrochlear nerve, 2 to 3 mL of 1 percent lidocaine is injected along the upper orbital margin, 1 cm medial to the supraorbital foramen. To block both nerves, approximately 5 to 7 mL of 1 percent lidocaine is infiltrated just above the bone beneath the medial two thirds of the eyebrow.
FIGURE 5.
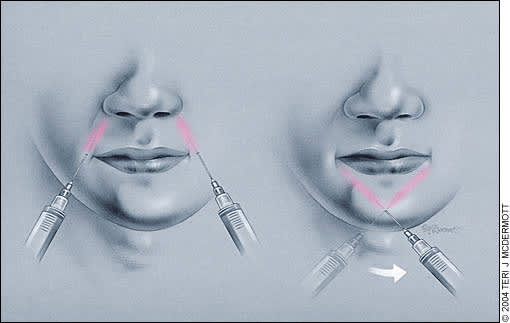
Upper and lower lip block.
Infraorbital Nerve Block
The infraorbital nerve supplies the central area of the face, including the upper lip, cheeks, and part of the external nose. The nerve exits from the infraorbital foramen, which is located just inferior to the orbit slightly nasal to an imaginary line drawn through the middle of the infraorbital rim.17
For the nerve block, the needle is inserted approximately 1 cm inferior to the infraorbital foramen and advanced upward toward the foramen, and 2 to 4 mL of 1 percent lidocaine is injected (Figure 3). The needle is directed upward and laterally to avoid passing through the foramen into the orbit.
Ear Block
The ear is supplied by the greater auricular, lesser occipital, and auriculotemporal nerves, and the mastoid branches of the lesser occipital nerve.17 A field block is required for anesthesia. Approximately 10 to 20 mL of anesthetic is injected above and below the ear to produce a rhomboid-shaped block (Figure 4). Caution should be used in the vicinity of the temporal artery.
Lip Block
Upper lips are anesthetized from two points, one on each side of the angle of the mouth (Figure 5). A total of 5 to 10 mL of anesthetic is injected along two lines in the direction of the nasal alae.
For lower lip anesthesia, the needle is injected at the midpoint of the chin and soft tissues are infiltrated obliquely upward toward the angle of the mouth (Figure 5). A total of 10 to 15 mL of anesthetic generally is required.
FIGURE 6.
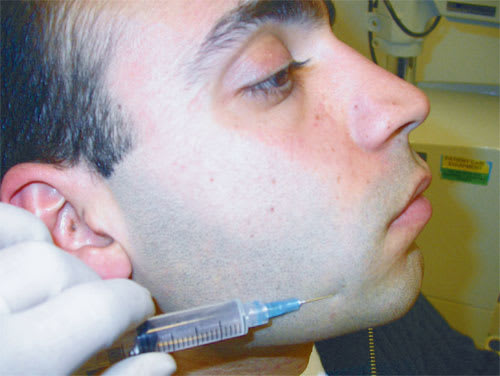
Mental nerve block.
Mental Nerve Block
The mental nerve supplies the sensory innervation to the anterior aspect of the mandible. It emerges from the mental foramen, which lies between the upper and lower borders of the mandible, and is located on the continuation of an imaginary line from the supraorbital foramen through the pupil and the infraorbital foramen.18 The needle is injected about 1.5 cm posterior and lateral to the foramen and directed toward the foramen; 2 to 3 mL of 1 percent lidocaine is injected (Figure 6).

