Urticaria (i.e., pruritic, raised wheals) and angioedema (i.e., deep mucocutaneous swelling) occur in up to 25 percent of the U.S. population. Vasoactive mediators released from mast cells and basophils produce the classic wheal and flare reaction. Diagnosis can be challenging, especially if symptoms are chronic or minimally responsive to therapy. A thorough medical history, physical examination, and methodical investigation are necessary to uncover diagnostic clues. Although serious medical illness can occur concurrently with chronic urticaria, acute urticaria generally is benign and self-limited. The mainstay of therapy for urticaria is avoidance of known triggering agents, judicious use of oral corticosteroids, and treatment with long-acting second-generation antihistamines, H2-receptor antagonists, tricyclic antidepressants, and anti-inflammatory leukotriene antagonists. Consultation for investigative therapy may be necessary if symptoms continue despite a stepwise approach to diagnosis and therapy.
Primary care physicians frequently encounter patients with acute-onset urticaria and angioedema; the prevalence in the United States population is 14 to 25 percent.1 Caring for patients with these disorders becomes challenging when symptoms are severe, involve multiple organ systems, or recur over months or years. Diagnostic testing can be expensive and may not determine a cause. Patients may become anxious, fearing an undiagnosed illness, and physicians may become frustrated by the lack of data to determine an etiology.
FIGURE 1.
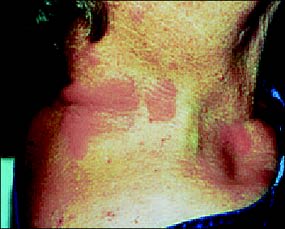
Chronic urticaria in an elderly patient.
Clinical Manifestations
Urticarial lesions are polymorphic, round or irregularly shaped pruritic wheals that range in size from a few millimeters to several centimeters (Figure 1). Lesions can develop anywhere on the body and are spread by scratching, combining into large, fiery-red patches. Sometimes a vascular steal phenomenon causes lesions to appear hyperemic in the center with a white halo along the circumference.2
Angioedema, which can occur alone or with urticaria, is characterized by nonpitting, non-pruritic, well-defined, edematous swelling that involves subcutaneous tissues (e.g., face, hands, buttocks, genitals), abdominal organs, or the upper airway (i.e., larynx). Angioedema tends to occur on the face and may cause significant disfigurement (Figure 2). Laryngeal angioedema is a medical emergency requiring prompt assessment. Acute intestinal and stomach swelling may mimic symptoms of an abdominal surgical emergency.
Chronology differentiates subcategories of urticaria. Wheal and flare reactions last fewer than six weeks in patients with acute urticaria, but chronic urticaria can persist for months or years. In a recent study, 47 percent of patients with chronic urticaria of unknown etiology had spontaneous remission after one year.3 Patients with physical urticaria (i.e., lesions produced by physical stimuli) had more persistent disease, with only 16 percent undergoing spontaneous remission.3
FIGURE 2.
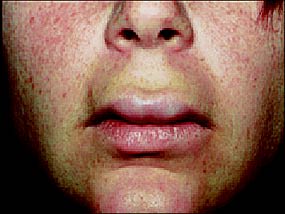
Disfiguring angioedema of the face and lips.
Acute urticaria also is differentiated from chronic urticaria by ongoing or longstanding urticarial symptoms that trigger an IgE-mediated process. Chronic urticaria and angioedema tend to be idiopathic, with no identifiable cause, or to be precipitated by a multitude of endogenous or exogenous factors that can be immunologic or nonimmunologic (Table 1).
Clinical Evaluation and Pathogenesis
Evaluation of patients with urticaria begins with a thorough history that details travel, recent infection, occupational exposure, medications (prescription drugs and herbal and vitamin supplements), ingestion of foods, timing and onset of lesions, morphology, and associated symptoms. Family medical history, preexisting allergies, and exposure to physical stimuli should be documented. A comprehensive physical examination can uncover important diagnostic clues that may help diagnose comorbidities. Physicians should ensure that proper health maintenance testing is up to date and consider diagnostic testing directed by history and physical examination findings, especially in patients with chronic urticaria.4,5
Acute urticaria is self-limited and requires minimal laboratory evaluation. In asymptomatic patients with chronic urticaria and minimal history or physical examination findings, clinical practice guidelines suggest consideration of a complete blood count with differential, urinalysis, erythrocyte sedimentation rate, and liver function tests to screen for a medical condition.4,5
A recent systematic review of more than 6,000 patients with urticaria and angioedema found that routine laboratory screening tests independent of the patient's history and physical examination should be discouraged, because these tests are of little value in discovering the cause of the reactions.6 [Recommendation level B, systematic review of lower quality trials] Clinical scenarios may offer diagnostic clues. For example, an IgE-mediated reaction would be suspected in patients with a history of acute urticaria within an hour after ingesting a food or drug. Skin testing or radioallergosorbent testing may document a causal relationship.4
Histamine released from cutaneous mast cells and basophils in response to inciting stimuli is the primary mediator of urticaria. In this process, specific IgE antibodies cross-link the IgE receptors bound to mast cells and stimulate the production of preformed and newly generated inflammatory mediators. Complement anaphylatoxins also may induce mast cell histamine release, as can certain medications or physical stimuli through direct nonimmunologic mast cell activation.1,7
IMMUNOLOGIC RESPONSES
Immunologic urticaria and angioedema are a result of IgE antibody-mediated reactions that usually occur within one hour of exposure to the allergen. Type I IgE-mediated allergic reactions can be caused by drugs (most notably penicillin and cephalosporin), insect venom, foods (e.g., fish, shellfish, eggs, nuts, legumes, milk, soy, wheat), preservatives, latex, and aeroallergens (e.g., dust mites, molds, pollens, animal dander).4,8
A rarer cause of acute urticaria is a type II hypersensitivity reaction mediated by cytotoxic antibodies and complement activation. An example is a transfusion reaction in which IgG and IgM anti–red-cell antibodies activate complement and cause cell lysis.9 Serum sickness caused by drugs or proteins is an example of a type III hypersensitivity (antigen-antibody complex-mediated) reaction. Clinical presentation may include urticaria of several weeks' duration, arthralgias, fever, and glomerulo-nephritis.8 Urticaria also has been associated with herpes virus, cytomegalovirus, Epstein-Barr virus, and chronic hepatitis infections, and with bacterial, fungal, and parasitic infections.4,5,9 Patients with chronic urticaria and a family history of thyroid disease may be at higher risk for Hashimoto's thyroiditis.10
Urticarial vasculitis should be considered if a single urticaria lesion lasts longer than 24 hours, if lesions are burning or painful, if they are more common in the lower extremities, and if they leave an area of hemosiderin pigment after they have resolved.4,5,9 Infection, drug sensitivity, serum sickness, chronic hepatitis, hypocomplementemic urticarial vasculitis syndrome, and systemic lupus erythematosus may cause urticarial vasculitis.11,12 A 4-mm punch biopsy may confirm neutrophilic infiltration consistent with leukocytoclastic vasculitis. Patients with urticarial vasculitis should be referred to a dermatologist for further evaluation and management, which may include immunomodulatory therapy to down-regulate the inflammatory response.4,5,9
NONIMMUNOLOGIC RESPONSES
Ingestion of certain foods, including strawberries, tomatoes, shrimp, lobster, cheese, spinach, and eggplant, also can trigger hives through direct mast cell degranulation. Several medications, including opiates (especially codeine and morphine), muscle relaxants (e.g., curare [Tubocurarine]), vancomycin (Vancocin), dextran, bile salts, nonsteroidal anti-inflammatory drugs, aspirin, and radiographic contrast media, may produce acute-onset wheal and flare reactions in susceptible patients.4,9 Angioedema has been reported in patients taking angiotensin-converting enzyme inhibitors.5 Patients with a rare inherited or acquired disorder linked to C1 esterase deficiency or autoimmune consumption may present with recurrent angioedema without urticaria.
TABLE 1 Common Causes of Urticaria and Angioedema
| Immunologic causes | ||
| Type I IgE-mediated | ||
| Foods: tree nuts, legumes, crustacea, mollusks, fish, eggs, milk, soy, wheat | ||
| Organic substances: preservatives, latex, hymenoptera venom | ||
| Medications: penicillin, cephalosporin, aspirin, NSAIDs | ||
| Aeroallergens: dust mites, pollens, molds, animal dander | ||
| Type II cytoxic antibody-mediated: transfusion reaction | ||
| Type III antigen-antibody mediated: serum sickness reaction | ||
| Type IV delayed hypersensitivity: medication, food handling, or exposure to animals | ||
| Autoimmune disease: Hashimoto's disease, systemic lupus erythematosus, vasculitis, hepatitis | ||
| Infection: viral (e.g., cytomegalovirus, Epstein-Barr, hepatitis), parasitic, fungal, or bacterial | ||
| Nonimmunologic causes | ||
| Physical stimuli: exposure to sun, water, or temperature extremes; delayed pressure (e.g., wearing a heavy backpack); vibration | ||
| Direct mast cell degranulation: opiates, vancomycin (Vancocin), aspirin, radiocontrast media, dextran, muscle relaxants, bile salts, NSAIDs | ||
| Foods containing high levels of histamines: strawberries, tomatoes, shrimp, lobster, cheese, spinach, eggplant | ||
NSAIDs = nonsteroidal anti-inflammatory drugs.
Although most cases of urticaria and angioedema are idiopathic with benign courses, physicians should follow up on factors that might appear inconsequential at first but may prove to be worthy of further evaluation. Table 2 gives diagnostic clues from the clinical investigation and an associated rationale for the development of urticaria and angioedema.
TABLE 2 Clinical Clues and Associated Rationale for Diagnosis of Urticaria and Angioedema
| Clinical clue | Rationale for diagnosis of urticaria or angioedema |
|---|---|
| Wheals and swelling develop immediately or up to 60 minutes after food ingestion, recent change in diet, ingestion of processed foods | Allergy to foods, preservatives, or food coloring agents |
| Medication usage: new medication or supplement started or dosage changed (prescription or over-the-counter, particularly aspirin, NSAIDs, and ACE inhibitors) | Allergy to medication or related molecules, preservatives, or food coloring agents |
| Exercise (particularly jogging), sun exposure, cold or heat exposure, water exposure, pressure, vibration | Physical or environmental exposure |
| Occupational exposure: latex products, chemical irritants (particularly formaldehyde) | Allergy (can manifest as IgE-mediated reaction, contact dermatitis, or irritant dermatitis) |
| Fatigue, weight gain, family history of thyroid disease | Hypothyroidism or Hashimoto's disease |
| Weight loss and fatigue in patient with family historyof lymphoma | Malignancy or lymphoma |
| Travel out of country, exposure to disease | Parasitic, fungal, bacterial, or viral infection |
NSAIDs = nonsteroidal anti-inflammatory drugs; ACE = angiotensin-converting enzyme.
Physical urticaria is triggered by environmental factors, such as pressure to the skin, heat or cold, exercise, sun or water exposure, and mechanical vibration.1,9 Most patients with physical urticaria develop wheals and itching soon after contact with the offending stimuli. However, patients with delayed pressure urticaria develop symptoms two to eight hours after exposure to the pressure stimulus. Physicians should take a thorough history, keeping in mind that the patient may have more than one cause for urticaria. Challenge testing, which reproduces exposure to the suspected stimuli in a supervised clinical environment, can confirm the diagnosis.
Approach to Therapy
Treatment of urticaria should be directed at avoiding known triggering agents and alleviating associated symptoms. Patients should be advised to avoid alcoholic drinks and over-the-counter drugs such as aspirin or nonsteroidal anti-inflammatory drugs because they may aggravate the condition.2,4 [Recommendation level C, expert opinion] Step therapy guidelines for pharmacotherapeutic management of chronic urticaria is given in Figure 3.
FIGURE 3. Pharmacotherapeutic Management of Chronic Urticaria

Step therapy guideline for patients with chronic urticaria. All medications are given orally.
The mainstay of therapy for acute urticaria is a long-acting, nonsedating histamine H1-receptor antagonist such as fexofenadine (Allegra-D), desloratadine (Clarinex), or loratadine (Claritin).5,8,13,14 [Reference 14—Recommendation level C, expert opinion] Cetirizine (Zyrtec) also is effective but may be mildly sedative and should be taken at night. The additive effect of a first-generation H1-receptor antagonist, such as hydroxyzine (Atarax, 10 to 50 mg nightly), with a second-generation H1-receptor antagonist is beneficial for its soporific effects and to alleviate nocturnal pruritus.11 Because of the adjunctive effect of blocking both histaminic receptors, the addition of a histamine H2-receptor antagonist has shown benefit in the management of urticaria in controlled clinical studies.2 Either cyproheptadine (Periactin) or the tricyclic antidepressant doxepin (Sinequan) in titrated dosages is beneficial as supplemental therapy for nocturnal pruritus and the associated anxiety that is common in patients with chronic urticaria and angioedema.9
Patients should be advised of possible carryover of cognitive effects when using sedating antihistamines at night. Leukotriene modifiers such as montelukast (Singulair, 10 mg daily) or zafirlukast (Accolate, 20 mg twice daily) may play a role in a select subgroup of patients with chronic urticaria, especially those with aspirin sensitivity.15 Patients with a history of urticaria and angioedema or isolated angioedema episodes should be prescribed epinephrine in an auto-injectable instrument (EpiPen) in a dosage of 0.3 mg given intra-muscularly in the thigh and be instructed in its proper use for laryngeal edema, bronchospasm, and hypotension.16 [Recommendation level C, expert opinion] Patients with unresponsive urticaria or angioedema should be referred to an allergist or dermatologist and may require a short-term course of oral glucocorticoids (e.g., oral prednisone, 10 to 20 mg daily). Investigative treatment using immunomodulatory therapies such as cyclosporine, plasmapheresis, and intravenous immunoglobulin have been shown to be beneficial in autoimmune chronic urticaria.17–19

