A 64-year-old man with a 50 pack-year history of smoking presented with a lesion on the tongue that was unknown to him but found on a routine examination (Figure 1). His medical history was significant for a recent biopsy-proven squamous cell carcinoma of the right lower lip. On oral examination, a nontender 4-mm, firm, round, pink papule was noted on the right dorsal lateral tongue. Regional lymphadenopathy was not appreciated. Biopsy of the tongue lesion revealed epidermal hyperplasia and characteristic cells in the dermis (Figure 2).
FIGURE 1.
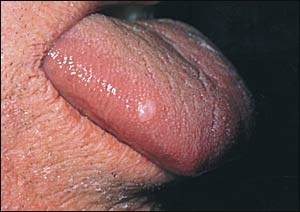
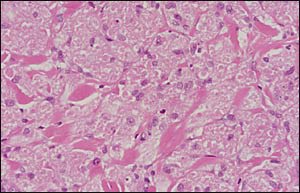
FIGURE 2.
Question
Given the patient's history, physical examination and biopsy findings, which one of the following is the correct diagnosis?
A. Squamous cell carcinoma.
B. Traumatic fibroma.
C. Granular cell tumor.
D. Mucosal neuroma.
E. Minor salivary gland tumor.
Discussion
The answer is C: granular cell tumor, which was established by biopsy. Granular cell tumor, thought to be of Schwann cell origin, occurs as a small solitary tumor on the tongue in about one half of cases. However, it can occur in the skin or subcutaneous tissue anywhere on the body and may present as single or multiple lesions. Granular cell tumors are more common in women in the fourth to sixth decades of life. The incidence is higher in blacks. Histopathology demonstrates pseudocarcinomatous hyperplasia (epidermal thickening). Sheets of abnormal cells with central hyperchromatic nuclei and eosinophilic granular cytoplasm are seen (Figure 2). The granular appearance of the cytoplasm is caused by an abundance of lysosomes.
Most granular cell tumors demonstrate benign histopathology and also have a benign clinical course. Malignant transformation may occur in up to 2 percent of cases.1 Signs of aggressive behavior that signal possible malignancy include tumor size greater than 5 cm, rapid growth, vascular invasion, and necrosis.2 The most effective treatment for granular cell tumor is wide local excision with a 2- to 3-cm margin.3 In areas where tissue preservation is essential, such as the oral cavity or genitalia, Mohs' micrographic surgery may be indicated.4
Patients with a diagnosis of granular cell tumor should have a complete physical examination to exclude other primary tumors or metastasis from an aggressive malignant tumor. An oral examination is essential because the tongue is the most frequent site of occurrence of granular cell tumors.
Intraoral squamous cell carcinoma may present with a similar tongue lesion, though it typically has a rough, granular surface. Biopsy reveals epidermal hyperplasia similar to that seen in a granular cell tumor; however, varying degrees of cellular atypia are seen, consistent with the malignant nature of this lesion. Squamous cell carcinoma of the tongue most commonly involves the posterior lateral or ventral surfaces.
Traumatic fibroma is the most common lesion of the oral cavity. It is caused by fibrous tissue hyperplasia at a site of localized irritation. This benign type of growth usually presents as a smooth pink nodule along the buccal mucosal bite line, but the tongue also may be affected.
Mucosal neuromas are associated with multiple endocrine neoplasia syndrome, type IIb. They may occur on the tongue but usually present as multiple coalescing papules.
Minor salivary gland tumors, such as mucoepidermoid and adenocystic carcinoma, also are possible sources of intraoral lesions. Biopsy findings distinguish this type of tumor from the entities previously mentioned.

