Family physicians often encounter patients with incidentally noted microscopic hematuria. Cohen and Brown reviewed the management of patients 18 years or older with microscopic hematuria.
The definition of microscopic hematuria varies from one to more than 10 red blood cells per high-power field on urine microscopy, with trade-offs in sensitivity and specificity for diagnosing serious underlying disease. The review authors advocate a cutoff of two or more red cells per field for the diagnosis. They think that urine dipstick testing for heme may be too sensitive and nonspecific. Before work-up is pursued in an asymptomatic patient with a single instance of microscopic hematuria, the authors suggest repeat urine testing several days later, especially if vigorous exercise, menstruation, sexual activity, or urinary tract injury occurred close to the initial episode of hematuria.
Microscopic Hematuria
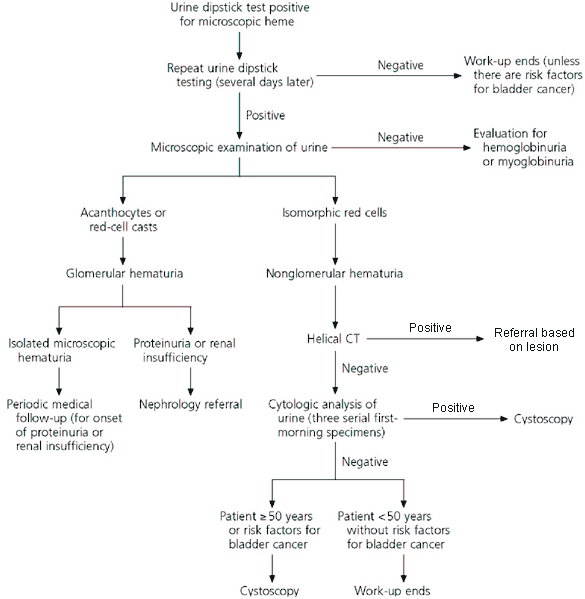
FIGURE. Evaluation of microscopic hematuria. If hematuria is determined to be nonglomerular in origin, computed tomography (CT) should be performed without contrast medium if a stone is suspected to be present or first without and then with contrast medium if no stone is suspected. Ultrasonography should be performed instead of CT in pregnant patients and those with hypersensitivity to contrast medium. Risk factors for bladder cancer include cigarette smoking, occupational exposure to chemicals used in certain industries (leather, dye, and rubber or tire manufacturing), heavy phenacetin use, past treatment with high dosages of cyclophosphamide, and ingestion of aristolochic acid found in some herbal weight-loss preparations.
Adapted with permission from Cohen RA, Brown RS. Microscopic hematuria. N Engl J Med 2003;348:2336.
Urine microscopy is the first step in the evaluation of hematuria (see accompanying figure), to differentiate upper-tract (glomerular) bleeding from a lower-tract source. Red-cell casts in the urine are highly specific for an upper source but are not commonly encountered. Crenated red cells, traditionally considered an indication of glomerular bleeding, may be encountered in any concentrated urine specimen. Acanthocytes, which are doughnut-shaped red cells with a central hole and membrane blebs attached peripherally, are more specific for an upper-tract bleeding source. The most common cause of glomerular bleeding is inherited immunoglobulin A nephropathy, followed by thin basement membrane disease and hereditary nephritis (Alport’s syndrome).
If a glomerular source is considered unlikely, the next step in the evaluation is upper-tract imaging. The authors prefer computed tomography without contrast when urolithiasis is suspected, and computed tomographic urography when stone disease is clinically unlikely. Ultrasonography, excretory urography, or both are alternatives. These methods have lower sensitivity and specificity for detection of small renal neoplasms but are useful options if computed tomography is too expensive or unavailable.
More than two thirds of patients with microscopic hematuria do not have a firm diagnosis after upper-tract imaging. The authors suggest proceeding with cystoscopy if risk factors for bladder cancer are present. Older men and patients who smoke have increased rates of bladder cancer. Observational studies in women have had conflicting results. Urine cytology is highly specific for bladder cancer but has limited sensitivity (e.g., 66 and 79 percent sensitivity in two large studies). Sensitivity is improved by using first-morning voided specimens from three consecutive days.
In many cases, complete upper- and lower-tract work-up of hematuria fails to identify a cause. No controlled studies of follow-up management have been done, but the case series available to date have not identified any occult cancers with later repetition of diagnostic studies.

