The loss of physical function in the elderly is a growing health care problem. Loss of physical function can have a substantially negative impact on patients’ independence and quality of life, as well as social and economic effects. Anemia occurs in approximately 13 percent of persons 70 years and older. It can cause fatigue and weakness that may affect physical function. In addition, anemia can decrease myocardial function and cause the progression of heart and renal failure. Anemia in the elderly is caused most often by cancer, infectious disease, malnutrition, and iron deficiency. However, in at least 20 percent of patients, the cause is unknown. Despite this chronic and common problem, no studies have examined the impact of anemia on the physical function of elderly persons. Penninx and colleagues conducted a four-year longitudinal observational study to evaluate whether anemia would affect physical decline among community-dwelling older persons.
This prospective cohort study was part of the Established Populations for Epidemiologic Studies of the Elderly. The authors enrolled a sample population of persons 65 years and older in two Iowa counties. Home interviews were performed at the start of the study in 1981 and 1982, and were repeated every year for six years and again at 10 years. The physical assessment started in 1988 and included standing balance, walking speed, and ability to rise from a chair. Each task was rated on a scale from zero to 4, with zero representing inability to perform the task and 4 representing the highest level of performance. The decline in physical performance score from 1988 to 1992 was the main outcome recorded.
In 1988, blood was obtained to assess multiple blood levels. Using criteria of the World Health Organization (WHO), anemia was defined as a hemoglobin level below 12 g per dL (7.4 mmol per L) in women and below 13 g per dL (8.1 mmol per L) in men. The authors also defined borderline anemia as hemoglobin values within 1 g per dL (0.6 mmol per L) above the WHO criteria. Mean corpuscular volume was used to define the anemia as macrocytic, normocytic, or microcytic.
FIGURE 1. Physical Performance in Women
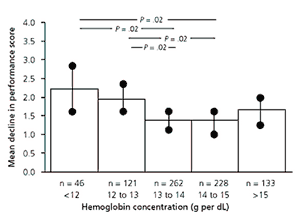
Adjusted mean decline in physical performance score (1988 to 1992) by hemoglobin concentration in women. Decline is adjusted for baseline performance score, age, education, smoking, blood pressure, body mass index, coronary heart disease, heart failure, stroke, diabetes, cancer, lung disease, infectious disease, and renal disease. P values indicate significant differences between categories. Vertical lines indicate 95 percent confidence intervals around the mean adjusted decline.
Reprinted with permission from Penninx BW, Guralnik JM, Onder G, Ferrucci L, Wallace RB, Pahor M. Anemia and decline in physical performance among older persons. Am J Med 2003;115:107.
When other variables were controlled, the adjusted mean decline in the physical performance score was significantly greater in the patients who had anemia compared with those who did not (see Figures 1 and 2). This decline in physical performance was noted even in patients who had no underlying reason or cause for their anemia. After adjusting for serum cholesterol, iron, and albumin levels, patients with anemia still had a significant decline in physical function. Patients whose hemoglobin values placed them in the borderline anemia category had a significant decline in physical function compared with patients with normal hemoglobin values.
Physical Performance in Men
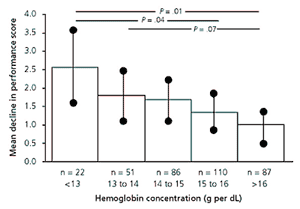
FIGURE 2. Adjusted mean decline in physical performance score (1988 to 1992) by hemoglobin concentration in men. Decline is adjusted for baseline performance score, age, education, smoking, blood pressure, body mass index, coronary heart disease, heart failure, stroke, diabetes, cancer, lung disease, infectious disease, and renal disease. P values indicate significant differences between categories. Vertical lines indicate 95 percent confidence intervals around the mean adjusted decline.
Reprinted with permission from Penninx BW, Guralnik JM, Onder G, Ferrucci L, Wallace RB, Pahor M. Anemia and decline in physical performance among older persons. Am J Med 2003;115:107.
The authors conclude that anemia in old age is a risk factor for decline in physical performance. Further research is needed to determine whether treating anemia in the elderly will preserve physical function.

