The visual appearance of the fingernails and toenails may suggest an underlying systemic disease. Clubbing of the nails often suggests pulmonary disease or inflammatory bowel disease. Koilonychia, or “spoon-shaped” nails, may stimulate a work-up for hemochromatosis or anemia. In the absence of trauma or psoriasis, onycholysis should prompt a search for symptoms of hyperthyroidism. The finding of Beau’s lines may indicate previous severe illness, trauma, or exposure to cold temperatures in patients with Raynaud’s disease. In patients with Muehrcke’s lines, albumin levels should be checked, and a work-up done if the level is low. Splinter hemorrhage in patients with heart murmur and unexplained fever can herald endocarditis. Patients with telangiectasia, koilonychia, or pitting of the nails may have connective tissue disorders.
Careful examination of the fingernails and toenails can provide clues to underlying systemic diseases (Table 1). Clubbing, which is one example of a nail manifestation of systemic disease, was first described by Hippocrates in the fifth century B.C.1 Since that time, many more nail abnormalities have been found to be clues to underlying systemic disorders.
TABLE 1 Nail Findings and Associated Systemic Conditions
| Nail finding | Associated systemic conditions |
|---|---|
| Shape or growth change | |
| Clubbing | Inflammatory bowel disease, pulmonary malignancy, asbestosis, chronic bronchitis, COPD, cirrhosis, congenital heart disease, endocarditis, atrioventricular malformations, fistulas |
| Koilonychia | Iron deficiency anemia, hemochromatosis, Raynaud’s disease, SLE, trauma, nail-patella syndrome |
| Onycholysis | Psoriasis, infection, hyperthyroidism, sarcoidosis, trauma, amyloidosis, connective tissue disorders |
| Pitting | Psoriasis, Reiter’s syndrome, incontinentia pigmenti, alopecia areata |
| Beau’s lines | Any severe systemic illness that disrupts nail growth, Raynaud’s disease, pemphigus, trauma |
| Yellow nail | Lymphedema, pleural effusion, immunodeficiency, bronchiectasis, sinusitis, rheumatoid arthritis, nephrotic syndrome, thyroiditis, tuberculosis, Raynaud’s disease |
| Color change | |
| Terry’s (white) nails | Hepatic failure, cirrhosis, diabetes mellitus, CHF, hyperthyroidism, malnutrition |
| Azure lunula | Hepatolenticular degeneration (Wilson’s disease), silver poisoning, quinacrine therapy |
| Half-and-half nails | Specific for renal failure |
| Muehrcke’s lines | Specific for hypoalbuminemia |
| Mees’ lines | Arsenic poisoning, Hodgkin’s disease, CHF, leprosy, malaria, chemotherapy, carbon monoxide poisoning, other systemic insults |
| Dark longitudinal streaks | Melanoma, benign nevus, chemical staining, normal variant in darkly pigmented people |
| Longitudinal striations | Alopecia areata, vitiligo, atopic dermatitis, psoriasis |
| Splinter hemorrhage | Subacute bacterial endocarditis, SLE, rheumatoid arthritis, antiphospholipid syndrome, peptic ulcer disease, malignancies, oral contraceptive use, pregnancy, psoriasis, trauma |
| Telangiectasia | Rheumatoid arthritis, SLE, dermatomyositis, scleroderma |
COPD = chronic obstructive pulmonary disease; SLE = systemic lupus erythematosus; CHF = congestive heart failure.
The nail plate is the hard keratin cover of the dorsal portion of the distal phalanx. The nail plate is generated by the nail matrix at the proximal portion of the nail bed (Figure 1). As the nail grows, the distal part of the matrix produces the deeper layers of the nail plate, while the proximal portion makes the superficial layers. This production is important, because a disruption of function in the proximal matrix (as may occur in patients with psoriasis) results in more superficial nail problems (e.g., pitting). A disruption of the distal matrix may cause problems with the deeper layers, resulting in ridging or splitting. A transient problem causing growth disturbance may lead to the formation of transverse lines across the nail plate, as in Mees’, Muehrcke’s, and Beau’s lines (Figure 2). Changes in the configuration of the capillaries in the proximal nail bed are responsible for some of the alterations that occur in patients with connective tissue disorders, while abnormalities in the periosteal vessels contribute to clubbing.2
FIGURE 1
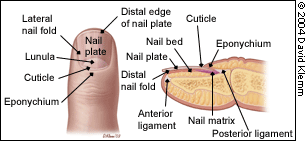
Anatomic structures of the nail.
FIGURE 2
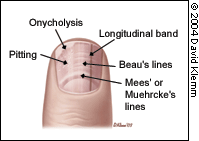
Pathologic findings in the nail.
The nail is bound proximally by the eponychium (the skin just proximal to the cuticle), laterally by the nail folds, and distally by the distal nail fold (defined by the separation created by the anterior ligament between the distal nail bed and the nail plate; Figure 1).
Localized bacterial and fungal infections of the nail, the most common nail problems seen by family physicians, have been reviewed elsewhere.3,4
Growth Disturbances
YELLOW NAIL SYNDROME
A 1964 study5 described “yellow nail syndrome,” in which nails grow more slowly and develop a “heaped-up” or thickened appearance. The lateral sides of the nail plate show exaggerated convexity, the lunula (i.e., the white half-moon at the proximal edge of the nail bed) disappears, and the nail takes on a yellow hue.
This syndrome may be seen in patients with chronic bronchiectasis or sinusitis, pleural effusions, internal malignancies, immunodeficiency syndromes, and rheumatoid arthritis.6 When it occurs in patients with rheumatoid arthritis, yellow nail syndrome commonly is found in the patients treated with thiol drugs (e.g., bucillamine and gold sodium thiomalate); these medications are thought to play a role in the nail condition.7
Because yellow nail syndrome often affects patients with impaired lymphatic drainage of the extremities or face, there may be an etiologic mechanism, although this theory has not been substantiated.8 Others researchers suspect that the cause of yellow nail syndrome may be related to protein leakage from increased microvascular permeability, which would account for its common association with hypoalbuminemia, pleural effusion, and lymphedema.9
CLUBBING
Clubbing of the nails (Figure 3) is a thickening of the soft tissue beneath the proximal nail plate that results in sponginess of the proximal plate and thickening in that area of the digit.1 The cause of clubbing is poorly understood; the condition may result from megakaryocytes and platelet clumps that have escaped filtration in the pulmonary bed and have entered the systemic circulation. Platelets then may release platelet-derived growth factor at the nail bed, causing periosteal changes.10 The angle between the finger proximal to the nail and the proximal nail plate is straightened, creating the “Schamroth sign,” which is an obliteration of the normally diamond-shaped space formed when dorsal sides of the distal phalanges of corresponding right and left digits are opposed (Figure 4).
FIGURE 3
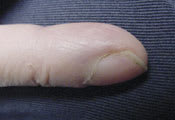
Clubbing. This condition may accompany neoplastic and other lung diseases, atrioventricular malformations, congenital heart disease, celiac disease, and inflammatory bowel disease.
FIGURE 4
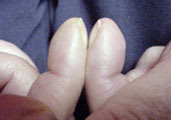
Schamroth sign. This finding, which defines clubbing, is the obliteration of the normal diamond-shaped space at the proximal end of the nail when the distal phalanges are opposed.
Clubbing occurs in patients with neoplastic diseases, particularly those of the lung and pleura. It also may accompany other pulmonary diseases, including bronchiectasis, lung abscess, empyema, pulmonary fibrosis, and cystic fibrosis. Arteriovenous malformations or fistulas have been associated with clubbing, as have celiac disease, cirrhosis, and inflammatory bowel disease. Clubbing also may occur in patients with congenital heart disease and endocarditis. The finding of clubbing without an obvious associated disease should prompt a search for bronchogenic carcinoma or another occult reason for the finding.
KOILONYCHIA
Koilonychia is represented by transverse and longitudinal concavity of the nail, resulting in a “spoon-shaped” nail. This abnormality is sometimes a normal nail variant in infants, but it usually corrects itself within the first few years of life. Koilonychia also may result from trauma, constant occupational exposure of the hands to petroleum-based solvents, or nail-patella syndrome.11 The latter is an autosomal-dominant condition that includes hypoplastic, easily dislocated patellas, renal and skeletal abnormalities, and glaucoma. Koilonychia has been associated with iron deficiency, with or without resultant anemia. Interestingly, it occasionally occurs in patients with hemochromatosis.12
Patients with Raynaud’s disease or lupus erythematosus can have spooning, but it usually is not an isolated finding. When spooning is present without an obvious associated illness, physicians should obtain a complete blood count and ferritin level to help rule out iron deficiency and hemochromatosis.
PITTING
Pitting of the nails shows as punctate depressions in the nail plate. Pitting usually is associated with psoriasis, affecting 10 to 50 percent of patients with that disorder.13 Pitting also may be caused by a variety of systemic diseases, including Reiter’s syndrome and other connective tissue disorders, sarcoidosis, pemphigus, alopecia areata, and incontinentia pigmenti.14 Because pitting is caused by defective layering of the superficial nail plate by the proximal nail matrix, any localized dermatitis (e.g., atopic or chemical dermatitis) that disrupts orderly growth in that area also can cause pitting.
ONYCHOLYSIS
Onycholysis, which occurs when the nail plate is separated from the nail bed, results in white discoloration of the affected area. It can be caused by any local problem, such as periungual warts or onychomycosis, that separates the nail plate from the bed, although the most common reason for this separation is trauma.
Separation may result if the nail is lifted mechanically off the bed or if a blow to the nail causes bleeding between the nail and the bed (Figure 5). Onycholysis can accompany psoriasis when the distal portion of the nail matrix is affected. If no clear local cause is discovered, a diagnosis of hyperthyroidism should be considered. In patients with hyperthyroidism, onycholysis is known as “Plummer’s nails.” Hyperthyroidism also can cause brown discoloration of the nail plate.
FIGURE 5
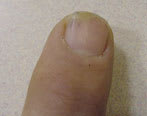
Onycholysis and splinter hemorrhage. This condition may result from trauma; onycholysis also results from hyperthyroidism, warts, and onychomycosis.
Transverse Linear Lesions
Transverse linear depressions in the nail plate have been called Beau’s lines since these lesions originally were described in 1846. Beau’s lines occur at the same spot of the nail plate in most or all of the person’s nails and may be caused by any disease severe enough to disrupt normal nail growth (Figure 6). Knowing that nails grow about 1 mm every six to 10 days, the timing of the disease process may be estimated by measuring the distance from the line to the nail bed. Other causes of Beau’s lines include trauma and exposure to cold temperatures in patients with Raynaud’s disease.7,8
FIGURE 6
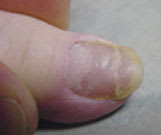
Beau’s lines. This condition demonstrates as transverse depressions in the nail that result from trauma, exposure to cold, Raynaud’s disease, or any episodic disease serious enough to disrupt normal nail growth.
Classically associated with arsenic poisoning, Mees’ lines are transverse white bands that frequently affect multiple nails, although they also may occur singly. If arsenic poisoning is suspected, hair or tissue samples should be obtained for verification; however, Mees’ lines also may be associated with multiple other conditions (Table 1).
In patients with Mees’ lines, the nail bed is normal, but the nail itself is microscopically fragmented, probably because of the disruption of normal growth at the nail matrix during the insult. The width of the lines varies and, because the defect is in the nail itself, the line moves distally with time. Thus, the timing of the insult can be determined by measuring the distance of the lines from the cuticle.
Pairs of transverse white lines that extend all the way across the nail are called Muehrcke’s lines. The lines represent an abnormality of the vascular nail bed and disappear while the nail is depressed and blood is squeezed from the vessels beneath the nail. Because the lesion is in the nail bed, it does not move with nail growth. These characteristics distinguish Muehrcke’s lines from Mees’ lines. Muehrcke’s lines occur in patients with hypoalbuminemic states (i.e., albumin level less than 2 g per dL [20 g per L]) and disappear when the protein level normalizes. They also may be present in patients with nephrotic syndrome, liver disease, and malnutrition.9
Children and active adults commonly have one or more white lines or spots on one or more nails; this condition is known as leukonychia (Figure 7). These lines and spots are nonuniform, appear in different places on different nails, do not span the nail, and are of no significance. They are thought to result from random minor trauma to the proximal nail bed. Unlike leukonychia, Mees’ and Muehrcke’s lines are always parallel to the edge of the lunula.10
FIGURE 7
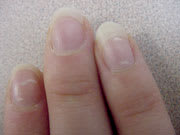
Leukonychia. These marks are common, nonuniform, white lines found in differing spots on one or more nails. They should not be confused with Mees’ and Muehrcke’s lines, which parallel the lunula across the entire nail bed and occur in more than one nail.
Longitudinal Linear Lesions
Longitudinal pigmented bands are normal findings in the nails of dark-skinned persons, occurring in more than 77 percent of blacks older than 20 years.9 These findings present a diagnostic problem because they must be differentiated from subungual melanomas (Figure 8), which also occur in older age groups and constitute 50 percent of melanomas in dark-skinned populations. Table 2 outlines factors that increase the likelihood of melanoma in individual patients.15,16 Nail symptoms in patients with increased likelihood should be considered melanoma until proved otherwise by biopsy. Proper technique for punch biopsy was discussed recently in this journal.17
FIGURE 8
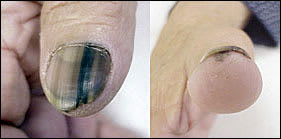
Longitudinal melanotic bands. (Left) Common in dark-skinned persons, when these bands are accompanied by pigmentation of underlying skin and disruption of nail growth (right), affected patients should undergo biopsy to rule out melanoma.
TABLE 2 Factors Increasing the Likelihood of Melanoma in a Patient Who Has a Nail with Longitudinal Pigmented Bands
| New longitudinal band in a light-skinned person |
| Sudden change in appearance of band (e.g., proximally wider, darker, blurred border) |
| Single-nail involvement (especially thumb, index finger, or great toe) |
| Pigmentation of the skin of the nail fold or proximal nail bed (i.e., Hutchinson’s sign) |
| New pigmentation in older persons (i.e., 60 to 79 years of age) |
| Band width of more than 3 mm |
| Family history of melanoma or dysplastic nevi |
| Abnormal nail structure (i.e., destruction or disruption of the nail plate) |
Longitudinal striations are accentuated ridges in the nail surface that can occur as a normal part of the aging process. If nails become thin and lusterless (i.e., sandpapered appearance), the condition may be referred to as trachyonychia; when all of the nails are affected, the condition is called 20-nail dystrophy. In this situation, associated conditions, including alopecia areata, psoriasis, atopic dermatitis, and lichen planus, must be considered.18 Trachyonychia also may be seen in patients with vitiligo.19
Nail Bed and Vascular Changes
Splinter hemorrhages are longitudinal thin lines, red or brown in color, that occur beneath the nail plate. They are visible when capillaries within the epidermal ridges leak (Figure 5). While splinter hemorrhages may denote benign problems such as local trauma, psoriasis, or localized fungal infection, they are a classic finding in patients with endocarditis (Figure 9).
FIGURE 9
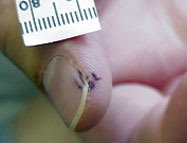
Splinter hemorrhage and Janeway’s lesions. These findings should stimulate a work-up for endocarditis.
Splinter hemorrhages are thought to be a more specific indicator of endocarditis if they are present proximally rather than distally on the nail plate, and they are more common in subacute than acute infection.20 However, splinter hemorrhages occur in only about 15 percent of patients with endocarditis and may be present in up to 20 percent of persons without endocarditis.21 Many other diseases can cause a similar appearance (Table 1). The causes of splinter hemorrhage are so varied and common that their usefulness as an isolated sign of illness has been questioned,7 except when they are accompanied by fever, Roth’s spots, Osler’s nodes, Janeway’s lesions (Figure 9), or a murmur, any of which would greatly increase their significance.
Examination of the capillaries at the eponychium normally shows an orderly array of parallel vessels. In patients with rheumatoid arthritis, systemic lupus erythematosus, dermatomyositis, or scleroderma, examination of the eponychium with a magnifying glass may show irregular, twisted, and dilated vessels (Figure 10). These attributes give the area an injected, erythematous appearance when viewed with the naked eye.
FIGURE 10
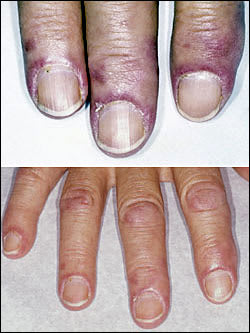
Dermatomyositis. (Top) Twisted and dilated capillaries just proximal to the cuticle give a blush to the skin of the eponychium and may signal systemic lupus erythematosus, dermatomyositis, or scleroderma. (Bottom) The blush and the pathognomonic finding of Gottron’s papules (i.e., thickened skin over the interphalangeal joints) indicate a diagnosis of dermatomyositis.
Changes in the color of the lunula can be revealing. In patients with Wilson’s disease (hepatolenticular degeneration), the area takes on a blue coloration, a phenomenon called azure lunula. Heart failure can turn the lunula red, and tetracycline therapy can turn it yellow. Silver poisoning will turn the nail itself a blue-gray color. Excessive fluoride ingestion can turn nails brown or black.
In patients with Terry’s nails, most of the nail plate turns white with the appearance of ground glass, and the lunula is obliterated.22 The condition may occur on only one finger, but more commonly all fingers are affected. This condition was described originally in relation to severe liver disease, usually cirrhosis, with 80 percent of these patients having Terry’s nails.13 Subsequently, in another study,23 25 percent of hospitalized patients with varied diseases were found to have Terry’s nails. The condition is thought to be caused by a decrease in vascularity and an increase in connective tissue in the nail bed.24
Similarly, in patients with chronic renal failure, increased melanin production may cause the distal part of the nail bed to turn brown. In patients with severe renal disease, the proximal portion of the nail bed can turn white, obliterating the lunula and giving a half-brown, half-white appearance, also called half-and-half nails (Figure 11).
FIGURE 11
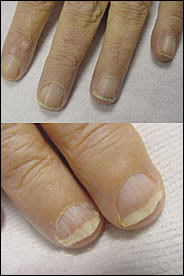
Half-and-half nails. (Top) This condition, with the lunula obliterated, the proximal nail turned white, and the distal nail turned brown, can occur in patients with renal failure. (Bottom) This patient, who has chronic renal failure, shows half-and-half nails, as well as straightening of the distal nail bed as a result of onycholysis.
Patients rarely present with complaints related to the appearance of their nails. Therefore, it is necessary for the physician not only to be familiar with common nail findings, but also to inspect nails carefully during physical examinations. Nail findings may provide important clues to the diagnosis of systemic illness, limit the differential diagnosis, and focus further work-up.

