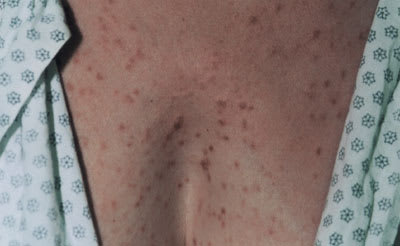
A 50-year-old white woman presented with a rash that first erupted on her trunk three years earlier and never fully cleared (see accompanying figure). The lesions became pruritic after a warm shower or strenuous physical exercise, but were otherwise asymptomatic. Physical examination revealed many discrete erythematous papules spread over the abdomen, upper chest, and back. On vigorous rubbing of a papule, a wheal formed at the site. The patient did not have hepatosplenomegaly, gastrointestinal complaints, or any palpable lymphadenopathy.
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Lichen planus.
B. Pityriasis rosea.
C. Scabies.
D. Urticaria.
E. Urticaria pigmentosa.
Discussion
The answer is E: urticaria pigmentosa. Biopsy of a skin lesion revealed superficial infiltrates of mononuclear cells and some eosinophils. The mononuclear cells stained strongly for tryptase, which confirmed the diagnosis of urticaria pigmentosa. The patient was given hydroxyzine for pruritus and referred to a hematologist for further testing.
Urticaria pigmentosa is part of a group of disorders that shares an abnormal growth of mast cells, termed mastocytosis. With urticaria pigmentosa, a type of cutaneous mastocytosis, abnormal mast cell accumulation is limited to the skin. In contrast, systemic mastocytosis affects not only the skin, but also may involve the liver, spleen, lymph nodes, gastrointestinal tract, and bone marrow.
Because mast cells often are missed using conventional staining, special stains must be ordered when mastocytosis is suspected. These include the metachromatic stains (e.g., toluidine blue O) or enzymatic stains (e.g., chloroacetate esterase).
Urticaria pigmentosa is the most common form of mastocytosis. Approximately one half of cases occur before six months of age, and another one fourth before puberty.1 Onset of urticaria pigmentosa in adulthood, such as occurred with this patient, is less common. Accumulation of mast cells in organs other than the skin occurs primarily in adults.
Mast cell degranulation with hormone release and direct organ infiltration lead to the symptoms seen with systemic mastocytosis. Histamine-induced hypersecretion may cause gastritis, peptic ulcers, and diarrhea, and ultimately, malabsorption may occur. Other histamine-induced symptoms include pruritus, urticaria, bronchoconstriction, and vasopermeability (possibly leading to vascular collapse). Release of prostaglandins may cause skin flushing, intestinal cramping, and cardiovascular abnormalities (e.g., tachycardia, vascular collapse).
Adults with urticaria pigmentosa should undergo bone marrow biopsy to look for evidence of systemic mastocytosis.2 In addition, serum tryptase levels greater than 20 ng per mL suggest systemic involvement.
The most common symptom in urticaria pigmentosa is pruritus, which may be treated with H1-receptor antagonists. Inhibitors of mast cell degranulation, such as cromolyn and ketotifen, have been found to have a moderate effect on pruritus, whealing, and flushing. Finally, some patients may benefit from topical corticosteroids or psoralens and ultraviolet A (PUVA) therapy.
Adults with urticaria pigmentosa usually progress slowly to systemic disease, but rarely develop hematologic disease. Clinical factors associated with poor prognosis include anemia, hypercellular bone marrow, cytologic atypia, hepatosplenomegaly, and an associated hematologic disorder.3
Lichen planus also is a pruritic, often chronic, rash, but the lesions are typically flat-topped, violaceous papules with scale. They usually are less widespread than urticaria pigmentosa and would not wheal when rubbed.
Pityriasis rosea may lead to a truncal macular rash, sometimes with pruritus. The eruption may last up to two or three months, but not years. In addition to many small macules, a large patch (i.e., herald patch) may be seen.
Scabies, a contagious skin infestation caused by a mite, is typically highly pruritic. Skin lesions may be widespread but tend to cluster in the intertriginous areas, such as the axilla, groin, inframammary area, and finger webs.
Urticaria typically presents with larger areas of erythema, but also may occur as small erythematous papules. Unlike urticaria pigmentosa, individual urticarial skin lesions wax and wane over a course of hours and would not persist in the same location as chronic papules.

