Primary care physicians must be able to recognize wrist and hand injuries that require immediate attention. A complete history and physical examination, including assessment of distal limb function, are essential. Hemorrhage control is necessary in patients with vessel lacerations and amputations. Amputations require an understanding of the indications and contraindications in the management of the amputated limb. High-pressure injection injuries and compartment syndromes require a high index of suspicion for early recognition. Infectious entities include “fight bite,” open fractures, purulent tenosynovitis, animal bites, and retained foreign bodies. Tendon disruptions should be recognized early to optimize management.
Although some severe hand injuries seem obvious, a thorough evaluation is needed to detect other, more subtle injuries. Failure to diagnose, manage, and rehabilitate hand injuries has the potential to result in permanent disability.1 Part two of this two-part article focuses on the emergent evaluation of hand and wrist injuries. Part one2 addresses management evaluation of hand and wrist injuries.
Physicians must be able to evaluate, triage, and stabilize emergent hand injuries before obtaining surgical consultation. Assessment of distal limb function and a complete history and physical examination are important before addressing the injury.
Vessel Laceration
Completely transected digital vessels usually retract, constrict, and clot; partial transections may continue to hemorrhage and result in traumatic aneurysm.3(pp1–18) To avoid further damage to arteries or other nearby structures, lacerated vessels should not be clamped3(pp1–18); instead, direct pressure or approximal limb tourniquet application should be considered.
FIGURE 1.
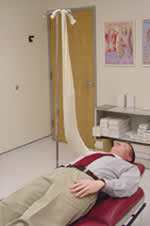
A six-foot cast stockinette used to elevate the arm and control hemorrhage. The stockinette is cut in half at each end. One end is tied around the patient, and the other is tied to a support.
The simplest method for controlling hemorrhage is to apply direct pressure to the wound for 10 to 15 minutes with sterile, semicompressible material. After hemorrhaging is controlled, the limb is elevated above the heart, and the wound is wrapped with an elastic bandage tightly enough to hold the material in place and control bleeding. With wounds in the proximal arm, the compressive bandage should be wrapped beginning at the hand and arm distal to the injury. A stockinette can be used to elevate the arm and stabilize the wound4,5 (Figure 1).
TABLE 1 Indications and Contraindications for Attempted Reattachment of an Amputated Finger or Hand
| Indications | Relative contraindications | Absolute contraindications |
| Amputations occurring in children Clean amputations of the hand, wrist, or distal forearm Multiple digit injury (amputated digit with other digits partially severed) Thumb amputations | Amputations that are due to severe crush or avulsion injuries Heavily contaminated amputations Patient has a significant smoking history Single amputations between the metacarpal and proximal phalangeal joints, especially border digits (index and fifth fingers) in adults | Life-threatening medical problem or injury that pre-cludes surgery or transfer Patient refusal to fully abstain from smoking for three months post-implantation Psychiatric patient who has intentionally self-amputated the extremity Severe multilevel injury of the amputated part |
Information from reference 6.
If heavy bleeding persists despite direct pressure, an air-inflated arm tourniquet may be used. This device resembles a blood pressure cuff and is used during upper extremity surgery. Alternatively, an inflated blood pressure cuff secured externally with cast padding to prevent unwrapping is effective. Before the cuff is inflated, the arm is exsanguinated by elevation and distal-to-proximal centrifugal wrapping. Tourniquet pressure should be 250 mm Hg in adults and 100 to 200 mm Hg in children.3(pp10–18) The cuff tubes are clamped with hemostats to maintain pressure, and the wrapping is removed. An ischemic hand can withstand lack of arterial flow for 90 to 120 minutes.3(pp10–18) The use of tourniquets fashioned at the scene of the injury (e.g., belts, cloths) is discouraged because their narrow width often causes neurovascular injury. Emergent consultation with a hand or vascular surgeon is required.3(pp10–18)
Amputations
Table 16 lists indications and contraindications for finger and hand replantation. A replant surgeon should be consulted when replantation is considered, but reattachment never should be guaranteed to patients.6
The health care team should assign some staff members to tend to the amputated part while others attend to the patient. The wound is gently cleansed and irrigated with sterile saline. The residual limb is dressed with nonadherent petroleum gauze and covered with a dry, sterile compression bandage. An intravenous line is inserted for hydration and administration of medication. Appropriate tetanus prophylaxis is administered (Table 2).7 Analgesics may be given, but the patient must remain able to communicate with the replant surgeon.3(pp44–61)
The amputated limb is gently cleansed, and the wound surface is irrigated with saline or lactated Ringer's solution. The limb should not be submerged in any type of liquid or manipulated any more than is necessary. It is wrapped in nonadherent petroleum gauze, moistened with saline or lactated Ringer's solution, and put in a sterile container or tied-off plastic bag. The container or bag is put into a larger container of ice and water.3(pp44–61)
The initial management of incompletely amputated but devascularized limbs is more difficult. Manipulation must be kept to a minimum. The wound is gently cleansed and dressed. If the injured limb has been rotated, it is gently realigned and splinted to avoid kinking or tourniqueting. Well-insulated water packs are placed around the limb to keep it cool. As soon as the patient is stabilized, the replant surgeon should be contacted. No tissue or devascularized limb—no matter how damaged—should be discarded without first consulting with the replant surgeon, because these tissues may be harvested for grafting to the residual limb.3(pp44–61)
High-Pressure Injection Injuries
High-pressure injection injuries, often caused by spray or paint guns,8 usually involve the nondominant index finger.9(pp373–9) Nozzle pressures may reach 10,000 psi10; hence, contact with the nozzle is not necessary to incur serious injury.
The patient may present with numbness or burning, as well as pain and swelling increasing over time. The wound may appear deceptively benign, resembling a small puncture. The presence of crepitus indicates subcutaneous emphysema.
Severity depends on the wound's location and the substance injected. Material injected on the volar (palmar) aspect of the hand at the interphalangeal (IP) joint creases usually penetrates the thenar membrane sheath and enters the intrasynovial space, and possibly the midpalmar space. Injections between creases are more likely to result in superficial wounds, although they may spread circumferentially around the finger, affecting the neurovascular bundle. Paint solvents produce intense inflammatory responses, while grease and hydraulic fluid produce fibrosis with chronic effects.10
Although rare, Staphylococcus aureus is the most common cause of secondary infection, and therapy with a first-generation cephalosporin and an aminoglycoside is recommended.11,12 Because some injected substances are hepatotoxic and cause hematuria, liver studies and monitoring of blood, urea, nitrogen and creatinine levels are recommended.10
If patients with high-pressure injection injuries are not immediately identified and surgically treated, their injuries may be catastrophic.8 Injections inflicted at 2,000 psi or greater have a 50 percent amputation rate, and injections inflicted at less than 2,000 psi have a 40 percent or lower amputation rate.13 Because many injected substances are radiopaque, radiographs may help quantify the extent of the injury.14 High-pressure injection injuries require immediate surgical consultation.
TABLE 2 Tetanus Prophylaxis in Persons 7 Years and Older
| History of absorbed tetanus toxoid vaccinations | Clean, minor wounds | All other wounds |
|---|---|---|
| Unknown or fewer than three doses | Td | Td and TIG |
| Three or more doses* | No prophylaxis † | No prophylaxis ‡ |
Td = tetanus and diphtheria toxoid; TIG = human tetanus immune globulin.
*—If only three doses of fluid toxoid have been received, a fourth dose of toxoid (preferably an absorbed toxoid) should be given.
†—If more than 10 years since last dose, Td should be given.
‡—If more than five years since last dose, Td should be given.
Adapted from Centers for Disease Control and Prevention. Diphtheria, tetanus, and pertussis: recommendations for vaccine use and other preventive measures: recommendations of the Immunization Practices Advisory Committee (ACIP). Accessed online on March 29, 2004, at:http://www.cdc.gov/mmwr/preview/mmwrhtml/00041645.htm#00001676.htm.
Compartment Syndrome
The forearm has three compartments: the volar and dorsal compartments and the mobile wad. The volar compartment includes forearm wrist flexors, pronator tendons, and median and ulnar nerves and arteries. The dorsal compartment includes wrist and finger extensor tendons. The mobile wad contains only muscle. The hand has 10 compartments: the hypothenar and thenar compartments, adductor pollicis, four dorsal interossei, and three volar interossei.
Acute upper extremity compartment syndrome is a rare, disastrous injury resulting from compromised circulation caused by increased pressure within a closed fascial space.15 Increased pressure may result from external compression (e.g., an unconscious patient lying on his or her arm for a prolonged time), circumferential pressure (e.g., a cast or burn eschar), and increased volume within the compartment secondary to edema or hematoma.
Anatomic variations of the hand, multiple compartment involvement, the presence of other injuries, or an obtunded patient make it difficult to predict physical findings of compartment syndrome.16 Paresthesia and pain disproportionate to the injury or increasing levels of pain following treatment are initial indicators that should alert the physician to the possibility of compartment syndrome. The “6 Ps” (i.e., pain, pressure, paresthesia, paresis, pallor, and pulselessness) should be assessed.15 Pressure refers to increased tension on palpation of the extremity. Paresthesia is an important early sensitive sign but lacks specificity. Paresis and pallor appear very late, and pulselessness, usually the last sign to appear, may be present early in patients with injury to major arteries17 By the time all six symptoms manifest, the patient has been irreparably harmed. Dorsal and mobile wad compartment syndrome may not present with the classic signs. Hence, compartment syndrome is diagnosed on the basis of a high degree of clinical suspicion.17 A swollen hand, tense on palpation, in an intrinsic minimus position (i.e., extension of the metacarpophalangeal [MCP] joints and flexion of the IP joints) strongly indicates this condition.18
TABLE 3 Antibiotic Prophylaxis for Hand Injuries
| Clinical situation | Antibiotic prophylaxis |
|---|---|
| Low-risk, traumatic injuries (clean wounds with easily demarcated borders, no devitalized tissue) | None |
| Injuries in immunocompromised patients (e.g., patients with human immunodeficiency virus infection, diabetes) | Gram-positive cocci coverage |
| Wounds with devitalized tissue | Gram-positive cocci coverage if wound tendon or joint space is contaminated* |
| Animal and human bites (other than superficial abrasions) | First-generation cephalosporin. In patients with bites that may contain Pasteurella multocida or Eikenella corrodens, consider penicillin or amoxicillin-clavulanate potassium (Augmentin). In immunocompromised patients, consider erythromycin or amoxicillin-clavulanate. In patients with sepsis and petechial rash, consider intravenous ciprofloxacin (Cipro) and clindamycin (Cleocin).† |
| Puncture wounds | Case-by-case decision |
*—If the wound is contaminated, débridement is required.
†—Patients with sepsis or petechial rash should be hospitalized.
Information from reference 11.
An emergent surgical consult is necessary when considering this diagnosis.17 Compartment pressure measurement is recommended for diagnosis. Pressures of 15 to 25 mm Hg, or greater than 25 mm Hg in the absence of clinical signs and symptoms, are indicative of compartment syndrome.18 Two methods are used to measure compartment pressure: a pressure monitor; or an 18-gauge needle, stopcock, and blood pressure sphygmomanometer (the latter method may be less accurate). Because training, asepsis, and a detailed knowledge of compartments are required to use these methods, compartment pressure measurement is best left to the surgeon.
Fight Bite
A clenched fist injury that occurs when one person strikes another person's mouth is referred to as a “fight bite.” This is a serious injury with an annual estimated incidence of 11.8 per 100,000 persons.19 A tooth typically penetrates the dorsum of the hand over the third MCP joint. Although initial findings may reveal a small, seemingly innocuous puncture, the penetration often injures the soft tissue, extensor tendon, and sheath, and may disrupt the MCP joint.
Radiographs are recommended to exclude foreign bodies, identify fractures, and assess possible soft tissue damage.20 Staphylococcus and Streptococcus bacteria frequently are cultured from these injuries.21 [Strength of recommendation C, case series] Recommended antibiotic prophylaxis includes a first-generation cephalosporin, and amoxicillin-clavulanate potassium (Augmentin) (Table 3).11 [Strength of recommendation C, consensus guideline]
The wound should be irrigated and covered. Surgical intervention with irrigation and debridement vastly improves prognosis. Although wound exploration and treatment in the operating room are recommended, they may be unnecessary if deep structures have not been penetrated.20 A hand surgeon should be consulted immediately.
Open Fractures
Open fractures are surgical emergencies, constitute incomplete amputations, and may present subtly or as full-blown emergencies. Fracture of the distal aspect of the fifth metacarpal is a relatively common presentation. Fight bite should be discounted.12 [Strength of recommendation C, consensus guideline]
The patient should be hemodynamically stabilized, the wound covered with sterile saline dressings, and intravenous antibiotics administered; most protocols recommend a first-generation cephalosporin and, for highly contaminated wounds, an aminoglycoside. If contamination by anaerobic organisms (e.g., Clostridium) is suspected, high-dosage penicillin is added.22 Radiographs should be taken after neurovascular function is evaluated.
Trauma protocols preserve, in order, life, limb, and function; therefore, sophisticated protocols for open fracture management may result in salvaged but nonfunctional extremities.11 [Strength of recommendation C, consensus guideline] These wounds require surgery, and consultation with a hand surgeon should be obtained immediately.
Purulent Tenosynovitis
Diagnosis of purulent tenosynovitis, associated with skin tears and tendon sheath contamination on the digit's palmar side, is based on suspicion in the presence of Kanavel's cardinal signs,4 although the signs may present variably: slight digital flexion, uniform volar swelling, flexor tendon sheath tenderness, or pain on passive extension. The clinical diagnosis may be substantiated with diagnostic ultrasonography. This condition often is associated with streptococcal or staphylococcal infections and sometimes presents as a benign puncture.20 Emergent consultation for drainage and antibiotic treatment should be obtained.
Thenar and Midpalmar Infections
Although it is uncommon, swelling in the thenar or midpalmar spaces of the hand suggests an infectious etiology. Usual signs include redness, tenderness, and eventual fluctuation. The dorsum may swell more than the palm.9(pp201–13) These infections and purulent tenosynovitis are treated just like fight bites, with urgent consultation for drainage and antibiotic coverage.
FIGURE 2.
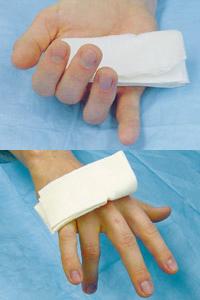
Typical hand and finger positions in patients with tendon injuries. (Top) Flexor tendon rupture. (Bottom) Extensor tendon rupture.
Tendon Injuries
Flexor tendon injuries almost always result from lacerations and usually involve concomitant injury to adjacent structures. Rupture of the flexor tendons also occurs, particularly in the sports setting. When treated within several days of injury, isolated flexor tendon injuries are well tolerated, although some loss of function should be anticipated. The timeframe for definitive treatment is at the discretion of the consulting surgeon.22(pp2674–86) Undiagnosed digital flexor tendon injuries may result in serious disability.
Flexor tendon disruption is indicated by one finger lying in complete extension while others are in slight (10 degree) flexion at IP joints (Figure 2, top). These injuries should not be probed or clamped.
The superficialis and profundus tendons should be tested independently, with the patient actively flexing individual proximal and distal IP joints. Gently pressing the fingertip of each digit reveals loss of normal tension in fingers with injured flexor tendons.22(p3,424) Flexor digitorum superficialis tendon function may be tested without influence by the flexor digitorum profundus in the following manner: hold the two adjacent fingers in maximal extension, anchor the affected finger's distal IP joint in extension, and tell the patient to flex the affected proximal IP joint. This is not possible in patients with a completely severed superficialis tendon.
To differentiate the index finger flexor digitorum profundus, the patient is told to pinch and pull a sheet of paper with each hand using the index fingers. If the superficialis tendon is injured, the distal IP joint will hyperflex, and the proximal IP joint will hyperextend. The finger with an intact superficialis tendon will allow hyperextension of the distal IP joint so that the maximal pulp of the finger stays in contact with the paper.
To assess the flexor pollicis longus, the MCP joint of the thumb is held in extension while the patient flexes the IP joint. If a tendon laceration occurs at the wrist, the fingers still may be able to flex, and a definitive diagnosis of flexor tendon transection is not possible.22(p3,435) Extensor tendon disruption can be ascertained by observing the hand in a resting position. The finger with a disrupted extensor tendon may rest in a flexed position compared with the other digits (Figure 2, bottom). The patient should be asked to extend the affected digit against resistance.22(pp3,399–423)
Depending on their training and experience, family physicians may be able to repair extensor tendon injuries. Familiarity with suturing techniques and rehabilitation protocols is essential. If referral is necessary, the physician's principal responsibilities are accurate diagnosis and complete description of the injury.3(pp29–43),17
Primary coverage of the injured tendon by skin suturing after wound irrigation protects the tendon and retards infection but should be undertaken only after consulting with the physician who will perform the definitive repair. Dressing the wound, usually with four layers, and transporting patients with tendon injuries are important aspects of care.3(pp29–43)
The first layer of dressing, petroleum-impregnated gauze, is applied after cleaning and irrigating the hand (complete immersion is not recommended) and blotting it dry. Petroleum-impregnated gauze prevents wound adherence to the bandage. Because this layer should permit passage of fluid, impermeable dressings are not recommended.
The second layer is composed of non–cotton-filled gauze soaked in normal saline or Ringer's solution. Soaked gauze conforms to the contour of the hand and permits blood and other tissue outside the wound to escape, thereby preventing hematoma or seroma accumulation. Avoid “sloppy” wet dressings by wringing out excess moisture before application.
The third layer is made up of gauze “fluff” and sponges for extra padding. Placing gauze between the fingers prevents maceration, but the gauze should not be packed. A loose circumferential wrap using additional 2 × 2-inch fluff gauze completes this layer.3(pp29–43)
The outer dressing is composed of a single layer of cast padding with a fiberglass or plaster splint, if necessary.
Retained Foreign Bodies and Puncture Wounds
A patient's perception of a foreign body in a wound often is correct.23 [Strength of recommendation B, single diagnostic study] Sharp, localized pain on palpation and a detailed history about the injury are important to diagnosing retained foreign bodies in puncture wounds.
Although infection is the most common complication of retained foreign bodies, the use of prophylactic antibiotics remains controversial. Most protocols recommend a first-generation cephalosporin with an aminoglycoside for highly contaminated wounds.22,24 However, recent evidence fails to support this practice.12 [Strength of recommendation B, systematic review of poor-quality clinical trials] Tetanus prophylaxis is warranted for patients with these injuries.
Lacking clinical evidence, most authorities recommend irrigating wounds with normal saline at pressures of 5 to 8 psi to flush as much organic material, clothing, sand, and chemicals as possible from the wound. Additives such as povidoneiodine (Betadine), antibiotics, and surfactants are not recommended.22
Before removing foreign bodies, their size, location, and composition, and the mechanical and inflammatory effects of removal must be considered. Small, metal objects deeply embedded in soft tissue pose a lower risk for complication than even superficially embedded organic material, such as wood.
Underpenetrated radiographs are the most readily available method to for assessing wounds for retained foreign bodies. Metal, bone, teeth, pencil graphite, certain plastics, glass, gravel, stone, some fish spines, wood, and aluminum are visible in plain radiographs.25 Computed tomographic (CT) scanning is 100 times more sensitive in differentiating densities than plain radiography.26 However, CT scanning should be reserved for difficult cases when radiographs fail to show a foreign body, or the patient is at high risk for infection or joint involvement.11 Ultrasonographic sensitivity to foreign bodies ranges from 50 to 90 percent, and specificity ranges from 70 to 90 percent.27 Magnetic resonance imaging has not been assessed in this regard.27
A number of foreign-body removal techniques are described but should not be attempted by inexperienced physicians.24 Unless removal can be accomplished in a controlled, sterile environment while maintaining hemostasis, urgent referral to a hand surgeon is indicated.
TABLE 4 Irrigation Protocol in Uncomplicated Puncture Wounds from Animal Bites
| Inject a 1 percent lidocaine (Xylocaine) solution through intact skin, not in the wound. |
| Place a rubber mat or waterproof barrier beneath the patient to collect fluid. |
| Administer 500 mL of saline in an IV bag connected to tubing and a 20-gauge angiocatheter. |
| Insert the IV bag into a blood pressure cuff and pump to 300 mm Hg. Irrigate wound, using all of the saline. |
| As an alternative irrigation method, gas-sterilize a hand-squeeze spray bottle that allows a concentrated stream. Irrigate with 500 mL of sterile saline. |
| Explore wounds with fine-tissue scissors; excise skin, devitalized tissue, and fat globules from wound edges. |
| Apply dressing. |
| Start a seven-day course of appropriate antibiotics and re-evaluate patient in eight to 12 hours. Follow closely for signs of increased redness, swelling, or pain. |
IV = intravenous.
Information from reference 28.
Animal Bites
Deep puncture wounds from animal bites become morbid if not promptly tended and closely followed.28 Dog bites cause approximately 0.4 percent of emergency department visits and account for 60 to 90 percent of treated bite injuries.29 Cat bites account for 1 to 15 percent of treated bites.29
A dog's jaws generate forces up to 200 psi, although, unlike cats, their teeth generally are not sharp. Dog bites may be crushing and superficial, while cat bites resemble punctures.29 The use of antibiotics in patients with animal bites is controversial, and some studies have shown little benefit.30–32 [Strength of recommendation B, inconsistent randomized trials] However, bites at higher risk for infection, such as those on the hands or extremities, should be treated with antibiotics.11 [Strength of recommendation C, consensus guidelines]
More than 100 different organisms have been isolated from dog bites, including Staphylococcus, Streptococcus, Capnocytophaga canimorsus, Klebsiella, Bacillus subtilis, Pseudomonas, and Enterobacteriaceae. Some, such as Pasteurella multocida, are slightly infectious, while others, such as C. canimorsus, may cause serious complications, including hypotension, disseminated intravascular coagulation, and renal failure. Penicillin or amoxicillin-clavulanate potassium is recommended for use in nonallergic patients with dog bites. Clindamycin (Cleocin), erythromycin, or azithromycin (Zithromax) may be used in patients who are allergic to penicillins.12,29
Cat bites likely will cause infection.29 P. multocida, staphylococcal, and streptococcal infections are common in patients with cat bites. Amoxicillin-clavulanate potassium and second-generation cephalosporins are recommended for prophylaxis and infection treatment.12,29
The affected extremity should be elevated, and ice should be applied to reduce swelling. The history should include reconstruction of the bite incident; review of drug, alcohol, and steroid use; diabetes and tetanus status; and whether the patient is asplenic. The skin should be cleansed but not shaved, and radiographs should be obtained as indicated by the history and physical examination. (If rabies is a concern, scrub the wound with soap and water, then rinse.20) When rabies is not a concern, anesthetize the wound and irrigate with normal saline; Table 428 describes an irrigating treatment protocol using readily available equipment. The physician should explore and débride the wound, although puncture wounds should not be probed. Generally, animal bites to the extremities should not be sutured. The physician should consult a surgeon if tendon, bone, or compartment injury is suspected.29

