Patients with chronic cough should avoid exposure to irritants that can trigger cough, and those who smoke should stop smoking. Patients who develop chronic cough in association with angiotensin-converting enzyme inhibitor therapy should be switched to an agent from another drug class. If cough persists, a chest radiograph should be ordered to rule out malignancy and other serious conditions. Postnasal drip syndrome, asthma, and gastroesophageal reflux disease are the most likely causes of chronic cough in adults. If postnasal drip syndrome is suspected, a trial of a decongestant and a first-generation antihistamine is warranted. Pulmonary function testing with a methacholine challenge is the preferred test for confirming the diagnosis of asthma. Gastroesophageal reflux disease usually is diagnosed based on the symptoms and after a trial of therapy. If the cause of chronic cough remains unclear, high-resolution computed tomographic scanning of the chest, bronchoscopy, and referral to a pulmonary specialist may be indicated. The approach to diagnosing chronic cough in immunocompromised patients and children is similar to the approach in immunocompetent adults. However, a CD4+ cell count can help determine the potential for opportunistic infections in immunocompromised patients. Respiratory tract infections, asthma, and gastroesophageal reflux disease are the most common causes of chronic cough in children. Foreign body aspiration should be considered in young children. Congenital conditions, cystic fibrosis, and immune disorders are possible diagnoses in children with chronic cough and recurrent infection.
Chronic cough is a common reason for physician visits in the United States and other industrialized nations.1–3 However, some patients with chronic cough fail to seek medical attention because of lack of concern or denial. This article presents a systematic, evidence-based approach to the evaluation of chronic cough. The approach is based on the results of prospective studies and an evidence-based practice guideline.1
Pathophysiology
Cough is important because it clears foreign objects and secretions from the respiratory tract. Unfortunately, it also can transmit disease via droplets and the contamination of objects.
The cough reflex is complex. Although some evidence suggests the presence of a cough center in the medulla, cough generally results from irritant stimulation of one or more receptors in the respiratory system.1
For a cough to be effective in removing mucus and foreign objects from the airways, high intrathoracic pressures and airflow must be achieved. These high pressures are thought to contribute to the discomfort associated with coughing.1
Differential Diagnosis of Chronic Cough
Cough may be characterized as acute (lasting less than three weeks), subacute (lasting three to eight weeks), or chronic (persisting beyond eight weeks).2 Acute cough may develop because of viral upper respiratory tract infection (the most common cause), acute bacterial sinusitis, exacerbation of chronic obstructive pulmonary disease (COPD), allergic rhinitis, and environmental exposure.2
Subacute cough most often results from bacterial sinusitis or asthma; it also can occur after an infection (i.e., upper respiratory tract infection not accompanied by pneumonia).2,3 Subacute cough resolves without treatment. Pertussis may be acute or subacute.2
Chronic cough can have many causes, but only a few diseases account for most cases2,4 (Table 1).1,2,5–7 In adults, postnasal drip syndrome, asthma, and gastroesophageal reflux disease (GERD) are the most common causes and have been referred to as a “pathogenic triad of chronic cough.”5(p284) This disease triad accounts for nearly all cases of chronic cough in nonsmokers who have essentially normal chest radiographs and are not taking an angiotensin-converting enzyme (ACE) inhibitor.1,4 Chronic cough is found to have two or more causes in 18 to 62 percent of patients, and three causes in up to 42 percent of patients.1,3
TABLE 1 Causes of Cough in Adults and Children
| Age group | Common causes | Less common causes | Uncommon causes |
|---|---|---|---|
| Adults | Angiotensin-converting enzyme inhibitors Asthma Bronchitis Gastroesophageal reflux disease Postnasal drip syndrome Smoking and other irritants | Bronchiectasis Eosinophilic bronchitis Postinfectious | Aspiration Bronchogenic carcinoma Carcinomatosis Irritable larynx Lymphoma Persistent pneumonia Psychogenic cough Pulmonary abscess Sarcoidosis Tuberculosis |
| Children | Asthma Gastroesophageal reflux disease Upper and lower respiratory tract infections | Foreign body (young children) | Aspiration Congenital abnormality or disorder Cystic fibrosis Environmental exposures Immunologic disorder Primary ciliary dyskinesia Psychogenic cough Tourette’s syndrome Tuberculosis |
Evaluating Immunocompetent Adults
The evaluation of chronic cough should begin with a thorough medical history and a focused physical examination. If the history reveals tobacco smoking, the patient should be instructed to quit smoking. If the history reveals environmental exposures, the patient should be instructed to avoid the triggering substances. If the patient is taking a medication that is known to cause cough, the patient should be switched to another agent.
ACE inhibitors cause a nonproductive cough in 5 to 20 percent of persons (more often women than men). This side effect is not dose related, and the cough may begin one week to several months after ACE inhibitor therapy is initiated. The cough should subside in a few days to several weeks after the ACE inhibitor is stopped.1,8
If a patient is not taking an ACE inhibitor and chronic cough persists, a chest radiograph should be obtained. A chest radiograph is not required in pregnant women and is optional in the initial evaluation of younger nonsmokers with suspected postnasal drip syndrome or sinusitis. A suggested sequential approach to the evaluation of the immunocompetent patient with chronic cough is provided in Figure 1.1
ABNORMAL CHEST RADIOGRAPH
If the chest radiograph reveals abnormalities, further studies may be indicated. Possible studies include computed tomographic (CT) scanning of the chest, pulmonary function tests, barium esophagography, cardiac studies, and bronchoscopy.2 Referral to a pulmonologist may be required to obtain a definitive diagnosis for lesions detected on the chest radiograph.
Bronchiectasis
This condition, which results in airflow limitation, is a less frequent cause of chronic cough. The predominant feature of bronchiectasis is overproduction of sputum.1,9 Symptoms include fever, pleurisy, and malodorous or blood-tinged sputum. Bronchiectasis should be considered when chronic cough produces sputum and hemoptysis. Although high-resolution CT scanning of the chest is the gold standard for diagnosing bronchiectasis, the chest radiograph is abnormal in up to 87 percent of patients with this condition.9
Bronchogenic Carcinoma
In a patient who smokes, CT scanning should be performed if the findings of the chest radiograph are suspicious for malignancy. The patient who has a normal chest radiograph but persistent symptoms and a negative evaluation for common causes of chronic cough should be reevaluated and considered for CT scanning of the chest or referral to a pulmonologist for bronchoscopy.
Bronchogenic carcinoma is a much less likely diagnosis in a patient who has never smoked. However, this cancer remains a valid concern in the patient with a cough that has lasted for several months and a history of current or previous cigarette smoking or exposure to industrial toxins, radon, or secondhand smoke.1,10–12 The physician should remember that bronchogenic carcinoma is largely asymptomatic in its early stages, and that the use of chest radiography or other routine screening in smokers is not recommended.13
NORMAL CHEST RADIOGRAPH
A normal chest radiograph usually excludes malignancy, bronchiectasis, persistent pneumonia, sarcoidosis, and tuberculosis.2 The next step is to consider the most likely remaining causes of chronic cough: postnasal drip syndrome, asthma, and GERD.2,5 The timing of the cough (i.e., whether it occurs with meals or is nocturnal) and its character (i.e., wet, dry, paroxysmal, or barking) are not predictive of the cause.4
The physician should keep in mind that chronic cough may fail to resolve because of incorrect diagnosis or incorrect or insufficient treatment. The cause of chronic cough frequently is determined only when a specific therapy eliminates the symptom.2,3
For the conditions discussed below, two weeks of therapy generally should be tried before the next most likely cause of chronic cough is considered.
Postnasal Drip Syndrome
This syndrome should be one of the first conditions considered. Alone or in association with some other condition, postnasal drip syndrome is the most common cause of chronic cough in non-smoking, immunocompetent adults who have a normal chest radiograph.
No signs or symptoms are specific to cough caused by postnasal drip syndrome; therefore, the diagnosis cannot be made based on the history and physical examination alone.1 Throat clearing and a “cobblestone” posterior pharynx are features that suggest the presence of postnasal drip syndrome, but these features also occur in other conditions. Furthermore, even when suggestive features are lacking (“silent” postnasal drip syndrome), a patient still may respond to appropriate treatment.2
Radiography of the sinuses may be useful when rhinitis and asthma have been ruled out as causes of chronic cough. The physician should keep in mind that although a normal sinus radiograph may well rule out sinusitis, only 57 to 81 percent of patients with an abnormal radiograph have sinusitis.
FIGURE 1 Evaluation of Chronic Cough
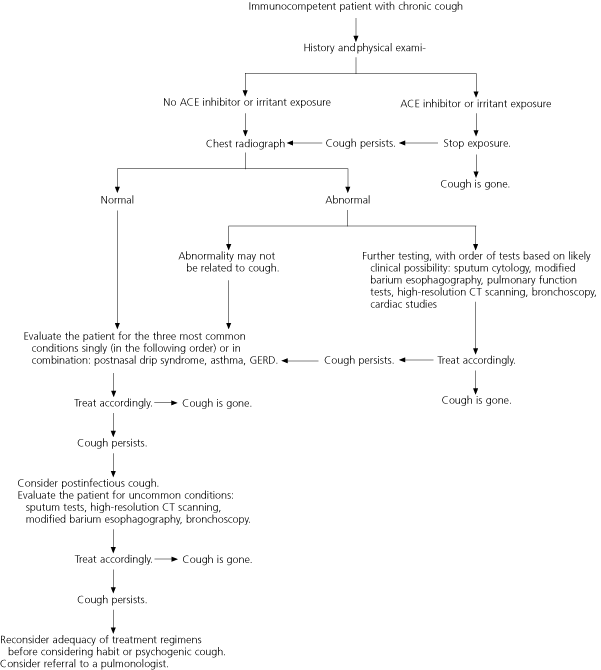
Sequential approach to the evaluation of chronic cough in the immunocompetent adult. (ACE = angiotensin-converting enzyme; GERD = gastroesophageal reflux disease; CT = computed tomography)
Adapted with permission from Irwin RS, Boulet LP, Cloutier MM, Fuller R, Gold PM, Hoffstein V, et al. Managing cough as a defense mechanism and as a symptom. A consensus panel report of the American College of Chest Physicians. Chest 1998;114(2 suppl managing):166S.
The diagnosis of postnasal drip syndrome often is made after a trial of therapy.2,9,14 Postnasal drip syndrome not caused by sinusitis consistently responds to the combination of a decongestant and a first-generation histamine-H1 antihistamine.1,3 The nonsedating H1 antihistamines are not as effective when postnasal drip is not mediated by histamine (e.g., nonallergic rhinitis).2,3,15
Asthma
After postnasal drip syndrome, asthma is the next most common cause of chronic cough in immunocompetent adults. If the patient is taking an antihistamine, the agent should be continued because the symptoms of allergic rhinitis and postnasal drip syndrome may cause confusion in determining whether chronic cough is caused by asthma.16
Coughing is the only manifestation of asthma (cough-variant asthma) in up to 57 percent of patients with the disease.2 Cough-variant asthma should be considered when persistent cough is exacerbated by cold or exercise, or when cough worsens at night.17 Airway hyperresponsiveness may suggest the diagnosis of cough-variant asthma.1 This disease responds to asthma medications such as bronchodilators and inhaled corticosteroids.2
A methacholine challenge test is recommended, because a negative result effectively rules out asthma.2 The disappearance of symptoms after treatment with systemic corticosteroids does not ensure the diagnosis of asthma, because eosinophilic bronchitis and other inflammatory conditions also improve with these medications.2
GERD
This disease is the third most common cause of chronic cough in nonsmoking, immunocompetent adults who have a normal chest radiograph. Although aspiration and irritation have been assumed to be the main causes of chronic cough in patients with GERD, it is more likely that a vagally mediated reflux mechanism is responsible.1,3 Heartburn and regurgitation suggest a GERD-induced chronic cough, but these features may be absent in “silent” GERD.2
The most sensitive and specific test for GERD is 24-hour esophageal pH monitoring.1 Because of the inconvenience of this test, it is not recommended in the routine evaluation of GERD.2 An alternative approach is the empiric use of antireflux medications such as proton pump inhibitors or histamine-H2 antihistamines.2,18 Patients diagnosed with GERD who do not respond to medical therapy may be candidates for surgery.1,19
Other Causes
Chronic bronchitis from exposure to cigarette smoke or other irritants is an important cause of chronic cough.2 Although chronic bronchitis is a relatively common cause of chronic cough, it accounts for only 5 percent of patients who present for evaluation and treatment, perhaps because many persons with “smoker’s cough” do not seek medical care.1 The initial treatment step is to eliminate tobacco smoke or other environmental irritants.1 In the absence of these irritants, sputum production and airway inflammation should decrease.
Although eosinophilic bronchitis only recently has been reported as a cause of chronic cough (airway inflammatory process), it has been found in 10 to 20 percent of patients evaluated in pulmonary medicine clinics.3,20 The presence and activation of eosinophils and metachromatic cells in the sputum differentiates eosinophilic bronchitis from classic chronic bronchitis; the lack of bronchial hyperresponsiveness differentiates it from asthma, which also may result in the presence of reactive cells in the sputum.3,20 Patients with eosinophilic bronchitis have normal spirometry results and respond to inhaled and systemic corticosteroids.2,20 Eosinophilic bronchitis usually can be ruled out if induced sputum contains insufficient eosinophils (less than 3 percent) or if corticosteroids fail to improve the cough.2,20,21
Postinfectious cough should be considered when cough persists after an upper respiratory tract infection. This cough eventually resolves, but patients may benefit from treatment with oral or inhaled corticosteroids, or ipratropium bromide (Atrovent).1
Psychogenic cough occurs less frequently in adults than in children and has lower rates of resolution in adults.3,22 Many patients with this condition do not cough during sleep, are not awakened by cough, and generally do not cough during enjoyable distractions.3,22 It is important to note that some patients with other causes of chronic cough do not cough once they fall asleep; furthermore, although a honking or barking cough has been associated with psychogenic cough, it may have an organic cause.23 The absence of definitive clinical characteristics requires that psychogenic cough be diagnosed only after all other possibilities have been eliminated.1,3 When psychogenic cough is diagnosed, removal of psychologic stressors, behavior modification therapy, and short-term use of antitussives may be beneficial.1,22
Evaluating Immunocompromised Adults
Adult patients with a compromised immune system require additional testing as part of the initial assessment. Immunocompromised patients, especially those with human immunodeficiency virus (HIV) infection, who present with respiratory complaints are more likely to have upper respiratory tract infection or acute bronchitis than pneumonia from mycobacteria, Pneumocystis carinii, fungi, viruses, and parasites.24 Chronic comorbid conditions and acute critical illness may cause depression of the immune system, thereby increasing the risk of infection.25
If a patient is HIV positive, a chest radiograph and an oxygen saturation level should be obtained. If these tests are normal, a CD4+ cell count should be obtained. If the chest radiograph, oxygen saturation level, and CD4+ count are normal, evaluation should proceed as for immunocompetent adults. If the chest radiograph or CD4+ cell count is abnormal, especially if the CD4+ cell count is below 200 cells per mm3 (0.2 × 109 per L), a more intensive evaluation for opportunistic infection is indicated.24
Evaluation of Children
In children, upper and lower respiratory tract infections, asthma, and GERD are the most common causes of chronic cough.1 In older children, cough-variant asthma, sinusitis, and psychogenic cough increase in frequency.26
The evaluation of chronic cough in children is similar to the evaluation in immunocompetent adults. However, in younger children, the adenosine 5’-monophosphate bronchial challenge has been shown to be more specific than the methacholine challenge (87 percent versus 57 percent) in differentiating asthma from other chronic pulmonary diseases of childhood.27,28
In children, asthmatic symptoms may be caused by GERD (prevalence ranging from 34 percent to 89 percent).29 Some evidence suggests that treatment of GERD with antireflux medications may reduce the symptoms of asthma, leading to a reduction in asthma medication requirements.30
Sinusitis, tuberculosis, pertussis, and cystic fibrosis are other causes of chronic cough that should be considered in children.6 Foreign body aspiration is a possibility in young children who have chronic cough. Recurrent infections may indicate an immunologic disorder as the cause of cough.6,31
Strength of Recommendations
| Key clinical recommendation | Strength of recommendation | References |
|---|---|---|
| In nonsmoking, immunocompetent adult patients with a normal chest radiograph, most cases of chronic coughs are caused by postnasal drip syndrome, asthma, and GERD. | C, expert opinion from practice guideline | 1 |
| B, nonrandomized clinical trial | 5 | |
| If a patient is not taking an ACE inhibitor and does not benefit from a reduction of irritant exposure, a chest radiograph should be obtained. | C, expert opinion from practice guideline | 1 |
| In patients with a normal chest radiograph, empiric trials of treatment for postnasal drip syndrome, asthma, and GERD are suggested. | C, expert opinion from practice guideline | 1 |
| HIV-positive patients with chronic cough should have a chest radiograph, an oxygen saturation level, and a CD4+ cell count as part of the initial evaluation. | C, expert opinion | 24 |
GERD = gastroesophageal reflux disease; ACE = angiotensin-converting enzyme; HIV = human immunodeficiency virus.
Finally, chronic cough in children can be caused by several congenital abnormalities and disorders, including vascular rings, tracheoesophageal fistulas, and primary ciliary dyskinesia. However, these conditions are rare.6

