Case Scenario
Because my father lives in another state, I usually am not involved in his medical care. Recently, though, I was contacted when he was hospitalized for pancreatitis. I knew that my father’s medical history included metabolic syndrome—diabetes, hyperlipidemia, and hypertension—and that his creatinine has been at an elevated level of 3.0 mg per dL.
During this hospitalization, an ultrasound detected a kidney mass of 3 to 5 cm, which was described to me by his physicians as exophytic. They also said they were considering the possibility that the mass was a renal cell carcinoma.
I soon learned that almost a year earlier Dad had undergone an abdominal CT scan for some other problem of which I was completely unaware. The mass had been detected at that time, as evidenced by a notation in the radiologist’s report. Nothing had been done since that CT scan to follow up on the mass.
During my father’s most recent hospitalization, the mass was once again detected and may have increased in size since the first CT last year.
According to his family physician, my father was advised to have an MRI in six months to follow the mass. The reason for waiting six months is that more invasive diagnostic work—a renal biopsy—would not alter management. If the biopsy revealed cancer, then he would require a nephrectomy which, his doctor told me, my father would not be able to tolerate because of his other underlying medical problems. “He would end up on dialysis,” his doctor said. My angry reaction was: so what? Maybe he would choose dialysis over doing nothing—isn’t that his right? Doesn’t he have the right to know what the mass is—whether it’s benign or malignant? Doesn’t he have the right to make decisions about his medical care based on this information?
Commentary
This case scenario, submitted by the patient’s son, brings up three interesting ethical questions. The first question involves whether it is ever ethically justifiable to withhold information from patients, and if so, under what circumstances? The second question is: who decides whether invasive medical procedures should be offered to a given patient? The last question is: does the patient have a right to determine his own health care?
Each question will be explored in response to exact questions posed by the patient’s son. The first question to be addressed is: “Doesn’t (my father) have the right to know what the mass is—whether it’s benign or malignant?”
In modern medicine, all patients deserve to be fully informed of their condition to the extent that physicians understand the situation.1 If information is withheld, the physician must justify his or her reasons, or risk being accused of delivering paternalistic care. As long as his mental faculties are intact, the patient has the right to know exactly what his physicians know about his condition in terms that the patient can easily understand.
All patients have the right to be fully informed in order to be active participants and to fully engage in informed decision-making.2 In this case scenario, the physician should have informed the patient of the results of his current CT scan and fully explained all viable alternatives for further diagnosis.
The physician may have withheld information about renal biopsy because he may fear that if a biopsy reveals renal carcinoma, he would be liable for not mentioning the renal mass seen on an earlier CT scan. In a self-protective manner, he concludes that this patient is too fragile to withstand a nephrectomy and appeases his feelings of guilt about silently following the mass noted previously. On the other hand, he may truly know that this patient is too fragile to survive a nephrectomy. If the likelihood of intraoperative or peri-operative mortality were so great that it would be maleficent or harmful to operate, then the physician could have said, “I will not operate because it is too risky and would surpass the standard of care.” Neither of these reasons ethically justifies withholding information from the patient and discussing the possibility of renal biopsy.
FIGURE Making Decisions About Health Care Options
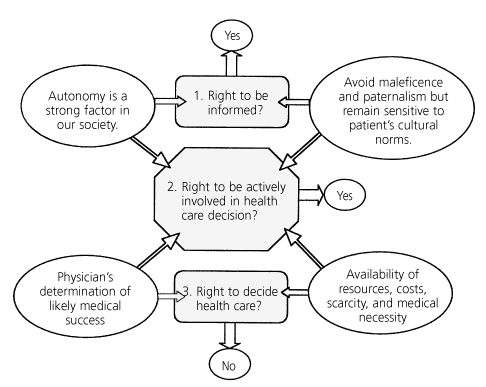
Deciding health care options.
The second question raised by the son is, “Maybe (my father) would choose dialysis over doing nothing—isn’t that his right?” This begs the more generic question: who decides how much invasive medical care will be offered to each patient? In a world where technological abilities far exceed returning patients to meaningful existence—and in a setting where costs as well as quality of life are significant issues—our society tends to avoid the question of who decides which patients receive the best and most expensive technologies. Because dialysis is paid for by Medicare, every person who can survive meaningfully on dialysis and desires this option should be offered dialysis. This is not true for more limited resources such as liver or kidney transplants.
The issue of cost and who pays is vitally important. Although dialysis would be paid for, many other treatments might be rationed, thus reducing the affordable options for a given patient. The recent Medicare legislation is a modern effort in that vein. For example, it has just cut back funding for chemotherapeutic options for cancer patients.3 Therefore, although the patient has the right to be informed, it is inaccurate to say that a patient has a right to decide, and choose to receive, the best available option for his care regardless of issues of justice, cost, and probable outcome.
A more pertinent question in this case is: who has the right to determine what forms a meaningful life? If the father has all of his mental faculties, he should make this decision for himself. If he does not, his health care proxies or next of kin should represent his wishes in deciding whether or not he can have a meaningful life on dialysis.4,5
These concepts and their interrelations are depicted graphically in the accompanying figure.
The third question posed by the son is: “Doesn’t my father have the right to make decisions about his medical care based on this information?” Or, more generically, what are the patient’s rights to determine his own health care? In order to best answer this question, we must be clear on what is meant by patient rights. When one has a right, he or she has the freedom to either do, or not do, that which is guaranteed by the right.
On the other hand, a duty is a moral obligation to do one specific thing over another without the freedom to decide. The interaction between rights and duties is important. When someone has a right, someone else has a duty.6 Hence, in this case, if the patient has the right to make decisions, then the physician has the duty to make sure the patient is given optimal information to make an informed decision.
I profess that in our current society, the patient has a right to know all that we know about his disease process, the available options for treatment, as well as costs and mechanisms for paying for these treatments. On the other hand, it is incorrect to say that the patient has a right to decide his own health care.7–9 We have already shown that the physician can deem the intervention too risky and choose not to perform a procedure such as offering nephrectomy to this patient.

