A 65-year-old woman presented for evaluation of a rash on her bilateral lower extremities that she noticed several days earlier while gardening. She denied pruritus or pain. She had no other symptoms and was otherwise well. Her medical history consisted of hypertension, depression, and a right facial nerve palsy secondary to Bell’s palsy. She had no recent additions to or changes in her medications. Physical examination showed extensive petechiae and occasional patches of brownish pigmentation confined to her lower extremities. The lesions were macular and nonpalpable (Figures 1 and 2). The remainder of her physical examination was within normal limits. Laboratory evaluation included a complete blood cell count, erythrocyte sedimentation rate (ESR), and a prothrombin and partial prothrombin time, all of which were all normal. A recent complete metabolic panel and urinalysis also were normal.
Figure 1.
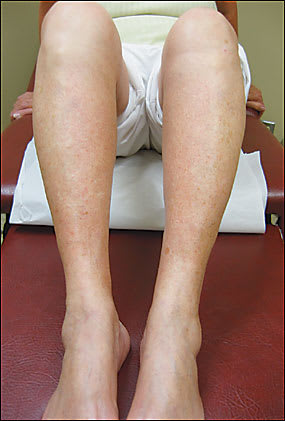
Figure 2.
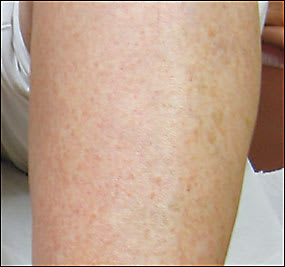
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Schamberg’s disease.
B. Henoch-Schönlein purpura.
C. Hypersensitivity (leukocytoclastic) vasculitis.
D. Idiopathic thrombocytopenic purpura.
E. Contact dermatitis.
Discussion
The answer is A: Schamberg’s disease. This is an uncommon eruption characterized by progressive, asymptomatic petechiae and patches of brownish pigmentation that may occur in any age range from children to elderly persons. The lesions may occur in any location but most often affect the lower extremities. Characteristic “cayenne pepper” spots appear within and at the edges of old lesions, caused by erythrocytes breaking down outside the capillary and leaving hemosiderin deposits. The skin lesions are nonpalpable macules that may persist for months to years and are typically asymptomatic except for the cosmetic appearance. Males tend to be affected more than females.
The exact etiology is unknown, but a cellular immune reaction may play a role. Occasionally, Schamberg’s disease occurs secondary to a drug reaction, and withdrawal of the medication may improve the lesions.1 Histologic examination shows a lymphocytic vasculitis involving the blood vessels of the upper dermis (i.e., mainly the capillaries), with endothelial swelling and extravasated red blood cells.2
Treatment of these asymptomatic lesions usually is not necessary, but some patients may wish to cover the affected areas with topical cosmetics. If mild itching occurs, topical steroids may be useful. Graduated compression elastic hose may help on the lower extremities, because this condition is thought to be caused by capillary leakage. Laser ablation of lesions has been attempted but has not proved successful.
Henoch-Schönlein purpura is an IgA-mediated hypersensitivity vasculitis that most commonly affects young children but may occur in adulthood. The constellation of symptoms occurring most often with this condition includes a palpable purpuric rash on the lower extremities or buttocks, arthritis, abdominal pain, gastrointestinal bleeding, and renal involvement. This patient was elderly and had no such associated symptoms, making this diagnosis unlikely.
Hypersensitivity vasculitis is a small vessel inflammatory disease mediated by deposition of immune complexes that cause palpable purpuric skin lesions. Prodromal symptoms usually include fever, malaise, myalgia, and joint pains. This type of vasculitis most commonly is caused by a drug reaction, but it also is associated with a number of infectious etiologies, such as hepatitis B and C, human immunodeficiency virus, and endocarditis. The ESR almost always is elevated during active vasculitis.3 Again, this patient had no such associated symptoms, her purpuric lesions were nonpalpable, and her ESR was normal.
Idiopathic thrombocytopenic purpura is a bleeding disorder characterized by low platelet numbers resulting from platelet destruction by the immune system. Skin hemorrhage, easy bruising, abnormal menstrual bleeding, or sudden and severe loss of blood from the gastrointestinal tract may occur. The diagnosis is apparent by a low platelet count and otherwise normal complete blood count. This patient had a normal platelet count.
Contact dermatitis is an inflammatory skin condition. It is unlikely in this patient because there were no signs of skin inflammation on examination and also no subjective symptoms such as pruritus or burning.
Selected Differential Diagnosis of an Unusual Petechial Rash
| Condition | Characteristics |
|---|---|
| Schamberg’s disease | Asymptomatic petechiae and patches of brownish pigmentation; cayenne pepper spots |
| Henoch-Schönlein purpura | Palpable purpuric rash; associated arthritis, abdominal pain, gastrointestinal bleeding, and renal involvement |
| Hypersensitivity (leukocytoclastic) vasculitis | Palpable purpuric rash; elevated erythrocyte sedimentation rate; prodromal fever, malaise, myalgia, and joint pains |
| Idiopathic thrombocytopenic purpura | Skin hemorrhage; low platelet numbers |
| Contact dermatitis | Inflammatory; pruritus and burning |

