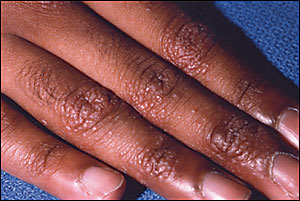
A 27-year-old man presents with a 10-year history of asymptomatic lesions on his hands and elbows. Hundreds of pinpoint-sized, skin-colored papules appear on the dorsum of his hands and the extensor surface of his upper extremities (see accompanying figure). He is otherwise in good health and is not taking any medications.
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Psoriasis.
B. Lichen nitidus.
C. Lichen simplex chronicus.
D. Prurigo nodularis.
E. Lichen planus.
Discussion
The answer is B: lichen nitidus. Lichen nitidus most commonly presents as an incidental finding on physical examination or after the patient notices an insidious onset of the lesions.1 It is characteristically asymptomatic.2 Physical examination reveals pinpoint- to pinhead-sized skin-colored papules that may be scaly or have a central depression.3 They usually are found on the forearms, trunk, and the glans and shaft of the penis.
Lichen nitidus can be discrete or generalized. In the discrete form, papules typically do not coalesce; however, they may form or group at sites of trauma or skin pressure (the isomorphic or “Koebner” phenomenon).2 In the generalized (confluent) form, papules coalesce into red-yellow to brown plaques, especially in joint flexures, wrist and forearm ventral surfaces, or inframammary areas, making the clinical diagnosis more challenging.3 Biopsy may be helpful because lichen nitidus has a characteristic histologic appearance.3
The etiology of lichen nitidus is unknown, and no laboratory abnormalities or associations with systemic disease have been established. Because lichen nitidus is rare, definitive establishment of the epidemiology is difficult. One study2 of 43 cases demonstrated a male-to-female ratio of almost 4:1, although the generalized (confluent) form may be more common in women.3 No racial predisposition or known genetic inheritance pattern has been noted.1,2 Lichen nitidus primarily affects children and young adults, with a median age of seven years in males and 13 years in females.2
Lichen nitidus may resolve spontaneously at any time without residual atrophy or pigmentary changes. This, along with its asymptomatic nature, makes clinical observation a reasonable treatment option. In one series,2 69 percent of eruptions resolved within one year; however, they can last for many years and new lesions may continue to appear as old lesions disappear.2 The evidence base for other treatments is limited. Topical steroids may cause lesions to flatten or resolve.4 Short courses of systemic corticosteroids, psoralen with long-wavelength ultraviolet light therapy,5 long-wavelength ultraviolet light/medium wavelength ultraviolet light with systemic corticosteroids,6 and sun exposure7 have been used to treat generalized disease.
The differential diagnosis includes psoriasis, lichen simplex chronicus, prurigo nodularis, and lichen planus. Psoriasis typically presents as erythematous plaques with thick, white scale on the elbows, knees, scalp, and lower lumbar area. Lichen simplex chronicus is a thickening of the skin caused by chronic rubbing, and typically presents as thick plaques. Prurigo nodularis is similar to lichen simplex chronicus in that the lesions develop because of external manipulation. These papules or nodules develop in areas that the patient can reach.
Lichen planus may appear similar to lichen nitidus. However, lichen planus often is pruritic, which may help to distinguish it from lichen nitidus.2 Characteristically, lichen planus lesions are violaceous and larger than those of lichen nitidus. Finally, lichen planus has a predilection for the ventral wrists and the buccal mucosa.
Selected Differential Diagnosis of Lichen Nitidus
| Condition | Characteristics |
|---|---|
| Psoriasis | Erythematous plaques with thick, white scale |
| Lichen simplex chronicus | Thick plaques with increased skin markings that develop after chronic rubbing |
| Prurigo nodularis | Skin-colored to hyperpigmented nodules that develop after external manipulation |
| Lichen planus | Pruritic, violaceous, flat-topped, polygonal papules |

