to the editor: Hidradenitis suppurativa is a chronic inflammatory disease of the apocrine glands that most commonly involves the perianal, perineal, axillary, and inframammary regions.1 The etiology is poorly understood, with a genetic component, hormonal influence, and obesity being linked to the expression.2 Characteristic findings include dilated keratin-filled pores, scarring and sinus tract formation, malodorous discharge, and inflammation with secondary infection.3 Medical management consists of cleaning the areas, application of mild topical steroids with the concurrent use of systemic antibiotics,4 topical antibiotics,5 and intralesional steroids. Rarely, with chronic hidradenitis suppurativa, Marjolin’s ulcer (a squamous cell carcinoma) develops.6 We report two cases of hidradenitis suppurativa in which squamous cell carcinoma developed after a latent period of 20 years and 35 years, respectively, despite repeated local excisions.
Case 1: A 51-year-old white man with a 35-year history of hidradenitis suppurativa presented with an ulcerated mass over the left scapular region (see accompanying figure). He previously had multiple local excisions. The entire mass was excised. After one month, the patient developed an abscess adjacent to the incision site, which proved to be squamous cell carcinoma on biopsy. Chemotherapy and radiotherapy were initiated. However, the tumor rapidly spread locally and a wider excision with latissimus dorsi flap reconstruction was performed. Unfortunately, the carcinoma spread rapidly to the axilla and neck, and the patient soon developed metastases in the lungs and spinal cord. He refused spinal decompression and died two weeks later.
Figure.
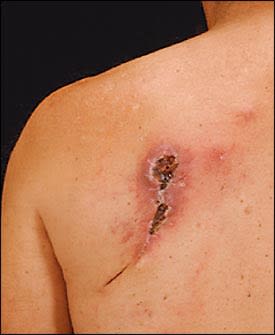
Ulcerative lesion over the left scapular region.
Case 2: A 44-year-old black woman presented with a 20-year history of hidradenitis suppurativa involving vulvar, perianal, perineal, and inframammary regions. She had undergone more than 20 surgical procedures including skin grafts to ablate the disease. Examination revealed a large abscess at the level of the vaginal introitus and an extensive ulcerated fungating lesion involving the right labial crural fold. Her entire perianal region was ulcerated and scarred, and vaginal examination was not possible. Multiple biopsies were performed revealing infiltrating, moderately differentiated squamous cell carcinoma of the right labia, distal vagina, and urethra, with satellite lesions on the mons and right medial thigh.
Magnetic resonance imaging and computed tomography (CT) of the abdomen and pelvis revealed extensive bilateral inguinal, pelvic, and periaortic lymphadenopathy extending to a level inferior to the renal arteries. CT also revealed metastases of the squamous cell carcinoma to the right pubic bone. The patient continued to refuse operative management, instead opting for palliative high-dose radiation to control bleeding. She died from the carcinoma in six months.
Both of these patients presented with widespread metastases and a resultant terminal outcome. It would appear that a clear association between chronic hidradenitis suppurativa and squamous cell carcinoma exists. Because of the poor prognosis associated with squamous cell carcinoma, we advocate wide excision of hidradenitis suppurativa lesions when other treatments have failed and recommend biopsy of all suspicious hidradenitis suppurativa lesions.

