to the editor: A 43-year-old man presented with a one-year history of bilateral facial swelling. Previously, he had been told the swelling was caused by enlargement of the parotids. No etiology was given, and simple observation was elected. Subsequently, the right side improved, but the left side worsened. The patient reported no pain, fever, chills, respiratory symptoms, testicular pain, weight loss, sicca syndrome, halitosis, trauma, recent dental work, or known tuberculosis exposure. The patient had a sulfa allergy.
On examination, the patient was afebrile and appeared well nourished. The parotids were firm, nontender, and enlarged, especially the left side (which measured 3 by 4 cm) obscuring the mandibular angle (Figure 1). The opening of Stensen’s duct had no drainage. Small, nontender cervical lymph nodes were appreciated. The remaining physical examination was unremarkable.
Figure 1.
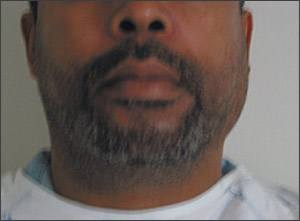
Enlarged left parotid gland.
A complete blood cell count, metabolic panel, and tuberculin skin test were normal. Immunoglobulin M antibodies to mumps and the Epstein-Barr virus were negative. Mumps immunoglobulin G antibodies were positive. The patient’s angiotensin-converting enzyme level was slightly elevated (56 U per L), and the rapid plasma reagin test was nonreactive. An enzyme-linked immunosorbent assay test was positive for human immunodeficiency virus (HIV), which was confirmed by Western blot technique. The CD4 count was 148 cells per mm3, CD8 count was 1,370 cells per mm3, and the viral load was 210,000 copies per mL. A chest radiograph was negative. Magnetic resonance imaging of the face and head revealed a 2.5-cm diameter cyst in the posterior aspect of the left parotid gland and an 8-mm cyst further anterior (Figure 2). The right parotid gland had a 3-mm simple cyst in the deep lobe. All cysts did not enhance with gadolinium and were consistent with simple lymphoepithelial parotid cysts. The patient did not undergo a biopsy.
Figure 2.
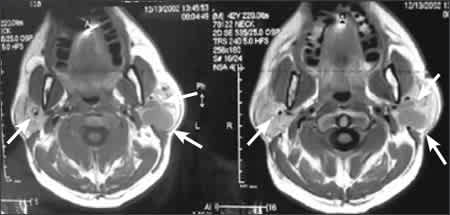
Benign lymphoepithelial cysts (arrows).
Benign lymphoepithelial cysts of the parotid, also occurring in diffuse infiltrative lymphocytosis syndrome, appear to be determined genetically.1 This condition occurs in approximately 5 percent of patients positive for HIV.2 The histopathogenesis of lymphoepithelial cysts of the parotid remains debated. It is postulated that parotid enlargement results from HIV replication within the five to 10 embryologic-derived lymph nodes within the parotid, causing lymphoproliferation.3 Lymphoid cells have been shown to infiltrate salivary gland tissue and incite a lymphoepithelial lesion of striated ducts with associated basal cell hyperplasia causing duct compression enhancing the cystic nature of the lesions.4,5 The T-cell population within the cysts has been found to be CD8 positive and CD4 negative, suggesting an HIV-induced autoimmune-like syndrome.4
Parotid benign lymphoepithelial cysts have no impact on the progression of HIV but can cause significant cosmetic deformities. Treatment options include radiation, chemotherapy, and surgery. Combination antiretroviral therapy with and without steroids has been shown to be effective in treating these lesions.6
The patient was started on dapsone for Pneumocystis carinii pneumonia prophylaxis and was referred to an infectious diseases subspecialist. He was started on a lamivudine-zidovudine (Combivir) combination and efavirenz (Sustiva) therapy without steroids. Improvement of the parotid lesions was noted in two weeks.
This case is a reminder that the initial presentation of HIV infection may be parotid enlargement.

