Health literacy is basic reading and numerical skills that allow a person to function in the health care environment. Even though most adults read at an eighth-grade level, and 20 percent of the population reads at or below a fifth-grade level, most health care materials are written at a 10th-grade level. Older patients are particularly affected because their reading and comprehension abilities are influenced by their cognition and their vision and hearing status. Inadequate health literacy can result in difficulty accessing health care, following instructions from a physician, and taking medication properly. Patients with inadequate health literacy are more likely to be hospitalized than patients with adequate skills. Patients understand medical information better when spoken to slowly, simple words are used, and a restricted amount of information is presented. For optimal comprehension and compliance, patient education material should be written at a sixth-grade or lower reading level, preferably including pictures and illustrations. All patients prefer reading medical information written in clear and concise language. Physicians should be alert to this problem because most patients are unwilling to admit that they have literacy problems.
The American Medical Association (AMA) defines health literacy as “a constellation of skills, including the ability to perform basic reading and numerical tasks required to function in the health care environment.”1 Inadequate health literacy contributes to poor compliance, uncontrolled chronic disease, and rising health care costs. A recent report by the Agency for Healthcare Research and Quality on health literacy concluded that “low reading skills and poor health are clearly related.”2
Epidemiology
Most health care materials are written at a 10th-grade level or higher. However, most adults read between the eighth and ninth grade level.3 Approximately one half of adults are unable to understand printed health care material, and approximately 90 million adults have fair to poor literacy.3 Twenty-one to 23 percent of adults read at the lowest reading level, approximately fifth-grade or lower.3 For patients whose primary language is not English, the problem is compounded.4 A survey of patients at two hospitals revealed that 35 percent of English-speaking patients and 62 percent of Spanish-speaking patients had fair to poor health literacy.5
The problem of inadequate literacy is greater in older patients. The majority of patients older than 60 years perform at the lowest levels of literacy,6 and 80 percent have limited ability to fill out forms, such as the ones they are asked to complete in physician waiting rooms. Ramifications are compounded in older patients because they are more likely to have chronic and comorbid conditions.
Impact of Inadequate Health Literacy
Patients with inadequate health literacy face many obstacles when accessing and using the health care system. Literacy problems can inhibit a patient’s ability to attend appointments because they may not be able to register for health insurance or follow directions to the physician’s office.7 Once at the office, they may not be able to complete forms proficiently,8 may be ashamed to ask for assistance in filling out forms, may leave with unanswered questions, or may sign a document they have not understood. Many patients complain that their physician did not explain their medical condition in words they could understand. Once the appointment is over, patients with inadequate health literacy may not know when to return or how to follow up on the visit.
The majority of patients with literacy problems are unable to follow the prescription directions. “Take 1 tablet X times a day,” with the X being a number8; the medicine is taken at inappropriate times or intervals, or in the wrong quantities. Patients are more likely to understand prescription directions, and follow them correctly, when they are written, “Take 1 tablet every X hours.”
Patients with inadequate health literacy have difficulty controlling chronic illnesses.9After adjusting for sociodemographic and health factors, results of one cross-sectional, observational study10 showed that patients with diabetes and inadequate health literacy have poorer glycemic control and higher levels of retinopathy than patients with adequate literacy skills. Patients with asthma and inadequate health literacy do not use their inhalers as well as patients with asthma and adequate literacy skills.11
Patients with health literacy problems are less likely to understand and participate in disease prevention and health promotion programs12,13 and are more likely to be hospitalized than those with adequate health literacy,14 resulting in an additional $69 billion in health care costs annually.4
Assessing Health Literacy
A group of medical residents were asked to identify which of their patients had inadequate health literacy. The residents identified 10 percent of their patients, but the actual figure was more than one third.15 Most physicians who attempt to measure the literacy level of their patients make the mistake of asking for the highest grade or level of education that they completed. It has been shown that the final grade completed often is higher than the actual level of literacy.3 Many high school graduates are illiterate; as age increases, so do the deficits in literacy as a result of declining cognitive function, increased time since formal education, and decreased sensory abilities. Another common mistake is to rely on patients’ own assessment of their reading skills. The majority of patients who have low health literacy say that they read “well.”1
Patients with inadequate health literacy often feel a sense of shame and decreased worth,3 and they may be too embarrassed to ask their physician to explain or repeat instructions and other relevant information. Many are so embarrassed by this handicap that they do not tell their spouse.16 Behaviors suggestive of limited literacy are listed in Table 1.7
TABLE 1 Behaviors Suggestive of Inadequate Health Literacy Skills
| Asking staff for help |
| Bringing along someone who can read |
| Inability to keep appointments |
| Making excuses (“I forgot my glasses.”) |
| Noncompliance with medication |
| Poor adherence to recommended interventions (e.g., changes to decrease acid reflux, such as elevating the head of the bed) |
| Postponing decision making (“May I take the instructions home?” or “I’ll read through this when I get home.”) |
| Watching others (mimicking behavior) |
Information from reference 7.
Many reading cognition assessment tools are available with which to measure health literacy and assess a patient’s recognition of health care terms4 and their ability to interpret written health-related material.17 The Rapid Estimate of Adult Literacy in Medicine is the quickest of these, taking two to three minutes to complete, and can be administered by a nurse or other staff member(Figure 1).4 The Test of Functional Health Literacy in Adults provides a more thorough picture of the patient’s ability to comprehend health material, but it is more time consuming and less practical.
Figure 1. Rapid Estimate of Adult Literacy in Medicine
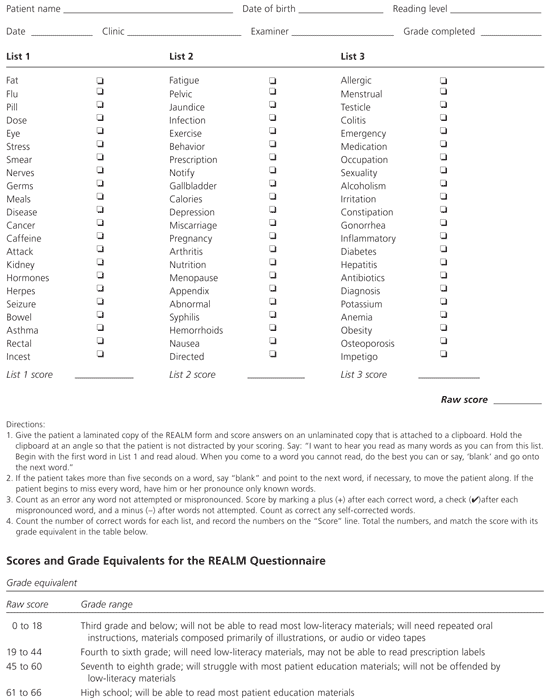
Rapid estimate of adult literacy in medicine (REALM).
Reprinted with permission from Health literacy: A prescription to end confusion. Institute of Medicine, 2004. Accessed online July 8, 2005, at:http://www. nap.edu/books/0309091179/html/301.html.
Addressing Health Literacy
In 1999, the AMA published a report that recommended increasing public awareness, educating the medical community, and encouraging research on health literacy.1The Joint Commission on Accreditation of Healthcare Organizations has added health literacy benchmarks for hospitals to achieve, and improving health literacy is one of the Healthy People 2010 goals. Most recently, the Institute of Medicine of the National Academies added health literacy to its list of areas for quality improvement.
Physicians need to provide patients with information that is simple and clear to help them understand their medical condition and its treatment. Many physicians rely on written material they send home with their patients to reinforce or explain further the information discussed during the visit. However, this information often is written at a grade level too high for most patients to understand. Educational materials should be short, clear, and simple, and should include pictures.18 One randomized controlled trial19 demonstrated the effectiveness of a low-literacy educational handout in increasing pneumococcal vaccine rates. Simplifying patient education material by writing it at a sixth-grade level or lower increases comprehension,4 and patients with adequate literacy prefer to read health information that is written at a lower grade level.19 The focus of the patient education handout should be on the patient’s experience of the condition, rather than the pathophysiology. Presenting too much information on the underlying pathophysiology and using long and complicated words can decrease a patient’s understanding of the material.18 Table 2 lists elements found in good patient education materials.20
When giving information verbally, talking too quickly reduces the chance that patients will understand what is being said. It is important for physicians to take time to ask their patients to repeat the instructions or otherwise demonstrate their understanding(Table 3).21 Physicians seldom check to see if patients understand what happened during these visits.22 A list of Web sites physicians can use to obtain free patient education materials and more information about health literacy is provided in Table 4. Patients who have the most difficulty comprehending health material are the least likely to have access to the Internet or know how to use it.
TABLE 3 Six Steps to Enhance Understanding Among Patients with Low Health Literacy
| Slow down, and take time to assess the patients’ health literacy skills. |
| Use “living room” language instead of medical terminology. |
| Show or draw pictures to enhance understanding and subsequent recall. |
| Limit information given at each interaction, and repeat instructions. |
| Use a “teach back” or “show me” approach to confirm understanding. This approach involves having physicians take responsibility for adequate teaching by asking patients to demonstrate what they have been told (e.g., repeat how to take their medication) to ensure that education has been adequate. |
| Be respectful, caring, and sensitive, thereby empowering patients to participate in their own health care. |
Adapted with permission from Williams MV, Davis T, Parker RM, Weiss BD. The role of health literacy in patient-physician communication. Fam Med 2002;34:387.
TABLE 4 Related Web Sites
| Information on health literacy | Patient Web sites* | ||
| American Medical Association Foundation | American Academy of Family Physicians | ||
| Health Literacy Initiative | https://www.aafp.org | ||
| http://www.amafoundation.org | American Dietetic Association | ||
| Center for Health Care Strategies | http://www.eatright.org | ||
| http://www.chcs.org | American Heart Association | ||
| Institute of Medicine of the National Academies | http://www.americanheart.org | ||
| http://www.iom.edu/project.asp?id=3827 | National Cancer Institute | ||
| National Institute for Literacy | http://www.nci.nih.gov | ||
| http://www.nifl.gov | National Heart, Lung, and Blood Institute | ||
| Pfizer Clear Health Communication Initiative | http://www.nhlbi.nih.gov | ||
| http://www.pfizerhealthliteracy.com | National Institutes of Health | ||
| http://www.nih.gov | |||
| North Country Care-Net | |||
| http://www.nchin.org/care-net | |||
*—These Web sites vary in quality and usefulness for low-literacy patients.

