Historically, osteopathic physicians have made an important contribution to the primary care workforce. More than one half of osteopathic physicians are primary care physicians, and most of these are family physicians. However, the proportion of osteopathic students choosing family medicine, like that of their allopathic peers, is declining, and currently is only one in five.
Traditionally, osteopathic students have been more likely than allopathic students to choose primary care specialties, and as such, they have been important contributors to the primary care physician workforce. In 2004, about 629,000 (67 percent) of the 936,000 physicians in the United States and its territories reported patient care as their major professional activity, and just 226,000 (36 percent) of these were in the primary care specialties of family medicine/general practice, internal medicine, and general pediatrics.1 Fourteen percent of direct patient care physicians were family physicians or general practitioners. Osteopathic physicians composed 5 percent of physicians involved in patient care, although 55 percent of these were in primary care specialties, and 41 percent of osteopathic physicians in patient care were family physicians or general practitioners (Figure 1).2
Figure 1.
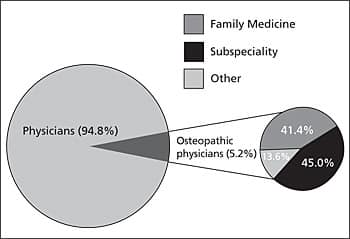
Osteopathic Physician Workforce, 2004
Information from reference 2.
Figure 2.
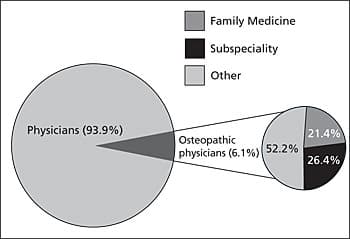
Osteopathic Residency Workforce, 2004
Information from reference 2.
The shift away from primary care and family medicine, particularly apparent in allopathic students, also is taking place in osteopathic schools. Slightly more than one half (52 percent) of osteopathic medical students are choosing residency training outside of primary care. Only 21 percent of osteopathic medical residents are in family medicine training programs, down from 37 percent in 1996 and 31 percent in 2002 (Figure 2).2 This trend mirrors choices by allopathic graduates, of whom 9 percent are currently in family medicine residency programs.
The reduced selection of primary care and family medicine by osteopathic students may be a normal fluctuation, but it is worth investigating to understand whether it is reversible or a sustained downturn. It would be particularly troubling if, as in allopathic schools, the shift is reflective of a change in valuation of and commitment to primary care by osteopathic medicine that affects student selection and mentoring arrangements.

