Spontaneous abortion, which is the loss of a pregnancy without outside intervention before 20 weeks’ gestation, affects up to 20 percent of recognized pregnancies. Spontaneous abortion can be subdivided into threatened abortion, inevitable abortion, incomplete abortion, missed abortion, septic abortion, complete abortion, and recurrent spontaneous abortion. Ultrasonography is helpful in the diagnosis of spontaneous abortion, but other testing may be needed if an ectopic pregnancy cannot be ruled out. Chromosomal abnormalities are causative in approximately 50 percent of spontaneous abortions; multiple other factors also may play a role. Traditional treatment consisting of surgical evacuation of the uterus remains the treatment of choice in unstable patients. Recent studies suggest that expectant or medical management is appropriate in selected patients. Patients with a completed spontaneous abortion rarely require medical or surgical intervention. For women with incomplete spontaneous abortion, expectant management for up to two weeks usually is successful, and medical therapy provides little additional benefit. When patients are allowed to choose between treatment options, a large percentage will choose expectant management. Expectant management of missed spontaneous abortion has variable success rates, but medical therapy with intravaginal misoprostol has an 80 percent success rate. Physicians should be aware of psychologic issues that patients and their partners face after completing a spontaneous abortion. Women are at increased risk for significant depression and anxiety for up to one year after spontaneous abortion. Counseling to address feelings of guilt, the grief process, and how to cope with friends and family should be provided.
Spontaneous abortion refers to pregnancy loss at less than 20 weeks’ gestation in the absence of elective medical or surgical measures to terminate the pregnancy. The term “miscarriage” is synonymous and often is used with patients because the word “abortion” is associated with elective termination. “Spontaneous pregnancy loss” has been recommended to avoid the term “abortion” and acknowledge the emotional aspects of losing a pregnancy.1 Another emotionally neutral term is “early pregnancy failure.”2
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The possibility of ectopic pregnancy should be considered when transvaginal ultrasonography reveals an empty uterus and the quantitative serum human chorionic gonadotropin level is greater than 1,800 mIU per mL (1,800 IU per L). | C | 5 |
| Transvaginal ultrasound should be performed in the first trimester of pregnancy when incomplete abortion is suspected and is extremely reliable in identifying intrauterine products of conception. | C | 7,8 |
| Expectant management should be considered for women with incomplete spontaneous abortions. It has an 82 to 96 percent success rate without the need for surgical or medical intervention. | A | 17–22,24 |
| When misoprostol (Cytotec) is used to treat women with a missed spontaneous abortion, it should be given vaginally rather than orally. | B | 27 |
| Patients who have had a spontaneous abortion should be given the opportunity to choose a treatment option. | B | 28 |
| A 50-mcg dose of Rho(D) immune globulin (Rhogam) should be administered to Rh-negative patients who have a threatened abortion or have completed a spontaneous abortion. | C | 5 |
| Physicians should be alert to the development of psychologic symptoms that frequently occur following spontaneous abortion (e.g., depression, anxiety). | C | 31–34 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1154 orhttps://www.aafp.org/afpsort.xml.
For clinical purposes, spontaneous abortion often is subdivided into threatened abortion, inevitable abortion, incomplete abortion, missed abortion, septic abortion, recurrent spontaneous abortion, and complete abortion (Table 1).
TABLE 1 Spontaneous Abortion: Definitions of Subcategories
| Complete abortion: all products of conception have been passed without the need for surgical or medical intervention |
| Incomplete abortion: some, but not all, of the products of conception have been passed; retained products may be part of the fetus, placenta, or membranes |
| Inevitable abortion: the cervix has dilated, but the products of conception have not been expelled |
| Missed abortion: a pregnancy in which there is a fetal demise (usually for a number of weeks) but no uterine activity to expel the products of conception |
| Recurrent spontaneous abortion: three or more consecutive pregnancy losses |
| Septic abortion: a spontaneous abortion that is complicated by intrauterine infection |
| Threatened abortion: a pregnancy complicated by bleeding before 20 weeks’ gestation |
Incidence
Approximately 20 percent of pregnant women will have some bleeding before 20 weeks’ gestation, and roughly one half of these pregnancies will end in spontaneous abortion.3 Up to 20 percent of recognized pregnancies will end in miscarriage. However, when women were followed with serial serum human chorionic gonadotropin (hCG) measurements, the actual miscarriage rate was found to be 31 percent.4 Many pregnancies are lost spontaneously before a woman recognizes that she is pregnant, and the clinical signs of miscarriage are mistaken for a heavy or late menses.
Diagnosis
Threatened abortion is defined by vaginal bleeding in a woman with a confirmed pregnancy. First-trimester bleeding in a pregnant woman has an extensive differential diagnosis (Table 2) and should be evaluated with a full history and physical examination. Laboratory tests should include potassium hydroxide and “wet prep” microscopy of any vaginal discharge, complete blood count, blood typing and Rh testing, and quantitative serum hCG testing. Gonorrhea and chlamydia testing also should be considered. Ultrasonography is crucial in identifying the status of the pregnancy and verifying that the pregnancy is intrauterine. When transvaginal ultrasonography reveals an empty uterus and the quantitative serum hCG level is greater than 1,800 mIU per mL (1,800 IU per L), an ectopic pregnancy should be considered.5 When transabdominal ultrasonography is performed, an empty uterus should raise suspicion of an ectopic pregnancy if quantitative hCG levels are greater than 3,500 mIU per mL (3,500 IU per L). A uterus found to be empty on ultrasound examination may signal a completed spontaneous abortion, but the diagnosis is not definitive until ectopic pregnancy is excluded. If an ultrasound examination finds an intrauterine pregnancy, ectopic pregnancy is unlikely, although heterotopic pregnancy has been reported (i.e., simultaneous intrauterine and ectopic pregnancies).5 The risk for spontaneous abortion decreases from 50 to 3 percent when a fetal heartbeat is identified on ultrasound examination.1
TABLE 2 Differential Diagnosis of First-Trimester Vaginal Bleeding
| Cervical abnormalities (e.g., excessive friability, malignancy, polyps, trauma) |
| Ectopic pregnancy |
| Idiopathic bleeding in a viable pregnancy |
| Infection of the vagina or cervix |
| Molar pregnancy |
| Spontaneous abortion |
| Subchorionic hemorrhage |
| Vaginal trauma |
When the clinical examination reveals a dilated cervix, spontaneous abortion is inevitable. However, cervical evaluation is not reliable for distinguishing between complete and incomplete abortion.6,7 Transvaginal ultrasonography should be performed and is extremely reliable for finding products of conception, with a 90 to 100 percent sensitivity and 80 to 92 percent specificity.7,8
A missed spontaneous abortion usually is diagnosed by routine ultrasonography or when an ultrasound scan is obtained because the symptoms and physical signs of pregnancy are regressing. Figure 1 presents an algorithm for diagnosing spontaneous abortion.1
Figure 1. Diagnosis of Spontaneous Abortion
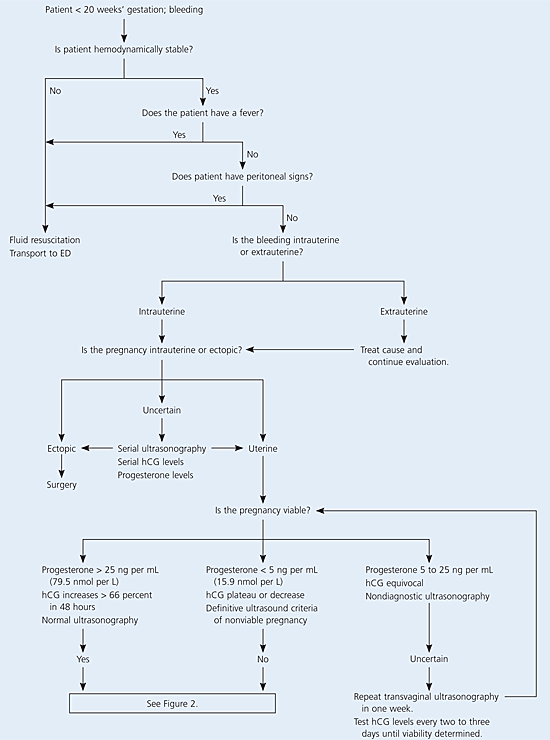
Algorithm for the diagnosis of spontaneous pregnancy loss. (ED = emergency department; hCG = human chorionic gonadotropin.)
Adapted with permission from Scroggins KM, Smucker WD, Krishen AE. Spontaneous pregnancy loss: evaluation, management, and follow-up counseling. Prim Care 2000;27:157.
Etiology and Risk Factors
Chromosomal abnormalities are a direct cause of spontaneous abortion. One meta-analysis9 found that a chromosomal abnormality occurs in 49 percent of spontaneous abortions. Autosomal trisomy was the most commonly identified anomaly (52 percent), followed by polyploidy (21 percent) and monosomy X (13 percent).9 Most chromosomal abnormalities that result in spontaneous abortion are random events, such as maternal and paternal gametogenesis errors, dispermy, and nondisjunction. Structural abnormalities of individual chromosomes (e.g., translocations, inversions) were reported in 6 percent of women who had spontaneous abortions, and approximately one half of these abnormalities were inherited.9 Chromosomal abnormalities are more likely to be associated with recurrent spontaneous abortion, but are uncommon even in that instance (4 to 6 percent).9
Risk factors for spontaneous abortion are listed in Table 3.1,10–14 However, other factors are notable for their lack of association with miscarriage. One study15 that examined the influence of stress on early pregnancy loss failed to find a clear association. Marijuana use, likewise, has not been proven to increase the risk for spontaneous abortion.11 Sexual activity also does not elevate risk in women with uncomplicated pregnancies.
TABLE 3 Risk Factors for Spontaneous Abortion
| Advanced maternal age |
| Alcohol use |
| Anesthetic gas use (e.g., nitrous oxide) |
| Caffeine use (heavy) |
| Chronic maternal diseases: poorly controlled diabetes, celiac disease, autoimmune diseases (particularly antiphospholipid antibody syndrome) |
| Cigarette smoking |
| Cocaine use |
| Conception within three to six months after delivery |
| Intrauterine device use |
| Maternal infections: bacterial vaginosis; mycoplasmosis, herpes simplex virus, toxoplasmosis, listeriosis, chlamydia, human immunodeficiency virus, syphilis, parvovirus B19, malaria, gonorrhea, rubella, cytomegalovirus |
| Medications: misoprostol (Cytotec), retinoids, methotrexate, nonsteroidal anti-inflammatory drugs |
| Multiple previous elective abortions |
| Previous spontaneous abortion |
| Toxins: arsenic, lead, ethylene glycol, carbon disulfide, polyurethane, heavy metals, organic solvents |
| Uterine abnormalities: congenital anomalies, adhesions, leiomyoma |
Treatment
Dilatation and curettage is the traditional treatment for spontaneous abortion; manual vacuum aspiration is another surgical option. Prompt surgical evacuation of the uterus has been recommended in the past because of the risk for infection and concerns about coagulation disorders that result from retained products of conception.1,2 However, the need for immediate surgical evacuation in all patients with a spontaneous abortion has been questioned. Many recent studies16–24 have examined the outcomes of expectant and medical management for women with spontaneous abortions.
Prompt surgical evacuation of the uterus is the treatment of choice when the patient is unstable because of heavy bleeding or has evidence of a septic abortion. Patient choice is another reason to proceed with surgical evacuation.
Some women may have already completed a spontaneous abortion by the time they present for clinical evaluation. If the ultrasound examination shows an empty uterus and evaluation of the expelled tissue confirms the presence of products of conception, no further action is needed; in these instances, patients have a completed spontaneous abortion and can be managed expectantly.16 If the products of conception are not physically confirmed when the uterus is empty, an ectopic pregnancy must be ruled out.
Many studies17–24 have compared expectant management, medical therapy, and surgical management for women with incomplete spontaneous abortion. Expectant management proved to be successful, with no need for surgical intervention in 82 to 96 percent of women.17–22,24 Most patients who had surgical intervention were followed expectantly for two weeks before intervention was recommended.17,19,21 Medical therapy with misoprostol (Cytotec) or mifepristone (Mifeprex) does not confer significant additional benefit.23 The average time to completion of the miscarriage was nine days.20
In women with missed spontaneous abortions, expectant management has a variable but generally lower success rate than medical therapy, ranging from 16 to 76 percent.17,20,25,26 In contrast, medical therapy for missed spontaneous abortion results in high success rates for completion of a spontaneous abortion without surgical intervention. One study25 found that patients had an 80 percent success rate after using 800 mcg of misoprostol, administered intravaginally and repeated after four hours, if necessary. Intravaginal administration of misoprostol causes less diarrhea than oral administration.27
Patient preferences should be considered when choosing a treatment for spontaneous abortion. Physicians should discuss the available options and the evidence to support each option with the patient. There is evidence to suggest that women who are given the opportunity to choose a treatment option have better subsequent mental health than women who are not allowed to choose their therapy.28 However, patients express less happiness with the mode of treatment they receive and are less willing to have the same care again when they begin with noninvasive management and later require surgical intervention.29 When patients are allowed to choose their therapy, 38 to 75 percent choose expectant management.20,26,30
An algorithm for managing women with spontaneous abortion is presented in Figure 2.1 A 50-mcg dose of Rho (D) immune globulin (Rhogam) should be given to patients who are Rh-negative and have a threatened abortion or have completed a spontaneous abortion.5
Figure 2. Management of Spontaneous Abortion
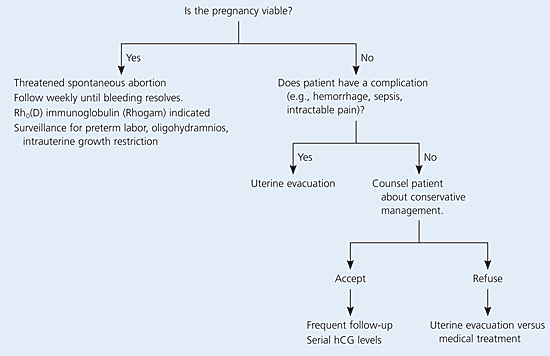
Algorithm for the management of spontaneous pregnancy loss. (hCG = human chorionic gonadotropin.)
Adapted with permission from Scroggins KM, Smucker WD, Krishen AE. Spontaneous pregnancy loss: evaluation, management, and follow-up counseling. Prim Care 2000;27:161.
Psychologic Issues After Spontaneous Abortion
Physicians should recognize the psychologic issues that affect a patient who experiences a spontaneous abortion. Although the literature lacks good evidence to support psychologic counseling for women after a spontaneous abortion, it is thought that patients will have better outcomes if these issues are addressed. The patient and her partner may be dealing with feelings of guilt, and they typically will go through a grieving process and have symptoms of anxiety and depression.
Women who have a spontaneous abortion frequently struggle with guilt over what they may have done to cause or prevent the loss. Physicians should address the issue of guilt with their patients and allay any concerns that they may have “caused” the spontaneous abortion.
Physicians should encourage the patient and her partner to allow themselves to grieve. The woman and her partner may grieve differently; specifically, they may go through the stages of grief in different orders or at different rates. They also should be aware that friends and family members may not recognize the magnitude of their loss. Friends and family members may ignore the subject of miscarriage, or they may make well-meaning comments that try to minimize the event. Connecting the couple with a counselor who has experience in helping couples cope with pregnancy loss may be beneficial. Many hospitals offer programs that provide follow-up care and literature to the woman and her partner. Two national organizations, the Compassionate Friends (http://www.compassionatefriends.org; telephone: 877–969–0010) and SHARE Pregnancy and Infant Loss Support, Inc. (http://www.nationalshareoffice.com; telephone: 800–821–6819), provide support for women and their partners as they progress through the grieving process after a miscarriage.
Most studies31–34 have found that a significant percentage of women experience psychiatric symptoms in the weeks to months after spontaneous abortion. Women who were found to be especially prone to these symptoms are childless and have lost a wanted pregnancy.31 One study28 showed that women who are managed expectantly have better overall mental health 12 weeks after a spontaneous abortion.
Physicians should realize the importance of providing care that is sensitive to the medical and psychologic aspects of a couple who experiences spontaneous abortion. Many patients report dissatisfaction with the medical care they receive.35,36 The Advanced Life Support in Obstetrics5 provider course offered by the American Academy of Family Physicians summarizes issues to discuss with women and their partners after a spontaneous abortion (Table 4).5
TABLE 4 Points to Cover with Women and Their Partners After Spontaneous Abortion
| Acknowledge and attempt to dispel guilt |
| Acknowledge and legitimize grief |
| Assess level of grief and adjust counseling accordingly |
| Counsel how to tell family and friends of the miscarriage |
| Include the patient’s partner in psychologic care |
| Provide comfort, empathy, and ongoing support |
| Reassure about the future |
| Warn about the “anniversary phenomenon” |
Information from reference 5.

