
Am Fam Physician. 2005;72(8):1503-1510
Author disclosure: Nothing to disclose.
Support of patient self-management is a key component of effective chronic illness care and improved patient outcomes. Self-management support goes beyond traditional knowledge-based patient education to include processes that develop patient problem-solving skills, improve self-efficacy, and support application of knowledge in real-life situations that matter to patients. This approach also encompasses system-focused changes in the primary care environment. Family physicians can support patient self-management by structuring patient-physician interactions to identify problems from the patient perspective, making office environment changes that remove self-management barriers, and providing education individually and through available community self-management resources. The emerging evidence supports the implementation of practice strategies that are conducive to patient self-management and improved patient outcomes among chronically ill patients.
A global rise in life expectancy and an increase in cultural and environmental risks such as smoking, unhealthy diet, lack of physical activity, and air pollution are associated with an epidemic of chronic illness. Approximately 120 million Americans have one or more chronic illnesses, accounting for 70 to 80 percent of health care costs. Twenty-five percent of Medicare recipients have four or more chronic conditions, accounting for two thirds of Medicare expenditures.1,2 Most patients with chronic conditions such as hypertension, diabetes, hyperlipidemia, congestive heart failure, asthma, and depression are not treated adequately, and the burden of chronic illness is magnified by the fact that chronic conditions often occur as comorbidities.3
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| To support self-management, family physicians should address goal setting and problem solving, make office system changes, provide self-management education, and link the patient to community self-management programs. | C | 10 |
| Motivational interviewing is recommended as an effective way to prevent relapse in alcohol dependence. | A | 18 |
| Weekly follow-up phone calls by a nurse manager and monthly calls by a physician are recommended as a way to improve blood sugar control and weight loss in patients with diabetes. | B | 5 |
Physician support of patient self-management is one of the key elements of a systems-oriented chronic care model.4 Increasing evidence shows that self-management support reduces hospitalizations, emergency department use, and overall managed care costs, although the cost of self-management interventions in individual nonmanaged care practices has yet to be determined.3,5–7 A review7 of 41 studies assessing interventions to improve diabetes outcomes in primary care revealed that adding patient-oriented interventions can lead to improvements in outcomes such as glycemic control. In 36 trials focused on adult asthma, self-management (self-monitoring coupled with medical review and a written action plan) produced greater reductions in nocturnal symptoms, hospitalizations, and emergency department use than did usual care.8 Another community-based group program, designed to increase self-efficacy among patients with diabetes, resulted in improved self-efficacy and A1C levels.9 Despite this encouraging evidence, self-management is the least implemented and most challenging area of chronic disease management.10
Although the terms patient self-management, self-management support, and patient education often are used interchangeably, they do not have the same meaning. Self-management is the ability of the patient to deal with all that a chronic illness entails, including symptoms, treatment, physical and social consequences, and lifestyle changes.11 With effective self-management, the patient can monitor his or her condition and make whatever cognitive, behavioral, and emotional changes are needed to maintain a satisfactory quality of life.11 Self-management support is the process of making multilevel changes in health care systems and the community to facilitate patient self-management.10,12 Patient education generally refers to knowledge-based instructions for a specific disease. Self-management education differs from traditional patient education in what is taught, how problems are formulated, the relation of what is taught to the disease, and the theory underlying the goal (Table 1).13
The theory underlying patient education is that increasing a patient’s knowledge about a disease leads to behavioral change that improves clinical outcomes. An underlying theory of self-management education is that self-efficacy, or the patient’s belief in his or her own ability to accomplish a specific behavior or achieve a reduction in symptoms, leads to improved clinical outcomes. Self-management support expands the role of health care professionals from delivering information to include helping patients build confidence and make choices that lead to improved self-management and better outcomes. Patient education typically is given by a health care professional; self-management can be taught and supported by health care professionals, office support staff, peer leaders, and other patients.
The self-management challenges for persons with chronic conditions can be divided into three types: medical management, role management, and emotional management.13–15 Physicians who want to provide increased support of their patients’ self-management are advised to address three areas: structuring patient-physician interactions to include goal-setting and problem-solving strategies, making office system changes, and providing self-management education by linking patients to community self-management programs.10
Practical Applications for Physicians
There are many ways that physicians can translate this evidence for self-management support into daily practice. Primarily, this involves a shift of focus away from clinical outcomes (e.g., reducing A1C levels) and toward providing help with the day-today problems of living with chronic illness (e.g., making healthful food selections in restaurants). It may be useful for physicians making this shift to remind themselves that, for the patient, self-management is inevitable and already occurring.10,16 More specific methods are discussed below, and summarized in Table 2.
| Physician actions |
| Address health literacy issues and medical obstacles to self-management. |
| Identify problems from the patient’s perspective by asking provocative questions and listening to patient responses (Figure 1). |
| Include goal-setting, action-planning, and problem-solving strategies to overcome barriers based on the patient’s immediate concerns. |
| Link patients to community-based self-management resources. |
| Provide self-management education. |
| Practice changes |
| Follow up with patients systematically about action plans and goals, in person, by phone, or by e-mail. |
| Provide group visits that include self-management education. |
| Schedule planned visits that allow time to address self-management tasks. |
MOTIVATIONAL INTERVIEWING
Motivational interviewing is an in-depth approach to decision making intended to help patients come to their own decisions by exploring their uncertainties. The interviewer uses directive questions and reflective listening to encourage the patient to participate (Figure 1).17 This style of interview, asking the patient provocative questions and discussing the responses, often can help uncover important self-management issues, and has been proven effective for preventing relapse in patients with alcohol dependence.18

IDENTIFYING BARRIERS
A common barrier to successful self-management is that chronic conditions often occur as comorbidities. Patients with chronic diseases who are asked to identify barriers to self-management often cite examples such as aggravation of one condition by the symptoms or treatment of another, and problems created by multiple medication regimens.16,19,20 Physicians can help patients set goals that will affect real-life challenges, rather than disease-oriented goals. For example, a patient with diabetes and asthma has limited ability to do the exercise needed for diabetes control; rather than focusing on reducing A1C levels, the patient could focus on breathing exercises to improve daily comfort. Additionally, the physician can address barriers that have medical treatment options. For example, if a patient with diabetes has untreated depression, this may create a barrier to effective self-management; treating the depression would help the patient cope more effectively with diabetes. Physicians could include depression assessment and treatment in diabetic care protocols as part of self-management support.
A low level of literacy is another potential barrier to active participation, and addressing health literacy in chronic illness has been associated with better outcomes.21 Asking the patient to repeat information that has been given them is an easy way to identify any misunderstanding.21 Additionally, giving patients clear instructions and information about how to monitor symptoms, use measurement tools, schedule appointments, and take medications makes it much easier for them to participate in setting goals and planning their actions.
PRACTICE CHANGES
Physicians can further support patient self-management by making changes in practice systems. Group visits could be scheduled for interested patients with comparable chronic illnesses (e.g., diabetes, heart disease) so that they can discuss self-managing their illnesses with others who are in similar situations.22 The scheduling of 30- to 45-minute planned individual visits would allow patients and physicians time to address medical management issues such as symptom control and potential complications. This also would allow time for setting goals, creating plans to reach those goals, and solving the challenges of role and emotional management.15 Office staff or other health care professionals can assist patients with planned visit tasks. Self-management support is most effective when it is consistently available from all members of the family practice.10 Disease management guidelines could be used as prompts for patient reminders and to structure planned visits.
Systematic follow-up is another means of providing patients with support. In one controlled study,5 weekly phone calls from a nurse manager and monthly calls from a physician were shown to improve blood sugar control and weight loss in patients with diabetes. In another trial23 involving patients with diabetes, feedback from a touch-screen computer assessment was used to identify key barriers, which were then checked at regular intervals; this was found to increase the efficacy of dietary self-management. It also provides an example of how technology can be used to support self-management of chronic conditions.
Simple time-saving devices, such as ensuring laboratory values are available when patients arrive, reminding patients with diabetes to remove footwear while they are waiting for the physician, having self-management materials on hand, or having ready access to Web-based resources also help support patients.
COMMUNITY INTERVENTIONS
Family physicians can support patient self-management by providing information about community resources such as the local health department, chamber of commerce, and YMCA, as well as local chapters of societies such as the Arthritis Foundation and the American Lung Association. Patients with arthritis have reported improved pain control and mood through participation in programs emphasizing four efficacy-enhancing strategies: mastery of skills through learning and practice, modeling by inspirational role leaders, encouraging participants to attempt more than they are currently doing, and reinterpretation of symptoms to distinguish pain caused by disease from that caused by therapeutic exercise.24 Many community organizations offer exercise programs, self-help groups, patient education classes, and self-management programs. The physician can serve as a conduit for directing patients to these resources, and could make office space available to community groups.
RESOURCES
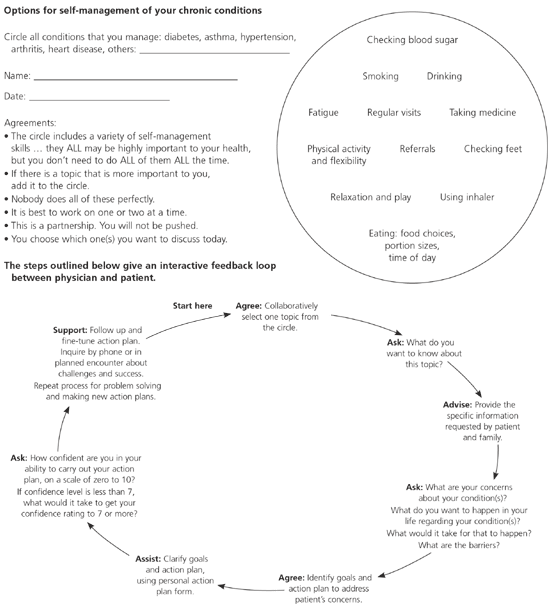
Self-management support tools are available to guide discussion between physician and patient in such a way that the patient determines his or her goal, identifies steps to achieve the goal, identifies barriers to reaching the goal, and plans for overcoming the barriers, including obtaining needed resources.20 The Target Practice model (Figure 2)25,26 can be used to guide the goal-setting conversation and lead the patient toward developing a personal action plan. If the patient reports a low confidence level in accomplishing the action steps (i.e., less than 7 on a scale of zero to 10, with 10 being extremely high confidence and zero being extremely low), the physician-as-partner works with the patient to modify the plan until the patient has a confidence level of 7 or higher.
The Personal Action Plan (Figure 3)27 helps patients with chronic illness to develop a personal plan for learning a new behavior, such as starting a program to increase their physical activity. “Stoplight” tools, such as the Diabetes Zones for Management guide (Figure 4),28 divide various signs and symptoms into green, yellow, and red management zones. Green indicates stability and good control over the condition; yellow indicates caution and suggests steps for regaining control; and red indicates a medical crisis that requires a physician’s attention.


Tools such as these may be particularly important when community resources are limited. Additional guidelines and tools for self-management are available at the Web site of the Institute for Healthcare Improvement (http://www.ihi.org/IHI/Topics/Chronic-Conditions/AllConditions/Tools) and the Improving Chronic Illness Care Web site (http://www.improvingchroniccare.org/tools/criticaltools.html).