A detailed history alone may lead to a specific diagnosis in approximately 70 percent of patients who have wrist pain. Patients who present with spontaneous onset of wrist pain, who have a vague or distant history of trauma, or whose activities consist of repetitive loading could be suffering from a carpal bone nonunion or from avascular necrosis. The hand and wrist can be palpated to localize tenderness to a specific anatomic structure. Special tests can help support specific diagnoses (e.g., Finkelstein’s test, the grind test, the lunotriquetral shear test, McMurray’s test, the supination lift test, Watson’s test). When radiography is indicated, the posterior-anterior and lateral views are essential to evaluate the bony architecture and alignment, the width and symmetry of the joint spaces, and the soft tissues. When the diagnosis remains unclear, or when the clinical course does not improve with conservative measures, further imaging modalities are indicated, including ultrasonography, technetium bone scan, computed tomography, and magnetic resonance imaging. If all studies are negative and clinically significant wrist pain continues, the patient may need to be referred to a specialist for further evaluation, which may include cineroentgenography, diagnostic arthrography, or arthroscopy.
Primary care physicians often are the first to evaluate and treat a patient with wrist pain. Although the wrist consists of a complicated group of bony articulations and soft tissues, many family physicians often use wastebasket diagnoses such as “wrist sprain” or “tendonitis” that do little to identify the true pathology of the condition. Despite the challenges this complex of joints presents, physicians are gaining a better understanding of wrist pathophysiology through an array of diagnostic capabilities.
Generally, the causes of wrist pain can be divided into three categories: mechanical, neurologic, and systemic. Table 11–11 lists common mechanical causes of wrist pain, their clinical presentations, and suggested imaging work-ups. Table 21,2 lists other common causes of wrist pain. Psychosocial factors can also have a profound influence on wrist pain, particularly when the patient may be eligible for workers’ compensation.
TABLE 1 Mechanical Causes of Wrist Pain
| Cause | Clinical presentation | Imaging | |
|---|---|---|---|
| Fracture | History of trauma and bony tenderness | Radiography | |
| Occult fractures identified with delayed radiography, CT, MRI, or bone scan | |||
| Nonunion of scaphoid or hook of the hamate | History of trauma with TTP at the anatomic snuffbox (scaphoid) and the proximal hypothenar area 1 cm distal to flexion crease of the wrist (hamate) | Radiography (“scaphoid view” [scaphoid] or the carpal tunnel and supinated oblique views [hamate]) | |
| MRI | |||
| Avascular necrosis of the scaphoid (Preiser’s disease) or the lunate (Kienböck’s disease) | Variable history of trauma with TTP at the scaphoid or lunate | Delayed radiography | |
| MRI | |||
| Ligament tear | |||
| Triangular fibrocartilage complex | TTP in distal hollow between pisiform and ulnar styloid | MRI | |
| Arthroscopy may be necessary to rule out a false-negative MRI | |||
| Distal radioulnar joint subluxation | Pain, instability with radioulnar “grind” test | Radiography (widened distal radioulnar joint space on PA view—usually normal) | |
| MRI, cineroentgenography, or arthroscopy | |||
| Carpal instability | Midcarpal TTP with a painful and audible “clunk” on ulnar deviation | Cineroentgenography | |
| Scapholunate dissociation | TTP at scapholunate interval | Radiography (“clenched-fist” and supinated oblique views) | |
| De Quervain’s tenosynovitis | TTP along radial aspect of distal radius | Ultrasonography may show synovial thickening | |
| Intersection syndrome | TTP and crepitus along dorsal aspect of distal radius | — | |
| Neoplasm or ganglion | Mass and TTP | Ultrasonography | |
CT = computed tomography; MRI = magnetic resonance imaging; TTP = tenderness to palpation; PA = posterior-anterior. Information from references 1 through 11.
TABLE 2 Additional Causes of Wrist Pain
| Neurologic causes |
| Distal posterior interosseous nerve syndrome |
| Injury of median nerve (carpal tunnel syndrome) |
| Injury of radial nerve |
| Injury of ulnar nerve (Guyon’s canal) |
| Thoracic outlet compression syndrome |
| Systemic causes |
| Amyloidosis |
| Granulomatous disease (e.g., sarcoid, tuberculosis) |
| Hematologic disease (e.g., leukemia, multiple myeloma) |
| Metabolic conditions (e.g., acromegaly, diabetes, gout, hyperparathyroidism, hypocalcemia, hypothyroidism, Paget’s disease, pregnancy, pseudogout) |
| Osteomyelitis |
| Peripheral neuropathy |
| Reflex sympathetic dystrophy (complex regional pain syndrome) |
| Rheumatologic disorders (e.g., psoriasis, rheumatoid arthritis, scleroderma, systemic lupus erythematosus) |
With the dawn of the computer age, wrist and hand pain became the most common complaint involving the upper extremity. The proximal row of bones in the wrist (i.e., scaphoid, lunate, triquetrum, and pisiform) articulate with the distal ends of the radius and ulna in a constrained space to allow three degrees of freedom at the wrist (Figure 1). Relative to the forearm, these hand movements include flexion-extension, pronation-supination, and radial or ulnar deviation. Relative stability of such mobility requires a coordinated system of ligaments, muscles, and tendons.
Figure 1.
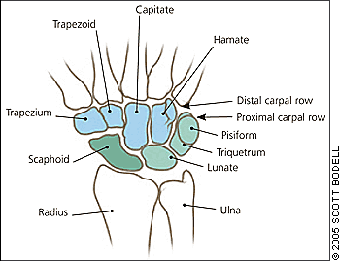
Palmer view of the bones of the left wrist.
Hand and wrist injuries have a major economic impact through health care costs and workers’ compensation claims. A study12 of workers’ compensation claims in Washington state from 1987 to 1995 demonstrated an incidence rate for hand and wrist disorders of 98.2 cases per 10,000 persons, higher than any other musculoskeletal condition related to an industrial injury claim. Furthermore, the average claim was around $7,500.12 For carpal tunnel syndrome alone, direct annual costs in the United States are estimated at $1 billion.13
History
A detailed history alone may lead to a specific diagnosis in approximately 70 percent of wrist pain cases.1 The physician must characterize the precise nature of the pain, including its quality, radiation, severity, and timing, as well as palliative and aggravating factors. In addition, the patient should point with one finger to the most painful area and indicate where the pain radiates.
A mechanical cause of wrist pain is suggested when the wrist has sustained a specific trauma. It is important to have patients describe the injury in their own words; acting out the traumatic event can be particularly useful. The physician must consider the age of the patient when evaluating the mechanism of injury. For example, the injury resulting from a fall on the outstretched hand with wrist extended will vary depending on the patient’s age. This dorsiflexion injury will typically cause a green-stick fracture in a toddler, a growth plate fracture in an adolescent, a scaphoid fracture in a young adult, and a Colles’ (distal radius) fracture in an older adult with osteoporosis.
If the wrist has sustained direct trauma, the nature of the injury must be considered, including the force, frequency, and direction of the event. Direct palmar trauma from swinging a baseball bat or golf club may result in a hook-of-the-hamate fracture (i.e., golfer’s fracture). Patients presenting with a spontaneous onset of wrist pain and a vague or distant history of trauma or repetitive loading activities could be suffering from a carpal bone nonunion or avascular necrosis. The scaphoid and hamate are the most common bones to have nonunion after a fracture because their blood supplies are delicate and prone to complete disruption.14 An idiopathic avascular necrosis usually occurs at the lunate (Kienböck’s disease) or the scaphoid (Preiser’s disease). Symptoms of nonunion and avascular necrosis may not become apparent for years after injury because dead bone fragments cause chronic hypermobility or irritation, which eventually leads to inflammation and arthritis with swelling, pain, and loss of grip strength.1,15
When a patient presents with excessive extension and with ulnar or radial deviation following an acute injury to the wrist, a ligament injury is probable, especially if a clicking or popping sound is present with loading.14 The ligament tears may be partial or complete, depending on the force involved, and mainly occur in the scapholunate (presents as radial deviation and pain) and lunotriquetral (presents as ulnar deviation and pain) ligaments. Physicians should suspect a torn ligament if a patient has pain that appears out of proportion to the injury.16 Ulnar wrist pain and weakness caused by a fall onto an outstretched hand may suggest injury to the triangular fibrocartilage complex (TFCC), which is the primary stabilizer of the distal radioulnar joint. TFCC injury is common in gymnasts and in racquetball, tennis, and hockey players; based on history alone, it is difficult to differentiate from extensor carpi ulnaris, tendonitis, or subluxation.14
Tendinopathy can occur with underlying bony or soft tissue injuries. For example, a tear of the extensor pollicis longus can occur with a minimally displaced distal radius fracture.17 An extensor tendon rupture is common in patients with rheumatoid arthritis, particularly when accompanied by clinically evident extensor tenosynovitis.18,19 A flexor tendon laceration may occur with repetitive attrition of a tendon against a hook-of-the-hamate nonunion.20
If the patient has not experienced a specific trauma, the physician must consider the patient’s vocational and recreational activities for possible causes of mechanical problems. For example, activities requiring forceful grasping with ulnar deviation or repetitive use of the thumb (e.g., caring for a newborn infant, needlepoint, knitting) can lead to de Quervain’s tenosynovitis with pain and swelling along the radial tendons.1,2,14
A thorough and accurate medical history and a review of systems is key to uncovering potential systemic causes of wrist pain. The wrist is often the first site of clinically detectable rheumatoid arthritis.2 Gouty arthritis and pseudogout can involve the wrist joint, although more commonly they affect the lower extremities. Patients with acute septic arthritis usually present with a history of constitutional symptoms or a recent infection and a barely moveable wrist with severe, deep, and unrelenting pain.1 Hypothyroidism, pregnancy, and diabetes are predisposing, but not causal, risk factors for carpal tunnel syndrome. Diabetes also can result in peripheral neuropathy in the hand, which may be misdiagnosed as carpal tunnel syndrome.
Physical Examination
After a detailed history and review of systems, the physician should perform a thorough neurologic and cardiovascular examination including peripheral pulses and examine other joints, particularly the spinal column, when indicated. A comprehensive examination of the neck and entire upper extremity must be performed before conducting the wrist examination to rule out radiating pain from a more proximal problem, such as a herniated cervical disc.
Evaluation of the wrist should begin with identifying erythema, swelling, masses, skin lesions, muscle atrophy, contractures, scars, or other obvious deformities. With acute wrist injury, the severe pain, swelling, non-specific tenderness, and guarding can limit the value of examination. In such cases, if radiographs are normal, the wrist can be splinted and reexamined after a brief immobilization.21 The injured wrist’s active and passive range of motion should be evaluated and compared with the contralateral wrist. Wrist flexion (average maximum, 70 degrees), extension (70 degrees), ulnar deviation (40 degrees), and radial deviation (20 degrees) are evaluated, as well as forearm supination (80 degrees) and pronation (80 degrees).1
The hand and wrist should be palpated to localize the tenderness to a specific location. Knowledge of topographic wrist anatomy is essential (Figure 2). For example, tenderness in the anatomic snuff box may suggest a scaphoid fracture or Preiser’s disease, whereas lunate tenderness may indicate Kienböck’s disease. Tenderness in the scapholunate interval (localized 1.5 cm distal to Lister’s tubercle in the distal radius) may suggest scapholunate dissociation. Tenderness in the distal carpal row may indicate nonunion of the hook of the hamate, which is localized in the proximal hypothenar area (1 cm distal to the flexion crease of the wrist). The mid-carpal area is a series of joints between the proximal and distal carpal rows. Tenderness in this area could indicate a midcarpal strain, instability, or possible arthritis of the scaphotrapeziotrapezoid joint. Midcarpal instability also presents as a painful and audible “clunk” with ulnar deviation.1,14,22
Figure 2.
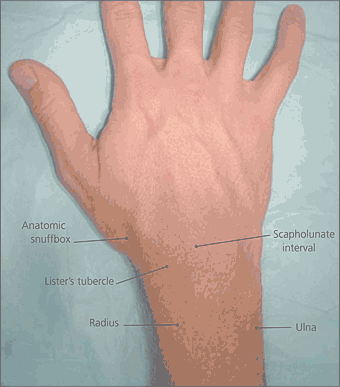
Anatomy of the wrist (dorsal view).
Next, the distal radius and ulna should be palpated along with the articulation between the two bones (i.e., the distal radioulnar joint). Bony tenderness or palpable step-offs can signify a fracture or nonunion. The grind test (i.e., compression of the distal ulnar and radial heads with forearm rotation) may identify distal radioulnar joint instability.14 Tenderness along the lateral aspect of the distal radius can indicate de Quervain’s tenosynovitis.22 Tenderness and crepitus along the dorsal aspect of the distal radius may indicate intersection syndrome (i.e., a bursal inflammation of the intersecting tendons of the radial wrist extensors and thumb abductor tendons).22Tenderness over the ulnar styloid can indicate a fracture or nonunion, whereas tenderness immediately distal in the hollow between the pisiform and ulnar styloid usually indicates a TFCC injury. Table 31,2,21–23 outlines the methods and utility of tests that can help support specific diagnoses.
TABLE 3 Special Maneuvers to Diagnose Wrist Pain
| Maneuver | Method | Utility |
|---|---|---|
| Finkelstein’s test | Provide ulnar deviation to the wrist while grasping the thumb. | Pain over radial styloid from this provocative stretch maneuver differentiates de Quervain’s tenosynovitis from arthritis of the first metacarpal. |
| Grind tests | Compress and rotate the first metacarpal bone along the trapezium. | Pain and crepitus from this provocative compression maneuver suggests arthritis or instability. |
| Compress and rotate the distal radioulnar joint. | ||
| Lunotriquetral shear test | Apply dorsal force to triquetrum and palmar force over lunate. | A painful “click” reveals a lunotriquetral ligament tear. |
| McMurray’s test | Manipulate the triquetrum against the head of the ulna with the wrist in ulnar deviation. | Pain, crepitus, or a snap identifies TFCC lesions. |
| Supination lift test | Ask the patient to lift examination table with palm flat on underside of table or to lift himself off of the table. | Pain and weakness indicate a TFCC injury. |
| Watson’s test (scaphoid shift test) | Press the scaphoid tuberosity on the palmar aspect while moving the wrist from ulnar to radial deviation. | A painful “click” or “pop” identifies scaphoid instability or scapholunate separation. |
TFCC = triangular fibrocartilage complex.
Psychosocial factors such as secondary gain also must be considered when evaluating wrist pain, particularly in patients who could receive workers’ compensation. Factitious injury should be suspected when the patient demonstrates subjective pain that is disproportionate to objective findings and if the examination reveals diffuse tenderness throughout the entire upper extremity in a nonanatomic pattern. A small cohort study23 has shown that the potential for financial workers’ compensation is inversely related to the likelihood of symptom resolution, and positive physical findings may be absent in up to 75 percent of persons who are financially compensated for their pain.23 Other red flags for severe psychologic morbidity include weakness inconsistent with muscle bulk, pain on the nondominant side, pain associated with ecchymosis, chronic swelling, and unexplained ulceration or open wounds.1
Imaging
Radiography is the first-line imaging modality for wrist pain, although it is not always indicated. Posterior-anterior (PA) and lateral radiographic views are essential to evaluate the bony architecture and alignment of the wrist, the width and symmetry of the joint spaces, and the soft tissues. For example, the lateral view assesses the radiolunocapitate alignment, which should be collinear, and the radioscaphoid, lunoscaphoid, and capitoscaphoid relations.2 Misalignment implies the presence of an interosseous ligament tear, which can progress to carpal instability, chronic osteoarthritis, advanced collapse, and chronic pain. When a scaphoid fracture or non-union is suspected, a scaphoid view should be obtained in addition to the routine views. The wrist should be prone in ulnar deviation with 30 degrees of supination for the scaphoid view, because ulnar deviation in the PA position elongates the scaphoid and improves detection of subtle fractures (Figure 3).3,4 Unfortunately, 20 percent of radiographs are initially negative for scaphoid fractures regardless of the view.2 Therefore, scaphoid fracture should be presumed in cases of anatomic snuff-box tenderness, and the patient should be treated with appropriate immobilization and follow-up radiographs two to three weeks after injury.3,5 When a fracture of the hook of the hamate is suspected, physicians should include the carpal tunnel and supinated oblique views. Stress views, such as the “clenched-fist” view and the supinated view in ulnar deviation, can help identify scapholunate dissociation14 (Figure 4).
Figure 3.
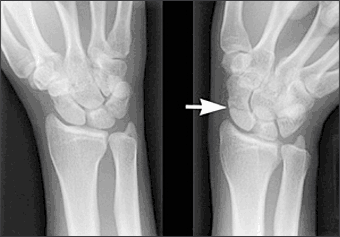
Routine (left) and scaphoid (right) views of non-displaced wrist fracture (arrow).
Figure 4.
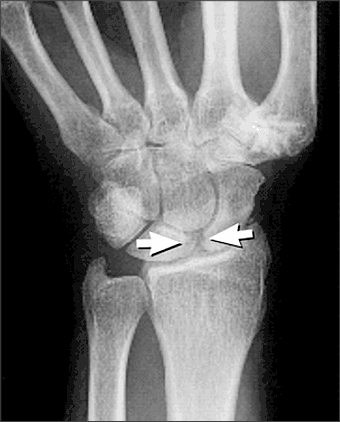
Scapholunate dissociation (arrows).
If the diagnosis remains unclear after radiography, or if the clinical course does not improve with conservative measures, further imaging modalities are indicated. For suspected mechanical pathology such as an occult ganglion, an occult fracture, nonunion, or bone necrosis, the physician must choose from several modalities (e.g., ultrasonography, technetium bone scan, computed tomography [CT], or magnetic resonance imaging [MRI]). Ultrasonography is a quick and accessible way to assess soft-tissue abnormalities such as tendon injury, synovial thickening, ganglia, and synovial cysts. However, the effectiveness of this modality is highly operator dependent, and it does not effectively assess the complex bony architecture.2,6 Bone scans can detect osteoblastic activity and have high sensitivity and low specificity.7 Bone scans also can identify early stress injuries and can effectively rule out a scaphoid fracture. However, MRI may be equally sensitive and more specific than a bone scan.8,9 CT can evaluate fractures and articular subluxations not identified by routine radiography;4 however, MRI may be more effective in evaluating soft tissue injuries (e.g., muscle, ligament, cartilage, and bony lesions).10,11 For example, subtle ligament injuries such as complete scapholunate ligament tears are more effectively identified with MRI than with CT.14 If all imaging results are negative, but clinically significant wrist pain persists, the physician should consider referring the patient to a specialist for further evaluation, which may include cineroentgenography (dynamic real-time imaging under fluoroscopy), a diagnostic arthrography, or arthroscopy.

