The trend of body piercing at sites other than the earlobe has grown in popularity in the past decade. The tongue, lips, nose, eyebrows, nipples, navel, and genitals may be pierced. Complications of body piercing include local and systemic infections, poor cosmesis, and foreign body rejection. Swelling and tooth fracture are common problems after tongue piercing. Minor infections, allergic contact dermatitis, keloid formation, and traumatic tearing may occur after piercing of the earlobe. “High” ear piercing through the ear cartilage is associated with more serious infections and disfigurement. Fluoroquinolone antibiotics are advised for treatment of auricular perichondritis because of their antipseudomonal activity. Many complications from piercing are body-site–specific or related to the piercing technique used. Navel, nipple, and genital piercings often have prolonged healing times. Family physicians should be prepared to address complications of body piercing and provide accurate information to patients.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Persons contemplating tongue piercing should be advised of the high incidence of tooth chipping associated with such piercings. | C | 2 |
| Rinsing with nonprescription oral cleansers (e.g., Listerine) or topical application of cleansers (e.g., Gly-Oxide) is recommended to prevent infection after oral piercing. | C | 17 |
| Antibiotics with good coverage against Pseudomonas and Staphylococcus species (e.g., fluoroquinolones) should be used when treating piercing-associated infections of the auricular cartilage. | C | 7, 18, 19 |
| Earrings with locking or screw-on backs are recommended for infants and young children because of the risk of ingestion or aspiration. | C | 29 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1949 or https://www.aafp.org/afpsort.xml.
In recent years, body piercing has increased in popularity and social acceptance. Piercing of various body parts with jewelry is no longer limited to teenagers, as evidenced by the growing number of adults with multiple ear piercings. Family physicians should be familiar with body piercing practices and associated health risks (Table 11–14). No reliable estimates are available for the number of persons who have experienced complications related to body piercing. Persons with increased vulnerability to infection (e.g., patients with diabetes, patients taking corticosteroids) and those who have an increased likelihood of hemorrhage (e.g., persons taking anticoagulant medication) may be at greater risk of complications from body piercing.
TABLE 1 Potential Complications of Body Piercings
| Piercing site | Potential complications |
|---|---|
| Ear | Allergic reaction, auricular perichondritis, embedded earrings, infection, keloid formation, perichondral abscess, traumatic tear |
| Genitals (women) | Allergic reaction, compromise of barrier contraceptives, infection, keloid formation |
| Genitals (men) | Frictional irritation, infection, paraphimosis, penile engorgement, priapism, recurrent condyloma, urethral rupture, urethral stricture, urinary flow interruption |
| Mouth | Airway compromise, altered eating habits, gingival trauma, hematoma formation, increased salivary flow, infection, injury to salivary glands, interference with radiographs, loss of taste, Ludwig’s angina, pain, permanent numbness, speech impediments, tooth fracture or chipping, uncontrolled drooling |
| Navel | Bacterial endocarditis,* frictional irritation, infection, jewelry migration and rejection |
| Nipples | Abscess formation, bacterial endocarditis,* breastfeeding impairment, infection |
| Nose | Infection, jewelry swallowing or aspiration, perichondritis and necrosis of nasal wall, septal hematoma formation |
*— In patients with moderate- to high-risk cardiac conditions.
Body Piercing Jewelry
Most body piercing jewelry consists of rings, hoops, studs, or barbell-shaped ornaments. The size and shape of jewelry is determined by the body site pierced and personal preferences. Jewelry is not always interchangeable between piercing sites. In particular, jewelry designed for ear piercing may not be suitable for another part of the body because of the length of the post or the pressure exerted by the clasp.
Most body piercing jewelry is made of metal, usually stainless steel, gold, niobium, titanium, or alloys. Surgical stainless steel rarely causes allergic skin reactions; however, not all stainless steel products are nickel-free.15 Gold often is combined with nickel or other metals to make alloys that have improved hardness and durability. Nickel in gold-filled or gold-plated jewelry is associated with a high prevalence of reactivity in persons who are nickel sensitive. Consumers must pay careful attention to the stud or clasp on earrings; jewelry with a high karat rating commonly is paired with less expensive gold-plated studs or earring backs. Niobium and titanium are light-weight elemental metals that rarely produce an allergic response. Other features to consider in body piercing jewelry include ease of removal (in case of trauma or radiographs), surface smoothness, and its capacity to with-stand autoclaving and cleaning.
Oral Piercings
The lips, cheeks, and midline of the tongue are popular sites for oral piercings. Perforation of lingual blood vessels can cause bleeding and hematoma formation. Edema frequently develops after tongue piercing, so a longer barbell is recommended initially.16
Another serious consequence of oral piercing is compromise of the airway from trauma, tongue swelling, or obstruction by jewelry.1 Securing an adequate airway or endotracheal intubation can be challenging when a patient has a tongue barbell. If lingual jewelry cannot be removed easily or expeditiously, precautions should be taken during intubation to ensure that jewelry is not loosened and aspirated or swallowed. Removal of oral and nasal jewelry also is recommended before nonemergent surgical procedures.
DENTAL COMPLICATIONS
Chipping (or fracture) of teeth is the most common dental problem related to tongue barbells (Figure 1).2 Switching to a shorter barbell reduces damage to the dentition and gingiva. Beaded jewelry may become trapped between teeth.
Figure 1 Tongue barbell with an acrylic ball.
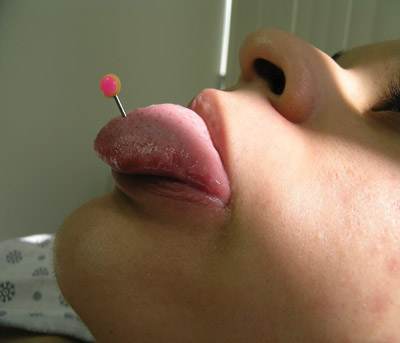
Although there is a risk of infection because of the vast amounts of bacteria in the mouth, the infection rate actually is low. Oral rinses (e.g., Listerine) or application of nonprescription cleansers (e.g., Gly-Oxide) may be recommended prophylactically after oral piercing.17 Ludwig’s angina is rare, but this rapidly spreading oral cellulitis has been reported as a complication of tongue piercing.5 Treatment involves maintaining an adequate airway, administration of systemic antibiotics, and surgical drainage of abscesses.
Ear Piercings
INFECTIOUS COMPLICATIONS
The ear is the most common site for body piercing. In one study,6 up to 35 percent of persons with pierced ears had one or more complications (e.g., minor infection [77 percent], allergic reaction [43 percent], keloid formation [2.5 percent], and traumatic tearing [2.5 percent]).
Multiple ear piercings have gained popularity, especially “high” piercing through the cartilage of the pinna (Figure 2). These piercings are associated with poor healing and more serious infection because of the avascular nature of auricular cartilage. Auricular perichondritis and perichondrial abscess typically occur in the first month after piercing, especially during warm-weather months.7 Auricular perichondritis presents as painful swelling, warmth, and redness in a portion of the auricle that often spares the earlobe. Acute tenderness on deflecting the auricular cartilage helps distinguish this deeper perichondrial infection from a superficial skin infection. Minor infections can progress to perichondritis, abscess formation, and necrosis with or without systemic symptoms. The most common pathogens (i.e., Pseudomonas aeruginosa, Staphylococcus aureus, and Streptococcus pyogenes) respond well to fluoroquinolone antibiotic treatment (e.g., ciprofloxacin [Cipro]).18, 19 If an abscess is present, surgical incision and drainage often are necessary. Once an abscess develops, good cosmetic preservation of the auricular cartilage is difficult to maintain.
Figure 2 “High” ear piercing through the cartilage.
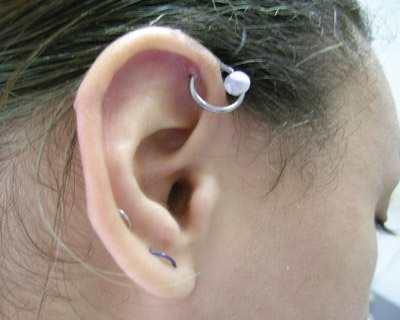
Persons with atopic dermatitis or allergic metal contact dermatitis are at increased risk for developing minor staphylococcal or streptococcal skin infections.20 A localized infection of the earlobe may not be easily differentiated from allergic contact dermatitis unless there is purulent drainage or a high index of suspicion.21 Superficial earlobe infections tend to have a benign course and respond well to local treatment, including warm, moist packs and application of over-the-counter topical antibiotic ointment. Treatment with 2 percent mupirocin ointment (Bactroban) or oral antistaphylococcal antibiotics may be warranted.
NONINFECTIOUS COMPLICATIONS
The earlobe is a common site for hypertrophic scarring and keloid formation. In addition to aesthetic concerns, patients with keloids may have itching and tenderness. Treatment options for keloids include surgical excision, intralesional corticosteroid injections, cryosurgery, pressure dressing, radiation, and laser therapy.22,23
Contact dermatitis resulting from nickel exposure is common. Contact sensitivity to gold and localized argyria, a skin discoloration resulting from silver salts, also have been described.21,24 Avoidance of the metals that trigger a reaction and application of topical corticosteroids hasten the resolution of allergic dermatitis.
Occasionally, inflammation or infection results in such significant swelling that an earring must be removed. The pierced hole can be maintained by inserting a ring made from a 20-gauge Teflon catheter with silicone tubing into the hole while the surrounding skin heals.25 Similarly, a loop fashioned from nylon suture material may keep a piercing intact during the healing process.
Earrings can become embedded in the earlobe, a complication common in persons with thick, fleshy earlobes that are pierced with spring-loaded guns.26 Piercing guns exert high pressure on the soft tissue of the earlobe and cannot be adjusted for varying tissue thickness. Embedding may be prevented by using longer earring posts with adjustable backings.
If gentle probing fails to locate an embedded ear-ring, a small incision under local anesthesia (without epinephrine) may be necessary to locate and remove the earring or backing. Any suspected infection should be treated. Over-the-counter topical antimicrobials (e.g., bacitracin, Polysporin, Neosporin) are indicated for treatment of superficial skin infections. Oral antibiotics such as the first-generation cephalosporins (e.g., cephalexin [Keflex], cefadroxil [Duricef]) and penicillinase-resistant penicillins (e.g., dicloxacillin [Dynapen]) are appropriate treatment options for more serious wound infections. An earring can be replaced or the ear repierced six to eight weeks after resolution of local swelling and tenderness.21
Trauma to the pierced external ear is common. Lacerations to the ear may occur after falls, motor vehicle crashes, contact sports, person-to-person violence, or accidental pulling of an earring. The simplest laceration occurs when an earring is pulled through the earlobe, especially if the original earring hole was close to the periphery (Figure 3) . Prolonged wearing of heavy jewelry also may result in an elongated tract or bifid deformity of the earlobe.
Figure 3 Traumatic tear of the earlobe.
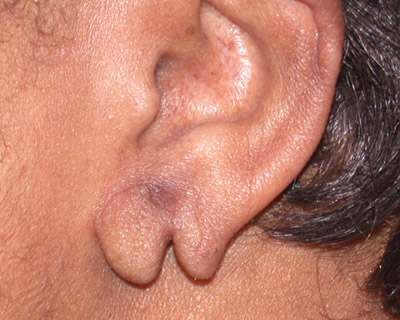
All wounds should be cleaned and repaired within 12 to 24 hours. A simple ear lobe tear can be sutured under local anesthesia. If the hole has closed, the ear lobe can be repierced in a nonscarred area after approximately three months.27 Various closure techniques have been described in the literature28 for more complex lacerations of ear cartilage. Many family physicians refer these complicated injuries to subspecialists for repair.
Pointed earring posts may cause pressure sores or postauricular skin irritation when worn during sleep. Removal of jewelry at bedtime is indicated if switching to a different ear-ring style does not resolve the problem. Parents of infants or young children with pierced ears should be informed of the risk of aspiration and ingestion of earring parts. In such situations, earrings with a locking back or screw back are advisable.29
Family physicians play an important role in promoting injury prevention by recommending that all jewelry be removed during contact sports to avoid endangering the wearer and other players. If body jewelry remains comfortable and does not produce frictional irritation, athletes should be able to keep the jewelry in place during noncontact personal workouts.30 Jewelry that interferes with mouthguards or protective equipment should be removed before play.
Nose Piercing
The nose can be pierced in the fleshy nares or through the cartilaginous septum. Septal piercings usually are performed in the inferior fleshy part of the septum and not through cartilaginous tissue. Piercing the cartilage can cause significant bleeding and lead to septal hematoma formation that often is accompanied by infection. Other potential complications that may result in cosmetic deformity include perichondritis and necrosis of the cartilaginous nasal wall. Infection requires aggressive treatment with antibiotics that have good coverage against Staphylococcus species that commonly colonize the nasal mucosa. Mupirocin is effective and offers excellent coverage against gram-positive cocci. Fluoroquinolones have the advantage of excellent skin penetration and added coverage against Pseudomonas species.
Nasal jewelry has the potential to be aspirated or swallowed. Rings placed in the nostril or septum also can migrate forward or be pulled out. As with ear piercing, the studs or backings of the jewelry may become embedded and require surgical removal.31
The navel or periumbilical area is a popular self-piercing site. Friction from clothing with tight-fitting waist-bands and subsequent skin maceration may account for the delayed healing and increased infection rates of navel piercings (Table 28,9). Careful placement of jewelry and avoidance of rigidly fixed jewelry may minimize these problems.
TABLE 2 Approximate Healing Times for Body Piercing Sites
| Site (piercing name) | Time to heal |
|---|---|
| Clitoris | 2 to 6 weeks |
| Coronal ridge (dydoe) | 6 to 8 weeks |
| Ear lobe and auricle | 6 to 8 weeks |
| Eyebrow | 6 to 8 weeks |
| Glans penis (ampallang) | 3 to 9 months |
| Labia majora | 2 to 4 months |
| Labia minora | 2 to 6 weeks |
| Lip | 6 to 8 weeks |
| Navel | Up to 9 months |
| Nipple | 2 to 4 months |
| Scrotum (hafada) | 2 to 3 months |
| Tongue | 3 to 6 weeks |
| Urethral meatus (Prince Albert) | 2 to 4 weeks |
Superficial navel piercings often tend to migrate to the skin surface. The problem of jewelry migration and rejection is compounded by wearing heavily weighted, thin-gauge jewelry. Migration of navel rings and subsequent scarring are more problematic in overweight patients and in the latter stages of pregnancy as abdominal girth expands (Figure 4) . Wearing a curved barbell instead of a ring until the navel piercing has healed may reduce irritation and scarring.
Figure 4 Hypertrophic scarring that developed after a navel ring began to migrate to the skin’s surface during the third trimester of pregnancy.
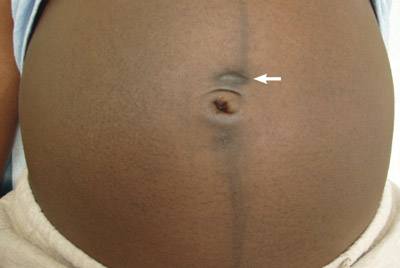
Nipple Piercing
Before nipple and areolae piercings, men and women should be counseled about the lengthy time required for complete healing and the risk of delayed infection. Abscess formation has been reported following nipple piercing.10 Except for case reports of cellulitis and spread of infection around an implant,32,33 little information is available about nipple piercing after breast implantation or chest wall augmentation. The effects of nipple piercings on lactation are not clear, but jewelry or scar tissue could impair latching on or block a milk duct and adversely affect an infant’s ability to breastfeed.
Genital Piercings
Genital piercings reportedly enhance sexual sensitivity. Piercing sites in men include the penile glans and urethra, foreskin, and scrotum; sites in women include the clitoral prepuce or body, labia minora, labia majora, and perineum.34
PIERCINGS IN MEN
Jewelry inserted through the glans penis often interrupts urinary flow. Paraphimosis (i.e., the inability to replace a retracted foreskin) has been associated with urethral and glans piercings in uncircumcised men.11 The foreskin may be reduced manually after a penile nerve block. If this maneuver is unsuccessful, the prepuce can be injected with hyaluronidase (Vitrase) to allow the edematous fluid to dissipate.35 Penile rings also can cause engorgement and priapism (i.e., persistent erection), requiring emergency treatment to preserve erectile function.
PIERCINGS IN WOMEN
Women with genital piercings can develop bleeding, infections, allergic reactions, keloids, and scarring.12 Sexually active persons with genital piercings should be counseled that jewelry may compromise the use of barrier contraceptive methods. Condoms may be more prone to break and diaphragms may be more easily dislodged during sexual activity when one or both partners have genital piercings. Avoiding jewelry with sharp edges and using looser-fitting condoms or double condoms may help avoid some of these problems.36
Systemic Infectious Complications
The American Heart Association guidelines on endocarditis prophylaxis37 do not specifically address the need for antibiotics in persons contemplating ear or body piercings. One small study38 of children and adults with congenital heart disease found no cases of endocarditis after ear piercing, even though only 6 percent of patients received prophylactic antibiotic treatment. Recent reports13,14 of bacterial endocarditis after nipple and navel piercings in patients with surgically corrected congenital heart disease should prompt physicians to consider antibiotic prophylaxis in patients with moderate- or high-risk cardiac conditions.
With any piercing, there is the danger of infection, including hepatitis B or C virus and tetanus.8 Body piercing as a possible vector for human immunodeficiency virus transmission has been suggested.39 Nonsterile piercing techniques and poor hygiene contribute significantly to the increased risk of infection. Although earrings may be sterilized before use, most piercing “guns” are not sterilized between procedures. Ear piercing systems using disposable sterile cassettes are available.
Family physicians should help patients make informed decisions about body piercings and counsel them about the importance of universal precautions. Physicians should remain nonjudgmental so that patients are not reluctant to report a problem. Because body piercing salons are unregulated in many states, some physicians may choose to perform body piercing procedures in the office setting.

