Constipation is a common complaint in older adults. Although constipation is not a physiologic consequence of normal aging, decreased mobility and other comorbid medical conditions may contribute to its increased prevalence in older adults. Functional constipation is diagnosed when no secondary causes can be identified, such as a medical condition or a medicine with a side effect profile that includes constipation. Empiric treatment may be tried initially for patients with functional constipation. Management of chronic constipation includes keeping a stool diary to record the nature of the bowel movements, counseling on bowel training, increasing fluid and dietary fiber intake, and increasing physical activity. There are a variety of over-the-counter and prescription laxatives available for the treatment of constipation. Fiber and laxatives increase stool frequency and improve symptoms of constipation. If constipation is refractory to medical treatment, further diagnostic evaluation may be warranted to assess for colonic transit time and anorectal dysfunction. Alternative treatment methods such as biofeedback and surgery may be considered for these patients.
Constipation is common in older adults and accounts for about 2.5 million physician office visits annually.1 The estimated prevalence of constipation varies from 22 to 28 percent,3 and the number of persons reporting constipation increases with age.4 Constipation is more common in women, blacks, persons from lower socioeconomic levels,4 and persons living in rural areas and northern states.5
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Review the patient’s medication list to evaluate for medications that may cause constipation. | C | 15 |
| Encourage patients to attempt to have a bowel movement soon after waking in the morning or 30 minutes after meals to take advantage of the gastrocolic reflex. | C | 18 |
| Increasing dietary fiber intake to 25 to 30 g daily may improve symptoms of constipation. | C | 19 |
| Encourage physical activity to improve bowel regularity. | B | 21,24,25 |
| If nonpharmacologic approaches fail, recommend increased fiber intake and/or laxatives to increase bowel movement frequency and improve symptoms of constipation. | B | 26 |
| Biofeedback therapy is the treatment of choice for anorectal dysfunction. | B | 43 |
| Surgery is reserved for persistent and intractable constipation in patients who have been evaluated and proven to have slow transit constipation. | B | 42,44 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 2160 orhttps://www.aafp.org/afpsort.xml.
In clinical practice, constipation is generally defined as fewer than three bowel movements per week. A working group of experts at an international congress of gastroenterology developed a consensus definition of constipation, known as the Rome II criteria (Table 16).
TABLE 1 Rome II Criteria for Defining Chronic Functional Constipation in Adults
| Two or more of the following for at least 12 weeks in the preceding 12 months: | |
| Straining in more than 25 percent of defecations | |
| Lumpy or hard stools in more than 25 percent of defecations | |
| Sensation of incomplete evacuation in more than 25 percent of defecations | |
| Sensation of anorectal obstruction or blockade in more than 25 percent of defecations | |
| Manual maneuvers (e.g., digital evacuation, support of the pelvic floor) to facilitate more than 25 percent of defecations | |
| Fewer than three defecations per week | |
Adapted with permission from Thompson WG, Longstreth GF, Drossman DA, Heaton KW, Irvine EJ, Muller-Lissner SA. Functional bowel disorders and functional abdominal pain. Gut 1999;45(suppl 2):II45.
Causes of Constipation
Constipation is not a physiologic consequence of normal aging. Many age-related problems (e.g., decreased mobility, comorbid medical conditions, increased use of medications with a side effect profile that includes constipation, and changes in diet) may contribute to the increased prevalence of constipation in older adults. A thorough medical history and physical examination are needed to exclude constipation secondary to an underlying condition. Constipation can be divided into primary and secondary causes.
PRIMARY CONSTIPATION
Primary causes of constipation can be classified into three groups: normal transit constipation, slow transit constipation, and anorectal dysfunction. Normal transit constipation, also known as functional constipation, is the most common. In patients with functional constipation, stool passes through the colon at a normal rate. Slow transit constipation is characterized by prolonged delay in the passage of stool through the colon.7 Patients may complain of abdominal bloating and infrequent bowel movements.8 The causes for slow transit constipation are unclear; the postulated mechanisms include abnormalities of the myenteric plexus, defective cholinergic innervation, and anomalies of the noradrenergic neuro-muscular transmission system.7 Anorectal dysfunction is the inefficient coordination of the pelvic musculature in the evacuation mechanism.9 These patients are more likely to complain of a feeling of incomplete evacuation, a sense of obstruction, or a need for digital manipulation.8 Anorectal dysfunction may be an acquired behavioral disorder, or the process of defecation may not have been learned in childhood.10
SECONDARY CONSTIPATION
Table 211–13 lists medical and psychiatric conditions that are potential causes of secondary constipation. These conditions may be excluded by a thorough history and physical examination. A consensus guideline14 from the American Gastroenterological Association (AGA) also recommends that most patients have tests for a complete blood count and serum glucose, thyroid stimulating hormone, calcium, and creatinine levels. A sigmoidoscopy or colonoscopy to exclude colon cancer is indicated in patients older than 50 years who have not had a recent examination and in those with concomitant rectal bleeding or weight loss.
TABLE 2 Causes of Secondary Constipation
Endocrine and metabolic diseases
|
An important secondary cause of constipation is the use of medications, especially those that affect the central nervous system, nerve conduction, and smooth muscle function. The most common medicines associated with constipation are listed in Table 3.11 In a study15 of patients who considered themselves constipated, 40 percent were using medications known to cause constipation. Over-the-counter medications, such as calcium- or aluminum-containing antacids and iron supplements, may also cause constipation.
TABLE 3 Medications Commonly Associated with Secondary Constipation
| Antacids* | |
| Anticholinergics | |
| Antidepressants | |
| Antihistamines | |
| Calcium channel blockers | |
| Clonidine (Catapres) | |
| Diuretics | |
| Iron | |
| Levodopa (Larodopa) | |
| Narcotics | |
| Nonsteroidal anti-inflammatory drugs | |
| Opioids | |
| Psychotropics | |
| Sympathomimetics |
*—Antacids containing aluminum or calcium.
Adapted with permission from Prather CM, Ortiz-Camacho CP. Evaluation and treatment of constipation and fecal impaction in adults. Mayo Clin Proc 1998;73:882.
Irritable bowel syndrome is a common cause of constipation. It can be distinguished from functional constipation because it is usually accompanied by cramps and lower abdominal pain that are typically relieved by defecation, and by periods of diarrhea.
Overview of Constipation Treatment
If a medication or a medical condition is the cause of constipation, eliminating the offending medication or treating the underlying medical condition may relieve the constipation. However, certain conditions require the use of a medication despite its side effects. Although opioid therapy almost always causes some degree of constipation, individual opioids induce constipation to different degrees. One study16 found that fentanyl (Duragesic) was less likely to cause constipation than oral morphine. In most cases, a prophylactic laxative should be considered when prescribing chronic opioid therapy because tolerance to the constipating effects of opioids does not develop over time.
When no secondary cause of constipation is identified, empiric treatment should be tried initially for functional constipation. Management should begin with nonpharmacologic methods to improve bowel regularity and should proceed to the use of laxatives if nonpharmacologic methods are not successful. If the constipation is refractory to medical treatment, the patient should be referred to a specialist for further diagnostic evaluation. This may include measurement of colonic transit time, anorectal manometry, defecography, or a balloon expulsion test to assess colonic transit and anorectal function. In rare cases, biofeedback therapy or surgery may be warranted.14
Nonpharmacologic Treatments
A stool diary may be helpful for some patients to record the nature of the complaint in terms of stool frequency, consistency, size, and degree of straining. Many patients incorrectly believe that they need to have a bowel movement every day; counseling on simple lifestyle changes may improve their perception of bowel regularity. Most importantly, patients should be educated on recognizing and responding to the urge to defecate.
BOWEL TRAINING
Having a bowel movement may be partly a conditioned reflex. One study17 showed that most patients with a regular bowel pattern empty their bowels at approximately the same time every day. The optimal times to have a bowel movement typically are soon after waking and after meals, when colonic activity is greatest.18 Patients should be encouraged to attempt defecation first thing in the morning, when the bowel is more active, and 30 minutes after meals, to take advantage of the gastrocolic reflex.
DIETARY FIBER INTAKE
Inadequate fiber intake is a common reason for constipation in Western society. Studies19 have shown that increased dietary fiber intake leads to decreased colonic transit time and to bulkier stools. A dietary diary may be helpful to assess whether an adequate amount of fiber is consumed daily. Most healthy Americans consume 5 to 10 g of fiber daily.12 The daily recommended fiber intake is 20 to 35 g daily.12 If fiber intake is substantially less than this, patients should be encouraged to increase their intake of fiber-rich foods such as bran, fruits, vegetables, and nuts. Prune juice is commonly used to relieve constipation. The recommendation is to increase fiber by 5 g per day each week until reaching the daily recommended intake.12 Adding fiber to the diet too quickly may cause excessive gas and bloating.
FLUID INTAKE
Adequate hydration is considered to be important in maintaining bowel motility. However, despite the belief that a lack of fluid increases the risk of constipation, few studies have provided evidence that hydration is associated with the incidence of constipation.20 Decreased fluid intake may play a greater role in the development of fecal impaction.21
REGULAR EXERCISE
The National Health and Nutrition Examination Survey22 found that a low physical activity level is associated with a twofold increased risk of constipation. Another epidemiologic study23 showed that patients who are sedentary are more likely to complain of constipation. Prolonged bedrest and immobility are often associated with constipation. Although patients should be encouraged to be as physically active as possible, there is no consistent evidence that regular exercise relieves constipation.24 However, the Nurses’ Health Study,25 which followed a cohort of 62,036 women, found that physical activity two to six times per week was associated with a 35 percent lower risk of constipation.
Pharmacologic Treatment
A systematic review26 found that increased fiber intake and the use of laxatives improved the frequency of bowel movements compared with placebo in adults. However, the data concerning the superiority of individual treatments were inconclusive because of the limited number of studies, small sample size, or methodologic flaws.26There also are limited data about long-term benefits and risks of laxatives and fiber preparations.26 The formulations, dosages, and costs of commonly used laxatives, stool softeners, and prokinetic agents are listed in Table 4.27 There are no evidence-based guidelines on the preferred order of using different types of laxatives; however, the AGA has developed a treatment algorithm for patients with functional, normal transit constipation (Figure 1).14
TABLE 4 Medications for Treatment of Chronic Constipation
| Agent | Formula/strength | Adult dosage | Cost* |
|---|---|---|---|
| Bulk laxatives | |||
| Methylcellulose (Citrucel) | Powder: 2 g (mix with 8 oz liquid) | One to three times daily | $13.05 for 840 g |
| Tablets: 500 mg (take with 8 oz liquid) | 2 tablets up to six times daily | $20.76 for 164 tablets | |
| Polycarbophil (Fibercon) | Tablets: 625 mg | 2 tablets one to four times daily | $10.80 for 90 tablets |
| Psyllium (Metamucil) | Powder: 3.4 g (mix with 8 oz liquid) | One to four times daily | $12.55 for 870 g |
| Stool Softeners | |||
| Docusate calcium (Surfak) | Capsules: 240 mg | Once daily | $16.92 for 100 capsules |
| Docusate sodium (Colace) | Capsules: 50 or 100 mg | 50 to 300 mg† | 50 mg: $14.50 for 60 capsules 100 mg: $17.71 for 60 capsules |
| Liquid: 150 mg per 15 mL | Liquid: $7.90 for 30 mL | ||
| Syrup: 60 mg per 15 mL | Syrup: $21.66 for 473 mL | ||
| Osmotic laxatives | |||
| Lactulose | Liquid: 10 g per 15 mL | 15 to 60 mL daily† | $36.35 for 480 mL |
| Magnesium citrate | Liquid: 296 mL per bottle | 0.5 to 1 bottle per day | $2.29 for 296 mL |
| Magnesium hydroxide (Milk of Magnesia) | Liquid: 400 mg per 5 mL | 30 to 60 mL once daily† | $2.64 for 12 fl oz |
| Polyethylene glycol 3350 (Miralax) | Powder: 17 g (mix with 8 oz liquid) | Once daily | $25.34 for 12 packets |
| Sodium biphosphate (Phospho-Soda) | Liquid: 45 mL, 90 mL (mix with 4 oz water, then follow with 8 oz water | 20 to 45 mL daily | $2.65 for 90 mL |
| Sorbitol | Liquid: 480 mL | 30 to 150 mL daily | $7.57 to $25 for 480 mL |
| Stimulant laxatives | |||
| Bisacodyl (Dulcolax) | Tablets: 5 mg | 5 to 15 mg daily | $13.46 for 100 tablets |
| Cascara sagrada | Liquid: 120 ml | 5 mL once daily | $3.75 for 120 mL |
| Tablets: 325 mg | 1 tablet daily | $4.50 for 100 tablets | |
| Castor oil | Liquid: 60 ml | 15 to 60 mL once daily† | $8.35 for 120 mL |
| Senna (Senokot) | Tablets: 8.6 mg | 2 or 4 tablets once or twice daily | $21.04 for 100 tablets |
| Prokinetic Agents | |||
| Tegaserod (Zelnorm) | Tablets: 2 mg, 6 mg | Two times daily‡ | $169.15 for 60 tablets 2 mg or 6 mg |
*—Average wholesale cost, based on Red Book. Montvale, N.J.: Medical Economics Data, 2005. Costs listed are brand name versions; generic versions are available for some of these medications.
†—May be taken in divided doses.
‡—Used for constipation related to irritable bowel syndrome in women.
Information from reference 27.
Figure 1. Treatment of Adult Patients with Functional, Normal Transit Constipation
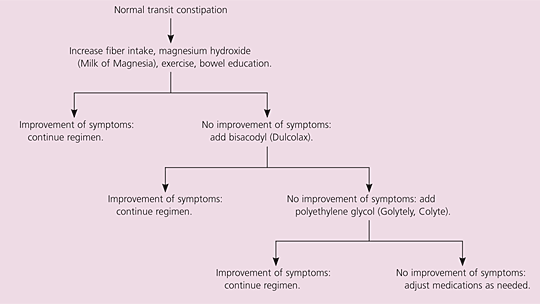
Algorithm for the treatment of adult patients with functional, normal transit constipation.
Adapted with permission from Locke GR III, Pemberton JH, Phillips SF. American Gastroenterological Association Medical Position Statement: guidelines on constipation. Gastroenterology 2000;119:1764.
BULK LAXATIVES
Bulk laxatives may contain soluble (psyllium, pectin, or guar) or insoluble (cellulose) products. They are hydrophilic, absorbing water from the intestinal lumen to increase stool mass and soften the stool consistency, and are generally well tolerated by most patients. Patients with functional normal transit constipation benefit the most from treatment with bulk laxatives. However, patients with slow transit constipation or anorectal dysfunction may not be helped by bulking agents.28 A systematic review26 found that bulk laxatives improve symptoms of constipation such as stool consistency and abdominal pain. As with increased dietary intake of foods rich in fiber, bloating and excessive gas production may be a complication of bulk laxatives.
EMOLLIENT LAXATIVES
Emollient laxatives or stool softeners, (e.g., docusates), act by lowering surface tension, allowing water to enter the bowel more readily. They are generally well tolerated but are not as effective as psyllium in the treatment of constipation. A study29 comparing a stool softener with psyllium found that psyllium was more effective in relieving constipation. Stool softeners are ineffective in chronically ill older adults.30 Stool softeners may be more useful for patients with anal fissures or hemorrhoids that cause painful defecation. Mineral oil is not recommended because of the potential to deplete fat-soluble vitamins and the risk of aspiration.13
OSMOTIC LAXATIVES
Saline or osmotic laxatives are hyperosmolar agents that cause secretion of water into the intestinal lumen by osmotic activity. The most commonly used osmotic laxatives are oral magnesium hydroxide (Milk of Magnesia), oral magnesium citrate, and sodium biphosphate (Phospho-Soda). In general, these agents are considered relatively safe because they work within the colonic lumen and do not have a systemic effect. However, they have been associated with electrolyte imbalance within the colonic lumen and may precipitate hypokalemia, fluid and salt overload, and diarrhea. Therefore, they should be used carefully in patients with congestive heart failure and chronic renal insufficiency. Chronic use of magnesium-containing laxatives may contribute to hypermagnesemia in patients with chronic renal insufficiency.
Alternative hyperosmotic laxatives are sorbitol, lactulose, and polyethylene glycol (PEG) 3350. Sorbitol and lactulose are undigestible agents that are metabolized by bacteria into hydrogen and organic acids. Poor absorption of these agents may lead to flatulence and abdominal distention. In a multicenter trial31 of 164 patients, lactulose was found to be more effective in producing a normal stool by day seven compared with laxatives containing senna, anthraquinone derivatives, or bisacodyl (Dulcolax). In a multicenter, placebo-controlled trial32 of 150 patients, PEG 3350 was found to be an effective agent for softening stools and increasing stool frequency. In a comparison study33 of 99 patients with chronic constipation, PEG 3350 was found to be more effective and caused less flatulence than lactulose.
STIMULANT LAXATIVES
Stimulant laxatives include products containing senna and bisacodyl. These laxatives increase intestinal motility and secretion of water into the bowel. They generally produce bowel movements within hours, but may cause abdominal cramping because of the increased peristalsis. Stimulant laxatives should not be used in patients with suspected intestinal obstruction. Chronic use of stimulant laxatives containing anthraquinone may cause a brown-black pigmentation of the colonic mucosa known as melanosis coli. This condition is benign and may resolve when the stimulant laxative is discontinued.34 Colonic inertia is seen in some chronic users of stimulant laxatives, but it is unclear if this is related to their prolonged use.13 In a trial35 of 77 nursing home residents, a combination of senna and bulk laxative was demonstrated to be more effective than lactulose in improving stool frequency and consistency and also was lower in cost.
PROKINETIC AGENTS
A number of prokinetic agents have been studied for the treatment of slow transit constipation. The most successful of these are colchicine36 and misoprostol (Cytotec).37 Both of these agents accelerate colonic transit time and increase stool frequency in patients with constipation, although neither has been approved by the U.S. Food and Drug Administration for this indication. A study38 of 12 patients with developmental challenges who required three or more laxatives to manage their chronic constipation found that colchicine increased the number of bowel movements and decreased the number of rectal laxatives used. In a more recent study39 of 16 women with chronic constipation who were receiving colchicine, the number of bowel movements improved significantly and the initial side effect of abdominal pain decreased with continued treatment. Larger trials are needed to confirm the efficacy and safety of the long-term use of colchicine for the treatment of chronic constipation.
In women with irritable bowel syndrome characterized by constipation, tegaserod (Zelnorm) is a colonic prokinetic agent that improves stool consistency and frequency.40 A recent systematic review41 evaluated eight short-term, placebo-controlled studies conducted mainly in women and found that although tegaserod increased the number of bowel movements, it did not significantly improve patients symptoms of abdominal pain and discomfort. Patients on higher doses of tegaserod (12 mg) experienced more diarrhea.41
Biofeedback
Biofeedback, or pelvic floor retraining, is the mainstay of treatment for patients with anorectal dysfunction. Biofeedback is used to emphasize normal coordination and function of the anal-sphincter and pelvic-floor muscles. Biofeedback can be performed with anorectal electromyography or a manometry catheter. Patients receive visual and auditory feedback by simulating an evacuation with a balloon or silicon-filled artificial stool.42 A systematic review43 of biofeedback studies revealed an overall success rate of 67 percent.
Surgery
Only patients who have been evaluated by physiologic testing and proven to have slow colonic transit constipation benefit from surgery. A subtotal colectomy with ileorectostomy is the procedure of choice for patients with slow transit constipation that is persistent and intractable.44 Complications after surgery may include small bowel obstruction, recurrent or persistent constipation, diarrhea, and incontinence.44 Surgery generally is not recommended for constipation caused by anorectal dysfunction.44 The relationship between rectocele and constipation is not entirely clear. Surgical correction is reserved for patients with large rectoceles that alter bowel function.44
Treating Constipation During Pregnancy
Constipation is a common problem in late pregnancy because of the rising level of circulating progesterone, which slows gastrointestinal motility. A Cochrane review45 found two randomized trials for treating constipation in pregnancy. The findings suggest that fiber supplements increase the number of bowel movements and lead to softer stools. Although stimulant laxatives are more effective than bulk-forming laxatives, they also are more likely to cause diarrhea and abdominal pain.45 Therefore, women who are pregnant should be encouraged to add more fiber to their diet; if constipation persists, a stimulant laxative may be recommended.

