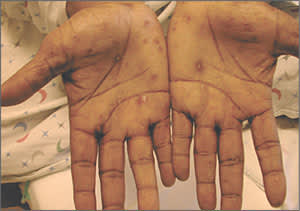
A 58-year-old woman presented with non-pruritic skin lesions on her hands (see accompanying figure) and back and sensorineural deafness in her left ear that had progressed over the previous four weeks. She did not have any known drug allergies. Her medical, personal, social, and family histories were noncontributory. The serum Venereal Disease Research Laboratory (VDRL) test was positive (1:128), and analysis of cerebrospinal fluid (CSF) showed that cell count and glucose and protein levels were within normal limits. The CSF VDRL test was nonreactive.
Question
Based on the patient’s history, physical examination, and laboratory investigations, which one of the following is the most likely diagnosis?
A. Primary syphilis.
B. Neurosyphilis.
C. Early latent syphilis.
D. Late latent syphilis.
E. Tertiary syphilis.
Discussion
The answer is B: neurosyphilis. A fluorescent treponemal antibody absorption test confirmed the serum VDRL test to be a true positive. Thus, the presence of skin lesions, laboratory evidence, and central nervous system (CNS) involvement (i.e., new onset sensorineural deafness) establish this as a case of secondary syphilis with neurosyphilis. Neurosyphilis can occur at any stage of the disease. However, current guidelines1 do not recommend CSF evaluation in patients with primary or secondary syphilis and no evidence of CNS or eye involvement.
The typical skin lesions of secondary syphilis are elevated papules (less than 1 cm in diameter) or plaques (greater than 1 cm in diameter) associated with scale. The appearance of papulosquamous syphilides can be described as “nickels and dimes.” Several diseases cause papulosquamous dermatosis (see accompanying table), which presents as pale red, discrete, round lesions that measure 5 to 10 mm in diameter, have a fine scale, and are distributed symmetrically on the trunk, as well as on the palms and soles.2,3
Secondary and tertiary syphilis may cause deafness.4,5 Eighth cranial nerve involvement can occur as an adverse reaction to syphilitic treatment.6 The classic findings in the CSF of pleocytosis, elevated protein level, and a positive CSF VDRL test may not be present in a significant proportion of patients with neurosyphilis who present with isolated eighth nerve palsy.7 Hearing loss associated with syphilis is one of the few treatable forms of progressive hearing loss, making correct diagnosis essential.7,8
Correct staging of syphilis is important because treatment recommendations vary by stage. The 2002 guidelines1 from the Centers for Disease Control and Prevention on treating sexually transmitted diseases outline appropriate evaluation and treatment for each stage of syphilis. Primary syphilis is characterized by a painless ulcer (chancre) at the site of primary infection. Secondary syphilis is characterized by cutaneous and mucosal lesions and systemic signs such as lymphadenopathy. Tertiary syphilis has cardiac manifestations or gumma formation. Latent syphilis describes seropositivity without disease manifestation. Early latent syphilis is latent syphilis acquired within the previous year, whereas late latent syphilis is acquired at a more remote or unknown time.1

