A 79-year-old man complained of a two-month history of a minimally pruritic rash on his abdomen, flanks, and buttocks. It had appeared initially over several days. He denied any recent travel or prolonged outdoor activities. His medical history included a smoking history of 30 pack-years, chronic obstructive pulmonary disease, and a non–small-cell carcinoma of the left upper lobe that was resected more than five years earlier. A presumptive diagnosis of tinea corporis was made and the patient was started on oral terbinafine (Lamisil).
After two months, he showed no signs of improvement. The review of systems revealed a 10-lb (4.5-kg) weight loss over three months. Physical examination of the trunk revealed large, erythematous annular and polycyclic patches with white scale at the leading edge (Figures 1 and 2) and an overall “wood-grain” appearance. Skin scrapings examined with potassium hydroxide failed to demonstrate fungal elements.
Figure 1.
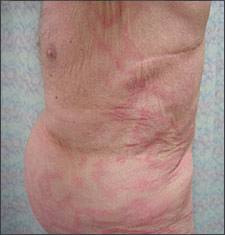
Figure 2.
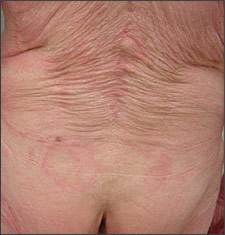
Question
Based on the patient’s history and physical examination, which one of the following is the correct diagnosis?
A. Erythema annulare centrifugum.
B. Mycosis fungoides (cutaneous T-cell lymphoma).
C. Erythema gyratum repens.
D. Erythema chronicum migrans.
E. Tinea corporis.
Discussion
The answer is C: erythema gyratum repens. A punch biopsy showed superficial perivascular lymphocytic inflammation consistent with a gyrate erythema. Chest radiography and computed tomography showed a right hilar nodule that was confirmed to be a new primary squamous cell carcinoma. The temporal relation of the rash, the new pulmonary malignancy, and a supportive biopsy led to the diagnosis of erythema gyratum repens.
Erythema gyratum repens is one of the four classic gyrate erythemas (the others are erythema marginatum, erythema chronicum migrans, and erythema annulare centrifugum). It represents a cutaneous manifestation of internal disease, and more than 80 percent of reported cases have occurred in association with an internal malignancy.1 The most commonly associated malignancy is a pulmonary carcinoma.1,2 If the underlying malignancy is treated, the rash and pruritus generally resolve within a few days to weeks.1–4 Other reported associations include pulmonary tuberculosis3 and autoimmune blistering diseases (e.g., bullous pemphigoid).5,6
The diagnosis of erythema gyratum repens usually precedes the diagnosis of cancer by an average of nine months, although it can range from one to 72 months.1 Three pathogenic immunologic theories have been proposed: (1) antibodies to tumor antigens may cross-react with the skin; (2) a tumor-produced peptide may render skin constituents antigenic; and (3) tumor antigen-antibody complexes may be deposited in the skin.4 To date, none of these theories has been able to consistently explain the pathogenesis.
Erythema gyratum repens is characterized by several concentric, erythematous, flat to slightly raised bands with fine white scale in waves at the leading edge of the erythema. The appearance may resemble a wood-grain pattern.7 Erythema gyratum repens typically affects the trunk and proximal extremities, generally sparing the hands, feet, and face. Bands can migrate up to 1 cm per day and often are pruritic.8
Erythema annulare centrifugum consists of few large, annular, thin, erythematous plaques that migrate centrifugally over weeks rather than days and leave central clearing. Erythema annulare centrifugum is a reactive process to infections or drugs, or is idiopathic. In differentiating erythema annulare centrifugum from erythema gyratum repens, the observer should look for a “trailing scale” at the inner margin of the expanding erythema in patients who have erythema annulare centrifugum, compared with a “leading scale” in patients who have erythema gyratum repens.
Mycosis fungoides, a type of cutaneous T-cell lymphoma, may present in a patch, plaque, or tumor stage. The patch stage consists of discrete, coin-shaped, macular erythema with fine white scale, most commonly located on the trunk and proximal extremities. Plaque and tumor stages have varying morphologies and are much thicker. The initial lesions of mycosis fungoides typically have a protracted clinical course over many years to decades. Most patients have nonspecific lesions and biopsy results suggesting a diagnosis of psoriasis or eczema long before the diagnosis is made.
Erythema chronicum migrans is an expanding erythematous thin plaque associated with an Ixodes tick bite and Borrelia infection. Although the “bull’s-eye” lesion of erythema chronicum migrans may have an appearance somewhat similar to that of erythema gyratum repens, it typically does not have scale. Furthermore, erythema chronicum migrans is often a solitary lesion at the site of the tick bite, although occasionally there may be smaller, separate lesions.
Tinea corporis was the patient’s initial diagnosis. It consists of annular erythematous patches or plaques with active inflammation and scale at the periphery of the lesions. This case highlights the importance of performing a skin scraping with potassium hydroxide when diagnosing fungal skin infections.
Selected Differential Diagnosis of Gyrate Erythema
| Condition | Characteristics |
|---|---|
| Erythema annulare centrifugum | Pink annular plaque; centrifugal spread; central clearing; trailing white scale |
| Erythema chronicum migrans | Pink annular plaque; centrifugal spread; central clearing; no scale; with or without crusted or vesicular advancing edge |
| Erythema gyratum repens | Concentric erythematous bands; scale at the leading edge; “wood-grain” appearance; rapid spread (up to 1 cm per day) |
| Mycosis fungoides | Slow progression from patch to plaque to tumor stage over many years; early lesions are pinkish nummular or annular patches with or without thin scale and epidermal atrophy |
| Tinea corporis | Pink annular patches or plaques; slow centrifugal spread; central clearing; peripheral scale; potassium hydroxide positive |

