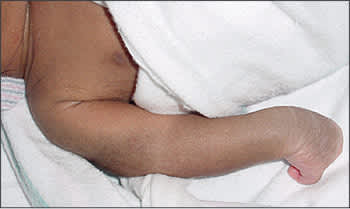
A mother expressed concern about her newborn's arm shortly after delivery. The infant was delivered at term by cesarean section because of a breech presentation. The mother's prenatal history was unremarkable and the infant's size was appropriate for gestational age. On delivery, the infant weighed approximately 2,900 g (6 lb, 6 oz) and had Apgar scores of 4 and 9 at one and five minutes, respectively. On examination, the affected upper extremity was adducted and internally rotated, with the elbow extended and the forearm pronated (see accompanying figure). Biceps and Moro reflexes were absent on the affected side. No sensory loss was noted. The other arm was normal and the rest of the physical examination was unremarkable. Spontaneous full recovery occurred at 48 hours.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Klumpke's paralysis.
B. Fractured clavicle.
C. Erb's palsy.
D. Cerebral palsy.
E. Fractured humerus.
Discussion
The answer is C: Erb's palsy. Erb's palsy, also called Erb-Duchenne paralysis, is a type of brachial plexus injury. The incidence of obstetric brachial plexus injuries ranges from 1.6 to 2.9 per 1,000 live births, with upper plexus palsies being most common.1 Different forces precipitate varying degrees of brachial plexus palsy, although widening of the head-shoulder angle because of lateral traction on the baby's head and neck during delivery generally is thought to cause Erb's palsy.1,2
Approximately 45 percent of brachial nerve injuries are associated with shoulder dystocia.3 However, shoulder dystocia is not present in all patients with Erb's palsy, and a number of cases of the disorder involve the posterior shoulder.4 Thus, forces other than physical traction during delivery, most likely maternal propulsive forces during fetal descent, may contribute.2,4
Erb's palsy results from an injury to the fifth and sixth cervical nerves. The arm is adducted with the forearm extended, internally rotated, and pronated, generating the classical “porter's tip” or “waiter's tip” appearance.5 The biceps and Moro reflexes are absent on the affected side. Sensory function usually is preserved. Loss of power in the forearm and loss of hand grasp indicate damage to the lower part of the brachial plexus.
Recovery of neurologic function is usually spontaneous and may occur within 48 hours; however, it can take up to six months. Nerve laceration may result in a permanent palsy. The presence of hand grasp and absence of forearm paralysis are favorable prognostic signs.3 Although the prognosis for an upper plexus palsy is generally good, the quality of the evidence supporting this conclusion is poor. Physicians should be cautious in predicting full recovery and closely follow affected infants.1
Treatment is indicated to prevent development of contractures and is achieved by partial immobilization and appropriate positioning of the upper extremity. The arm is abducted to 90 degrees with external rotation at the shoulder, the forearm is supinated, and the wrist is extended slightly with the palm turned toward the face. The extremity should be immobilized intermittently in a splint or brace. Active and passive range-of-motion exercises should be started by the end of the first week. Neurosurgical consultation should be obtained if the paralysis persists for more than three to six months.3 Furthermore, signs of nerve injury proximal to the brachial plexus may indicate more severe damage and warrant earlier consultation.6 Electromyography and nerve conduction velocities are not reliable indicators of injury severity.6
Klumpke's paralysis occurs when there is damage to the seventh and eighth cervical and the first thoracic nerve roots. This rare palsy presents as hand paralysis with or without Horner syndrome.6
Fractured clavicle should be considered in any newborn with a difficult shoulder delivery in vertex presentation or with extended arms in breech delivery. The infant may have restricted active movements on the affected side, with absent Moro reflex but normal biceps reflex. Although clavicular fracture initially may go unnoticed, crepitus with bony irregularity is felt at the fracture site. Occasionally, a bruise may appear. Diagnosis is confirmed by radiography.
Cerebral palsy may present with increased tone in the upper extremity, with increased biceps reflex and hyper-active grasp reflex.
The diagnosis of a fractured humerus is confirmed by radiographic findings in a newborn who has preserved biceps reflex but little or no active movement of the upper extremity. Both of the above fractures coexist with birth-related brachial plexus injury in approximately 10 percent of newborns.7
Selected Differential Diagnosis of Abnormal Arm Posture in a Newborn
| Condition | Characteristics |
|---|---|
| Klumpke's paralysis | Hand paralysis with possible ptosis, miosis, anhidrosis (Horner syndrome) |
| Fractured clavicle | Crepitus and bony irregularity felt; occasional bruising; possibly restricted active movements with absent Moro reflex on affected side; biceps reflex present |
| Erb's palsy | Restricted active movements and absent Moro and biceps reflexes on affected side; “porter's tip” or “waiter's tip” appearance of upper extremity |
| Cerebral palsy | Increased upper extremity tone; exaggerated biceps reflex; hyperactive grasp reflex |
| Fractured humerus | Restricted active movements and absent Moro reflex on affected side, biceps reflex present; crepitus may be felt |

