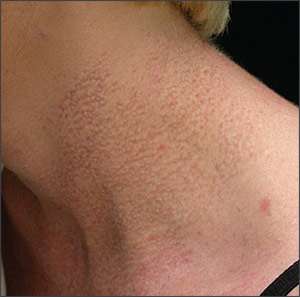
A 39-year-old woman presented with a rash on her neck and arms. The rash was not pruritic or painful. She was otherwise asymptomatic and had no significant medical or family history. On physical examination, confluent yellowish papules and plaques were noted in a cobblestone pattern on her lateral neck and bilateral antecubital fossae (see accompanying figure). The patient stated that the rash had been present as early as nine years of age.
Question
Based on the patient’s history and physical examination, which one of the following is the most likely diagnosis?
A. Eruptive xanthoma.
B. Toxicity from saltpeter (potassium nitrate) exposure.
C. Pseudoxanthoma elasticum.
D. Penicillamine (Cuprimine) therapy.
E. Cutis laxa.
Discussion
The answer is C: pseudoxanthoma elasticum. Pseudoxanthoma elasticum is a genetic defect of elastic tissue that manifests as dystrophic calcification of elastic fibers within the dermis, retina, and internal elastic lamina of medium-sized arteries. On the skin, pseudoxanthoma elasticum presents with multiple yellowish papules and plaques arranged in a cobblestone pattern resembling “plucked chicken skin.” The skin exhibits decreased elasticity and increased laxity. It typically involves the flexural surface of the neck and axillae, as well as antecubital and popliteal fossae. Inguinal, periumbilical, oral, rectal, and vaginal areas are involved less commonly. Occasionally, patients will not have any skin lesions.
Pseudoxanthoma elasticum produces ocular changes consisting of angioid streaks. These represent tears in Bruch’s membrane from weakening of calcified elastic fibers. The funduscopic examination reveals broad, irregular lines on the retina that are red-brown to gray. Angioid streaks also may occur with various clinical conditions including Ehlers-Danlos syndrome, sickle cell disease, and Paget’s disease.1
Pseudoxanthoma elasticum is inherited primarily in an autosomal recessive fashion.2 The estimated prevalence ranges from one in 70,000 to one in 100,000 persons, with a female-to-male ratio of 2:1.3,4 There is an average delay of nine years from initial presentation of skin lesions to diagnosis.1 Definitive diagnosis is established by performing a skin biopsy. Histopathologic changes reveal a fragmented appearance of curled and split, calcified elastic fibers.
The complications of pseudoxanthoma elasticum predominantly affect the ocular, cardiovascular, and gastrointestinal systems. Repeated tears in Bruch’s membrane lead to subretinal neovascularization with loss in central vision. Ophthalmology referral and regular follow-up are indicated.2 Furthermore, patients should avoid heavy straining or potentially traumatic activities (e.g., football, wrestling, weight lifting) that may induce retinal hemorrhage.1
Pseudoxanthoma elasticum accelerates the atherosclerotic process, leading to intermittent claudication, coronary artery disease, angina pectoris, myocardial infarction, and stroke. Physical examination may reveal diminished peripheral pulses and hypertension. Patients with pseudoxanthoma elasticum require aggressive modification of cardiovascular risk factors. Rupture of calcified gastric and duodenal vessels may lead to gastrointestinal bleeding. Thus, avoidance of platelet inhibitors, such as aspirin, should be recommended.5
Genetic counseling for patients with pseudoxanthoma elasticum and their families should be offered. First-degree relatives of patients with pseudoxanthoma elasticum should be screened with a thorough skin examination and dilated funduscopic examination. Dermatology consultation may be helpful. Effects of pseudoxanthoma elasticum on pregnancy are variable. Many women with pseudoxanthoma elasticum have uncomplicated pregnancies with the delivery of a healthy infant.6
Most forms of xanthoma present as a group of discrete, yellowish papules that are firm to palpation. Examples include xanthelasma and eruptive xanthomas. Eruptive xanthomas tend to occur on the buttocks and extensor aspects of the elbows and knees. They almost always are associated with an underlying familial cholesterol disorder and resolve with treatment of the dyslipoproteinemia.
Saltpeter is a form of potassium nitrate most commonly used as a fertilizer. Exposure can produce skin lesions identical to those of pseudoxanthoma elasticum; typically, the lesions are considered to be an exogenous, acquired form of the disease.7 Reported cases generally occur in adult men working in agriculture.
Long-term therapy with penicillamine has been found to produce elastolytic changes similar to those of pseudoxanthoma elasticum.8 Most reported cases have occurred in patients treated for Wilson’s disease.
Cutis laxa is a congenital disorder of elastic tissue resulting in loose, redundant folds of skin. It is most common in infants, but an acquired form can affect children and adults. Although skin laxity is present in cutis laxa and pseudoxanthoma elasticum, yellowish papules in a cobblestone pattern are not characteristic of cutis laxa.
Summary Table
| Condition | Characteristics |
|---|---|
| Cutis laxa | Skin laxity; congenital disorder of elastic tissue; most common in infants |
| Eruptive xanthoma | Firm yellow papules grouped most often on the buttocks and extensor surface of the elbows and knees; dyslipidemia |
| Penicillamine (Cuprimine) therapy | Changes in elastic tissue similar to pseudoxanthoma elasticum; potential complication of long-term treatment |
| Pseudoxanthoma elasticum | Multiple yellowish papules and plaques in a cobblestone pattern; ocular, dermatologic, and cardiovascular sequelae |
| Toxicity from saltpeter (potassium nitrate) exposure | Similar appearance to pseudoxanthoma elasticum; most often from agricultural exposure |

