A 46-year-old man with a history of alcohol abuse and hemorrhoids presented with a perianal and perineal rash of three to four weeks’ duration. It was associated with severe tenderness and a small amount of discharge. On examination, a violaceous erythema with a rim scale on the gluteal crease and perineum (Figure 1) was noted. He had severe inflammation with multiple crypts and abscesses around the anus. There was a short period of improvement after he was treated with 14 days of cefazolin (Ancef). After several weeks, the lesion recurred with extension to the perineal area and was associated with draining sinuses (Figure 2). Colonoscopy results were negative for changes consistent with Crohn’s disease. Herpes culture and syphilis serology were negative.
Figure 1.
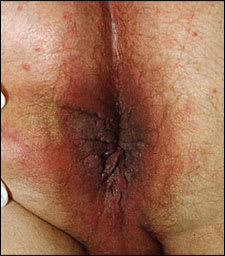
Figure 2.
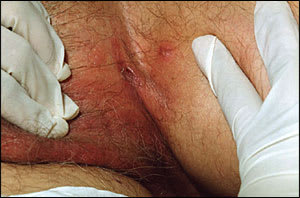
Question
Based on the patient’s history and physical examination, which one of the following is the most likely diagnosis?
A. Carbuncle.
B. Hidradenitis suppurativa.
C. Infected epidermoid cyst.
D. Lymphogranuloma venereum.
E. Lymphadenitis.
Discussion
The answer is B: hidradenitis suppurativa. This chronic, inflammatory, scarring disease can occur in both sexes after puberty, most often in the second or third decade of life.1 Lesions usually affect the apocrine sweat gland–bearing skin, most commonly the axilla, groin, and perianal and inframammary areas.1 Early lesions are tender, red, dermal abscesses that increase in size and may open to the surface, discharging purulent material if untreated. The inflammation gradually subsides, but recurrence or formation of a new abscess is the rule. Sinus tracts often occur, sometimes with foul-smelling, purulent discharge secondary to bacterial infection. If perianal hidradenitis involves the anus and rectum, it should prompt investigation to rule out Crohn’s disease, especially before surgical excision.1 Physicians also should consider other diagnoses such as tuberculosis, actinomycosis, tularemia, and ulcerative colitis.
Treatment is difficult, and medical management is recommended in the early stages. Local care includes gentle cleansing with antiseptic soaps or cleansers or warm compresses with saline or Burow’s solution (5% aluminum subacetate). Tight-fitting clothing and roll-on antiperspirant should be avoided, and weight loss should be encouraged if appropriate. Use of antibiotics such as minocycline (Minocin), cephalosporins, and clindamycin (Cleocin) after culture of the discharge is recommended. However, a surgical approach is preferred if scarring and sinus tract formation have occurred.1,2
Topical clindamycin often is used between flare-ups.1,2 Chronic oral antibiotics such as tetracyclines also are used, although evidence from controlled trials is lacking. Other treatment modalities include antitumor necrosis factor therapy; intralesional corticosteroids for isolated lesions; isotretinoin (Accutane); and the antiandrogen, cyproterone acetate (not available in the United States), in conjunction with ethinyl estradiol (Estinyl).3,4 Squamous cell carcinoma is a rarely reported complication.1,4 Patients may require counseling because of the recurrent and debilitating nature of the disease.
A carbuncle is a larger, more acute inflammatory lesion with a deeper base, typically occurring as a painful lesion at the nape of the neck. Fever and malaise often are present. The involved area is red and indurated and multiple pustules appear, often draining externally around hair follicles. The lesion develops a yellow-gray, irregular crater at the center, which then may heal by slow granulation.5
Epidermoid cysts are intradermal or subcutaneous, dome-shaped protuberances, 1 to 5 cm in diameter, that are freely mobile. They are most common on the face, neck, chest, and upper back. They grow slowly and are asymptomatic, but some may become inflamed or secondarily infected.6
Lymphogranuloma venereum is a sexually transmitted disease caused by a subtype of Chlamydia trachomatis. The primary lesion is a soft, erythematous, painless erosion, 5 to 8 mm in diameter, that heals spontaneously in a few days. Secondary inguinal adenopathy begins one to two weeks after the primary lesion; these discrete, movable, tender nodes later coalesce to form a firm, elongated, immovable mass. Nodal rupture may lead to chronic sinus formation.7
Lymphadenitis is an acute or chronic inflammation of a single or multiple lymph nodes. Staphylococcus aureus and group A streptococci are the most common etiologic agents. On examination, the involved area is swollen, and the node is usually 3 cm in diameter and tender. Fever is often present. The involved nodes may be firm or fluctuant. The overlying skin is warm and often erythematous and edematous.8
Selected Differential Diagnosis of Chronic, Draining Perianal Sinuses
| Condition | Characteristics |
|---|---|
| Carbuncle | Large, acute, inflammatory lesions on a deep base; red and indurated with multiple pustules |
| Hidradenitis suppurativa | Tender, red, dermal abscesses that gradually increase in size and open to the surface with purulent discharge |
| Infected epidermoid cyst | Intradermal or subcutaneous dome-shaped protuberances, freely mobile, red and indurated when infected |
| Lymphogranuloma venereum | Soft, erythematous, painless erosions; enlarged lymph nodes form after the primary lesion heals |
| Lymphadenitis | Tender, red, fluctuant lymph nodes associated with systemic symptoms |

