Guideline source: American Heart Association
Literature search described? N/A
Evidence rating system used? Yes
Published source: Circulation, 2007 (in press)
Available at:http://circ.ahajournals.org
Cardiovascular disease (CVD) is the most common cause of mortality among women, and it accounts for one third of all deaths. More women than men die each year from CVD in the United States. The public health impact of CVD on women is not solely related to mortality because advances in medicine have helped many women survive the disease. However, with the continued increase in the average life expectancy, the burden of CVD on women will also continue to rise.
CVD is often preventable in women, and even modest control could have a large impact. By reducing the rate of death from chronic diseases by 2 percent over one decade, it is estimated that 36 million lives could be saved.
Although some exceptions do exist, the guidelines presented by the American Heart Association (AHA) to prevent CVD in women do not differ for men. However, health care professionals should be aware that some of these recommendations are contraindicated in women who are pregnant or who want to become pregnant. This update represents the most current clinical recommendations for the prevention of CVD in women 20 years and older.
Risk Factors
Women who have one or more risk factors for heart disease, evidence of subclinical disease with or without risk factors, poor exercise capacity, or unhealthy lifestyles may be at risk of CVD (Figure 1). Factors such as medical and lifestyle history, Framingham risk score, and family history of CVD and other genetic conditions (e.g., familial hypercholesterolemia) should be considered when determining a patient's risk of CVD (Table 1).
Figure 1. CVD Preventive Care in Women
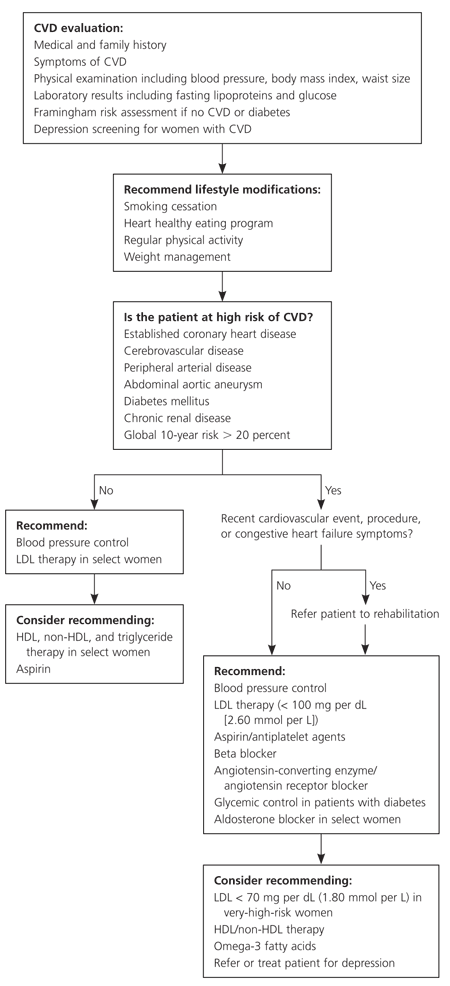
Preventing cardiovascular disease in women. (CVD = cardiovascular disease; LDL = low-density lipoprotein; HDL = high-density lipoprotein.)
Adapted from American Heart Association. Evidence-based guidelines for cardiovascular disease prevention in women: 2007 update. Circulation 2007 [In press].
Clinical Recommendations
Recommendations for the prevention of CVD in women are based on the level of evidence to support a clinical recommendation as well as other factors, such as their practical application in randomized controlled trials with women. They are divided into the following categories: lifestyle interventions, major risk-factor interventions, and preventive drug interventions.
LIFESTYLE INTERVENTIONS
Cigarette Smoking
Counseling women against smoking is recommended, as is nicotine replacement or another indicated pharmacotherapy combined with participation in a behavioral or formal smoking cessation program. Women should also try to avoid secondhand smoke.
Physical Activity
Women at risk of CVD should aim for a minimum of 30 minutes of moderate exercise (e.g., brisk walking) on most, and preferably all, days of the week and 60 to 90 minutes of daily moderate exercise for those who need to lose weight or sustain weight loss.
Weight Maintenance
To maintain or lose weight, it is recommended that women find an appropriate balance of physical activity and caloric intake. Body mass index should be between 18.5 and 24.9 kg per m2, and waist circumference should not exceed 35 inches.
Dietary Intake
A high intake of fruits and vegetables is recommended for women at risk. Selecting whole-grain, high-fiber foods and consuming oily fish at least twice a week is recommended. Dietary cholesterol should be less than 300 mg per day, and saturated fat should make up no more than 7 to 10 percent of the diet; women at risk of hypercholesterolemia should have diets with less than 7 percent saturated fat and less than 200 mg of cholesterol each day.
In conjunction with diet, omega-3 fatty acids in capsule form may be considered for women with coronary heart disease (CHD).
Rehabilitation
Women who have had a recent cerebrovascular event; acute coronary syndrome or coronary intervention; peripheral arterial disease; new-onset or chronic angina; or symptoms of heart failure should be offered a comprehensive risk-reduction regimen (e.g., physician-guided community- or home-based exercise training program, cardiovascular or stroke rehabilitation).
Depression
Screening for depression in women with CHD should be considered.
MAJOR RISK-FACTOR INTERVENTIONS
Blood Pressure
Optimal blood pressure is less than 120/80 mm Hg. Physicians should encourage patients to achieve optimal blood pressure through weight control; sodium restriction; increased physical activity; and consumption of low-fat dairy products, fruits, and vegetables.
If blood pressure is 140/90 mm Hg or more, or if the patient has chronic kidney disease or diabetes with blood pressure of 130/80 mm Hg or more, pharmacotherapy is recommended. Unless contraindicated or other agents are indicated for specific vascular diseases, thiazide diuretics should be considered as part of the drug regimen. Beta blockers used alone or in conjunction with angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs), with the addition of thiazides as needed to control blood pressure, are recommended for the initial treatment of women at high risk of CVD.
Lipids
Lifestyle changes are recommended to achieve an optimal low-density lipoprotein (LDL) cholesterol level of less than 100 mg per dL (2.60 mmol per L), high-density lipoprotein (HDL) cholesterol level greater than 50 mg per dL (1.30 mmol per L), triglycerides less than 150 mg per dL (3.90 mmol per L), and non-HDL levels less than 130 mg per dL (3.35 mmol per L).
For women with CHD or another atherosclerotic CVD, with diabetes, or with a 10-year absolute risk of more than 20 percent, LDL-cholesterol–lowering drug therapy in conjunction with lifestyle therapy is recommended to achieve an LDL cholesterol level of less than 100 mg per dL. A reduction to less than 70 mg per dL (1.80 mmol per L) is considered reasonable for women with CHD who are already at very high risk (e.g., women with diabetes mellitus and coronary heart disease).
LDL-cholesterol–lowering therapy is recommended for moderate-risk women (multiple risk factors, and who had a 10-year absolute risk of 10 to 20 percent) if the LDL cholesterol level is 130 mg per dL or more despite lifestyle therapy. For low-risk women whose 10-year absolute risk is less than 10 percent, LDL-cholesterol–lowering therapy is recommended if the patient's LDL cholesterol level is 160 mg per dL (4.15 mmol per L) or more despite lifestyle therapy. Regardless of the absence or presence of other risk factors or CVD, LDL-cholesterol–lowering therapy is recommended if the patient's LDL is 190 mg per dL (4.90 mmol per L) or more despite lifestyle therapy.
For women at high risk and women with multiple risk factors and a 10-year absolute risk of 10 to 20 percent, consider the use of fibrate therapy or niacin (Niacor) when HDL cholesterol is low or when non-HDL cholesterol is elevated after an appropriate LDL cholesterol level is reached.
Diabetes
If an A1C level of less than 7 percent can be accomplished without significant hypoglycemia, lifestyle therapy and pharmacotherapy should be used as indicated in women with diabetes.
PREVENTIVE DRUG INTERVENTIONS
Aspirin
Unless contraindicated, 75 to 325 mg per day of aspirin is recommended for women with CHD or another atherosclerotic CVD, diabetes, or with a 10-year absolute risk of more than 20 percent. For patients at high risk who are intolerant of aspirin, clopidogrel (Plavix) may be substituted.
For women 65 years and older, aspirin in a dosage of 81 mg daily or 100 mg every other day is recommended if blood pressure is controlled and the benefit for the prevention of myocardial infarction and ischemic stroke is likely to outweigh the risk of hemorrhagic stroke and gastrointestinal bleeding. The same recommendations apply for women younger than 65 years when the benefit for prevention of ischemic stroke will likely outweigh the adverse effects of aspirin therapy.
Beta Blockers
Unless contraindicated, beta blockers should be used indefinitely in all women with acute coronary syndrome; left ventricular dysfunction, with or without heart failure symptoms; and after myocardial infarction.
ACE Inhibitors/ARBs
For women with diabetes or who have had a myocardial infarction, or if clinical evidence suggests heart failure or a left ventricular ejection fraction of 40 percent or less, ACE inhibitors should be considered. ARBs should be used instead if the patient is intolerant to ACE inhibitors.
Aldosterone Blockade
Aldosterone blockade is recommended after a myocardial infarction in women who also have diabetes or heart failure or are already receiving therapeutic doses of an ACE inhibitor and beta blocker, but who do not have significant renal dysfunction or hyperkalemia.
Clinical Limitations
Variations in therapy adherence and patient characteristics exist, so the effectiveness of therapies prescribed in an office or hospital setting may vary widely from the efficacy and safety profiles shown in clinical trials. Therefore, the development of guideline recommendations has limitations that vary from one population to another. Many of the studies used to formulate the AHA guidelines did not include older women, especially those older than 80 years in whom CVD and other comorbidities are common. Health care professionals should use clinical judgment about the aggressiveness of preventive therapy provided to all women, especially those who are older.

