A young woman came to the office with large plaques on her lower extremities. The plaques had been present for many years. Pruritus was mild to minimal, and she had no personal or family history of atopic disease. On examination, large erythematous plaques with silvery scales were noted; they covered her lower extremities and mid- to lower back (see accompanying figures). The lesions were not distributed along skinfolds, and there was no facial or oral mucosal involvement. A potassium hydroxide preparation was negative.
Figure 1.
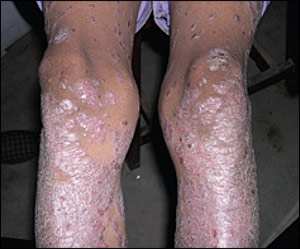
Figure 2.
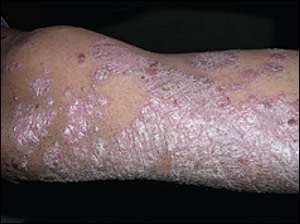
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Hypertrophic lichen planus.
B. Nummular eczema.
C. Psoriasis.
D. Seborrheic dermatitis.
E. Tinea corporis.
Discussion
The answer is C: psoriasis. Psoriasis is a chronic inflammatory dermatosis that affects 0.6 to 4.8 percent of the population and occurs in persons of all ages.1 Although no predilection by sex has been noted, psoriasis appears to be less prevalent in blacks than in the rest of the U.S. population.2
The disease is characterized by a well-demarcated, salmon-colored plaque covered by silver-white scales. Lesions are only mildly pruritic, and involved areas exhibit scaling that bleeds when peeled from the plaque (Auspitz sign). Acute lesions may be marked by inflammation and erythema, whereas more chronic lesions appear as the characteristic plaques. Microscopically, there are epidermal hyperplasia (acanthosis), parakeratosis, Munro's microabscesses, and an abnormal proximity between the highly vascularized dermal papillae and overlying scales.3
The strongest genetic association appears to be with the major histocompatibility complex class I region on chromosome 6, termed PSORS1 (psoriasis susceptibility 1).4 In persons who are genetically predisposed, environmental factors that appear to trigger initial presentations or exacerbations include streptococcal infections; human immunodeficiency virus infection; medications; and chemical, physical, or infectious skin trauma.4 Smoking and alcohol consumption also are triggers.
Treatment goals are to induce and maintain remission with minimal side effects. Most agents can be used alone or in combination with other treatment modalities. Mild disease is effectively managed with topical therapy; first-line treatment is class I and II corticosteroids. Vitamin D3 analogues (e.g., calcipotriene [Dovonex]) interrupt keratinocyte cellular proliferation and also are first-line therapy. Tazarotene (Tazorac), which binds to the retinoic acid receptor ligand, is a second-line agent that has minimal side effects.5 Tar preparations have unknown mechanisms and are useful for psoriasis affecting the scalp and body.
When psoriasis does not respond to topical therapy or when skin involvement is extensive, phototherapy or systemic drugs are often indicated.5 Systemic treatments approved by the U.S. Food and Drug Administration (FDA) include methotrexate and cyclosporine (Sandimmune). Both agents are effective but require close patient monitoring. Acitretin (Soriatane) is an oral retinoid for the systemic treatment of psoriasis. It is indicated for generalized pustular and erythrodermic disease forms, although its use is limited because of teratogenic and hepatotoxic effects.
Newer FDA-approved treatments focus on the migration and activation of T-cells, as well as the propagation of the immunologic cascade. These include efalizumab (Raptiva) and alefacept (Amevive).4 Cytokine tumor necrosis factor B is a key inflammatory mediator of psoriasis; thus, other newer treatments (e.g., etanercept [Enbrel]) focus on this mechanism. Current investigations on the treatment of psoriasis include infliximab (Remicade), adalimumab (Humira), photodynamic therapy, excimer lasers, anti-IL 12 antibodies, T-cell receptor vaccines, pimecrolimus (Elidel), and gene therapy.
A number of diseases are included in the differential diagnosis of psoriasis. Lichen planus can be distinguished by its pruritic, violaceous, shiny papules with a white lace-pattern (Wickham's striae) and involving the mucous membranes and flexor surfaces. Hypertrophic lichen planus, often involving the anterior leg, features thick plaques on an erythematous base. Nummular (discoid) eczema, usually seen in patients with a history of atopic disease, can be ruled out based on clinical background and histologic examination in which the hallmark finding is epidermal spongiosis and lymphocytic infiltrate. Seborrheic dermatitis lesions have a predilection for sebaceous glands and hair follicles on the scalp and face. Tinea corporis is characterized by a pruritic, scaling, annular lesion with erythematous borders and central clearing that shows branching hyphae on potassium hydroxide preparation. The accompanying table lists additional differential diagnoses that may appear similar to psoriasis.
Additional Differential Diagnosis of Large, Silvery Plaques
| Condition | Characteristics |
|---|---|
| Cutaneous T-cell lymphoma | Scaly, erythematous patches, plaques, or tumors affecting numerous body surface areas |
| Pityriasis rosea | Mildly pruritic, salmon-colored plaques arranged along skin cleavage lines, typically on the trunk, neck, and proximal extremities; preceded by herald patch |
| Secondary syphilis | Diffuse maculopapular lesions, mainly involving palms and soles, with systemic symptoms of fever, malaise, anorexia, and generalized lymphadenopathy |
| Squamous cell carcinoma in situ | Red-brown, scaling, poorly defined plaques, usually involving sun-exposed areas |

