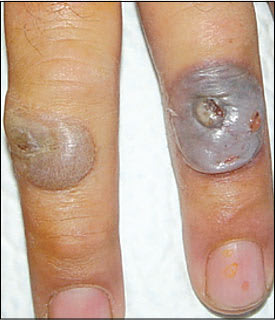
A 52-year-old man presented with a 10-day history of enlarging, painful lesions on his right hand. He was experiencing some fever and malaise. The man was a farmer who butchered his own meat. He gave no history of recent medication use. Examination of his hand revealed three tender, red nodules with a weeping, dark blue, umbilicated center; a white middle ring; and an erythematous periphery (Figures 1 and 2). There was mild axillary lymphadenopathy. His white blood cell count and blood chemistries were within normal limits, and a Gram stain of the lesion was negative for bacterial organisms.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Cutaneous anthrax.
B. Contagious ecthyma.
C. Ecthyma gangrenosum.
D. Fixed drug eruption.
E. Necrotic spider bite (necrotic arachnidism).
Discussion
The answer is B: contagious ecthyma. Contagious ecthyma (also known as orf) is a zoonotic, mucocutaneous infection caused by a parapoxvirus (i.e., orf virus). It is an occupational disease typically found in farmers, butchers, veterinarians, and shepherds who come in contact with infected sheep or goats or their products (e.g., wool, meat).1
After a three- to seven-day incubation period, a small, firm, red-blue papule develops, most often on the dorsa of the hands and the fingers.2 The papule develops into a hemorrhagic pustule or bulla that may contain a central crust and bleed easily. In the later stages, the lesion develops into a nodule that may weep fluid and occasionally is covered by a thin crust. Finally, a thick crust develops.3 The lesion may be accompanied by a mild fever or lymphadenopathy, and it usually resolves spontaneously in two to six weeks without scarring unless secondary infection occurs.4 Barrier protection and hand washing are recommended for persons working with susceptible animals, particularly if the person has broken skin or a skin disease such as eczema. Although the diagnosis is often clinical, because this infection is similar in appearance to cutaneous anthrax, definitive diagnosis may be needed. This can be obtained by polymerase chain reaction testing in cooperation with local public health services and the Centers for Disease Control and Prevention.5
Skin lesions of orf and anthrax exhibit a similar appearance and course. However, the initial anthrax lesion is a painless, pruritic macule or papule.6 After a few days, a clear, fluid-filled bulla, usually 1 to 2 cm in diameter, develops. The bulla soon ruptures and is followed by the formation of a necrotic ulcer with a black central eschar. A major diagnostic characteristic is the development of edema around the lesion. The eschar separates from the skin in one to two weeks, and healing usually results in scar formation.7
Ecthyma gangrenosum usually occurs in immuno-compromised patients, burn victims, and in patients receiving long courses of antibiotic therapy. The skin lesions are a localized septic vasculitis with subsequent skin infarction that is highly associated with systemic Pseudomonas aeruginosa infection. The lesions begin as a painless, erythematous macule that enlarges to a tender papule or nodule with a gray center and surrounding induration. The papule may develop into a hemorrhagic bullous lesion, possibly extending several centimeters in diameter. It undergoes central necrosis to become a deep, gangrenous ulcer with a gray-black eschar and an erythematous, sometimes violaceous, halo.8
Fixed drug eruption is a pruritic or burning, sharply circumscribed, round-to-oval patch with violaceous or dusky erythema. Rarely, bullous, ulcerative, or hemorrhagic components may develop. The patch appears within days to weeks of initiating the culprit drug and resolves after stopping the medication.9
Most spider bites are painless and cause little or no injury. Bites from a few spiders, such as the brown recluse, can cause skin necrosis. After two to three hours, intense pain develops at the bite site, as does erythema, cyanosis, and edema. A central dark vesicle or bulla soon appears, and 12 to 24 hours later, the vesicle may become hemorrhagic.8 An area of central necrosis may evolve, but presentation varies from no necrosis to severe necrosis requiring skin grafting. Unless witnessed, a spider bite is a speculative diagnosis and other causes should be considered, particularly when more than one necrotic lesion appears.10
Summary Table
| Condition | Characteristics |
|---|---|
| Cutaneous anthrax | Painless, necrotic ulcer with a black central eschar; surrounded by characteristic, nonpitting edema |
| Contagious ecthyma | Weeping nodule; scab formation but no distinctive, large eschar; occurs mostly on hands |
| Ecthyma gangrenosum | Lesions usually larger than 3 cm in diameter; highly associated with Pseudomonas aeruginosa infection |
| Fixed drug eruption | Violaceous or dark erythema; recurrence at same location with drug rechallenge; rarely bullous |
| Necrotic arachnidism | Quick necrosis development in 12 to 24 hours; painful |

