Fibromyalgia is an idiopathic, chronic, nonarticular pain syndrome with generalized tender points. It is a multisystem disease characterized by sleep disturbance, fatigue, headache, morning stiffness, paresthesias, and anxiety. Nearly 2 percent of the general population in the United States suffers from fibromyalgia, with females of middle age being at increased risk. The diagnosis is primarily based on the presence of widespread pain for a period of at least three months and the presence of 11 tender points among 18 specific anatomic sites. There are certain comorbid conditions that overlap with, and also may be confused with, fibromyalgia. Recently there has been improved recognition and understanding of fibromyalgia. Although there are no guidelines for treatment, there is evidence that a multidimensional approach with patient education, cognitive behavior therapy, exercise, physical therapy, and pharmacologic therapy can be effective.
Fibromyalgia is an idiopathic, chronic, nonarticular pain syndrome defined by widespread musculoskeletal pain and generalized tender points (Table 1). Other common symptoms include sleep disturbances, fatigue, headache, morning stiffness, paresthesias, and anxiety.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Treat fibromyalgia with a multidimensional clinical approach comprising patient education, cognitive behavior therapy, pharmacotherapy, and exercise. | A | 22 | Based on five RCTs |
| Use antidepressant medications to improve pain, sleep quality, and global well-being in patients with fibromyalgia. | B | 23 | Based on few RCTs |
| Prescribe cyclobenzaprine (Flexeril) 10 to 30 mg at bedtime to improve sleep and decrease pain in patients with fibromyalgia. | A | 31 | Systematic review of RCTs |
| Advise patients that aerobic exercise training has beneficial effects on fibromyalgia symptoms. | A | 35, 36 | Systematic review of RCT |
RCT = randomized controlled trial.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 176 or https://www.aafp.org/afpsort.xml.
Table 1. Characteristics and Associated Features of Fibromyalgia
| Characteristic features |
| Chronic widespread pain for at least three months |
| Tender points in 11 of 18 specific anatomic locations |
| Associated features |
| Anxiety |
| Cognitive difficulties |
| Fatigue |
| Headache |
| Paresthesias |
| Sleep disturbance |
Initially called fibrositis, the name was changed to fibromyalgia when it became evident that inflammation was not a part of this condition.1 The American College of Rheumatology (ACR) 1990 criteria for the classification of fibromyalgia was the product of the first well-designed, multicenter study on fibromyalgia and remains a cornerstone for the diagnosis.2
Epidemiology
Fibromyalgia is a common rheumatologic disorder that is underdiagnosed. Using the 1990 ACR classification criteria, the prevalence of fibromyalgia in the general population of the United States is reported to be 3.4 percent in women and 0.5 percent in men.3 Prevalence increases steadily through 80 years of age, and then declines. This condition affects women 10 times more often than men.3 Fibromyalgia is usually considered a disorder of women 20 to 50 years of age; however, it also has been observed in males, children, adolescents, and older persons. Fibromyalgia is more common in relatives of patients with fibromyalgia, suggesting the contribution of both genetic and environmental factors.4
Demographic and social characteristics associated with the presence of fibromyalgia are female sex, being divorced, failing to complete high school, and low income. Psychological factors associated with this syndrome include somatization disorder, anxiety, and personal or family history of depression.5
Pathophysiology
The pathophysiology of fibromyalgia is unclear. Fibromyalgia clusters in families, suggesting a genetic predisposition. Environmental and psychological factors, which could impact various members of the same family, may contribute to the symptomatology of the disease.6 Current theories of pathogenesis include central sensitization and hypothalamic-pituitary-adrenal axis dysregulation; however, more research is needed to determine a definite pathophysiology.
Clinical Features
Presenting complaints include pain at multiple sites, fatigue, and poor sleep. Patients often complain of low back pain, which may radiate into the buttocks and legs. Others complain of pain and tightness in the neck and across the upper posterior shoulders. The pain may be described as a burning or gnawing soreness, stiffness, or aching. Stiffness is typically present on arising in the morning; for most patients, stiffness improves as the day progresses. Patients complain of feeling exhausted, even upon waking. Many patients awaken frequently at night and have difficulty falling back to sleep. A subjective swollen joint feeling without objective swelling, and paresthesias without objective neurologic findings, are two important features of fibromyalgia.7
Many patients with fibromyalgia complain of cognitive difficulties such as mem ory problems, groping for words, and poor vocabulary. Headaches, including migraine type, also are common. Other manifestations include episodes of light-headedness, dizziness, anxiety, or depression. Symptoms are aggravated by cold and humid weather, poor sleep, and physical or mental stress. They are improved by warm and dry weather, moderate physical activity, adequate sleep, and relaxation.2
Assessment of physical activity is important because functional impairment is common in patients with fibromyalgia. The Fibromyalgia Impact Questionnaire (http://www.myalgia.com/FIQ/fiq.pdf) is a useful tool in assessing functional abilities in daily life and measures patient status, progress, and outcomes.8 It is a self-administered instrument that is composed of 10 items and can be completed in about 10 minutes. This questionnaire has been translated into numerous languages and has been shown to retain its validity.8
Relevant social, personal, and family history is helpful in establishing the diagnosis of fibromyalgia. A history of trauma, childhood abuse, anxiety, depression, or sleep disorder is useful for a comprehensive evaluation because there is evidence that fibromyalgia may be triggered by emotional stress, medical illness, surgery, or trauma. Patients with high tender point counts are more likely to report adverse childhood experiences like loss of a parent or abuse.9 Although physical trauma, especially cervical spinal injury, is associated with onset of fibromyalgia symptoms, further studies are needed to determine whether it has a causal role in the development of fibromyalgia.10,11 A family history of fibromyalgia or presence of any of the comorbid conditions increases the likelihood of a diagnosis of fibromyalgia.
Diagnosis
Fibromyalgia is not a diagnosis of exclusion and should be identified by its own characteristics. The ACR criteria have two components: (1) widespread pain involving both sides of the body, above and below the waist as well as the axial skeletal system, for at least three months; and (2) presence of 11 tender points among the nine pairs of specified sites (18 points) as shown in Figure 1.2
Figure 1.
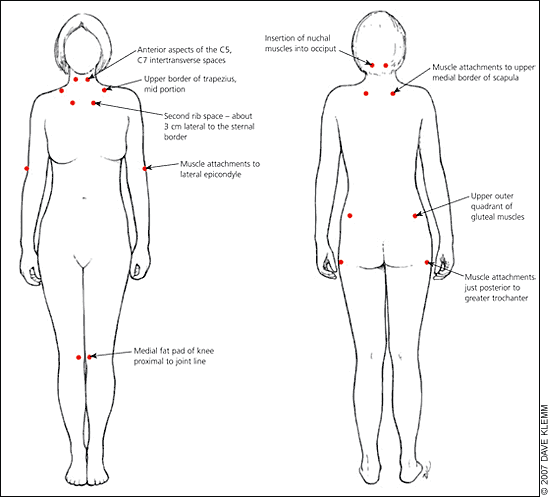
The American College of Rheumatology 1990 Criteria recommended anatomic tender point locations for diagnosis of fibromyalgia.
Information from reference 2.
An important portion of the physical examination for a diagnosis of fibromyalgia is to systematically palpate the 18 sites.2 A moderate and consistent degree of pressure should be used in digital palpation (using the thumb of the dominant hand) of these tender points. The amount of force applied should be 8.8 lb (4.0 kg), which should just blanch the examiner's thumbnail. This amount of pressure does not produce significant tenderness or pain in patients without fibromyalgia. The Manual Tender Point Survey describes the pressure application technique and the precise identification of survey sites.12
Diagnosis is primarily based on clinical findings from the history and physical examination, with diagnostic testing having a limited role. Although routine tests of complete blood count and thyroid-stimulating hormone and a comprehensive metabolic panel can be performed to rule out other pathology, additional tests are not recommended for a diagnosis unless they are clinically indicated.
Comorbid Conditions
Fibromyalgia is associated with sleep disorders. Polysomnographic findings in fibromyalgia patients include an alpha frequency rhythm, termed alpha-delta sleep anomaly. Sleep pattern is altered in these patients and there is evidence of an increase in stage 1 sleep, a reduction in delta sleep, and an increased number of arousals.13 Sleep disruption also is common in depression and other chronic pain syndromes.
Anxiety and depression are two of the most commonly encountered comorbid conditions in patients with fibromyalgia.14 Evidence in the medical literature suggests underdiagnosis and inadequate treatment of mood disorders in patients with chronic pain, including fibromyalgia.15
Headaches are present in more than one half of all patients with fibromyalgia.2,16 The high prevalence of migraine in patients with fibromyalgia suggests a common pathogenesis.16 Migraine has been characterized by a defect in the serotonergic and adrenergic systems. A parallel dramatic failure of serotonergic systems and a defect of adrenergic transmission also have been shown to affect patients with fibromyalgia.17
Patients with fibromyalgia often also have irritable bowel syndrome (IBS).18 IBS is a functional disorder of the gastrointestinal tract. Patients suffer from chronic abdominal pain and disturbed bowel function without evidence of structural or laboratory abnormalities on routine testing. An increased awareness of the clinical impact of fibromyalgia on patients with IBS, and vice versa, and recognition of the implications of this association for quality of life should enable physicians to reassure their patients regarding the nature and severity of their symptoms and to provide appropriate treatment. This may lead to a reduction in referrals and unnecessary tests for these patients.
Other disorders commonly associated with fibromyalgia include irritable bladder, dysmenorrhea, premenstrual syndrome, restless leg syndrome, temporomandibular joint pain, noncardiac chest pain, Raynaud's phenomenon, and sicca syndrome.
Differential Diagnosis
The differential diagnosis of fibromyalgia includes myofascial pain syndrome, chronic fatigue syndrome, and hypothyroidism. These conditions also can affect patients with fibromyalgia, thereby making the diagnosis more difficult.
Myofascial pain syndrome is characterized by painful, tender areas in the muscles. It is a localized disorder without any systemic manifestations. It commonly affects the axial muscles. In contrast to the widespread pain of fibromyalgia, the pain in myofascial pain syndrome arises from trigger points in individual muscles. On examination, the presence of trigger points is characteristic of myofascial pain syndrome.
Chronic pain and fatigue are common to chronic fatigue syndrome and fibromyalgia. Chronic fatigue syndrome appears to be an ongoing subclinical inflammatory process manifested by low-grade fever, lymph gland enlargement, and acute onset of the illness, whereas there is no evidence of inflammatory response in fibromyalgia.
Hypothyroidism, manifested by profound fatigue, muscle weakness, and generalized malaise, closely resembles fibromyalgia. Patients need to be examined for clinical signs of thyroid dysfunction and, if in doubt, thyroid function tests should be ordered to rule out hypothyroidism.
The differential diagnosis also might include metabolic and inflammatory myopathies (especially in patients taking statins), polymyalgia rheumatica, and other rheumatic diseases.19
Management
Although pharmacologic treatment remains the mainstay of therapy for the majority of patients with fibromyalgia, recent evidence shows that the optimal intervention is an approach that also includes nonpharmacologic treatments, specifically exercise and cognitive behavior therapy20,21 (Table 222 ). In fact, the American Pain Society Fibromyalgia Panel recommends a multidisciplinary clinical approach including education, cognitive behavior strategies, physical training, and medications for treatment of fibromyalgia.22
Table 2. Treatment of Fibromyalgia Syndrome
| Effectiveness | Pharmacologic therapies | Nonpharmacologic therapies |
|---|---|---|
| Strong evidence |
|
|
| Moderate evidence |
|
|
| Weak evidence | — |
|
| No evidence |
|
|
Adapted with permission from Goldenberg DL, Burckhardt C, Crofford L. Management of fibromyalgia syndrome. JAMA 2004;292:2390.
PHARMACOLOGIC TREATMENT
Although currently there are no medications approved by the U.S. Food and Drug Administration for treatment of fibromyalgia, there is evidence that antidepressant medications improve pain, sleep quality, and global well-being in these patients. Tricyclic antidepressants, specifically amitriptyline 25 to 50 mg at bedtime, are effective in providing analgesic effect, aiding sleep, and treating concomitant mood disorders.23 Although selective serotonin reuptake inhibitors in general have poor analgesic effect, 80 mg per day of fluoxetine (Prozac) has been shown to have a small but significant effect on symptoms in women with fibromyalgia.24 The combination of amitriptyline and fluoxetine has been determined to be more effective than either agent alone, and physicians should consider this unless otherwise contraindicated.25
Newer serotonin-norepinephrine reuptake inhibitors like duloxetine (Cymbalta) and milnacipran (not available in the United States) have shown some promise in improving symptoms of fibromyalgia. Duloxetine 60 mg twice per day has been shown to be effective in improving the pain and tenderness in patients who have fibromyalgia with or without major depressive disorders.26 The potential adverse effects of duloxetine include insomnia, dry mouth, and constipation. A double-blind, placebo-controlled trial of milnacipran showed some reduction in pain intensity and overall improvement of symptoms when compared with placebo.27 Although venlafaxine (Effexor) has been effective in alleviating pain and depressive symptoms in small trials,28,29 this has not yet been corroborated by placebo-controlled, double-blind studies.
Tramadol (Ultram), a central-acting narcotic analgesic, is effective in patients with mild to moderately severe pain. It should be titrated to avoid nausea and dizziness associated with high initial doses. A tramadol/acetaminophen (Ultracet) (37.5/325 mg) combination has been shown to be effective for fibromyalgia pain without any serious adverse effects.30 The muscle relaxant cyclobenzaprine (Flexeril) (10 to 30 mg at bedtime), which is structurally similar to tricyclic antidepressants, has been shown to be effective in improving sleep and decreasing pain.31 Nonsteroidal anti-inflammatory drugs have no evidence of effectiveness, although they are commonly used. The use of chronic analgesics can set up a cycle of rebound headaches, thus complicating the management of fibromyalgia.
A recent study has shown that pregabalin (Lyrica) (a second-generation anticonvulsant that is used for neuropathic pain, postherpetic neuralgia, and epilepsy) has been effective at a dosage of 450 mg per day in relieving pain, decreasing fatigue, and improving sleep.32 Side effects include dizziness, increased sleepiness, weight gain, and peripheral edema.
NONPHARMACOLOGIC MANAGEMENT
Exercise. Exercise is one of the nonpharmacologic strategies advocated for patients with fibromyalgia. In several clinical trials, pain was the outcome variable that most commonly improved in patients in the experimental groups.33,34 The major goal is to maintain function in everyday activities. Any exercise program should include multiple dimensions: strength, aerobic (endurance) conditioning, flexibility, and balance. Many studies have shown that aerobic exercise produces significant positive changes in patients. Exercise should be low impact and of sufficient intensity to change aerobic capacity.35,36
Cognitive Behavior Strategies. Evidence suggests that cognitive and behavioral strategies are effective in treating patients with fibromyalgia.37 The major goal of cognitive behavior therapy is to help patients understand the effect that thoughts, beliefs, and expectations have on their symptoms. One of the most useful behavioral skills is to prioritize time so that a balance between meaningful work, leisure, and the activities of daily living is achieved.38
Patient Education. Evidence shows that intensive patient education is an effective treatment for fibromyalgia when used in combination with other modalities such as behavioral therapy and exercise.39 Although a significant portion of patient education takes place informally during the physician-patient interaction, the effectiveness of organized educator programs in providing information, facilitating behavior change, and improving symptoms is well documented. This can be done using lectures, written materials, group discussions, and demonstrations.22 A self-help course specific to fibromyalgia is available through the Arthritis Foundation. Other useful sites are the Fibromyalgia Network Web site (http://www.fmnetnews.com) and the American College of Rheumatology site (http://www.rheumatology.org).
Complementary and Alternative Therapy. The effectiveness of acupuncture and biofeedback has been supported by some studies.40,41 Serum levels of substance P and serotonin were significantly elevated after acupuncture treatment, suggesting possible mechanisms in pain relief.42 Although their effectiveness has not been proven by controlled trials, other treatment modalities employed include chiropractic therapy, yoga, tai chi, massage therapy, magnetic therapy, and tender-point injections.

