A 64-year-old woman presented with a one-month history of painful nodules that started on her right hand and extended to her upper arm. The nodules began with a single lesion on her right middle finger (Figure 1), which had since become crusted and violaceous. Over the course of the month, the lesions began to appear on her arm and spread (Figure 2). She had no fever or chills, and denied experiencing any trauma. Previous treatment with a 10-day course of cephalexin (Keflex) had not altered the lesions.
Figure 1.
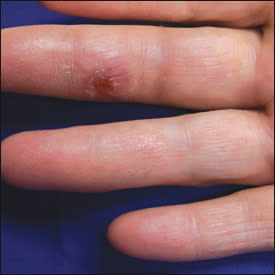
Figure 2.
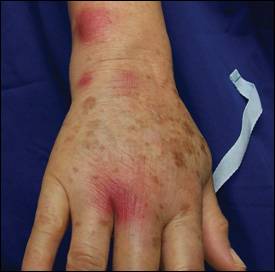
Her medical history included hypertension, gastroesophageal reflux, and chronic lymphocytic leukemia four years earlier that had not required treatment. She had no allergies and was taking hydrochlorothiazide (Microzide), rabeprazole (Aciphex), and estrogen. After recently retiring, she was enjoying her hobby of collecting tropical fish. She denied any other new activities or exposures.
On examination, markedly tender, violaceous nodules beginning on the dorsal web space of her right third and fourth fingers, dorsolateral wrist, and mid-biceps region were noted. The lesion over her ulnar styloid was fluctuant. Her middle finger and dorsal hand were slightly swollen and tender.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Buruli ulcer.
B. Mycobacterium marinum infection.
C. Sporotrichosis.
D. Staphylococcal abscess.
E. Streptococcal cellulitis.
Discussion
The answer is B: Mycobacterium marinum. Infection with M. marinum most commonly results in a granulomatous skin infection, also known as “fish tank” or “swimming pool” granulomas, that can occur after exposure to contaminated fresh- or saltwater. Persons whose occupations may expose them to contaminated fresh- or saltwater are also at risk. Previous skin trauma or open wound, in addition to an occupation or hobby involving environmental water, may indicate possible M. marinum infection.
Diagnosis is usually obtained by tissue culture, although clinical suspicion is often enough to begin presumptive treatment in areas without adequate testing facilities. Fluorochrome staining can also identify acid-fast bacilli, but it does not allow species identification.
Primary skin lesions typically present as a solitary, erythematous nodule or papule on an extremity. This lesion can slowly enlarge into a verrucous plaque and become more violaceous. About 20 to 40 percent of patients have a “sporotrichoid spread” of lesions along areas of lymphatic drainage.1 Occasionally these nodules ulcerate, releasing a serosanguineous discharge. Painful lesions occur in less than one half of cases.2
M. marinum infections are usually confined to the skin; however, deeper infections have occurred.3 Invasion into deeper tissue may result in arthritis, bursitis, tenosynovitis, and osteomyelitis. Localized lymphadenopathy and systemic symptoms are uncommon.4 A significant time lapse between the initial appearance of symptoms and the seeking of medical attention is common.
The optimal treatment for M. marinum infection is unknown. The most commonly described therapies are tetracyclines, clarithromycin (Biaxin), rifampin (Rifadin), ethambutol (Myambutol), and trimethoprim/sulfa-methoxazole (Bactrim, Septra).3 Other drugs, including levofloxacin (Levaquin) and amikacin (Amikin), are used less often. Treatment success and failure have been reported with almost all antimicrobial agents.3,5,6
Suggestions for initial therapy include minocycline (Minocin), doxycycline (100 mg twice daily), or clarithromycin (500 mg twice daily) for relatively uncomplicated cases.5,7 An alternative is to add ethambutol, 15 to 25 mg per kg daily, to rifampin (600 mg daily) or clarithromycin (500 mg twice daily) for more widespread cases. Duration of therapy will vary by case, but treatment should continue for four to eight weeks after the lesions have disappeared. Surgical debridement should be reserved for infections that involve the deep tissues or cause continual pain.4 Surgery, cryotherapy, electrodesiccation, and irradiation have been proposed to treat M. marinum infections; however, no method has been proven more effective than another.5
Buruli ulcer, caused by Mycobacterium ulcerans, is the third most common mycobacterial disease worldwide and is endemic in much of central and western Africa. However, no cases have been reported in the United States. It is best characterized as a chronic, indolent, necrotizing disease presenting as a painless subcutaneous nodule over sites of skin trauma. Eventually the nodules ulcerate, sometimes spreading extensively to other parts of the body.
Sporotrichosis (Sporothrix schenckii) is characterized by a painless erythematous nodule occurring at the inoculation site. It presents in a pattern similar to M. marinum infection, and lesions may ulcerate. Occupational or recreational exposure is likely.
Staphylococcal and streptococcal infections can cause skin diseases such as cellulitis and abscess. However, they do not usually develop slowly and do not typically show sporotrichoid spread. Furthermore, most such cases would promptly respond to common antimicrobials.
Selected Differential Diagnosis of Painful Erythematous Nodules
| Condition | Characteristics |
|---|---|
| Buruli ulcer | Firm, nontender nodules, 1 to 2 cm in size; extensive tissue destruction may result |
| Mycobacterium marinum | Erythematous nodule, 0.5 to 3.0 cm in size, on extremity; may show “sporotrichoid spread”; disseminated disease uncommon |
| Sporotrichosis | Sporotrichoid spread; erythematous nodules; slow-healing ulcers |
| Staphylococcal abscess | Pustules and deep-seated nodules with surrounding edema and erythema |
| Streptococcal cellulitis | Erythematous, tender, swollen areas with a distinct border; acute course with advancing area of involvement; fever, malaise, leukocytosis |

