Background: Anxiety disorders have significant lifetime effects on work productivity, patient functioning, and health-related expenditures in an estimated 30 million Americans. Although effective therapies exist, previous studies have suggested that patients with these disorders go largely unrecognized in primary care. Kroenke and colleagues determined the prevalence of the four most common anxiety disorders (i.e., generalized anxiety disorder, panic disorder, social anxiety disorder, and post-traumatic stress disorder [PTSD]) in a research network of primary care practices. Additionally, they validated a brief screening questionnaire for generalized anxiety disorders and assessed functional impairment and symptoms in patients with an anxiety disorder.
The Study: Adult patients from 13 family medicine and two internal medicine practices in 12 states were enrolled in the study. All patients completed a questionnaire that included demographic information; functional status measures; several previously validated psychiatric scales; and the seven-item Generalized Anxiety Disorder scale. This scale assesses anxiety on a scale of 0 to 21; increasing scores represent increasing degrees of anxiety (see accompanying figure). Of the 2,149 consecutive patients who were invited to participate in the validation substudy, 1,654 patients agreed to undergo a structured telephone interview with a mental health professional, but only 965 patients were randomly selected to be interviewed. These interviews were used to diagnose patients with anxiety disorders according to the Diagnostic and Statistical Manual of Mental Disorders, 4th ed., criteria. Interviewers were blinded to the results of the questionnaire.
Results: The most common anxiety disorder identified among the study population was PTSD (83 patients), followed by generalized anxiety disorder (73 patients), panic disorder (66 patients), and social anxiety disorder (60 patients). More than one third (64 patients) of patients with anxiety disorders had more than one disorder, and 41 percent (77 patients) were not currently receiving pharmacologic or behavioral treatments. The number of anxiety disorders was strongly associated with self-reported disability and worsened functional status. Although it was designed only to specifically detect generalized anxiety, the Generalized Anxiety Disorder scale had good sensitivity and specificity for detecting any of the four disorders, depending on the cutoff point used.
Figure. Generalized Anxiety Disorder Scale
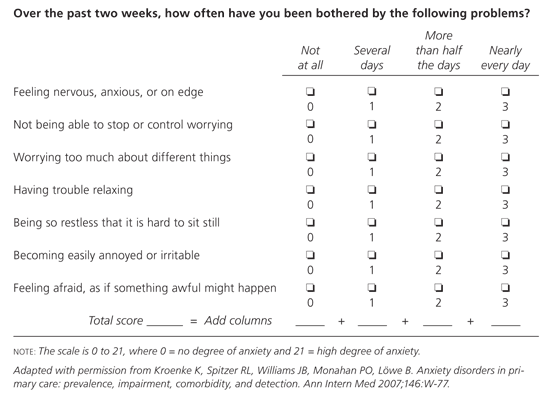
Generalized Anxiety Disorder Scale.
Conclusion: These four anxiety disorders are common among patients in primary care and produce similar symptoms, functional impairment, comorbidities, and disability. Additionally, a substantial number of patients had one or more anxiety disorders or were not receiving any treatment. The Generalized Anxiety Disorder scale, however, shows promise as a brief screening instrument for patients with anxiety.
editor's note: In an accompanying editorial, Katon and Roy-Byrne note that the high prevalence of anxiety disorders and the existence of accurate screening instruments do not by themselves mean that screening for anxiety disorders should be performed in primary care.1 As the U.S. Preventive Services Task Force noted about screening for depression, physicians must have systems in place to ensure effective follow-up and monitor adherence to prescribed treatments to improve health outcomes.2 Close collaboration between family physicians and mental health professionals can achieve this goal.—k.l.

