Diagnostic criteria for acute otitis media include rapid onset of symptoms, middle ear effusion, and signs and symptoms of middle ear inflammation. Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis are the most common bacterial isolates from the middle ear fluid of children with acute otitis media. Fever, otalgia, headache, irritability, cough, rhinitis, listlessness, anorexia, vomiting, diarrhea, and pulling at the ears are common, but nonspecific symptoms. Detection of middle ear effusion by pneumatic otoscopy is key in establishing the diagnosis. Observation is an acceptable option in healthy children with mild symptoms. Antibiotics are recommended in all children younger than six months, in those between six months and two years if the diagnosis is certain, and in children with severe infection. High-dosage amoxicillin (80 to 90 mg per kg per day) is recommended as first-line therapy. Macrolide antibiotics, clindamycin, and cephalosporins are alternatives in penicillin-sensitive children and in those with resistant infections. Patients who do not respond to treatment should be reassessed. Hearing and language testing is recommended in children with suspected hearing loss or persistent effusion for at least three months, and in those with developmental problems.
Acute otitis media, a viral or bacterial infection of the middle ear, is the most common infection for which antibiotics are prescribed for children in the United States.1,2 Direct and indirect costs of treatment and time lost from school and work because of acute otitis media totaled nearly $3 billion in 1995.3 Acute otitis media is most common between six and 24 months of age; by age three, more than 80 percent of children have been diagnosed.4
Otitis media with effusion is middle ear effusion in the absence of acute infection. About 2.2 million cases of otitis media with effusion occur annually in the United States.5 Chronic suppurative otitis media is persistent infection and resultant perforation of the tympanic membrane.6 This article will review recent evidence, including the evidence-based guideline from the American Academy of Pediatrics and the American Academy of Family Physicians, about the diagnosis and treatment of acute otitis media and otitis media with effusion.1,5
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Diagnosis of acute otitis media requires confirmation of acute onset, identification of signs of middle ear effusion, and evaluation for signs and symptoms of middle ear inflammation. | C | 1 |
| Antihistamines and decongestants should not be prescribed for children with acute otitis media or otitis media with effusion. | B | 5, 22 |
| Observation without antibiotic therapy is an option in selected children with acute otitis media. | B | 1, 22 |
| Amoxicillin at a dosage of 80 to 90 mg per kg per day should be the first-line antibiotic for most children with acute otitis media. | B | 1 |
| Patients with otitis media who fail to respond to the initial treatment option within 48 to 72 hours should be reassessed to confirm the diagnosis. If the diagnosis is confirmed, antibiotics should be started in patients for whom antibiotics were initially deferred, and a different antibiotic should be prescribed for patients already taking an antibiotic. | C | 1 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 1595 or https://www.aafp.org/afpsort.xml.
Pathophysiology
Genetic, infectious, immunologic, and environmental factors predispose children to ear infections (Table 1).4,7 In most cases, an allergy or upper respiratory tract infection causes congestion and swelling of the nasal mucosa, nasopharynx, and eustachian tube. Obstruction at the eustachian tube isthmus (i.e., the narrowest portion) results in accumulation of middle ear secretions; secondary bacterial or viral infection of the effusion causes suppuration and features of acute otitis media.8 The effusion may persist for weeks or months after the infection resolves.4 Otitis media with effusion may occur spontaneously as a result of eustachian tube dysfunction or as an inflammatory response after acute otitis media.5
Table 1 Factors Affecting Risk of Acute Otitis Media
| Factor | Comments |
|---|---|
| Age | Maximal incidence between six and 24 months of age; eustachian tube shorter and less angled at this age. Underdeveloped physiologic and immunologic responses to infection in children |
| Breastfeeding | Breastfeeding for at least three months is protective; this effect may be associated with position maintained during breastfeeding, suckling movements, and protective factors in breast milk |
| Daycare attendance* | Contact with multiple children and daycare providers facilitates spread of bacterial and viral pathogens |
| Ethnicity* | Native American, Alaskan, and Canadian Inuit children have increased incidence |
| Exposure to cigarette smoke | Increased incidence with cigarette smoke and air pollution, especially if parents smoke |
| Male sex | Slightly increased incidence |
| More than one sibling living at home* | Increased risk of antibiotic treatment failure |
| Pacifier use | Increased incidence |
| Previous antibiotic use* | Increased risk of antibiotic treatment failure |
| Previous otitis media* | Increased risk of antibiotic treatment failure |
| Season* | Increased incidence in fall and winter |
| Underlying pathology* | Increased incidence in children with allergic rhinitis, cleft palate, Down syndrome |
*— These factors also increase the risk of recurrent acute otitis media.
Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis are the most common bacterial isolates from the middle ear fluid of children with acute otitis media (Table 24,6–10).8–10 Penicillin-resistant S. pneumoniae is the most common cause of recurrent and persistent acute otitis media.7
Table 2 Organisms in Acute and Chronic Suppurative Otitis Media
| Organism | Frequency (%) | Comments |
|---|---|---|
| Acute otitis media | ||
| Streptococcus pneumoniae* | 40 to 50 | Most common pathogens are serotypes 19F, 23F, 14, 6B, 6A, 19A, and 9V |
| Haemophilus influenzae* | 30 to 40 | Nearly one half produce β-lactamase |
| Moraxella catarrhalis* | 10 to 15 | Most produce β-lactamase |
| Group A streptococcus* | — | Common in older children. More frequently associated with perforated tympanic membrane and mastoiditis |
| Staphylococcus aureus* | Rare | More common in chronic infection |
| Anaerobic organisms | Rare | More common in chronic infection |
| Gram-negative bacilli | — | In newborns, immunosuppressed patients, and patients with chronic suppurative otitis media |
| Viruses | Less than 10 | Respiratory syncytial virus, adenovirus, rhinovirus, or influenza virus may act in synergy with bacteria. Coinfection with bacteria present in more than 40 percent of children with viral-induced acute otitis media |
| Other | Rare | Mycoplasma pneumoniae, Chlamydia pneumoniae, Chlamydia trachomatis (in infants younger than six months), Mycobacterium tuberculosis (in developing countries), parasitic infestation (e.g., ascariasis), mycotic infections (e.g., candidiasis, aspergillosis, blastomycosis) |
| Chronic suppurative otitis media | ||
| Aerobic organisms | — | Pseudomonas aeruginosa, Proteus mirabilis, S. aureus, Streptococcus pyogenes, Escherichia coli, or Klebsiella species |
| Anaerobic organisms | — | Bacteroides, Peptostreptococcus, or Propionibacterium species |
note:No bacterial pathogen is identified in up to 20 to 30 percent of patients with acute otitis media.
*— Also responsible for recurrent and persistent otitis media.
Diagnosis
Diagnostic criteria for acute otitis media include rapid onset of symptoms, middle ear effusion, and signs and symptoms of middle ear inflammation (Table 31,2,6,7,11).1 Nonspecific symptoms of acute otitis media (e.g., fever, headache, irritability, cough, rhinitis, listlessness, anorexia, vomiting, diarrhea, pulling at the ears) are common in infants and young children. Otalgia is less common in children younger than two years and more common in adolescents and adults.4 Acute otitis media cannot be reliably differentiated from upper respiratory tract infection on the basis of symptoms alone.10 However, otalgia, ear rubbing or pulling, and parental suspicion of otitis media have positive likelihood ratios (LR+) of 3.0 or more and are moderately useful for ruling in the diagnosis (Table 412–16).12,13
Table 3 Diagnostic Criteria for Otitis Media
| Type | Diagnostic criteria | |
|---|---|---|
| Acute otitis media | Acute onset | |
| and | ||
| Middle ear effusion, indicated by bulging tympanic membrane, limited or absent mobility of membrane, air-fluid level behind membrane | ||
| and | ||
| Symptoms and signs of middle ear inflammation, indicated by erythema of tympanic membrane or otalgia affecting sleep or normal activity | ||
| Persistent acute otitis media | Persistent features of middle ear infection during antibiotic treatment | |
| or | ||
| Relapse within one month of treatment completion | ||
| Recurrent acute otitis media | Three or more episodes of acute otitis media within six to 18 months | |
| Otitis media with effusion | Fluid behind the tympanic membrane in the absence of features of acute inflammation | |
| Chronic otitis media with effusion | Persistent fluid behind intact tympanic membrane in the absence of acute infection | |
| Chronic suppurative otitis media | Persistent inflammation of the middle ear or mastoid cavity | |
| Recurrent or persistent otorrhea through a perforated tympanic membrane | ||
Table 4 Usefulness of Clinical Findings and Tests in the Diagnosis of Acute Otitis Media
| Clinical feature | Sensitivity (%) | Specificity (%) | LR+* | LR–† |
|---|---|---|---|---|
| Signs | ||||
| Bulging tympanic membrane14 | 61 | 97 | 20.3 | 0.4 |
| Cloudy tympanic membrane14 | 81 | 95 | 16.2 | 0.2 |
| Impaired mobility of tympanic membrane14 | 98 | 79 | 4.7 | 0.03 |
| Symptoms | ||||
| Parental suspicion of otitis media12 | 70 | 80 | 3.4 | 0.4 |
| Pulling at or rubbing the ear13 | 42 | 87 | 3.3 | 0.7 |
| Otalgia13 | 54 | 82 | 3.0 | 0.6 |
| Excessive crying13 | 55 | 69 | 1.8 | 0.7 |
| Rhinitis13 | 75 | 43 | 1.3 | 0.6 |
| Poor appetite13 | 36 | 66 | 1.1 | 1.0 |
| Cough13 | 47 | 45 | 0.9 | 1.2 |
| Fever13 | 40 | 48 | 0.8 | 1.2 |
| Diagnostic methods | ||||
| Acoustic reflectometry16 | 65 to 97 | 85 to 99 | ||
| Pneumatic otoscopy15 | 94 | 81 | ||
| Portable tympanometry15 | 89 | 58 | ||
| Professional tympanometry15 | 34 to 94 | 49 to 94 | ||
LR+ = positive likelihood ratio; LR− = negative likelihood ratio.
*— Higher values indicate a greater likelihood of acute otitis media when the sign or symptom is present.
†— Lower values indicate a lower likelihood of acute otitis media when the sign or symptom is absent.
PNEUMATIC OTOSCOPY AND OTHER DIAGNOSTIC TESTS
Detection of middle ear effusion by pneumatic otoscopy is key in establishing the diagnosis of acute otitis media. The tympanic membrane normally is convex, mobile, translucent, and intact; a normal color and mobility of the membrane indicate that otitis media is unlikely (negative likelihood ratio [LR–], 0.03).10 A bulging membrane greatly increases the likelihood of otitis media (LR+, 20.3), as do impaired mobility of the membrane (LR+, 4.7) and a distinctly red membrane (LR+, 2.6), albeit to a lesser extent.14
Using pneumatic otoscopy with tympanometry improves the accuracy of diagnosis. The handheld tympanometer records compliance of the tympanic membrane and provides quantitative information on structural function and the presence of middle ear effusion.15 A flattened tracing with a low static admittance (type B tracing) indicates middle ear effusion; highly negative middle ear pressures (type C tracing) indicate a retracted tympanic membrane; and highly positive peak pressures are consistent with a bulging membrane15 (Figure 1). Acoustic reflectometry detects middle ear fluid by analyzing the spectral gradient of sound reflected off the tympanic membrane.16
Figure 1.
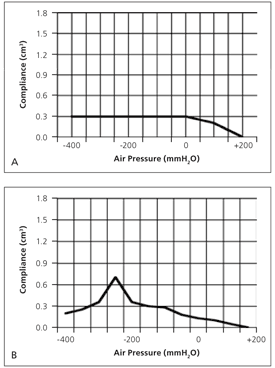
Sample tympanograms. (A) Results suggest middle ear effusion. (B) Results correlate with retracted tympanic membrane.
Information from Esse S, Thibodeau L. Pediatric hearing loss: diagnostic evaluation. Accessed online July 23, 2007, at: http://www.utdallas.edu/~thib/rehabinfo/de.htm.
Tympanocentesis, followed by aspiration and culture of middle ear fluid samples, is useful in children who are toxic, have failed multiple courses of antibiotics, or have immune deficiencies.4 Although negative nasopharyngeal cultures correlate well with negative middle ear fluid cultures, they are not routinely recommended.17
Chronic suppurative otitis media presents with persistent or recurrent otorrhea through a perforated tympanic membrane (active), or with a dry but permanent perforation of the tympanic membrane (inactive).6 Other features include thickened granular mucosa, polyps, and cholesteatoma in the middle ear.18 Aerobic and anaerobic bacteria may enter the middle ear through the perforation.6 Rarely, Pseudomonas species may cause deep-seated destructive infections of the middle ear and the mastoid cavity. Diagnosis is made by history and examination, including otoscopy. Examination may detect other foci of infection requiring treatment (e.g., nose, paranasal sinuses, lungs, pharynx). Careful cleaning of the ear is useful for visualizing the tympanic membrane and the attic, and for excluding cholesteatoma.19
Treatment
ACUTE OTITIS MEDIA
Treatment goals in acute otitis media include symptom resolution and reduction of recurrence.20 Most children with acute otitis media (70 to 90 percent) have spontaneous resolution within seven to 14 days; therefore, antibiotics should not routinely be prescribed initially for all children.21,22 Delaying antibiotic therapy in selected patients reduces treatment-related costs and side effects and minimizes emergence of resistant strains.23
Symptomatic Treatment. Pain management is important in the first two days after diagnosis. Options include acetaminophen (15 mg per kg every four to six hours) and ibuprofen (Motrin; 10 mg per kg every six hours).24 Antipyrine/benzocaine otic suspension (Auralgan) can be used for local analgesia (Table 5).1,5,25
Table 5 Agents Used in the Treatment of Otitis Media
| Agent | Dosage | Comments |
|---|---|---|
| Antimicrobials* | ||
| Amoxicillin | 80 to 90 mg per kg per day, given orally in two divided doses | First-line drug. Safe, effective, and inexpensive |
| Amoxicillin/clavulanate (Augmentin) | 90 mg of amoxicillin per kg per day; 6.4 mg of clavulanate per kg per day, given orally in two divided doses | Second-line drug. For patients with recurrent or persistent acute otitis media, those taking prophylactic amoxicillin, those who have used antibiotics within the previous month, and those with concurrent purulent conjunctivitis |
| Azithromycin (one dose; Zithromax) | 30 mg per kg, given orally | For patients with penicillin allergy. One dose is as effective as longer courses |
| Azithromycin (three-day course; Zithromax Tripak) | 20 mg per kg once daily, given orally | For patients with recurrent acute otitis media |
| Azithromycin (five-day course; Zithromax Z-pak) | 5 to 10 mg per kg once daily, given orally | For patients with penicillin allergy (type 1 hypersensitivity) |
| Cefdinir (Omnicef) | 14 mg per kg per day, given orally in one or two doses | For patients with penicillin allergy, excluding those with urticaria or anaphylaxis to penicillin (i.e., type 1 hypersensitivity) |
| Cefpodoxime (Vantin) | 30 mg per kg once daily, given orally | For patients with penicillin allergy, excluding those with urticaria or anaphylaxis to penicillin (i.e., type 1 hypersensitivity) |
| Ceftriaxone (Rocephin) | 50 mg per kg once daily, given intramuscularly or intravenously. One dose for initial episode of otitis media, three doses for recurrent infections | For patients with penicillin allergy, persistent or recurrent acute otitis media, or vomiting |
| Cefuroxime (Ceftin) | 30 mg per kg per day, given orally in two divided doses | For patients with penicillin allergy, excluding those with urticaria or anaphylaxis to penicillin (i.e., type 1 hypersensitivity) |
| Clarithromycin (Biaxin) | 15 mg per kg per day, given orally in three divided doses | For patients with penicillin allergy (type 1 hypersensitivity). May cause gastrointestinal irritation |
| Clindamycin (Cleocin) | 30 to 40 mg per kg per day, given orally in four divided doses | For patients with penicillin allergy (type 1 hypersensitivity) |
| Topical agents† | ||
| Ciprofloxacin/hydrocortisone (Cipro HC Otic) | 3 drops twice daily | — |
| Hydrocortisone/neomycin/polymyxin B (Cortisporin Otic) | 4 drops three to four times daily | — |
| Ofloxacin (Floxin Otic) | 5 drops twice daily (10 drops in patients older than 12 years) | — |
| Analgesics | ||
| Acetaminophen | 15 mg per kg every six hours [ | — |
| Antipyrine/benzocaine (Auralgan) | 2 to 4 drops three to four times daily | — |
| Ibuprofen (Motrin) | 10 mg per kg every six hours | — |
| Narcotic agents | Variable | May cause gastrointestinal upset, respiratory depression, altered mental status, and constipation |
*— These drugs should be given for 10 days, unless otherwise indicated. A five- to seven-day course is an option for patients six years and older. These agents may cause diarrhea, vomiting, abdominal pain, rash, anorexia, and dermatitis.
†— These drugs should be used for seven to 10 days in patients with chronic suppurative otitis media.
Antihistamines may help with nasal allergies, but they may prolong middle ear effusion.26 Oral decongestants may be used to relieve nasal congestion. However, neither antihistamines nor decongestants improve healing or minimize complications of acute otitis media, and they are not routinely recommended.27 Corticosteroid use has no benefit in acute otitis media.26
Antibiotics. A meta-analysis of randomized trials found that antibiotics are most beneficial in children younger than two years with bilateral acute otitis media and in children with acute otitis media and otorrhea.28 Antibiotics are recommended for all children younger than six months, for those six months to two years of age when the diagnosis is certain, and for all children older than two years with severe infection (defined as moderate to severe otalgia or temperature greater than 102.2° F [39° C]).1 Antibiotics may be deferred in otherwise healthy children six months to two years of age with mild otitis in whom the diagnosis is uncertain, and in children older than two years with mild symptoms or in whom the diagnosis is uncertain (Figure 2).1,5 If this option is chosen, it is mandatory to have a reliable care-giver who will observe the child, recognize signs of serious illness, and be able to access medical care easily.
Figure 2. Management of Otitis Media
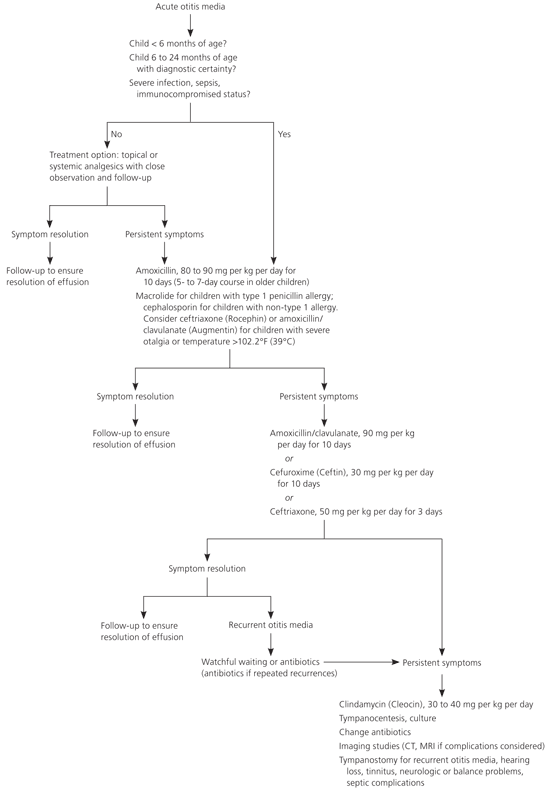
Treatment algorithm for acute otitis media. (CT = computed tomography; MRI = magnetic resonance imaging.)
Information from references 1 and 5.
Antibiotic Selection. High-dosage amoxicillin (80 to 90 mg per kg per day, divided into two daily doses for 10 days) is recommended as first-line antibiotic therapy in children with acute otitis media.1,24 In children older than six years with mild to moderate disease, a five- to seven-day course is adequate.1 Amoxicillin is effective, safe, and relatively inexpensive, and it has a narrow microbiologic spectrum.29 First-line treatment with amoxicillin is not recommended in children with concurrent purulent conjunctivitis, after antibiotic therapy within the preceding month, in children taking amoxicillin as chemoprophylaxis for recurrent acute otitis media or urinary tract infection, and in children with penicillin allergy.
Cephalosporins may be used in children allergic to penicillin if there is no history of urticaria or anaphylaxis to penicillin. If there is a history of penicillin-induced urticaria or anaphylaxis, a macrolide (e.g., azithromycin [Zithromax], clarithromycin [Biaxin]) or clindamycin [Cleocin] may be used. A single dose of parenteral ceftriaxone (Rocephin, 50 mg per kg) may be useful in children with vomiting or in whom compliance is a concern.1 Single-dose azithromycin is safe and effective in uncomplicated acute otitis media and compares well with longer courses of azithromycin or other antibiotics.30
Persistent Acute Otitis Media. If there is no clinical improvement within 48 to 72 hours, the patient must be reassessed to confirm the diagnosis, exclude other causes of illness, and initiate antibiotic therapy in those on symptomatic treatment alone. Patients who are already taking antibiotics should be changed to second-line therapy.1 Options include high-dose amoxicillin/clavulanate (Augmentin), cephalosporins, and macrolides. Parenteral ceftriaxone administered daily over three days is useful in children with emesis or resistance to amoxicillin/clavulanate. For children who do not respond to second-line antibiotics, clindamycin and tympanocentesis are appropriate options. Although it is not approved for use in children, levofloxacin (Levaquin) is effective in children who have persistent or recurrent acute otitis media.31
Computed tomography (CT) is useful if bony extension is suspected. Magnetic resonance imaging is superior to CT in evaluating potential intracranial complications.32
Recurrent Acute Otitis Media. Most children with recurrent acute otitis media improve with watchful waiting.20 Although antibiotic prophylaxis may reduce recurrence, there are no widely accepted recommendations for antibiotic choice or prophylaxis duration.33 Minimizing risk factors (e.g., exposure to cigarette smoke, pacifier use, bottle feeding, daycare attendance) decreases recurrence. Heptavalent pneumococcal vaccine (Prevnar) reduces the incidence of acute otitis media, but it does not reduce recurrence.
OTITIS MEDIA WITH EFFUSION
Persistent middle ear effusion after resolution of acute otitis media does not indicate treatment failure and requires only monitoring and reassurance. Risk factors for persistent acute otitis media with effusion include hearing loss greater than 30 dB, prior tympanostomy tube placement, adenoid hypertrophy, and onset during summer or fall.34
Clinical examination, pneumatic otoscopy, and tympanometry may be performed during the observation period.5 There is no role for antihistamines and decongestants; adverse effects include insomnia, hyperactivity, drowsiness, behavioral changes, and labile blood pressure.5 Oral and topical intranasal corticosteroids alone or in combination with an antibiotic produce faster short-term resolution of otitis media with effusion, but there is no evidence of long-term benefit.35 Autoinflation (i.e., opening the eustachian tube by raising intranasal pressure) is useful in older children with persistent acute otitis media with effusion who are able to perform the Valsalva maneuver.36
Children older than two years who have otitis media with effusion and no developmental issues must be seen at three- to six-month intervals until effusion resolves, hearing loss is identified, or structural abnormalities of the tympanic membrane or middle ear are suspected.5 Hearing and language testing is recommended in patients with suspected hearing loss or persistent effusion for at least three months, or when developmental problems are identified. Children with hearing loss of 20 dB or less who do not have speech, language, or developmental problems can be observed. Those with hearing loss of 21 to 39 dB can be observed or referred for surgery, and those with hearing loss of 40 dB or more should be referred for surgery.5
Tympanostomy with ventilation tube insertion is the preferred initial procedure. Meta-analyses of randomized controlled trials evaluating the effect of ventilation on hearing, effusion duration, language development, cognition, behavior, and quality of life show that benefits in children are marginal at best.37,38 Ventilation tubes may be more beneficial in young children in an environment with a high infection load (e.g., children attending daycare) and in older children with hearing loss of 25 dB or greater in both ears for at least 12 weeks.37 Adenoidectomy may be considered in children who have recurrent otitis media with effusion after tympanostomy (20 to 50 percent of children) if chronic adenoiditis is present or if adenoidal hypertrophy causes nasal obstruction.5 Tonsillectomy does not improve outcomes. Complications of tympanostomy include transient and persistent otorrhea, tympanosclerosis, atrophy, perforation of the tympanic membrane, and cholesteatoma.39 A mild conductive hearing loss may also occur as a result of changes in the tympanic membrane. Topical antibiotics (e.g., quinolones, aminoglycosides, polymyxins) are more effective than systemic antibiotics in clearing the infection in patients with chronic suppurative otitis media; topical quinolones are preferred.6 Nonquinolone antibiotics may produce ototoxicity and vestibular dysfunction, but these complications are unlikely with short-term use.39 Oral or parenteral antibiotics are useful in patients with systemic sepsis or inadequate response to topical antibiotics. They should be selected on the basis of culture and sensitivity results. Tympanoplasty (using a soft-tissue graft), with reconstruction of the ossicular chain if necessary, is an option in patients with chronic perforation and hearing loss. Mastoidectomy is often recommended for patients with chronic mastoiditis.
Complications
The overall incidence of complications from otitis media is extremely low; infratemporal and intracranial complications occur in one in 100,000 children and in one in 300,000 adults per year.40,41 Patients with middle ear effusion may have persistent or fluctuating conductive hearing loss (loss of about 25 dB).4 Children with chronic middle ear effusion score lower on tests of speech, language, and cognitive abilities.42 Central perforation of the eardrum may cause chronic infection in the middle ear and mastoid cavity. Acute mastoiditis (i.e., pus in the mastoid air cells) may erode through the bone, forming a subcutaneous collection of pus (Bezold's abscess). Contiguous spread or hematogenous seeding may infect the inner ear, petrous portion of the temporal bone, meninges, and the brain. Mastoiditis and intracranial complications of acute otitis media are more common in developing countries where persons have limited access to medical care.4
Mild to moderate conductive hearing loss occurs in one half of children with chronic suppurative otitis media, and extracranial and intracranial complications may also develop. Meningitis is the most serious intracranial complication.
Otitis Media in Adults
Adults make up less than 20 percent of patients presenting with acute otitis media.43 H. influenzae and S. pneumoniae are common bacterial isolates in these patients. Compared with children, adults more often present with otalgia, ear drainage, diminished hearing, and sore throat. Opacity and redness of the tympanic membrane are equally common in children and adults. Guidelines for antibiotic use are the same in children and adults. Smoking should be discouraged. Nasal and oral steroids may be beneficial in patients with persistent acute otitis media and associated allergies. Adults with unilateral middle ear effusion lasting longer than two months should undergo imaging studies to rule out intracranial neoplasm, especially if the effusion is associated with cranial nerve palsy.11

