
A more recent article on paronychia is available.
Am Fam Physician. 2008;77(3):339-346
Patient information: See related handout on chronic paronychia, written by the authors of this article.
Author disclosure: Nothing to disclose.
Paronychia is an inflammation of the folds of tissue surrounding the nail of a toe or finger. Paronychia may be classified as either acute or chronic. The main factor associated with the development of acute paronychia is direct or indirect trauma to the cuticle or nail fold. This enables pathogens to inoculate the nail, resulting in infection. Treatment options for acute paronychia include warm compresses; topical antibiotics, with or without corticosteroids; oral antibiotics; or surgical incision and drainage for more severe cases. Chronic paronychia is a multifactorial inflammatory reaction of the proximal nail fold to irritants and allergens. The patient should avoid exposure to contact irritants; treatment of underlying inflammation and infection is recommended, using a combination of a broad-spectrum topical antifungal agent and a corticosteroid. Application of emollient lotions may be beneficial. Topical steroid creams are more effective than systemic antifungals in the treatment of chronic paronychia. In recalcitrant chronic paronychia, en bloc excision of the proximal nail fold is an option. Alternatively, an eponychial marsupialization, with or without nail removal, may be performed.
Paronychia (synonymous with perionychia) is an inflammatory reaction involving the folds of tissue surrounding a fingernail or toenail. The condition is the result of infection and may be classified as acute or chronic. This article discusses the etiology, predisposing factors, clinical manifestation, diagnosis, and treatment of acute and chronic paronychia.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The digital pressure test may be helpful in the early stages of paronychial infection when there is doubt about the presence or extent of an abscess. | C | 14 |
| There is no evidence that treatment with oral antibiotics is any better or worse than incision and drainage for acute paronychia. | C | 23 |
| Topical steroids are more effective than systemic antifungals in the treatment of chronic paronychia. | B | 21 |
| Patients with simple chronic paronychia should be treated with a broad-spectrum topical antifungal agent and should be instructed to avoid contact irritants. | C | 22 |
Nail Structure and Function
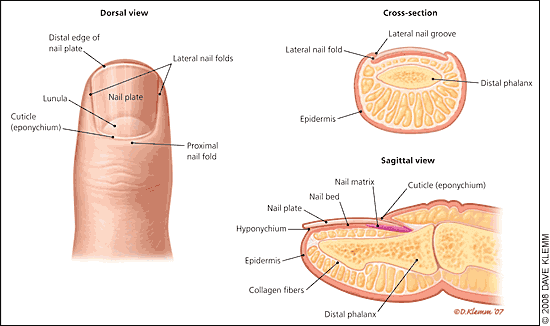
The nail is a complex unit composed of five major modified cutaneous structures: the nail matrix, nail plate, nail bed, cuticle (eponychium), and nail folds1 (Figure 1). The cuticle is an outgrowth of the proximal fold and is situated between the skin of the digit and the nail plate, fusing these structures together.2 This configuration provides a waterproof seal from external irritants, allergens, and pathogens.
Acute Paronychia
ETIOLOGY AND PREDISPOSING FACTORS
The most common cause of acute paronychia is direct or indirect trauma to the cuticle or nail fold. Such trauma may be relatively minor, resulting from ordinary events, such as dishwashing, an injury from a splinter or thorn, onychophagia (nail biting), biting or picking at a hangnail, finger sucking, an ingrown nail, manicure procedures (trimming or pushing back the cuticles), artificial nail application, or other nail manipulation.3–5 Such trauma enables bacterial inoculation of the nail and subsequent infection. The most common causative pathogen is Staphylococcus aureus, although Streptococcus pyogenes, Pseudomonas pyocyanea, and Proteus vulgaris can also cause paronychia.3,6,7 In patients with exposure to oral flora, other anaerobic gram-negative bacteria may also be involved. Acute paronychia can also develop as a complication of chronic paronychia.8 Rarely, acute paronychia occurs as a manifestation of other disorders affecting the digits, such as pemphigus vulgaris.9
CLINICAL MANIFESTATIONS
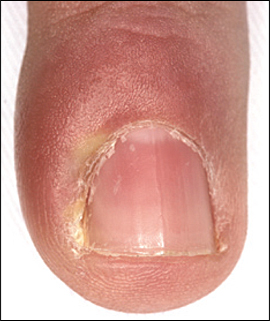
In patients with acute paronychia, only one nail is typically involved.10 The condition is characterized by rapid onset of erythema, edema, and discomfort or tenderness of the proximal and lateral nail folds,11 usually two to five days after the trauma. Patients with paronychia may initially present with only superficial infection and accumulation of purulent material under the nail fold, as indicated by drainage of pus when the nail fold is compressed12,13 (Figure 2). An untreated infection may evolve into a subungual abscess, with pain and inflammation of the nail matrix.11 As a consequence, transient or permanent dystrophy of the nail plate may occur.10 Pus formation can proximally separate the nail from its underlying attachment, causing elevation of the nail plate.10,11 Recurrent acute paronychia may evolve into chronic paronychia.7,12
DIAGNOSIS
The diagnosis of acute paronychia is based on a history of minor trauma and findings on physical examination of nail folds. The digital pressure test may be helpful in the early stages of infection when there is doubt about the presence or extent of an abscess.14 The test is performed by having the patient oppose the thumb and affected finger, thereby applying light pressure to the distal volar aspect of the affected digit. The increase in pressure within the nail fold (particularly in the abscess cavity) causes blanching of the overlying skin and clear demarcation of the abscess. In patients with severe infection or abscess, a specimen should be obtained to identify the responsible pathogen and to rule out methicillin-resistant S. aureus (MRSA) infection.13
DIFFERENTIAL DIAGNOSIS
Psoriasis and Reiter syndrome may also involve the proximal nail fold and can mimic acute paronychia.10 Recurrent acute paronychia should raise suspicion for herpetic whitlow, which typically occurs in health care professionals as a result of topical inoculation.12 This condition may also affect apparently healthy children after a primary oral herpes infection. Herpetic whitlow appears as single or grouped blisters with a honeycomb appearance close to the nail.8 Diagnosis can be confirmed by Tzanck testing or viral culture. Incision and drainage is contraindicated in patients with herpetic whitlow. Suppressive therapy with a seven-to 10-day course of acyclovir 5% ointment or cream (Zovirax) or an oral antiviral agent such as acyclovir, famciclovir (Famvir), or valacyclovir (Valtrex) has been proposed, but evidence from clinical trials is lacking.15
MEDICAL TREATMENT
Treatment of acute paronychia is determined by the degree of inflammation.12 If an abscess has not formed, the use of warm water compresses and soaking the affected digit in Burow's solution (i.e., aluminum acetate)10 or vinegar may be effective.5,11 Acetaminophen or a nonsteroidal anti-inflammatory drug should be considered for symptomatic relief. Mild cases may be treated with an antibiotic cream (e.g., mupirocin [Bactroban], gentamicin, bacitracin/neomycin/polymyxin B [Neosporin]) alone or in combination with a topical corticosteroid. The combination of topical antibiotic and corticosteroid such as betamethasone (Diprolene) is safe and effective for treatment of uncomplicated acute bacterial paronychia and seems to offer advantages compared with topical antibiotics alone.7
For persistent lesions, oral antistaphylococcal antibiotic therapy should be used in conjunction with warm soaks.11,16,17 Patients with exposure to oral flora via finger sucking or hangnail biting should be treated against anaerobes with a broad-spectrum oral antibiotic (e.g., amoxicillin/clavulanate [Augmentin], clindamycin [Cleocin]) because of possible S. aureus and Bacteroides resistance to penicillin and ampicillin.3,11,17,18 Medications commonly used in the treatment of acute paronychia are listed in Table 1.3,10–13,17–22
| Drug | Typical dosage | Comments | ||
|---|---|---|---|---|
| Antibiotics (oral) | ||||
| Amoxicillin/clavulanate (Augmentin)* | 500 mg/125 mg orally three times daily for seven days | Dosage adjustment may be necessary in patients with renal impairment; cross-sensitivity documented with cephalosporins; diarrhea may occur | ||
| or | ||||
| 875 mg/125 mg orally twice daily for seven days | ||||
| Clindamycin (Cleocin)* | 150 to 450 mg orally three or four times daily (not to exceed 1.8 g daily) for seven days | Adjust dosage in patients with severe hepatic dysfunction; associated with severe and possibly fatal colitis; inform patient to report severe diarrhea immediately | ||
| Trimethoprim/sulfamethoxazole (TMP/SMX; Bactrim, Septra)* | 160 mg/800 mg orally twice daily for seven days | High doses may cause bone marrow depression; discontinue therapy if significant hematologic changes occur; caution in folate or glucose-6-phosphate dehydrogenase deficiency | ||
| Antibiotics (topical) | ||||
| Bacitracin/neomycin/polymyxin B ointment (Neosporin) | Three times daily for five to 10 days | Overgrowth of nonsusceptible organisms with prolonged use | ||
| Gentamicin ointment | Three or four times daily for five to 10 days | — | ||
| Mupirocin ointment (Bactroban) | Two to four times daily for five to 10 days | Avoid contact with eyes; may irritate mucous membranes; resistance may result with prolonged use | ||
| Antifungal agents (oral) | ||||
| Fluconazole (Diflucan) | 100 mg orally once daily for seven to 14 days | Hepatotoxicity and QT prolongation may occur | ||
| Itraconazole (Sporanox) | 200 mg orally twice daily for seven days | Antacids may reduce absorption; edema may occur with coadministration of calcium channel blockers; rhabdomyolysis may occur with coadministration of statins; inhibition of cytochrome P450 hepatic enzymes may cause increased levels of many drugs | ||
| Nystatin (Mycostatin) 200,000-unit pastilles | One or two pastilles four times daily for seven to 14 days | Adverse effects include nausea, vomiting, and diarrhea | ||
| Antifungal agents (topical) | ||||
| Ciclopirox topical suspension (Loprox TS) | Twice daily until clinical resolution (one month maximum) | Avoid contact with eyes and mucous membranes | ||
| Clotrimazole cream (Lotrimin) | Three times daily until clinical resolution (one month maximum) | Avoid contact with eyes; if irritation or sensitivity develops, discontinue use and begin appropriate therapy | ||
| Econazole cream (Spectazole) | Three or four times daily until clinical resolution (one month maximum) | Avoid contact with eyes; if irritation or sensitivity develops, discontinue use and begin appropriate therapy | ||
| Ketoconazole cream (Nizoral; brand no longer available in the United States) | Once or twice daily until clinical resolution (one month maximum) | Avoid contact with eyes; if irritation or sensitivity develops, discontinue use and begin appropriate therapy | ||
| Nystatin cream | Three times daily until clinical resolution (one month maximum) | Avoid contact with eyes; if irritation or sensitivity develops, discontinue use and begin appropriate therapy | ||
| Antiviral agents for herpetic whitlow | ||||
| Acyclovir (Zovirax) † | 200 mg orally five times daily for 10 days | Nausea, vomiting, rash, deposition in renal tubules, and central nervous system symptoms may occur | ||
| Famciclovir (Famvir)† | 250 mg orally twice daily for 10 days | Dosage adjustment recommended in patients with renal impairment | ||
| Valacyclovir (Valtrex)† | 500 mg orally twice daily for 10 days | Associated with onset of hemolytic uremic syndrome | ||
| Corticosteroids (topical) | ||||
| Betamethasone 0.05% cream (Diprolene) | Twice daily for one to two weeks | If infection develops and is not responsive to antibiotic treatment, discontinue use until infection is controlled | ||
| Betamethasone valerate 0.1% solution or lotion (Beta-Val) | Once or twice daily for one to two weeks | Prolonged therapy over large body surface areas may suppress adrenal function; if infection develops, discontinue use until infection is controlled | ||
| Combination antifungal agent and corticosteroid | ||||
| Nystatin and triamcinolone cream (Mytrex; brand no longer available in the United States) | Two or three times daily until the cuticle has regrown | Check precautions for both components | ||
SURGICAL TREATMENT
Although surgical intervention for paronychia is generally recommended when an abscess is present, no studies have compared the use of oral antibiotics with incision and drainage.23 Superficial infections can be easily drained with a size 11 scalpel or a comedone extractor.12 Pain is quickly relieved after drainage.17 Another simple technique to drain a paronychial abscess involves lifting the nail fold with the tip of a 21- or 23-gauge needle, followed immediately by passive oozing of pus from the nail bed; this technique does not require anesthesia or daily dressing.24 If there is no clear response within two days, deep surgical incision under local anesthesia (digital nerve block) may be needed, particularly in children.8,10,11 The proximal one third of the nail plate can be removed without initial incisional drainage. This technique gives more rapid relief and more sustained drainage, especially in patients with paronychia resulting from an ingrown nail.8,17,19 Complicated infections can occur in immunosuppressed patients and in patients with diabetes or untreated infections.11,16 Preventive measures for acute paronychia are described in Table 2.3,10,13,19,20
| Paronychia type | Recommendation |
|---|---|
| All | Avoid trimming cuticles or using cuticle removers |
| Improve glycemic control in patients with diabetes | |
| Provide adequate patient education | |
| Acute | Avoid nail trauma, biting, picking, and manipulation, and finger sucking |
| Keep affected areas clean and dry | |
| Chronic | Apply moisturizing lotion after hand washing |
| Avoid chronic prolonged exposure to contact irritants and moisture (including detergent and soap) | |
| Avoid finger sucking | |
| Keep nails short | |
| Use rubber gloves, preferably with inner cotton glove or cotton liners |
Chronic Paronychia
ETIOLOGY AND PREDISPOSING FACTORS
Chronic paronychia is a multifactorial inflammatory reaction of the proximal nail fold to irritants and allergens.12,19–21 This disorder can be the result of numerous conditions, such as dish washing, finger sucking, aggressively trimming the cuticles, and frequent contact with chemicals (e.g., mild alkalis, acids).
In chronic paronychia, the cuticle separates from the nail plate, leaving the region between the proximal nail fold and the nail plate vulnerable to infection by bacterial and fungal pathogens.12,21 Chronic paronychia has been reported in laundry workers, house and office cleaners, food handlers, cooks, dishwashers, bartenders, chefs, fishmongers, confectioners, nurses, and swimmers. In such cases, colonization with Candida albicans or bacteria may occur in the lesion.19,21
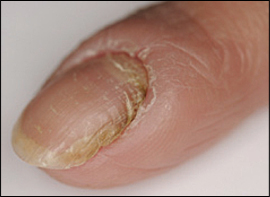
There is some disagreement about the importance and role of Candida in chronic paronychia.10,21 Although Candida is often isolated in patients with chronic paronychia, this condition is not a type of onychomycosis, but rather a variety of hand dermatitis21 caused by environmental exposure (Figure 3). In many cases, Candida disappears when the physiologic barrier is restored.12
Chronic paronychia can result as a complication of acute paronychia20 in patients who do not receive appropriate treatment.7 Chronic paronychia often occurs in persons with diabetes.3 The use of systemic drugs, such as retinoids and protease inhibitors (e.g., indinavir [Crixivan], lamivudine [Epivir]), may cause chronic paronychia. Indinavir is the most common cause of chronic or recurrent paronychia of the toes or fingers in persons infected with human immunodeficiency virus. The mechanism of indinavir-induced retinoid-like effects is unclear.25,26 Paronychia has also been reported in patients taking cetuximab (Erbitux), an anti-epidermal growth factor receptor (EGFR) antibody used in the treatment of solid tumors.27,28
DIAGNOSIS
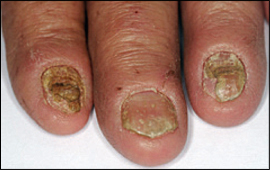
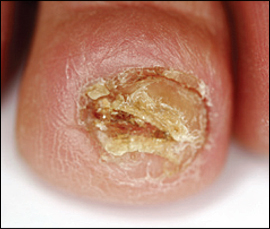
Diagnosis of chronic paronychia is based on physical examination of the nail folds and a history of continuous immersion of hands in water10; contact with soap, detergents, or other chemicals; or systemic drug use (retinoids, antiretroviral agents, anti-EGFR antibodies). Clinical manifestations are similar to those of acute paronychia: erythema, tenderness, and swelling, with retraction of the proximal nail fold and absence of the adjacent cuticle. Pus may form below the nail fold.8 One or several fingernails are usually affected, typically the thumb and second or third fingers of the dominant hand.13 The nail plate becomes thickened and discolored, with pronounced transverse ridges such as Beau's lines (resulting from inflammation of the nail matrix), and nail loss8,10,13 (Figure 4). Chronic paronychia generally has been present for at least six weeks at the time of diagnosis.10,12 The condition usually has a prolonged course with recurrent, self-limited episodes of acute exacerbation.13
DIFFERENTIAL DIAGNOSIS
Other entities affecting the fingertip, such as squamous cell carcinoma of the nail29,30 (Figure 5), malignant melanoma, and metastases from malignant tumors,31 may mimic paronychia. Physicians should consider the possibility of carcinoma when a chronic inflammatory process is unresponsive to treatment.30 Any suspicion for the aforementioned entities should prompt biopsy. Several diseases affecting the digits, such as eczema, psoriasis, and Reiter syndrome, may involve the nail folds.10
TREATMENT
Treatment of chronic paronychia includes avoiding exposure to contact irritants and appropriate management of underlying inflammation or infection.12,20 A broad-spectrum topical antifungal agent can be used to treat the condition and prevent recurrence.22 Application of emollient lotions to lubricate the nascent cuticle and the hands is usually beneficial. One randomized controlled trial assigned 45 adults with chronic paronychia to treatment with a systemic antifungal agent (itraconazole [Sporanox] or terbinafine [Lamisil]) or a topical steroid cream (methylprednisolone aceponate [Advantan, not available in the United States]) for three weeks.21 After nine weeks, more patients in the topical steroid group were improved or cured (91 versus 49 percent; P < .01; number needed to treat = 2.4).
The presence or absence of Candida seems to be unrelated to the effectiveness of treatment. Given their lower risks and costs compared with systemic antifungals, topical steroids should be the first-line treatment for patients with chronic paronychia.21 Alternatively, topical treatment with a combination of steroid and antifungal agents may also be used in patients with simple chronic paronychia, although data showing the superiority of this treatment to steroid use alone are lacking.19 Intralesional corticosteroid administration (triamcinolone [Amcort]) may be used in refractory cases.8,19 Systemic corticosteroids may be used for treatment of inflammation and pain for a limited period in patients with severe paronychia involving several fingernails.
In patients with recalcitrant chronic paronychia, en bloc excision of the proximal nail fold is effective. Simultaneous avulsion of the nail plate (total or partial, restricted to the base of the nail plate) improves surgical outcomes.8,32 Alternatively, an eponychial marsupialization, with or without nail removal, may be performed.33 This technique involves excision of a semicircular skin section proximal to the nail fold and parallel to the eponychium, expanding to the edge of the nail fold on both sides.33 Paronychia induced by the EGFR inhibitor cetuximab can be treated with an antibiotic such as doxycycline (Vibramycin).28 In patients with paronychia induced by indinavir, substitution of an alternative antiretroviral regimen that retains lamivudine and other protease inhibitors can resolve retinoid-like manifestations without recurrences.25
PROGNOSIS
Chronic paronychia responds slowly to treatment. Resolution usually takes several weeks or months, but the slow improvement rate should not discourage physicians and patients. In mild to moderate cases, nine weeks of drug treatment usually is effective. In recalcitrant cases, en bloc excision of the proximal nail fold with nail avulsion may result in significant cure rates. Successful treatment outcomes also depend on preventive measures taken by the patient (e.g., having a water barrier in the nail fold). If the patient is not treated, sporadic, self-limiting, painful episodes of acute inflammation should be expected as the result of continuous penetration of various pathogens.