
Am Fam Physician. 2008;77(11):1584-1587
Author disclosure: Nothing to disclose.
A 54-year-old woman presented to the emergency department with altered mental status. She complained of headache with sinus pain and reported undergoing dental extractions 10 days earlier. Her white blood cell count was 26,800 cells per mm3 (26.8 × 109 per L), her serum glucose level was 588 mg per dL (32.65 mmol per L), and her pH level on arterial blood gas analysis was 7.21. Computed tomography of her head showed right nasopharyngeal fullness and possible right maxillary sinusitis; no other abnormalities were noted. The patient was admitted to the intensive care unit for treatment of diabetic ketoacidosis, and she received antibiotics.
The patient's mental status did not return to baseline, and her condition rapidly deteriorated despite correction of the metabolic abnormalities. Within 12 hours, she developed epistaxis and proptosis of the right eye. She also developed diplopia, which quickly progressed to vision loss, and dramatic right hemipalatal necrosis (see accompanying figure). The patient was emergently transferred for specialty care but died shortly after arriving at the facility.
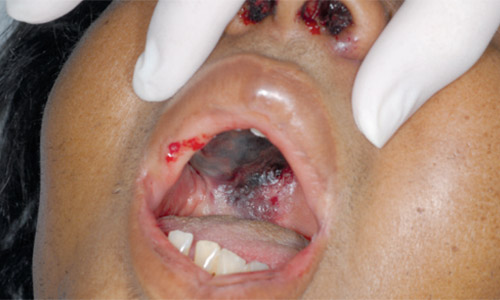
Question
Discussion
The answer is E: rhinocerebral mucormycosis. Mucormycosis can affect the upper respiratory, pulmonary, cutaneous, gastrointestinal, and central nervous systems. The clinical manifestation of the condition is headache with nasal discharge and sinus pain. Infection quickly spreads from the sinuses to contiguous structures. Ocular involvement manifests as proptosis, periorbital edema, ophthalmoplegia, or vision loss. Angioinvasion by hyphae leads to a black necrotic eschar on the palate or nasal mucosa. Infection spreading from the ethmoid sinus to the frontal lobe can cause obtundation.
Rhizopus species are the pathogens predominantly associated with rhinocerebral mucormycosis and are found in fruit, soil, dust, and manure. Rhizopus can be identified in nasal mucosa cultures of asymptomatic patients.1 In healthy persons, nasal cilia transport the fungi spores to the pharynx, and the spores are then cleared through the gastrointestinal tract.
Mucormycosis in immunocompromised patients typically occurs with spore inhalation or through skin lacerations. Hyperglycemia, usually with related metabolic acidosis, is the most common underlying condition associated with mucormycosis.2 Hematologic malignancy, neutropenia, high-dose corticosteroid therapy, organ transplantation, renal failure, and deferoxamine (Desferal) therapy may also precipitate mucormycosis.1,3 Dental extraction can create a portal of entry into the maxillofacial region, and case reports suggest a potential for fungal infection in immunocompromised patients.1
Rhinocerebral mucormycosis is rapidly fatal and should be suspected in high-risk patients presenting with sinusitis, particularly those with diabetes and metabolic acidosis. Altered mental status that persists after metabolic abnormalities are corrected suggests possible central nervous system (CNS) infection. Diagnosis is based on histopathology with culture confirmation. Early computed tomography (CT) with or without magnetic resonance imaging (MRI) is generally nonspecific.1,3,4
Treatment requires prompt and aggressive surgical debridement and antifungal therapy with amphotericin B (Fungizone; brand no longer available in the United States).2 However, despite early diagnosis and aggressive treatment with combined surgical and medical therapy, the prognosis is generally poor.
Bacterial orbital cellulitis can manifest as proptosis, globe displacement, limitation of eye movements, and diplopia or vision loss. Predisposing conditions include sinusitis; orbital trauma; and an infection of the teeth, middle ear, or face. Streptococci, Staphylococcus aureus, and non–spore-forming anaerobes are the pathogens most commonly associated with the condition.
Patients with cavernous sinus thrombosis usually seek medical attention for headache. The sharp, increasingly severe headache interferes with sleep and is not relieved with pain medications. Eye swelling begins unilaterally and then spreads to the other eye. Signs involving cranial nerves III through VI, diplopia, altered mental status, and coma may occur. Septic cavernous sinus thrombosis is easily differentiated from orbital cellulitis with high-resolution CT or MRI. The peripheral white blood cell count is typically elevated in patients with septic cavernous sinus thrombosis, suggesting a bacterial infection. S. aureus accounts for most infections, although Streptococci and anaerobes are occasionally identified.
CNS aspergillosis can manifest identically to mucormycosis in the sinuses. As with mucormycosis, the organism is ubiquitous and invasive disease is rare in healthy persons. However, infection can occur in immunocompromised persons, which may lead to rapid progression across tissue planes. Rhinocerebral aspergillosis is more common in patients with neutropenia than in those with diabetes. Symptoms may begin with nasal congestion, fever, and facial pain and then progress to blurred vision, proptosis, and conjunctival edema (chemosis) as the infection spreads to the orbits. Vascular invasion with subsequent infarction and tissue necrosis is a hallmark of the disease. Hyphae of aspergillosis are narrow and septated with acute-angle branching, which is distinctly different from the broad, nonseptated, right-angle branching hyphae of mucormycosis.
Ecthyma gangrenosum is a skin manifestation of underlying sepsis, typically from Pseudomonas aeruginosa. The condition, which involves the skin or mucous membrane, usually begins as a small area of edema and rapidly evolves into a painless, nodular lesion or multiple lesions. The lesions then form into a central hemorrhage, ulcerate, and necrose because of vascular bacterial invasion. If multiple lesions are present, they may be in different stages of development. Infection can quickly progress to localized bacterial invasion and damage to underlying tissues and contiguous structures.
| Condition | Characteristics |
|---|---|
| Bacterial orbital cellulitis | Proptosis, extraocular muscle impairment, diplopia, vision loss |
| Cavernous sinus thrombosis | Headache, loss of vision or visual acuity, ophthalmoplegia |
| CNS aspergillosis | More common in patients with neutropenia; blurred vision, proptosis, chemosis; vascular invasion with subsequent infarction and tissue necrosis is a hallmark |
| Ecthyma gangrenosum | Occurs as a result of sepsis from perivascular bacterial invasion; painless, nodular lesions affecting the skin or mucous membranes form into a central hemorrhage, ulcerate, and necrose |
| Rhinocerebral mucormycosis | More common in patients with hyperglycemia and associated metabolic acidosis; sinus involvement with spread to the CNS; ocular involvement (proptosis, periorbital edema, ophthalmoplegia, or vision loss); nasal and palatal necrosis |