A 27-year-old woman presented with pruritic papules in the right axilla that had persisted for five months. The lesions arose suddenly, and she denied a personal or family history of similar lesions. She had no history of skin disease. The patient's only medication was an oral contraceptive. She had not changed brands of deodorant or soaps recently.
On physical examination, the right axillary vault contained confluent, flesh-colored, firm, perifollicular papules, 2 mm in size (Figures 1 and 2). Some of the lesions were umbilicated with atrophic hairs. The skin in the surrounding area and on the left axilla, areolae, inframammary folds, and groin was normal. Her lipid panel was unremarkable.
Figure 1.
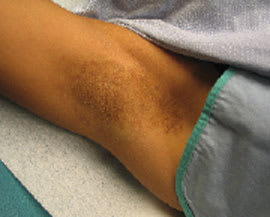
Figure 2.
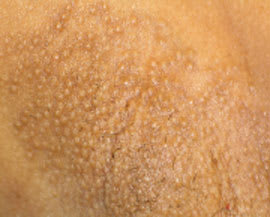
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Folliculitis.
B. Fox-Fordyce disease.
C. Lichen nitidus.
D. Miliaria rubra.
E. Syringomas.
Discussion
The answer is B: Fox-Fordyce disease. Fox-Fordyce disease (apocrine miliaria) is an uncommon chronic condition with characteristic clinical findings. Patients present with multiple small, firm, smooth, dome-shaped perifollicular papules in areas of apocrine sweat gland concentration. The papules are flesh-colored or have a slightly yellowish hue and occur, in decreasing order of frequency, in the axillae, groin, areolae, and inframammary folds.1
The condition predominantly affects post-pubescent women in their midteens through mid-30s. Rapid onset after exposure to hot conditions or after sweating is common. The chief complaint generally is intermittent, moderate-to-severe pruritus in the affected areas. The pathogenesis of Fox-Fordyce disease is poorly defined; however, the presence of a keratin plug in the follicular infundibulum, with apocrine duct rupture and spongiotic inflammation on histologic analysis, is characteristic.2
There are no reported cases of spontaneous resolution, and there is no known cure for Fox-Fordyce disease. Many treatment strategies have had poor success and include oral contraceptives; oral tretinoin; topical retinoids, antibiotics, and steroids; intralesional triamcinolone (Kenalog-10); ultraviolet light; and dermabra-sion.3 Irritation from topical retinoids generally limits long-term therapy. Successful treatment with clindamycin (Cleocin) in alcoholic propylene glycol solution has been reported.1,3 Surgical excision has been suggested for the treatment of recalcitrant cases.4 Because severe pruritus is often present and because of the nature and limitations of potential treatment modalities, dermatology consultation should be considered.
Folliculitis is characterized by tender perifollicular pustules with surrounding erythema. Lesions are caused by infection, mechanical trauma, or chemical irritation and may occur anywhere on the body surface.
Lichen nitidus appears as multiple and discrete pinpoint, pink or flesh-colored, flat-topped, round papules with a characteristic glistening appearance. These asymptomatic lesions typically occur on the genitalia, abdomen, or extremities.5
Miliaria rubra, also known as prickly heat or heat rash, occurs in susceptible persons as a result of eccrine sweat duct occlusion. Small, diffuse papules and vesicles with surrounding confluent erythema appear suddenly in occluded areas during sweating, such as with physical exertion. There is no follicular association, and patients may describe a “prickly” sensation.6
Syringomas are benign, flesh-colored or white-yellow, flat-topped papules that typically occur on the lower eyelids or vulva. The lesions are asymptomatic, arise gradually, and slowly increase in number.7
Summary Table
| Condition | Characteristics |
|---|---|
| Folliculitis | Tender perifollicular pustules with surrounding erythema |
| Fox-Fordyce disease | Firm, dome-shaped, perifollicular, skin-colored or yellowish, pruritic papules |
| Lichen nitidus | Multiple and discrete pinpoint, pink or flesh-colored, flat-topped, asymptomatic papules with a glistening appearance |
| Miliaria rubra | Small, diffuse papules and vesicles with surrounding confluent erythema |
| Syringomas | Asymptomatic, yellowish, flat-topped papules; typically occur on the lower eyelids or vulva |

