A 62-year-old man presented with intense pruritus that had persisted for two months. The pruritus began on his hands and feet, and was followed by the appearance of lesions on his hands, feet, nose, and ears. He also had abdominal pain, malaise, fatigue, anorexia, and weight loss. He smoked about 40 cigarettes per day for 40 years and had a history of alcoholic cirrhosis.
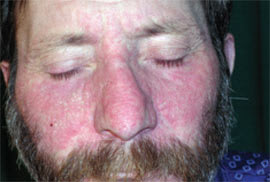
Physical examination revealed cachexia. Well-defined hyperkeratotic plaques were symmetrically distributed at pressure points on the palms and soles (Figure 1). His hands and feet also had thickened skin, longitudinal streaking, and severe subungual hyperkeratosis; the dorsal feet had severe dryness with scaling. Winered–colored, slightly scaly, erythematous plaques were noted on the dorsum of the nose and on the helices of the ears (Figure 2).
Figure 1.
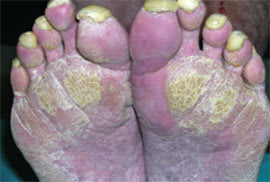
Figure 2.
A lesional biopsy was obtained from the medial plantar surface; histology showed orthokeratotic hyperkeratosis, mild acanthosis, irregular enlargement of the rete ridges, and superficial perivascular inflammatory infiltration. A periodic acid-Schiff stain was normal.
Laboratory tests showed the following: hypoalbuminemia (albumin level of 1.8 g per dL [18 g per L]); increased levels of aspartate transaminase (361 U per L), alanine transaminase (128 U per L), γ-glutamyltransferase (280 U per L [4.67 μkat per L]), and alkaline phosphatase (103 U per L [1.72 μkat per L]); mild hyperbilirubinemia (bilirubin level of 1.4 mg per dL [24 μmol per L]); α-fetoprotein level of 80 ng per mL (80 μg per L); and positive findings for hepatitis B surface antigen, hepatitis B e antigen, and anti-hepatitis B core immunoglobulin G.
Abdominal ultrasonography showed a hyperechoic, nonhomogeneous mass with irregular margins in the third hepatic segment; a hypoechoic capsule; multiple calcifications; and necrotic nonechoic areas.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Chronic eczema.
B. Paraneoplastic acrokeratosis.
C. Psoriasis.
D. Reactive arthritis (Reiter syndrome).
E. Superficial fungal infection.
Discussion
The answer is B: paraneoplastic acrokeratosis. Paraneoplastic acrokeratosis (Bazex syndrome) is a cutaneous marker of underlying malignancy. The first reported case was in a patient who had pyriform sinus cancer with cervical metastases; the cutaneous lesions resolved after the tumor was treated.1 Paraneoplastic acrokeratosis is a rare syndrome of unknown pathogenesis. It is more common in men and usually occurs around 60 years of age.
The syndrome includes three stages, with cutaneous findings often occurring several months before symptoms of the underlying malignancy are noted. The initial phase is characterized by red-violaceous, scaly, psoriasiform plaques with undefined margins and typical bilateral acral distribution on the hands, feet, nose, and earlobes; the elbows and knees are affected less often. During the initial stage, there are no symptoms of the underlying malignancy. The second stage involves local spread of the rash and symptoms of the malignancy. The third stage may occur if the malignancy is untreated and involves central spread of the rash.2 In 90 to 95 percent of cases, the skin lesions improve significantly or resolve after the malignancy is treated; however, they may not improve with persistent disease. The reappearance of skin lesions signals tumor recurrence.3
Paraneoplastic acrokeratosis is associated with squamous cell neoplasms of the upper respiratory and digestive tracts, including the pharynx, esophagus, tongue, and lungs. It has also been reported with adenocarcinoma of the stomach, prostate, colon, or lung; peripheral T-cell lymphoma; Hodgkin's disease; metastatic neuroendocrine tumor; bladder carcinoma; bronchial carcinoid tumor; and squamous cell carcinoma of the vulva.2,4 A thorough diagnostic work-up to detect the primary neoplasm should be performed in all patients with these cutaneous lesions. The initial work-up should focus on the upper respiratory and digestive tracts, although the neoplasm may be found in other areas. Treatment focuses on the underlying malignancy and includes surgery, chemotherapy, or radiotherapy.
Chronic eczema may also cause thick hyperkeratotic lesions on the palms and soles but is associated with a more longstanding history. Blisters or vesiculation supports an eczema diagnosis.3,4
Acral psoriasis can be distinguished clinically from paraneoplastic acrokeratosis because it does not affect the helices of the ears and the tip of the nose. Histologically, paraneoplastic acrokeratosis leads to psoriasiform changes (e.g., hyperkeratosis, parakeratosis, superficial lymphohistiocytic infiltration) and nonpsoriasiform changes (e.g., vacuolar degeneration, dyskeratotic keratinocytes).3,5
Reactive arthritis is a systemic condition that usually includes hyperkeratotic plaques on the palms and soles. It is characterized by arthritis, urethritis, and conjunctivitis; mucocutaneous lesions may occur.6
Trichophyton rubrum infection can affect the hands (tinea manuum) and feet (tinea pedis). This cutaneous infection is characterized by dryness and scaling. The lesions begin in toe webs and spread to the toenails, soles, undersurface of toes and, rarely, the dorsal feet. The lesions are usually asymmetric, with one foot more heavily involved. Although tinea pedis usually affects both feet, tinea manuum rarely spreads from one hand to the other.6
Selected Differential Diagnosis of Palmoplantar Hyperkeratosis
| Condition | Characteristics |
|---|---|
| Chronic eczema | Thick, hyperkeratotic lesions may appear on the palms and soles; blisters or vesiculation supports the diagnosis |
| Paraneoplastic acrokeratosis | Red-violaceous, scaly, psoriasiform plaques with undefined margins; bilateral, acral distribution, mainly on the hands, feet, nose, and earlobes |
| Psoriasis | Common erythematosquamous disorder with a number of morphologic subtypes, including acral variants |
| Reactive arthritis(Reiter syndrome) | Systemic condition that usually includes hyperkeratotic skin plaques on the palms and soles; characterized by arthritis, urethritis, and conjunctivitis; mucocutaneous lesions may occur |
| Superficial fungal infection | Dry, scaly, pruritic patches on the feet; the infection typically begins in the toe webs; potassium hydroxide preparations may show fungal elements |

