Atypical moles can be distinguished visually by clinical features of size greater than 6 mm in diameter, color variegation, indistinct borders, and textured surface. All patients who have atypical moles should be counselled about sun avoidance, screening of family members, and regular skin checks at least once per year. Total body photography and dermoscopy can aid in regular skin monitoring for changes in atypical moles and the emergence of new lesions. The presence of multiple atypical moles increases the risk of melanoma. The greatest risk of melanoma is in patients who have more than 50 atypical moles and two or more family members with melanoma (familial atypical mole and melanoma syndrome). Atypical moles should be removed when they have features suggestive of malignant transformation. Elliptical excision is the preferred removal technique. Removing all atypical moles is neither necessary nor cost effective.
Atypical moles were first described in 1978 as distinctive pigmented skin lesions present in 37 of 58 members of six families with melanoma.1 The term B-K mole syndrome was coined from the initials of two of the family surnames. Clinically, one person can have one to more than 100 of these moles that occur mainly on the upper trunk and extremities. Each lesion is typically larger than 6 mm in diameter, but the lesions vary in shape and color. Histologically, atypical moles show atypical melanocytic hyperplasia, fibroplasia, vascular proliferation, and lymphocytic infiltration.2
Several names have been used to describe atypical moles, including dysplastic nevus, atypical nevus (and syndromes), familial atypical multiple mole and melanoma (FAM-M) syndrome, and Clark nevus.3 In 1992, the National Institutes of Health recommended using “atypical mole” instead of dysplastic nevus, and “FAM-M syndrome” to describe melanoma-prone families.4
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| It is not cost-effective to remove all atypical moles. | C | 26 |
| Excisional biopsy is the preferred biopsy method for atypical moles. | C | 27, 28, 31 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Epidemiology
An estimated 5 to 10 percent of the population has atypical moles,5 with a higher incidence in immunosuppressed adults.6 Because atypical moles are markers for melanoma and are possible precursor lesions, careful clinical attention is warranted. Melanoma is a common neoplasm and is the deadliest form of skin cancer. The American Cancer Society projected that there would be 62,480 new cases of melanoma and 8,420 attributable deaths in 2008.7 The incidence of melanoma is increasing by 4.1 percent per year, faster than any other malignancy.8
A single atypical mole does not increase the lifetime risk of melanoma; however, when multiple atypical moles are present, the relative risk of melanoma is increased. The greatest risk is in patients who have multiple atypical moles (more than 50 lesions) plus two or more family members with melanoma. This has been termed the FAM-M syndrome. In patients with FAM-M syndrome, the cumulative lifetime risk of melanoma approaches 100 percent.9
Clinical Features
Physicians must be able to distinguish normal moles (Figure 1) from atypical moles (Figures 2 through 5), and to recognize overt melanoma (Figure 6). Atypical moles may have some of the same features as melanoma; therefore, a precise diagnosis can be difficult to determine. Atypical moles are usually greater than 6 mm in diameter and have color variegation, indistinct borders, and a textured surface (Table 1).10–14 They may also have a raised central papule and a surrounding macular component (“fried-egg” appearance).
Figure 1.
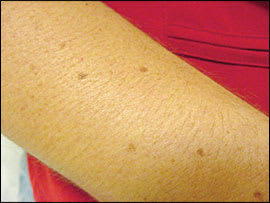
Normal moles on the forearm of a 45-year-old woman.
Figure 2.
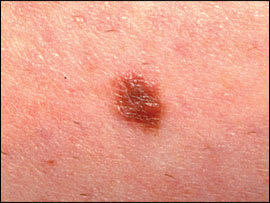
Atypical mole with a raised portion, irregular border, and two to three shades of brown.
Figure 3.
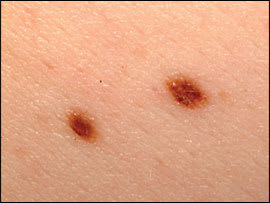
Two atypical moles; mole on right has two to three shades of brown.
Figure 4.
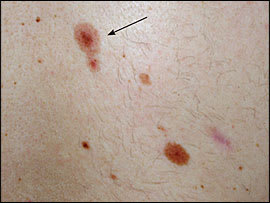
Atypical mole (arrow) that has an outer ring of lighter pigment and an irregular border.
Figure 5.
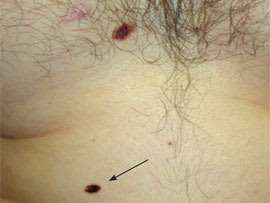
Atypical mole (arrow) on abdomen; biopsy showed moderate cytologic atypia.
Figure 6.
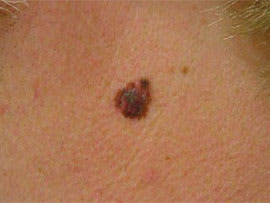
Melanoma on the neck of a 43-year-old man; primary depth of invasion was 2 mm (Clark level IV).
Table 1 Clinical Features of Normal Moles, Atypical Moles, and Melanoma
| Mole or melanoma | Clinical features | ||||||
|---|---|---|---|---|---|---|---|
| Age at onset | Location | Number | Size | Color distribution | Shape | Border | |
| Normal moles | After six to 12 months of age, usually by 20 years of age |
| Few to 100s | Most < 6 mm in diameter |
| Round, oval | Smooth, regular, well-demarcated |
| Atypical moles | After six to 12 months of age, usually by 20 years of age |
| One to 100s | No lower size limit |
| Round, oval, asymmetric | Irregular and/or poorly demarcated, fuzzy |
| Usually > 6 mm in diameter | |||||||
| Melanoma | Adulthood |
| One | No lower size limit to > 6 mm in diameter |
| Asymmetric | Irregular |
| It can occur in children with giant congenital moles, atypical mole syndrome, or xeroderma pigmentosum | |||||||
Potential for Malignant Transformation
Several studies have examined the relationship between atypical moles and melanoma. Precursor lesions with melanocytic atypia and architectural disorder have been reported in 5 to 39 percent of melanoma specimens.15 A prospective study based on episodic complete skin examinations of 153 patients with atypical moles over five years reported that 50 percent of lesions showed no change over time; 15 percent developed greater clinical atypia during follow-up; and in 35 percent of lesions, atypia decreased or the lesion disappeared altogether. In this study, 11 patients developed melanoma; two had in situ lesions and seven had melanoma associated with existing atypical moles.16 Nodular melanomas have less association with atypical moles, with only 3 percent of these specimens showing atypical features.10
A patient who has atypical moles has an increased risk of melanoma even in the absence of a personal or family history of melanoma. In a case-control study of 287 white patients with atypical mole syndrome followed for an average of 88 months, 10 patients (3.5 percent) developed melanoma. In contrast, of the 831 control patients without atypical mole syndrome, only two (0.2 percent) developed melanoma. The 10-year cumulative risk of developing melanoma in patients with atypical mole syndrome is 10.7 percent compared with 0.62 percent in patients without atypical mole syndrome.9 A systematic meta-analysis of observational studies of melanoma development determined that patients with five atypical moles had a six times higher risk of developing melanoma than patients without atypical moles.17
Management
DIAGNOSIS AND SCREENING
Prevention and early detection of atypical moles should be discussed with all patients. Sun avoidance and skin protection should be reviewed, especially the importance of avoiding sunburns in childhood. For patients who have atypical moles, a reasonable practice is to examine the skin at least every 12 months. However, no outcome studies or consensus guidelines have established the optimal frequency of skin examination. Using a blow dryer on the scalp helps facilitate visualization of pigmented lesions. In patients with atypical moles, the physician should suggest that family members also be screened.5 Patient self-examination of the skin should be encouraged. Table 2 lists recommendations for the management of atypical moles.3,5
Table 2 Management of Atypical Moles
| Sun avoidance and protection, especially sunburns in childhood |
| Regular physician follow-up at least every 12 months |
| Screen family members |
| Use diagnostic aids, such as total body photography and dermoscopy |
| Biopsy of suspicious lesions |
| Instruct patients in self-examination |
Diagnostic aids to detect and monitor atypical moles include total body photography and dermoscopy. Total body photographs (which may be reimbursed by insurance) are useful for identifying moles that are changing significantly or detecting new moles that should be removed. These photos may be given to the patient to assist in monitoring by self-examination of the skin. Dermoscopy, also called dermatoscopy or epiluminescent microscopy, can be used to monitor moles. Benign lesions, such as hemangiomas and seborrheic keratosis, are easily ruled out using dermoscopy. The use of dermoscopy by untrained and inexperienced physicians is highly controversial. Dermoscopy has been shown to improve the early detection of melanoma18 and to increase the sensitivity for melanoma diagnosis by primary care physicians.19 One study has shown that physicians inexperienced with dermoscopy who do self-guided compact disc training in dermoscopy performed as well as experts.20 Other studies report that experience and training are needed for proper use.21,22 The cost of a standard handheld dermatoscope (Figure 7) is around $500. Digital dermatoscopes linked to computer hardware and software systems can cost thousands of dollars. A free dermoscopy tutorial can be found at http://www.dermoscopy.org/atlas/base.htm.
Figure 7.

Standard handheld dermatoscope. To use, first put oil on the skin, which eliminates surface reflection. Then place the magnifying lens (10×) on the skin, which allows the physician to see the pigment beneath the skin surface.
The dermoscopic features of atypical moles are based on patterns (reticular, globular, or homogeneous) and pigment distribution (hypo-or hyperpigmentation in central, eccentric peripheral, or multifocal areas). In patients with multiple atypical moles, one type is usually predominant. Any atypical mole that does not belong to the predominant type in an individual patient should be given special attention.23
BIOPSY
The primary purpose of biopsy in atypical moles is to rule out melanoma. With nearly 80 percent of melanomas arising de novo (on skin without a mole), only changing or new moles with clinical features that are worrisome for melanoma need to be biopsied. The physician must decide between incisional biopsy (using superficial shave, deep shave, or punch techniques) and excisional biopsy (Table 3).24 Incisional biopsy techniques are appropriate when the suspicion for melanoma is low, the lesion is large, or when complete excision is impractical.25 Several well-conducted studies demonstrate the futility of removing all atypical moles. In a prospective cohort study of 278 adults who each had five or more atypical moles, 20 new melanomas were detected in 16 patients during an average of 42 months' follow-up. Eleven of these lesions were discovered because of change in pigmented lesions compared with baseline photographs and the other nine lesions were discovered by the patients or their partners. Thirteen of the 20 melanomas arose from new lesions, and only three from existing atypical moles. The authors concluded that if all atypical moles in the patients were removed (almost 6,000 moles), only three melanomas would have been prevented. The cost/benefit ratio of removing all atypical moles is unsatisfactory.26
Table 3 Biopsy Methods for Atypical Moles
| Biopsy method | Description |
|---|---|
| Superficial shave | A flat, thin disk of tissue is removed, typically by scalpel; sample is limited to epidermis and upper dermis (< 1 mm in depth) |
| Deep shave | A thick disk of tissue is removed by a curved blade; sample extends to at least mid dermis (1 to 4 mm in depth) |
| Punch | A disk of tissue is removed by skin punch instrument (4 to 8 mm punch); sample is cylindrical |
| Excisional | Lesion is completely removed by elliptical incision (> 4 mm in depth, including fat on deep surgical margin), with a 2- to 5-mm border of surrounding normal skin |
Information from reference 24.
Excisional biopsy provides the pathologist with optimal tissue for histologic diagnosis, and deep shave biopsy provides adequate tissue for histologic assessment in about 88 percent of cases. Deep shave biopsy is quicker, less expensive, less scarring, and has fewer complications, but lesions may recur at a rate three times higher than with excision.27,28 Shaving a pigmented lesion may also result in disruption of the ability to determine the depth of the melanoma. Nevertheless, in a retrospective study of 145 persons with melanoma, 88 percent of initial shave and punch biopsies were accurate, with Breslow depth greater than or equal to the Breslow depth in subsequent excision. Superficial and deep shave biopsies were more accurate than punch biopsies for melanomas less than 1 mm in diameter, and excisional biopsy was the most accurate biopsy method.24 Excisional biopsy is the preferred method of obtaining diagnostic tissue.
If the decision has been made to completely remove an atypical mole, a 2-mm specimen margin is important to avoid the need for reexcision. Residual moles were more common in lesions removed by punch biopsy than those removed by shave biopsy or elliptical excision. In a study of the value of reexcision in 189 atypical moles, only 25 percent of the reexcised lesions contained residual mole cells, and only one of the 189 lesions contained melanoma.29
Because most melanomas arise on normal skin and because most atypical moles do not progress to melanoma, reexcision of most lesions is probably unnecessary unless lesions show moderate to severe architectural disorder or moderate to severe cytologic atypia.30 The National Institutes of Health recommends reexcision with margins of 2 to 5 mm when there is involvement of the margin.4 If severe cytologic atypia is present, a 5-mm margin is recommended. Physicians who biopsy and follow atypical moles should send the specimens to a dermatopathologist with experience in the interpretation of complex pigmented lesions.31 The risk of false-positive pathologic diagnosis of melanoma is increased in a recurrent mole in the scar of a previously biopsied lesion.31
Referral
Referral to a dermatologist should be considered in patients with multiple atypical moles, depending on the physician's comfort level with monitoring and biopsying these lesions.

