Fatigue, a common presenting symptom in primary care, negatively impacts work performance, family life, and social relationships. The differential diagnosis of fatigue includes lifestyle issues, physical conditions, mental disorders, and treatment side effects. Fatigue can be classified as secondary to other medical conditions, physiologic, or chronic. The history and physical examination should focus on identifying common secondary causes (e.g., medications, anemia, pregnancy) and life-threatening problems, such as cancer. Results of laboratory studies affect management in only 5 percent of patients, and if initial results are normal, repeat testing is generally not indicated. Treatment of all types of fatigue should include a structured plan for regular physical activity that consists of stretching and aerobic exercise, such as walking. Caffeine and modafinil may be useful for episodic situations requiring alertness. Short naps are proven performance enhancers. Selective serotonin reuptake inhibitors, such as fluoxetine, paroxetine, or sertraline, may improve energy in patients with depression. Patients with chronic fatigue may respond to cognitive behavior therapy. Scheduling regular follow-up visits, rather than sporadic urgent appointments, is recommended for effective long-term management.
One fifth of family medicine patients present with fatigue, and one third of adolescents report having fatigue at least four days per week.1 Men and women differ in the way they describe fatigue: men typically say they feel tired, whereas women say they feel depressed or anxious.2,3 No etiology can be identified in one third of cases of fatigue. Overexertion, deconditioning, viral illness, upper respiratory tract infection, anemia, lung disease, medications, cancer, and depression are common causes.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Exercise therapy should be prescribed for patients with fatigue, regardless of etiology. | A | 16–18, 32, 43, 44, 46 | There is no evidence that exercise therapy worsens outcomes. |
| Selective serotonin reuptake inhibitors, such as fluoxetine (Prozac), paroxetine (Paxil), or sertraline (Zoloft), may be helpful for patients with fatigue in whom depression is suspected. | B | 22, 49 | A six-week trial is recommended to evaluate effectiveness. |
| Cognitive behavior therapy is an effective treatment for adult outpatients with chronic fatigue syndrome. | A | 22, 47, 48 | — |
| Stimulants seldom return patients to predisease performance. | B | 21, 45 | Stimulants are associated with headaches, restlessness, insomnia, and dry mouth. |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Sleepiness is the impairment of the normal arousal mechanism and is characterized by a tendency to fall asleep. Persons who are sleepy are temporarily aroused by activity, whereas fatigue is intensified by activity, at least in the short-term.4 Patients with sleepiness feel better after a nap, but patients with fatigue report a lack of energy, mental exhaustion, poor muscle endurance, delayed recovery after physical exertion, and nonrestorative sleep. Figure 1 provides a questionnaire to help differentiate between sleepiness and fatigue.5,6
Figure 1. Patient Health Questionnaire: Differentiating Between Sleepiness and Fatigue
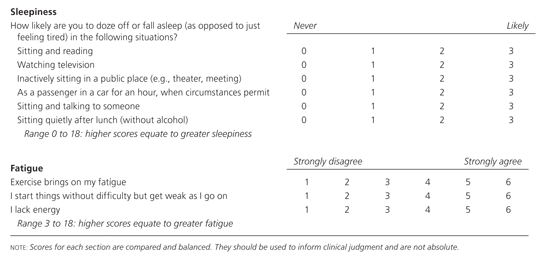
Patient questionnaire for differentiating between sleepiness and fatigue.
Information from references 5 and 6.
Fatigue may be classified as secondary, physiologic, or chronic. Secondary fatigue is caused by an underlying medical condition and may last one month or longer, but it generally lasts less than six months. Physiologic fatigue is an imbalance in the routines of exercise, sleep, diet, or other activity that is not caused by an underlying medical condition and is relieved with rest Chronic fatigue lasts longer than six months and is not relieved with rest.7
Evaluation
Physicians should begin the evaluation of patient presenting with fatigue by identifying common causes. The doses and scheduling of prescribed and over-the-counter medications should be reviewed. Medication classes that are commonly associated with fatigue, although sometimes only in the first week or two of use, include sedative-hypnotics, antidepressants, muscle relaxants, opioids, antihypertensives, antihistamines, and many types of antibiotics Even “nonsedating” antihistamines have an to 15 percent sedation rate.8 Six to 12 weeks of fatigue is not unusual during recovery from even minor surgery.9 The quality and quantity of sleep in patients with fatigue should also be evaluated (Table 1).
Table 1 Questions to Evaluate the Quality and Quantity of Sleep in Patients Presenting with Fatigue
| Question | Comments/follow-up questions |
|---|---|
| What time do you go to bed? | Regular bedtimes are associated with better sleep patterns. |
| What time do you fall asleep? | Many patients read or watch television in bed before falling asleep. |
| After you lie down, how long does it take you to fall asleep? | This time is known as sleep latency; the duration reflects sleepiness or anxiety at bedtime. |
| Do you leave the television or radio on as you are attempting to fall asleep? | Television and radio programs are intended to be stimulating and keep viewers and listeners awake. |
| After falling asleep, what time do you first wake up? What awakens you? | Does the patient wake up due to pain or the urge to urinate? |
| How often do you use the bathroom at night? | Does the patient develop the urge to urinate within a few minutes of waking up, or does the urge awaken the patient? |
| Do you have pain at night? | Does the patient have conditions, such as arthritis or muscle cramps, that could be better controlled? |
| How long does it take you to return to sleep after waking up? | Do certain thoughts keep the patient from returning to sleep? Are they anxiety-provoking, worrisome, depressing? |
| What time do you get out of bed in the morning? | Is the patient trying to get too much sleep? Does the patient have a natural sleep cycle? |
| Do you feel rested in the morning? | Was sleep restorative? |
| Do you nap during the day? | What time of day does the patient nap and for how long? |
| What medications do you take? | Has the patient tried sleep aids? Is the patient taking a medication that may interfere with sleep? |
| Do you drink alcohol or use other drugs? | Alcohol has a short half-life and, when used to assist sleep, often causes rebound wakefulness. |
| Do you exercise? What time of day? | Evening exercise tends to be stimulating and may increase sleep latency. |
Although it is possible for fatigue and depression to coexist, physicians should attempt to distinguish between them in order to guide management. Patients with fatigue report being unable to complete specific activities because of a lack of energy or stamina, whereas grief and depression are associated with a patient description that is more global, such as being unable to do “anything.”
Physical examination findings that suggest specific secondary causes of fatigue include lymphadenopathy (indicating tumor spread or recurrence), cardiac murmurs (endocarditis), goiter (thyroid hormone imbalance), edema (heart failure, liver disease, or malnutrition), poor muscle tone (advancing neurologic condition), and neurologic abnormalities (stroke or brain metastases).
Laboratory studies should be considered (Table 210–12), although their results affect management in only 5 percent of patients.12 Many physicians order a complete blood count, erythrocyte sedimentation rate, chemistry panel, thyroid-stimulating hormone measurement, and urinalysis. Women of childbearing age should receive a pregnancy test. No other tests have been shown to be useful unless the history or physical examination suggests a specific medical condition.10–12
Table 2 Laboratory Testing for Patients with Unexplained Fatigue
| Test* | Possible conditions | Comments |
|---|---|---|
| Complete blood count Erythrocyte sedimentation rate Chemistry panel Thyroid function tests Human immunodeficiency virus antibodies Pregnancy test, if indicated | Anemia Inflammatory state Liver disease, renal failure, protein malnutrition Hypothyroidism Chronic infection, if not previously tested Pregnancy, breathlessness due to progestins | Should be performed in most patients with a two-week history of fatigue; results change management in 5 percent of patients12 |
| Chest radiography Tuberculin skin test Electrocardiography Pulmonary function tests Toxicology screen Lyme titers Rapid plasma reagin Brain magnetic resonance imaging Echocardiography Specialized blood testing (e.g., ferritin, iron, vitamin B12, and folate levels; iron-binding capacity; direct antiglobulin test) | Adenopathy, cancer Tuberculosis, chronic infection Congestive heart failure, arrhythmia Chronic obstructive pulmonary disease, cancer Substance abuse Chronic Lyme disease Syphilis infection Multiple sclerosis Valvular heart disease, congestive heart failure Iron deficiency, Addison disease, celiac disease, myasthenia gravis, poisoning | Rarely useful; consider only if indicated by physical findings or abnormal baseline blood test results |
*— Arranged by the relative frequency that the tests produce results.
Managing Secondary Fatigue
Medications that may be causing fatigue should be replaced or discontinued, if possible, and physiologic parameters should be corrected. With cancer, renal disease, or other chronic diseases associated with anemia, patients are likely to be less fatigued if their hemoglobin level is maintained at 10 g per dL (100 g per L), using erythropoietin agents if needed.13,14 Nonanemic, menstruating women who have low normal ferritin levels report modest increased energy after four weeks of iron supplementation.15
Performing some form of daily exercise, sustaining interpersonal relationships, and returning to work are consistently associated with improvement in fatigue of any etiology.16,17 Regular moderate aerobic activity (i.e., 30 minutes of walking or an equivalent activity on most days of the week) reduces disease-related fatigue more effectively than rest. Yoga, group therapy, and stress management diminish fatigue in patients with cancer.18 Patients who have features suggestive of depression may be offered a six-week trial of a selective serotonin reuptake inhibitor (SSRI).19 Psychostimulants (e.g., methylphenidate [Ritalin], modafinil [Provigil]) improve fatigue in the short-term in patients with human immunodeficiency virus, multiple sclerosis, or cancer.20 Stimulants seldom return patients to predisease performance, and the drugs are associated with headaches, restlessness, insomnia, and dry mouth.21,22 If used, stimulants are best used as needed for episodic situations requiring alertness.
Physiologic Fatigue
Physiologic fatigue is initiated by inadequate rest, physical effort, or mental strain unrelated to an underlying medical condition. Diminished motivation and boredom also play a role. Physiologic fatigue is most common in adolescents and older persons. In the United States, 24 percent of adults report having fatigue lasting two weeks or longer, and two thirds of these persons cannot identify the cause of their fatigue.23
During intense training, well-conditioned athletes occasionally misinterpret fatigue as illness or depression.24 Conversely, fatigue and depression can emerge in a physically fit athlete after as little as one week with no exercise. Submaximal exercise mitigates these symptoms when training is limited because of injury.25
MANAGEMENT
Adequate sleep (i.e., generally seven to eight hours per night for adults) decreases tension and improves mood.26 Patients should be instructed to restructure their daily activities to get the sleep they need, and to practice good sleep hygiene. Recommendations for good sleep hygiene include the following: maintaining a regular morning rising time; increasing activity level in the afternoon; avoiding exercise in the evening or before bedtime; increasing daytime exposure to bright light; taking a hot bath within the two hours before bedtime; avoiding caffeine, nicotine, alcohol, and excessive food or fluid intake in the evening; using the bedroom only for sleep and sex; and practicing a bedtime routine that includes minimizing light and noise exposure and turning off the television.27 Naps may help, but should be limited to less than one hour in the early afternoon. One study showed that when hospitals provided patient coverage for medical intern naps (averaging 40 minutes) during overnight shifts, the interns achieved morning fatigue scores equivalent to those who were not on call.28 Time off from work also minimizes fatigue and decreases stress.29
Stimulants improve short-term performance. A randomized, double-blind, crossover study of persons driving in nighttime conditions showed that participants had fewer errors after consuming regular coffee (i.e., 200 mg of caffeine) or taking a 30-minute nap.30 Modafinil, which is approved to manage fatigue that is induced by shift work, has the same effect on performance as 600 mg of caffeine. Modafinil and caffeine do not have most of the adverse cardiovascular effects and abuse potential that are associated with amphetamines.30 Although modafinil and caffeine temporarily improve performance, they are not a substitute for adequate rest, and long-term use of modafinil has been associated with depression.
Physical fitness also improves energy levels. One study showed that truck drivers who engaged in 30-minute exercise sessions more than once a week had fewer traffic incidents.31 Another study showed that 10 weeks of supervised exercise increased energy levels among persons with fatigue, regardless of the underlying cause.32
Chronic Fatigue
Chronic fatigue is defined as fatigue that lasts longer than six months. Medical conditions that may cause or contribute to chronic fatigue are listed in Table 3. The prevalence of idiopathic chronic fatigue ranges from five to 40 per 100,000, depending on the population studied.33
Table 3 Selected Differential Diagnosis of Chronic Fatigue
| Cardiopulmonary: congestive heart failure, chronic obstructive pulmonary disease, peripheral vascular disease, atypical angina |
| Disturbed sleep: sleep apnea, gastroesophageal reflux disease, allergic or vasomotor rhinitis |
| Endocrine: diabetes mellitus, hypothyroidism, pituitary insufficiency, hypercalcemia, adrenal insufficiency, chronic kidney disease, hepatic failure |
| Infectious: endocarditis, tuberculosis, mononucleosis, hepatitis, parasitic disease, human immunodeficiency virus, cytomegalovirus |
| Inflammatory: rheumatoid arthritis, systemic lupus erythematosus |
| Medication use (e.g., sedative-hypnotics, analgesics, antihypertensives, antidepressants, muscle relaxants, opioids, antibiotics) or substance abuse |
| Psychological: depression, anxiety, somatization disorder, dysthymic disorder |
EPIDEMIOLOGY AND NATURAL HISTORY
Chronic fatigue occurs in all age groups, including children. Women, minorities, and persons with lower educational and occupational statuses have a higher prevalence of chronic fatigue.
On average, a typical family physician has in his or her practice two patients with fatigue of longer than six months for which no explanation can be determined.33 The diagnostic criteria for chronic fatigue syndrome (Table 434) are useful for defining disability or for research purposes, but may not be clinically helpful in all circumstances. Two thirds of patients with chronic fatigue do not meet these criteria, but they share many similarities to those with the syndrome and have only a slightly better prognosis.35
Table 4 Diagnostic Criteria for Chronic Fatigue Syndrome
| Major criteria: |
| At least six months' duration; does not resolve with bed rest; reduces daily activity to less than 50 percent; other conditions have been excluded |
| Physical criteria: |
| Low-grade fever; nonexudative pharyngitis; lymphadenopathy |
| Minor criteria: |
| Sore throat; mild fever or chills; lymph node pain; generalized muscle weakness; myalgia; prolonged fatigue after exercise; new-onset headaches; migratory noninflammatory arthralgia; sleep disturbance; neuropsychological symptoms (e.g., photophobia, scotomata, forgetfulness, irritability, confusion, inability to concentrate, depression, difficulty thinking); description of initial onset as acute or subacute |
note:A diagnosis of chronic fatigue syndrome includes all major criteria plus: eight minor criteria, or six minor criteria and two physical criteria.
Information from reference 34.
Only 2 percent of patients who are chronically fatigued report complete long-term resolution of symptoms, but 64 percent have limited improvement. Patients whose symptoms worsen for longer than 24 hours after physical exertion have a poor prognosis.36,37
EVALUATION
Detailed psychiatric and sleep histories may help determine possible psychosocial contributors to fatigue. A focused examination that communicates the physician's interest in, and engagement with, the patient's problem should be performed at every visit.38 Laboratory tests for chronic fatigue demonstrate some abnormality in 12 percent of patients and lead to alternate diagnoses in up to 8 percent of patients.39 However, when initial test results are normal, referral to an occupational sub-specialist, psychiatrist, or another physician is more helpful than repeating the tests.40,41
MANAGEMENT
Patients who believe that their symptoms are related to modifiable factors (e.g., workload, stress, coping strategies, depression, overcommitment) are much more likely to recover than those who believe that their symptoms are due to external factors, such as a viral infection.42 In a British study, 90 percent of patients who saw generalists for chronic fatigue received medication, diagnostic testing, or referral.38 The patients, however, were seeking to engage the physician, convey their suffering, and receive reassurance; the patients reported greatest satisfaction with physician explanations linking physical and psychological factors to psychosocial management.
Meta-analyses confirm the effectiveness of regular structured exercise. Four weeks of aerobic, strength, or flexibility training is associated with improved energy and decreased fatigue,43 and moderate aerobic exercise (e.g., a daily 30-minute walk) has a more consistently positive impact on fatigue than any other intervention studied.44 With the exception of patients with depression, pharmacologic therapy (including stimulants) only has a short-term impact.45,46 Cognitive behavior therapy is effective.22,47,48
A six-week trial of an SSRI (e.g., fluoxetine [Prozac], paroxetine [Paxil], sertraline [Zoloft]) may be considered in patients with chronic fatigue if depression is possible.22 If the patient has difficulty getting restful sleep, trazodone (Desyrel, brand no longer available in the United States), doxepin, or imipramine (Tofranil) may be effective.49 If pain is present, the patient may respond to venlafaxine (Effexor), desipramine (Norpramin), nortriptyline (Pamelor), duloxetine (Cymbalta), or a nonsteroidal anti-inflammatory drug.
Many patients perceive that physicians and their staff are more responsive to them when they describe physical symptoms.50 Fatigue, even when linked with a disease process, is associated with an imbalance of sleep, stress, or psychological coping skills. Balancing these factors reduces reliance on and is more effective than medication.38 Regular visits (i.e., every two weeks to two months) allow physicians to focus on fatigue as a central problem and circumvent the tendency for these patients to present at urgent care appointments.41
Data Sources: The review included a PubMed search for articles published from 1998 to 2007 using the terms sleep, sleep deprivation, fatigue, and insomnia; 665 references were evaluated for relevance to fatigue in primary care. A secondary review of cited references was also performed.

