Chronic insomnia is highly prevalent in our society, with an incidence of 10 to 30 percent. It is a major cost to society in terms of health care expenditure and reduced productivity. Nonpharmacologic interventions have been studied and shown to produce reliable and sustained improvements in sleep patterns of patients with insomnia. Cognitive behavior therapy for insomnia has multiple components, including cognitive psychotherapy, sleep hygiene, stimulus control, sleep restriction, paradoxical intention, and relaxation therapy. Cognitive psychotherapy involves identifying a patient’s dysfunctional beliefs about sleep, challenging their validity, and replacing them with more adaptive substitutes. Sleep hygiene education teaches patients about good sleep habits. Stimulus control therapy helps patients to associate the bedroom with sleep and sex only, and not other wakeful activities. Sleep restriction therapy consists of limiting time in bed to maximize sleep efficiency. Paradoxical intention seeks to remove the fear of sleep by advising the patient to remain awake. Relaxation therapies are techniques taught to patients to reduce high levels of arousal that interfere with sleep. Cognitive behavior therapy involves four to eight weekly sessions of 60 to 90 minutes each, and should be used more frequently as initial therapy for chronic insomnia.
Insomnia is a common problem among patients who present to family physicians, resulting in lost productivity, decreased quality of life, and increased morbidity. Insomnia results in high health care utilization, with direct and indirect costs of $77 to $92 billion annually.1–3 Consequences of insomnia include fatigue, mood disturbances, and problems related to employment and relationships.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| CBT should be used as initial treatment for chronic insomnia. | A | 2, 3, 5, 17–21 |
| CBT for chronic insomnia is as effective as medications, and the results are more sustainable. | B | 2–7 |
| Medications may be useful for acute insomnia when immediate symptom relief is desired. | C | 18 |
| Stimulus control and sleep restriction are effective in the treatment of chronic insomnia. | B | 5, 9, 17 |
CBT = cognitive behavior therapy.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Many behavior therapies have been developed to help patients resolve their sleep problems without the use of medications. These therapies are designed to educate patients about proper sleep habits, correct misconceptions about sleep, and use established techniques to improve sleep. Many studies have shown that these behavior therapies are as effective as medical treatment for insomnia, with more sustainable results.2–5 Cognitive behavior therapy (CBT) sustained patients’ sleep improvements 12 and 24 months later. 6,7 Those who were treated with pharmacotherapy alone did not sustain their benefits. This has also been demonstrated for older adults.6,7 CBT alone yields the greatest number of normal sleepers,8 with reports of greater patient satisfaction than with pharmacotherapy.6
Definition
Chronic insomnia is a condition of difficulty with initiating or maintaining sleep, or of experiencing nonrestorative sleep, that lasts for at least one month and causes significant daytime impairment. By definition, primary insomnia is not caused by another sleep disorder, underlying psychiatric or medical condition, or substance abuse disorder.9,10 Secondary (or comorbid) insomnia implies an underlying cause, such as depression or another sleep disorder.1 Thirty-five to 44 percent of patients presenting to a sleep specialist may have an underlying cause for their insomnia, emphasizing the need to screen for other conditions (Table 111,12).5,13
Table 1 Causes of Secondary or Comorbid Insomnia
| Anxiety |
| Asthma |
| Chronic obstructive pulmonary disease |
| Congestive heart failure |
| Depression |
| Fibromyalgia |
| Gastroesophageal reflux disease |
| Hyperthyroidism |
| Medications (see Table 2) |
| Menopause |
| Obstructive sleep apnea |
| Pain |
| Periodic limb movement disorder |
| Pruritus |
| Restless legs syndrome |
| Urinary incontinence |
Insomnia may be further characterized as acute (i.e., less than four weeks) or chronic (i.e., greater than four weeks), with symptoms occurring on at least three nights per week. Regardless of duration or course, most studies have adopted an arbitrary definition of insomnia as a delay of more than 30 minutes in sleep onset or a sleep efficiency (i.e., the percentage of time in bed that is spent sleeping) of less than 85 percent.13
Incidence
Studies suggest that approximately 30 percent of the general population have symptoms of sleep disruption, and approximately 10 percent have associated daytime functional impairment.1,14 However, up to 50 percent of patients do not report this to their physicians.1,3 Older persons, women, those who are divorced or widowed, persons with lower socioeconomic status or concomitant health problems, and persons who snore are at an increased risk of insomnia.15
Older persons are at particular risk of insomnia, partly on the basis of age-related changes in sleep physiology.2,15 They have decreased sleep efficiency and deep sleep, and increased sleep latency (i.e., time until sleep onset). They often have circadian rhythm disturbances, with earlier bedtimes and wake times. This results in excessive daytime sleepiness with an increased risk of accidents (e.g., falls), fatigue, and decreased memory and concentration.1,11
Diagnostic Evaluation
Physicians should have a high index of suspicion for insomnia and might consider asking about it during the general review of systems.16 A detailed sleep history should be obtained, with information from family members or caregivers, when possible, and should include questions about medication and substance use (Table 2).11,12 Sleep records kept for at least two weeks are helpful. They should include the patient’s bedtime, total sleep time, number and length of awakenings after sleep onset, sleep quality, daytime symptoms, and use of sleep medications (Figure 1).16 To avoid disrupting sleep, estimates should be recorded in the morning.16 The shortfalls of sleep diaries are that patients tend to overestimate sleep latency and underestimate the number of awakenings and total sleep time.17
Table 2. Selected Medications That May Cause Insomnia
| Alcohol |
| Antidepressants (e.g., selective serotonin reuptake inhibitors, bupropion [Wellbutrin]) |
| Beta blockers |
| Caffeine |
| Chemotherapy agents (selected) |
| Cimetidine (Tagamet) |
| Diuretics |
| Herbal remedies (selected) |
| Illicit drugs (selected) |
| Nicotine |
| Phenytoin (Dilantin) |
| Pseudoephedrine (Sudafed) |
| Steroids |
| Stimulant laxatives |
| Theophylline |
Figure 1. Sleep Diary
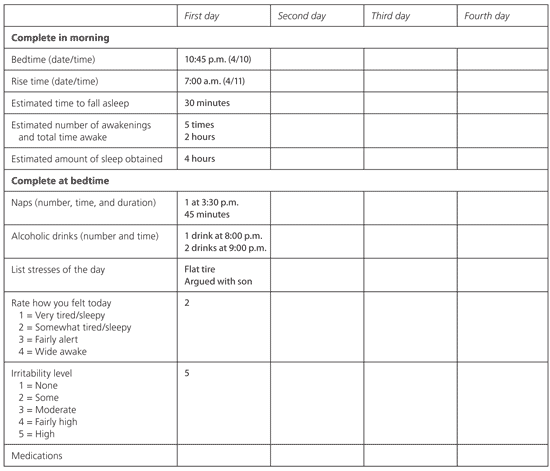
Sample sleep diary for use in patients with insomnia. The diary provides a night-to-night account of the patient’s sleep schedule and perception of sleep.
Adapted with permission from Insomnia: assessment and management in primary care. National Heart, Lung, and Blood Institute Working Group on Insomnia. Am Fam Physician. 1999;59(11):3033.
Polysomnography may be needed to evaluate for secondary causes of insomnia. Referral for polysomnography or to a sleep medicine specialist may also be indicated when the diagnosis is in doubt or when treatment is refractory or requires special expertise, such as with sleep apnea.
Treatment
CBT is effective for treatment of primary insomnia.3,17–21 However, its use is impeded by several factors, including underdiagnosis of insomnia and lack of awareness among health care professionals.18 Cost can be a perceived barrier, but because of its sustained effects, nonpharmacologic therapy may be more cost-effective than pharmacotherapy.17 In addition to cognitive therapy, CBT for insomnia comprises behavior therapies such as sleep hygiene education, stimulus control, sleep restriction, paradoxical intention, and relaxation therapy. Therapy consists of four to eight 60- to 90-minute sessions to educate patients about good sleep practices, modify maladaptive coping mechanisms, reduce hyperarousal states, and resolve misconceptions about sleep.
Extensive outcomes research supports the use of CBT for primary insomnia and, more recently, for patients with a psychiatric or medical comorbidity (i.e., secondary insomnia)20–22 and for chronic users of hypnotics.20,21 Two meta-analyses of 29 trials showed that CBT is effective for the treatment of insomnia in older adults.2,23 Studies evaluating physical exercise in older adults found significant improvement in sleep parameters with the addition of exercise.24,25
One meta-analysis of 59 trials and 2,102 patients with chronic insomnia found that psychological interventions averaging five hours of therapy time produced reliable changes in sleep latency and time awake after sleep onset.17 Sleep latency was decreased by 43 percent with CBT, compared with a 30 percent decrease with pharmacotherapy alone. Clinical improvements were maintained at the average follow-up of six months.
Another meta-analysis found that CBT is comparable with pharmacotherapy for treatment of primary insomnia in general, and is superior to pharmacotherapy for sleep-onset insomnia.18 CBT is useful when the patient is reluctant to use medications. Pharmacotherapy may be considered when the condition is acute and immediate symptom reduction is required.18
CBT Techniques
Although CBT has demonstrated effectiveness for insomnia treatment in randomized controlled trials, few physicians are experienced in this therapy.18 However, most physicians can teach patients the basic CBT principles of stimulus control and sleep restriction.5 Physicians may also utilize nurse practitioners20 and physician assistants who have had training in CBT to teach patients these techniques.
COGNITIVE THERAPY
The goal of cognitive therapy is to break the cycle of insomnia, emotional distress, dysfunctional beliefs, and further sleep disturbances.11 It consists of identifying a patient’s dysfunctional beliefs about sleep, challenging their validity, and replacing them with more adaptive substitutes.5 This may be more important when dealing with insomnia in older patients.12 Examples of concepts to discuss with patients include realistic expectations about sleep requirements, realistic consequences of insomnia, and healthy strategies to promote sleep.6
SLEEP HYGIENE EDUCATION
Sleep hygiene education seeks to optimize sleep quality by teaching patients about good sleep habits (Table 312,13).5 Avoiding the use of caffeine in the later hours of the day is important because of its half-life of four hours, as is limiting the amount of overall caffeine consumption. Heavy meals should be avoided within two hours of bedtime. There should be minimal intake of fluids after dinner to prevent frequent nighttime urination. Exercise is important to maintaining healthy sleep because fit persons are better sleepers.26 However, it is important to avoid exercise for 90 minutes to four hours before sleep.26 Ear-plugs can be used if noise is a problem.5 Patients should be exposed to daytime light for at least 30 minutes in the morning.27 Regardless of the cause, most patients with insomnia benefit from approaches that focus on good sleep habits,11,12 especially when combined with other CBT approaches.5
Table 3. Sleep Hygiene
| Avoid caffeine and nicotine, especially late in the day. |
| Avoid exercise during the four hours before bedtime; daily exercise is beneficial to sleep, but can interfere if done close to bedtime. |
| Avoid large meals in the evening. |
| Avoid taking naps. |
| Go to sleep and wake up at the same times each day. |
| Keep the bedroom at a comfortable temperature. |
| Make the bedroom as dark as possible. |
| Set aside a time to relax before bed and use relaxation techniques. |
STIMULUS CONTROL
One of the most effective therapies for insomnia is stimulus control, even when used alone.5,9,17 Patients are taught to eliminate distractions and associate the bedroom only with sleep and sex. Reading and television watching should occur in a room other than the bedroom. Stimulus control also involves going to bed only when a person is tired and leaving the room if not asleep within 15 to 20 minutes. This pattern should be repeated throughout the night as often as necessary. Patients should avoid napping and should get out of bed at the same time each day. This therapy has been shown to decrease sleep latency from 64 to 34 minutes.17 Contraindications for stimulus control therapy include conditions of restricted mobility, frailty, and increased risk of falls.22
SLEEP RESTRICTION
Sleep restriction consists of limiting the time in bed to maximize sleep efficiency. Patients are asked to estimate their total time asleep by using sleep diaries, and to restrict their time in bed to the average estimated sleep time. Time in bed must not be less than five hours, and morning wake time should be held constant throughout treatment. Sleep efficiency is calculated by dividing total sleep time by time spent in bed and multiplying by 100. When sleep efficiency exceeds 90 percent, the patient’s time in bed is increased by 15 to 20 minutes. This calculation is repeated on a weekly basis. Sleep restriction therapy has been shown to decrease sleep latency from 48 to 19 minutes5 and is one of the more effective therapies, even when used alone.17,28 Sleep restriction therapy should be used with caution in patients with epilepsy, bipolar disorder, and parasomnias (e.g., sleepwalking) because it may worsen these disorders. Sleep restriction also may increase daytime sleepiness and make activities such as driving unsafe.22
PARADOXICAL INTENTION
Paradoxical intention is another therapy proven to be effective for insomnia.9 This therapy seeks to remove the fear of not being able to sleep by advising the patient to remain awake. The patient is asked to follow other sleep hygiene instructions and to remain awake as long as possible.
RELAXATION THERAPY
Relaxation therapies are based on the premise that patients with insomnia display high levels of physiologic and cognitive arousal throughout the day and night.5 Positron emission tomography has shown increased cerebral metabolism of glucose in patients with insomnia.13 Relaxation therapies are meant to deactivate this hyperarousal. Table 4 provides a list of relaxation techniques and definitions.12,17,27,29 Most therapies can be self-administered by patients after initial professional guidance and regular practice over several weeks.5
Table 4 Relaxation Therapies
| Technique | Comments |
|---|---|
| Autogenic training | Imagine a peaceful environment and comforting body sensations, such as warmth and heaviness in the limbs, warmth in the upper abdomen, and coolness on the forehead |
| Biofeedback training | Visual or auditory feedback is provided to the patient to control chosen physiologic parameters |
| Hypnosis | — |
| Imagery training | Visualization technique with focus on pleasant or neutral images |
| Meditation, abdominal Breathing | — |
| Paced respirations | Take a deep breath and hold for five seconds, repeat several times; focus on the sound of the breath |
| Progressive muscle relaxation | Tense and relax large muscle groups; usually begin with the feet and work your way up to the facial muscles |
| Repetitive focus | Focus on a word, sound, prayer, phrase, or muscle activity |

