
Am Fam Physician. 2009;79(6):511-512
Author disclosure: Nothing to disclose.
A 45-year-old woman with a history of human immunodeficiency virus (HIV) infection, acquired immunodeficiency syndrome (AIDS), diabetes, and depression presented with pruritic papules on her face and trunk that had persisted for two days. She reported that the itching led to fatigue and difficulty sleeping. The patient was being treated with highly active antiretroviral therapy (HAART), including ritonavir (Norvir), emtricitabine (Emtriva), and tenofovir (Viread). She denied taking any new medications, including over-the-counter products. The patient’s last documented CD4 cell count was 8 per mm3 (8 × 109 per L). She denied having fever, chills, nausea, diarrhea, or cough.
Multiple firm, symmetric, flesh-colored, nearly confluent papules were noted on the forehead, cheeks, and chin (Figures 1 and 2). Several similar papules were present on the chest and back. The excoriated lesions were nontender to palpation. Laboratory results included normal liver function tests, pancytopenia, and negative antinuclear antibody and rapid plasma reagin tests.
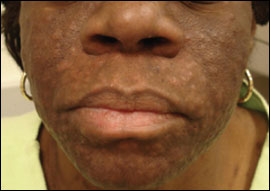
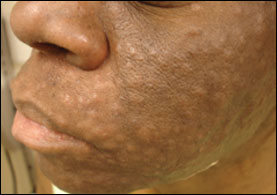
A skin biopsy of the patient’s chin was performed. A hematoxylineosin stain revealed chronic folliculosebaceous inflammation, accompanied by a polymorphous infiltrate with scattered eosinophils. The results of direct Gram stain, bacterial, fungal, and viral tissue cultures were negative.
Question
Discussion
The answer is A: AIDS-associated eosinophilic folliculitis. Eosinophilic folliculitis, or Ofuji disease, occurs in otherwise healthy persons. AIDS-associated eosinophilic folliculitis differs from Ofuji disease in that it has a greater pruritic intensity and lacks circinate and palmoplantar lesions. Typically, the lesions of eosinophilic folliculitis are 2- to 3-mm, erythematous papules or pustules that primarily affect the upper body. The disease is rarely generalized. Patients report severe pruritus and fatigue, and deep excoriation may be present.1 Eosinophilic folliculitis also may be associated with lymphoma, leukemia, and myelodysplastic syndrome.2 Opportunistic infections, follicular hypersensitivity reactions, and an autoimmune reaction to sebum are possible etiologic causes.3 Eosinophilic folliculitis usually occurs in late-stage AIDS or when the CD4 cell count is less than 250 per mm3 (250 × 109 per L). Thus, AIDS-associated eosinophilic folliculitis is considered a marker of immunosuppression.4 Fifty percent of patients with the condition may also have peripheral eosinophilia and elevated immunoglobulin E levels. The prevalence is unknown, although it is thought to be declining since the advent of HAART.3
The patient’s eosinophilic folliculitis remained active despite treatment with antihistamines, itraconazole (Sporanox), and topical corticosteroids. An attempt to control her eosinophilic folliculitis with phototherapy was discontinued because of painful herpes simplex virus type 1 eruptions. Isotretinoin (Accutane) was not an option because of her severe depression. Treatment with a daily application of permethrin 5% cream (Elimite) was initiated. This treatment is thought to reduce the number of Demodex mites in the skin, as well as the inflammatory response they trigger.1
The uniformity and confluence of the patient’s eruption differ from the classic presentation of arthropod bites, which is linear papules arranged in groups of three on exposed areas.5 No lice were noted on her clothing.
The cutaneous eruption of secondary syphilis typically is symmetric and papular and involves the trunk and extremities, including the palms and soles. The lesions are red or copper-colored and are often scaly. The syphilitic rash is rarely pustular or severely pruritic. The treatment of choice for syphilis is penicillin G (Pfizerpen).6
Because the patient denied taking any new medications, a drug eruption is unlikely. New medication use typically causes a more generalized erythematous eruption within 10 to 14 days of initiating the therapy.
The patient had no personal or family history of eczema, asthma, or seasonal respiratory allergies (atopy). Also, no eczematous changes in the skin, especially in the flexural areas, were noted on physical examination, ruling out papular atopic dermatitis.3 Pruritic popular eruption (PPE) of HIV should be considered in any patient with HIV infection who has nonfollicular papules. PPE of HIV is controversial because some experts consider it to be a variant of eosinophilic folliculitis. PPE of HIV appears as sterile pustules and flesh-colored to reddish papules with a symmetric distribution on the trunk and extremities. Most patients with PPE of HIV have a CD4 cell count of less than 100 per mm3 (100 × 109 per L).1,7 The etiology is unclear, but PPE may be an exaggerated immune response to arthropod antigens in the follicular epithelium.8
| Condition | Characteristics |
|---|---|
| Arthropod bites | Papules in a linear pattern; usually appearing in groups of three on exposed skin |
| Secondary syphilis | Red or copper-colored lesions on the trunk and extremities, including palms and soles, that may have thin scaling |
| Drug eruption | Patient history of prescription or over-the-counter medication use; often has a more diffuse distribution, including the chest and back |
| Eosinophilic folliculitis | Pruritic papules, typically on the upper body; can be associated with human immunodeficiency virus infection |
| Papular atopic dermatitis | Possible patient history of asthma, seasonal respiratory allergies (atopy), itching, or skin eruption in flexural areas |