
Am Fam Physician. 2009;79(7):595-596
Author disclosure: Nothing to disclose.
A 47-year-old man presented with chronic neck and lower back pain that had persisted for more than 20 years. The pain had noticeably worsened in the previous two years. He also had progressive stiffness and limited range of motion in his neck and lower back. The patient occasionally experienced sharp pain and numbness down his left arm. Various over-the-counter anti-inflammatory drugs did not provide much relief. He had a history of obesity, hypertension, and coronary artery disease.
The patient had severely limited range of motion in his cervical spine of only 10 to 15 degrees in all directions. The lumbar forward flexion was mildly limited at 85 degrees, but extension was intact. He also had significant paraspinous muscle spasms. Results of a complete blood count, metabolic profile, liver panel, erythrocyte sedimentation rate, and C-reactive protein level were unremarkable. Lateral cervical spine radiography was obtained (see accompanying figure).
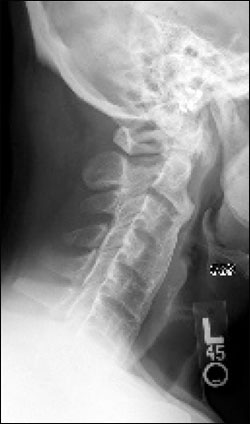
Question
Discussion
The correct answer is C: diffuse idiopathic skeletal hyperostosis (DISH). DISH, or Forestier disease, is a common skeletal disorder characterized by ossification of the anterior longitudinal ligament of the spine, but may involve other axial or peripheral joint ligaments and insertion points. This ossification leads to a “flowing osteophytes” pattern as shown in the accompanying figure. There is loss of normal cervical lordosis, but the disk height is preserved.
DISH is common among persons older than 50 years, and the reported prevalence ranges from 10 to 35 percent among those older than 70 years. The condition is more common and usually more severe in men. There is no known etiology, but it is associated with various metabolic and cardiovascular conditions, including diabetes, hyperinsulinemia, obesity, hyperuricemia, dyslipidemia, hypertension, coronary artery disease, and stroke.1,2 Because patients with DISH have higher levels of serum uric acid, alkaline phosphatase, growth hormone, and insulin-like growth factor-I, metabolic disturbances may have a role in the underlying pathogenesis of the condition.3
Patients with DISH usually present with chronic spinal pain and limited mobility. Other potential sequelae include dysphagia, spinal stenosis, myelopathy, and radiculopathy. The diagnosis is based on Resnick's radiographic criteria4:
Presence of flowing calcification and ossification along the anterolateral aspects of at least four contiguous vertebral bodies, with or without associated localized, pointed excrescences at the intervening vertebral body-disk junctions
A relative preservation of intervertebral disk height in the involved vertebral segments and the absence of extensive radiographic “degenerative” changes
Absence of apophyseal joint bony ankylosis and sacroiliac joint erosion, sclerosis, or bony fusion
There is no specific treatment that can halt the process of DISH. Therefore, treatment usually focuses on relieving pain, maintaining physical function, and preventing and treating sequelae. In addition to analgesics and physical therapy, surgical intervention is occasionally required. Treatment of underlying metabolic disorders is also needed to reduce associated morbidity and mortality.5
The differential diagnosis of chronic cervical pain and prominent spinal osteophytes include ankylosing spondylitis, cervical spondylosis, psoriatic arthritis, and congenital anomalies such as Klippel-Feil syndrome. Differentiating among these entities helps prevent unnecessary evaluation and treatment.