Generalized anxiety disorder is common among patients in primary care. Affected patients experience excessive chronic anxiety and worry about events and activities, such as their health, family, work, and finances. The anxiety and worry are difficult to control and often lead to physiologic symptoms, including fatigue, muscle tension, restlessness, and other somatic complaints. Other psychiatric problems (e.g., depression) and nonpsychiatric factors (e.g., endocrine disorders, medication adverse effects, withdrawal) must be considered in patients with possible generalized anxiety disorder. Cognitive behavior therapy and the first-line pharmacologic agents, selective serotonin reuptake inhibitors, are effective treatments. However, evidence suggests that the effects of cognitive behavior therapy may be more durable. Although complementary and alternative medicine therapies have been used, their effectiveness has not been proven in generalized anxiety disorder. Selection of the most appropriate treatment should be based on patient preference, treatment success history, and other factors that could affect adherence and subsequent effectiveness.
Anxiety disorders, such as generalized anxiety disorder (GAD), panic disorder, posttraumatic stress disorder, and obsessive-compulsive disorder, are the most common mental health problems in the United States.1,2 As with other anxiety disorders, GAD is associated with impairments in mental health, social/role functioning, general health, bodily pain, physical functioning, and daily activities. It is also associated with an increase in physician visits.3 One third of patients with GAD have one or more additional anxiety disorders, often accompanied by a decline in functional status and an increased risk of other psychiatric problems or substance abuse.3,4 GAD is linked to self-medication with alcohol or other drugs5 and to suicidal ideation.6 Impairment associated with GAD is equal to that associated with major depression,7 and it is related to increased health care use and economic costs.7,8 Despite the prevalence of GAD and its subsequent impact on health, functioning, and the economy, the condition is too often misdiagnosed and managed incorrectly.7
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Patients experiencing anxiety should be evaluated for depression. | C | 3 |
| Cognitive behavior therapy has been shown to be at least as effective as medication for GAD with less attrition and more durable effects. | A | 17, 19 |
| Some SSRIs (escitalopram [Lexapro], paroxetine [Paxil], sertraline [Zoloft]); SNRIs (venlafaxine [Effexor], duloxetine [Cymbalta]); and benzodiazepines are more effective than placebo in the treatment of GAD. | A | 25–27, 30–35 |
| SSRI or SNRI therapy is more beneficial for patients with GAD and comorbid depression than benzodiazepine or buspirone (Buspar) therapy. | A | 24–27, 40 |
| Kava is effective in the treatment of GAD, but safety concerns limit its use. | B | 49–52 |
GAD = generalized anxiety disorder; SNRI = serotonin-norepinephrine reuptake inhibitor; SSRI = selective serotonin reuptake inhibitor.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Epidemiology
GAD is the most common anxiety disorder in primary care. The 12-month prevalence of GAD is 3.1 percent in population-based surveys,2 and between 5.3 and 7.6 percent among patients who visit primary care offices.3,9 The highest rate of GAD (7.7 percent) occurs in persons 45 to 49 years of age, and the lowest rate (3.6 percent) occurs in persons 60 years and older.1 Women are almost twice as likely as men to be diagnosed with GAD over their lifetime.10 Although the prevalence of GAD decreases with age in men, it increases in women.11
Diagnosis
The diagnostic criteria for GAD from the Diagnostic and Statistical Manual of Mental Disorders, 4th ed., text revision (DSM-IV-TR) are shown in Table 1.12 Controversy exists regarding the duration of symptoms necessary to make a diagnosis. Some authors suggest using a one-month symptom duration because the six-month requirement may unnecessarily exclude from treatment those patients whose symptoms fluctuate.13,14
Table 1 DSM-IV-TR Diagnostic Criteria for Generalized Anxiety Disorder
| A. Excessive anxiety and worry (apprehensive expectation), occurring more days than not for at least six months, about a number of events or activities (such as work or school performance). | |
| B. The person finds it difficult to control the worry. | |
| C. The anxiety and worry are associated with three (or more) of the following six symptoms (with at least some symptoms present for more days than not for the past six months). | |
| (1) Restlessness or feeling keyed up or on edge | |
| (2) Being easily fatigued | |
| (3) Difficulty concentrating or mind going blank | |
| (4) Irritability | |
| (5) Muscle tension | |
| (6) Sleep disturbance (difficulty falling or staying asleep, or restless unsatisfying sleep) | |
| D. The focus of the anxiety and worry is not confined to features of an Axis I disorder (e.g., the anxiety or worry is not about having a panic attack [as in panic disorder], being embarrassed in public [as in social phobia], being contaminated [as in obsessive-compulsive disorder], being away from home or close relatives [as in separation anxiety disorder], gaining weight [as in anorexia nervosa], having multiple physical complaints [as in somatization disorder], or having a serious illness [as in hypochondriasis]), and the anxiety and worry do not occur exclusively during posttraumatic stress disorder. | |
| E. The anxiety, worry, or physical symptoms cause clinically significant distress or impairment in social, occupational, or other important areas of functioning. | |
| F. The disturbance is not due to the direct physiologic effects of a substance (e.g., a drug of abuse, a medication) or a general medical condition (e.g., hyperthyroidism) and does not occur exclusively during a mood disorder, a psychotic disorder, or a pervasive developmental disorder. | |
DSM-IV-TR = Diagnostic and Statistical Manual of Mental Disorders, 4th ed., text revision. Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed., text revision. Washington, DC: American Psychiatric Association; 2000:476.
Patients with GAD may constantly worry about their health, family, work, and finances. Worrying is difficult to control, often negatively affecting relationships and social and work activities.3 Patients with GAD commonly present with nonspecific somatic symptoms (e.g., insomnia, headaches, muscle aches, fatigue, gastrointestinal symptoms).5 Because of the high level of comorbidity with other mental health and medical problems, physicians must rule out other psychiatric disorders (e.g., depression)3 and nonpsychiatric conditions (e.g., hypoglycemia, cardiomyopathy; Online Table A). Some medications and other substances may also cause symptoms of anxiety (e.g., caffeine, alcohol, amphetamines; Online Table B).
Several self-report questionnaires are available to assist physicians in the diagnosis of anxiety disorders. The seven-item GAD scale (GAD-7; Figure 1)3,15 is a reliable, valid, and easy-to-use self-report questionnaire for evaluating the presence and severity of GAD. A cutoff score of 8 points demonstrates strong sensitivity (92 percent) and specificity (76 percent) for the diagnosis of GAD, and higher scores are related to worsening functional impairment. The GAD-7 detects only a probable diagnosis of GAD; positive scores should be followed by more extensive interviewing (e.g., using the DSM-IV-TR criteria) accompanied by appropriate management and referral. A simpler two-item scale, GAD-2, is also shown in Figure 1.3,15 Although it has nearly the same accuracy as GAD-7, the latter provides additional information that can guide management.
Figure 1. GAD-2 and GAD-7 Scales
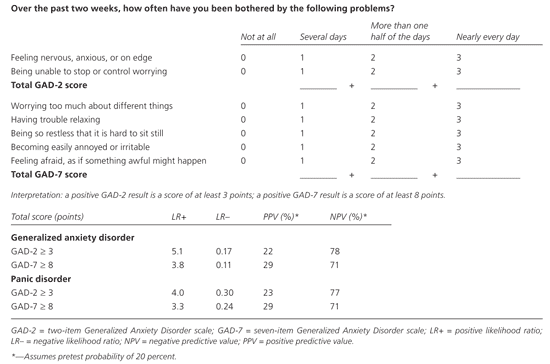
GAD-2 and GAD-7 scales.
Adapted with permission from Kroenke K, Spitzer RL, Williams JB, Monahan PO, Löwe B. Anxiety disorders in primary care: prevalence, impairment, comorbidity, and detection. Ann Intern Med. 2007;146(5):W77, with additional information from reference 15.
Treatment
Psychological, pharmacologic, and complementary and alternative medicine (CAM) interventions for GAD should begin with supportive listening and education about anxiety. Helping patients understand that anxiety is a manageable medical condition is essential. Patient education should include discussing the role of thoughts and lifestyle on anxiety and how modification of these can reduce symptoms.16,17
PSYCHOLOGICAL COUNSELING
Counseling effectively reduces anxiety symptoms in most patients. Specifically, cognitive behavior therapy (CBT) has been shown to reduce GAD symptomatology 18; it also appears to be at least as effective as medication with less attrition and more durable effects.16,18,19 Although formal CBT involves multiple sessions with trained mental health professionals, an awareness of the principles of therapy may assist physicians in incorporating CBT techniques into their practices and reinforcing formal therapeutic efforts.20,21
CBT addresses the role of irrational thinking in how patients feel and behave. CBT for GAD typically includes patient self-monitoring of worrying or related symptoms; cognitive restructuring, including evaluating and reconsidering interpretive and predictive thoughts/worries; relaxation training; and rehearsal of coping skills.22 Patients may be asked to monitor their symptoms of anxiety along with situational factors and thoughts leading up to episodes of increased anxiety. This information is used to help them recognize triggers of anxiety and patterns of maladaptive thinking. Patients are taught to challenge unrealistic or unwarranted worrying and to replace these thoughts with more realistic problem-solving strategies. They also may be instructed in the use of self-calming techniques, such as deep breathing, relaxation, and exercise, to reduce physiologic arousal and to enhance their sense of control over their symptoms. Patients are then encouraged to use these techniques outside of the clinical setting (Online Table C).16
PHARMACOLOGIC TREATMENT
In the past decade, the number of pharmacologic therapies for GAD has increased (Table 2).23 Selection of an agent is influenced by patient characteristics; adverse-effect profile; and the existence of comorbid mood disorders, especially unipolar depression.24
Table 2 Selected Pharmacologic Agents for the Treatment of Generalized Anxiety Disorder
| Agent | Usual initial dosage | Usual dosage range* | Cost of brand (generic)† |
|---|---|---|---|
| Antidepressants | |||
| Duloxetine (Cymbalta) | 30 mg daily | 30 to 120 mg daily | $127 |
| Escitalopram (Lexapro) | 10 mg daily | 10 to 20 mg daily | 91 |
| Imipramine (Tofranil)‡ | 25 to 50 mg daily | 100 to 300 mg daily | 282 (28) |
| Paroxetine (Paxil) | 20 mg daily | 20 to 50 mg daily | 110 (49 to 82) |
| Sertraline (Zoloft)‡ | 25 to 50 mg daily | 50 to 200 mg daily | 107 (81 to 85) |
| Venlafaxine (Effexor)‡ | 37.5 mg two times daily | 75 to 375 mg, divided, two to three times daily | 81 (66 to 78) |
| Benzodiazepines | |||
| Alprazolam (Xanax) | 0.25 to 0.5 mg three times daily | 0.5 to 6 mg daily | 49 (9 to 30) |
| Chlordiazepoxide (Librium) | 5 to 10 mg two to three times daily | 10 to 25 mg two to four times daily | 129 (20 to 30) |
| Clonazepam (Klonopin)‡ | 0.25 mg two times daily | 0.5 to 4 mg, divided, two times daily | 37 (7 to 22) |
| Clorazepate (Tranxene) | 7.5 to 15 mg two times daily | 15 to 60 mg, divided, two to three times daily | 178 (62 to 96) |
| Diazepam (Valium) | 2 to 5 mg two to four times daily | 2 to 10 mg, divided, four times daily | 87 (25 to 40) |
| Lorazepam (Ativan) | 0.5 to 1 mg three times daily | 0.5 to 2 mg three times daily | 126 (49 to 56) |
| Oxazepam (formerly Serax) | 10 mg three times daily | 10 to 30 mg three to four times daily | 92 (40 to 77) |
| Other | |||
| Buspirone (Buspar) | 7.5 mg two times daily | 30 to 60 mg, divided, two to three times daily | 172 (20 to 80) |
| Hydroxyzine (Vistaril) | 50 mg four times daily | 50 to 400 mg daily | 52 (3 to 20) |
| Pregabalin (Lyrica)‡ | 75 mg two times daily | 200 to 600 mg daily | 135 |
*— Dosage should be 50 percent less in adults 65 years and older.23
†— Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar) in Red Book. Montvale, N.J.: Medical Economics Data; 2009. Cost to the patient will be higher, depending on prescription filling fee.
‡— Not specifically approved by the U.S. Food and Drug Administration for the treatment of generalized anxiety disorder.
SSRIs and SNRIs. Selective serotonin reuptake inhibitors (SSRIs) have emerged as first-line therapies for patients with GAD. A well-defined mechanism of action for these agents has yet to be determined, but it may involve down-regulation of noradrenergic receptors. The primary advantage of SSRIs is their potential for long-term use without fear of tolerance or abuse. Many SSRIs and serotonin-norepinephrine reuptake inhibitors (SNRIs) have effectively treated GAD in clinical trials, but only paroxetine (Paxil), escitalopram (Lexapro), duloxetine (Cymbalta), and venlafaxine (Effexor) are approved by the U.S. Food and Drug Administration (FDA) for this indication.25-27 In general, comparable effectiveness has been reported in studies of paroxetine versus sertraline (Zoloft), extended-release venlafaxine versus paroxetine, extended-release venlafaxine versus duloxetine, and paroxetine versus escitalopram; no single agent has emerged as superior.28-33 Similar studies are necessary before one SSRI can be recommended over another or before an SSRI can be recommended over an SNRI based on effectiveness.
Some of the more common adverse events associated with SSRI and SNRI use include nausea, sexual dysfunction, agitation, weight gain, and insomnia. Although these effects tend to be mild, they may be mistaken for worsening anxiety and may lead to nonadherence; thus, patients should be advised accordingly. Benzodiazepines may be prescribed concurrently during the initial few weeks of treatment to counteract some of these anticipated adverse effects. This practice may also offset the delay in onset of therapeutic effectiveness (typically one to four weeks) associated with SSRIs and SNRIs. Fewer adverse events have been reported with escitalopram than with paroxetine.32 Lastly, because withdrawal symptoms, such as nausea, paresthesias, anxiety, dizziness, and insomnia, are not uncommon with the use of SSRI and SNRI therapy, a slow taper over several weeks is recommended.
Benzodiazepines. Benzodiazepines are believed to interact with receptors activated by the neuroinhibitory transmitter, γ-aminobutyric acid (GABA). In doing so, they promote binding of GABA to GABA subunit receptors (GABA A) and enhance chloride ion influx.34 Benzodiazepines have been widely used because of their rapid onset of action and proven effectiveness in managing GAD symptoms.35 Their role in the long-term management of the disorder is less clear. Furthermore, with the exception of alprazolam (Xanax), benzodiazepines are not effective in resolving the depression that often accompanies GAD.
The various benzodiazepine agents appear to be equally effective in managing GAD. The choice of agent should be guided by pharmacokinetic differences and cost. Short- to intermediate-acting agents (oxazepam [formerly Serax], alprazolam, and lorazepam [Ativan]) are preferred because they are less likely to accumulate and lead to the excessive daytime sedation and confusion that often occur with the use of longer-acting agents (diazepam [Valium], chlordiazepoxide [Librium], and clorazepate [Tranxene]).36
Use of benzodiazepines in older adults is particularly troublesome because of a greater risk of adverse events.36,37 Among older adults and patients with impaired hepatic functioning, the metabolic characteristics of oxazepam, lorazepam, and temazepam (Restoril) are generally preferred because there is less tendency for accumulation.23 Despite a low risk of abuse, benzodiazepines are best avoided in patients who have previously demonstrated addictive behavior.38 Discontinuation should be carried out gradually over several weeks in all patients who have had four or more weeks of treatment to avoid withdrawal symptoms (e.g., a return of anxiety, agitation, insomnia, irritability, restlessness). Imipramine (Tofranil) may help patients discontinue long-term benzodiazepine use, although it does not alter the severity of withdrawal symptoms.39
Buspirone. Buspirone (Buspar) is an azapirone that has demonstrated superior effectiveness compared with placebo, but it may not be as effective as benzodiazepines.40 The mechanism of action of buspirone is thought to be mediated through serotoninergic activity, specifically as an agonist of the serotonin receptor subtype 5-hydroxytryptamine-1A. The FDA approved the drug as a nonaddictive, nonsedating alternative to benzodiazepines. However, buspirone has not been established as a first-line agent because of a one- to three-week delay in symptom relief, no impact on comorbid depression, and a relatively short half-life necessitating dosing two to three times per day. Overall, it is well tolerated with mild adverse effects, such as dizziness, blurred vision, and nausea. Buspirone is an FDA pregnancy category B agent, whereas SSRIs, SNRIs, and benzodiazepines are FDA pregnancy category C or D agents.
Other Agents. Pregabalin (Lyrica), despite having structural similarities to GABA, does not interact with the GABA receptor or the benzodiazepine receptor. Its mechanism of action is thought to be caused by inhibition of the release of excitatory neurotransmitters in a manner similar to gabapentin (Neurontin).41 Pregabalin has been approved in Europe for the treatment of GAD, although it has not been FDA approved for this indication. In multiple clinical trials, it has been shown to relieve psychic and somatic symptoms of anxiety in a manner similar to lorazepam,42,43 alprazolam,44 and venlafaxine.45 The onset of action occurred within the first week, and the most common adverse effects were nausea and dizziness. Additionally, there were no serious withdrawal symptoms with a one-week taper. However, there appears to be a marked dose-response relationship in patients taking pregabalin, with benefit occurring at a minimum threshold dosage of 200 mg per day.46 Dosage adjustments are necessary in patients with renal disease. Additional long-term studies are needed to further assess effectiveness and safety in patients with concomitant depression.
Hydroxyzine (Vistaril) has demonstrated superior effectiveness compared with placebo without evidence of rebound anxiety. Withdrawal symptoms did not differ markedly from those of placebo.47 Tricyclic antidepressants, such as imipramine, have been used for treatment of GAD, but have largely been replaced by the safer and better tolerated SSRIs and SNRIs.
CAM INTERVENTIONS
In the United States, CAM therapies are used more often than mainstream medicine to manage anxiety and depression.48 CAM treatments include herbal supplements, nutritional supplements, aromatherapy, meditation, and acupuncture.
Herbal Supplements. Kava extract (Piper methysticum) has been researched extensively. A Cochrane systematic review 49 and a meta-analysis50 noted the superiority of kava over placebo in treating anxiety. However, kava cannot be recommended for clinical use because of its association with hepatotoxicity.51,52 Although valerian, St. John's wort, and passionflower have also been used to manage GAD, there is insufficient evidence regarding their effectiveness and safety.53-55
Nutritional Supplements. Evidence is lacking on the effectiveness and safety of nutritional supplements, such as adrenal extracts, ginger, green tea, macrobiotic diets, oats, amino acids, melatonin, omega-3 fatty acids, or S-adenosylmethionine, in the treatment of anxiety disorders.53
Aromatherapy. In one small, open-label, noncontrolled study of aromatherapy combined with massage, improvements in anxiety and mood were noted over eight months.56 A larger study examined the use of aromatherapy and massage in patients with cancer.57 Improvements in mood and anxiety were noted after two weeks, but disappeared by 10 weeks. Although it was a randomized study, it also lacked a control group. These studies make it difficult to distinguish the effects of aromatherapy alone because both combined aromatherapy with massage.
Meditation. A recent Cochrane systematic review failed to draw any conclusions about the effectiveness of meditation compared with conventional treatments for anxiety.58 Meditation-based stress management, which entails a structured program involving meditation, has been shown to be helpful in treating several disorders, including anxiety.59 Another meditation-related program, mindfulness-based cognitive therapy, has been shown to reduce symptoms of anxiety and depression60-63; however, positive findings regarding the benefits of meditation-based therapies for anxiety are tempered by methodologic concerns.58-63
Acupuncture. A small study 64 demonstrated the superiority of acupuncture over breathing retraining in patients with hyperventilation syndrome, and another study 65 showed the usefulness of acupuncture in patients with posttraumatic stress disorder. However, no studies have shown acupuncture to be effective in patients with GAD.
Selecting a Treatment Approach
When selecting a treatment for patients with GAD, physicians should consider several factors, including patient preference, treatment success history, and other factors that may interfere with successful treatment (e.g., presence of comorbid psychological or medical problems, intolerable adverse effects, adherence potential, third-party reimbursement issues).66 Psychiatric or psychological referral should be considered in patients who fail to demonstrate improvement or if serious comorbid problems, such as suicidal/homicidal ideation or substance abuse, occur or worsen (Table 3).
Table 3 Resources on Anxiety for Physicians
| American Psychiatric Association (http://www.psych.org) |
| American Psychological Association (http://www.apa.org) |
| Anxiety Disorders Association of America (http://www.adaa.org) |
| Association for Behavioral and Cognitive Therapies (http://www.aabt.org/) |
| National Association of Cognitive-Behavioral Therapists (http://www.nacbt.org/) |
| National Institute of Mental Health (http://www.nimh.nih.gov/health/topics/anxiety-disorders/index.shtml) |
| Wright JH, Basco MR, Thase ME. Learning cognitive-behavior therapy: an illustrated guide. In: Gabbard GO, ed. Core Competencies in Psychotherapy. Arlington, Va.: American Psychiatric Publishing; 2006. |

