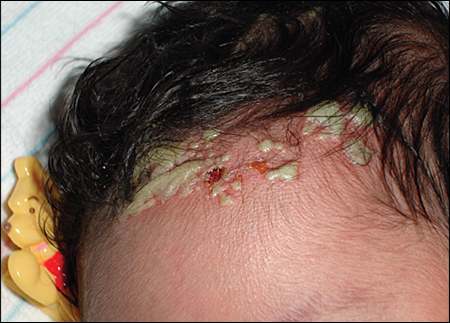
An otherwise healthy, full-term newborn presented with a rash on her scalp. The mother had no history of sexually transmitted infections, no genital rashes or lesions immediately before delivery, and no complications during pregnancy. The infant was delivered by cesarean because of arrest of descent. She was afebrile and showed no signs of toxicity after delivery. No rash was present on the initial physical examination. However, on the second day of life, physical examination showed a papulopustular rash confined to the intrapartum presenting area of the scalp (see accompanying figure). No lymphadenopathy, vesicles, or other pathologic findings were noted. Results of a complete blood count with differential were unremarkable. A potassium hydroxide preparation showed no fungal elements. Tzanck test and viral culture results were also unremarkable. Clusters of gram-positive cocci were present.
Question
Based on the patient's history, physical examination, and laboratory studies, which one of the following is the most likely diagnosis?
A. Cutaneous candidiasis.
B. Erythema toxicum neonatorum.
C. Herpes simplex virus (HSV) infection.
D. Methicillin-resistant Staphylococcus aureus (MRSA) pustulosis.
E. Neonatal acne.
F. Transient neonatal pustular melanosis.
Discussion
The answer is D: MRSA pustulosis. MRSA infections have been associated with patients in heath care facilities and in infants in neonatal intensive care units (i.e., because of premature birth, low birth weight, prolonged hospitalization, or indwelling catheters). However, the incidence of community-associated infections in full-term, otherwise healthy newborns is increasing.1–3 In full-term newborns, MRSA infection usually first appears as a skin and soft tissue infection, but may rapidly progress to osteomyelitis, pneumonia, and sepsis.2 Staphylococcal pustulosis manifests on any area of skin as a papulopustular rash that may coalesce and form bullae. Physicians should obtain a Gram stain and culture of any pustular lesions in a newborn.4 Culture is the first-line test for diagnosis of staphylococcal pustulosis. In one study, 44 percent of culture-positive patients had a negative Gram stain result.5 Patients with severe pustulosis or systemic symptoms may require blood, urine, and cerebrospinal fluid cultures to rule out systemic infection.5
Cutaneous candidiasis is uncommon in newborns but is thought to be acquired from maternal vaginal colonization. The condition may appear as an erythematous, papulopustular rash on any area of the skin, usually with crusting and desquamation. Systemic infection is rare in full-term infants.4
Erythema toxicum neonatorum is one of the most common benign rashes in the neonatal period. It is characterized by erythematous macules, often with a central pustule or vesicle. The macules may appear on the face, trunk, and extremities. The rash usually resolves spontaneously within a week.
HSV infection is a potentially devastating infection in newborns. It initially manifests as vesicles or pustules grouped on an erythematous base, and can lead to significant systemic disease. It may appear on the face and scalp. A maternal history of HSV infection can assist in the diagnosis, but most cases of neonatal HSV infection develop after delivery by an asymptomatic mother.4
Neonatal acne is characterized by an inflammatory, erythematous, papulopustular rash on the face and scalp. Although it may appear at birth, this condition usually occurs after two weeks of life and resolves spontaneously during the first few months of life.
Transient neonatal pustular melanosis is a benign skin condition of unknown etiology. It may appear at birth, usually on the chin, forehead, chest, or back. The condition is present in up to 5 percent of black newborns and in less than 1 percent of white newborns.6 It is characterized by nonerythematous vesicles filled with a milky fluid, superficial pustules, and pigmented macules that are usually 2 to 10 mm in size. If diagnosis is required, Wright stain of the pustular fluid would reveal neutrophils with few eosinophils. This condition usually resolves within 48 hours, although hyperpigmented macules may remain for several months.7
Summary Table
| Condition | Characteristics |
|---|---|
| Cutaneous candidiasis | Erythematous, papulopustular rash on any area of skin, usually with crusting and desquamation; uncommon in newborns |
| Erythema toxicum neonatorum | Erythematous macules, usually with small, central vesicles or pustules; may appear on the face, trunk, and extremities |
| Herpes simplex virus infection | Vesiculopustular rash, grouped on an erythematous base, on the face and scalp |
| Staphylococcal pustulosis | Papulopustular rash that may coalesce and form bullae; may appear on any area of skin |
| Neonatal acne | Inflammatory, erythematous, papulopustular rash on the face and scalp; usually appears after two weeks of life, although it may be present at birth |
| Transient neonatal pustular melanosis | Nonerythematous vesicles filled with a milky fluid, superficial pustules, and pigmented macules that are usually 2 to 10 mm in size; appears on the chin, forehead, chest, or back; more common in black newborns than in white newborns |

