
This is a corrected version of the article that appeared in print.
Am Fam Physician. 2009;80(8):841-846
Author disclosure: Nothing to disclose.
Vitamin D deficiency affects persons of all ages. Common manifestations of vitamin D deficiency are symmetric low back pain, proximal muscle weakness, muscle aches, and throbbing bone pain elicited with pressure over the sternum or tibia. A 25-hydroxyvitamin D level should be obtained in patients with suspected vitamin D deficiency. Deficiency is defined as a serum 25-hydroxyvitamin D level of less than 20 ng per mL (50 nmol per L), and insufficiency is defined as a serum 25-hydroxyvitamin D level of 20 to 30 ng per mL (50 to 75 nmol per L). The goal of treatment is to normalize vitamin D levels to relieve symptoms and decrease the risk of fractures, falls, and other adverse health outcomes. To prevent vitamin D deficiency, the American Academy of Pediatrics recommends that infants and children receive at least 400 IU per day from diet and supplements. Evidence shows that vitamin D supplementation of at least 700 to 800 IU per day reduces fracture and fall rates in adults. In persons with vitamin D deficiency, treatment may include oral ergocalciferol (vitamin D2) at 50,000 IU per week for eight weeks. After vitamin D levels normalize, experts recommend maintenance dosages of cholecalciferol (vitamin D3) at 800 to 1,000 IU per day from dietary and supplemental sources.
In the 19th century, vitamin D deficiency was identified as the cause of the rickets epidemic in children living in industrialized cities. This discovery led to the fortification of various foods, and the resolution of a major health problem associated with vitamin D deficiency. However, recent studies have shown that vitamin D deficiency and insufficiency are associated with other pathologic conditions in persons of all ages. Vitamin D plays an important role in skeletal development, bone health maintenance, and neuromuscular functioning. Because the signs and symptoms of vitamin D deficiency are insidious or nonspecific, it often goes unrecognized and untreated.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Vitamin D supplementation of 700 to 800 IU per day reduces falls in older adults. | B | 12, 13 |
| Vitamin D supplementation of 700 to 800 IU per day reduces fractures in older adults. | A | 16–18 |
| To prevent vitamin D deficiency, the recommended intake of vitamin D is 400 IU per day for infants and children with inadequate sun exposure, and 400 to 600 IU per day for adults with inadequate sun exposure. Maintenance dosages of 800 to 1,000 IU of vitamin D per day are recommended for adults with vitamin D deficiency, except in those with malabsorption syndromes. | C | 1, 8, 29 |
Definitions
In adults, vitamin D deficiency is defined as a serum 25-hydroxyvitamin D level of less than 20 ng per mL (50 nmol per L), and insufficiency is defined as a serum 25-hydroxyvitamin D level of 20 to 30 ng per mL (50 to 75 nmol per L).1
There are two forms of vitamin D: vitamin D2 (ergocalciferol), which comes from irradiation of the yeast and plant sterol; ergosterol; and vitamin D3 (cholecalciferol) which is obtained from oily fish and by skin synthesis. There are few dietary sources that contain vitamin D2 (Table 11); therefore, it is difficult to maintain adequate levels of vitamin D from dietary sources alone. Humans typically obtain 90 percent of vitamin D from sunlight.1,3,4
| Source | Approximate vitamin D content* |
|---|---|
| Fortified sources | |
| Cereal | 100 IU per serving |
| Milk | 100 IU per 8 oz |
| Orange juice | 100 IU per 8 oz |
| Nonfortified food sources | |
| Breast milk† | 20 IU per L |
| Cod liver oil | 400 IU per teaspoon |
| Egg yolk | 20 IU |
| Mackerel (canned) | 250 IU per 3.5 oz |
| Salmon (canned) | 300 to 600 IU per 3.5 oz |
| Salmon (fresh, farmed) | 100 to 250 IU per 3.5 oz |
| Salmon (fresh, wild) | 600 to 1,000 IU per 3.5 oz |
| Sardines (canned) | 300 IU per 3.5 oz |
| Tuna (canned) | 230 IU per 3.6 oz |
| Prescription supplements | |
| Vitamin D2 (ergocalciferol) | 50,000 IU per capsule |
| Vitamin D2 (ergocalciferol [Drisdol]) liquid supplements | 8,000 IU per mL |
| 1,25-dihydroxyvitamin D (calcitriol [Rocaltrol]) | 0.25 or 0.5 mcg per capsule |
| 1,25-dihydroxyvitamin D (calcitriol [Calcijex]) | 1 mcg per mL solution for injection |
| Over-the-counter supplements | |
| Vitamin D3or cholecalciferol | 400, 800, 1,000, or 2,000 IU per tablet |
Epidemiology and Risk Factors
Vitamin D deficiency in adults was previously thought to be limited to older persons living in institutions, but recent evidence suggests otherwise.5 A group of international experts concluded that approximately 50 percent of persons 65 years and older in North America and 66 percent of persons internationally (all ages) failed to maintain healthy bone density and tooth attachment because of inadequate vitamin D levels.3
Risk factors for vitamin D deficiency are listed in Table 2.4,5 A common cause of deficiency is medication use, such as anticonvulsants or glucocorticoids, which can increase catabolism and actively destroy vitamin D.1 However, approximately one third of persons with known deficiency have no identifiable risk factors.5 For example, in a study of 142 healthy persons, most of whom consumed milk and supplements, participants 18 to 29 years of age with no risk factors for deficiency were found to have the lowest levels of vitamin D.6
| Age older than 65 years |
| Breastfed exclusively without vitamin D supplementation |
| Dark skin |
| Insufficient sunlight exposure |
| Medication use that alters vitamin D metabolism (e.g., anticonvulsants, glucocorticoids) |
| Obesity (body mass index greater than 30 kg per m2) |
| Sedentary lifestyle |
Pathogenesis
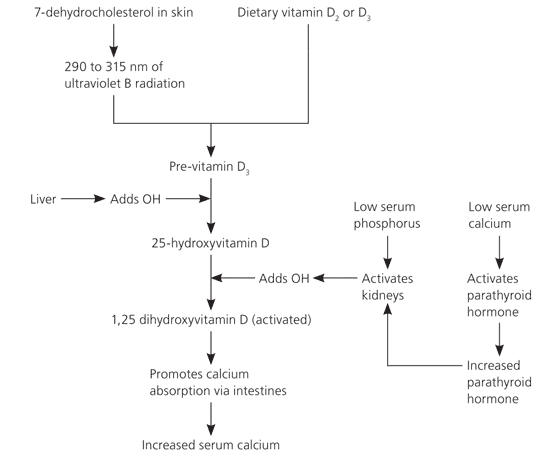
The interactions between parathyroid hormone, serum calcium, and vitamin D are outlined in Figure 1. Without the presence of activated vitamin D, normal bone metabolism is altered so that only 10 percent of calcium and 60 percent of phosphorus is absorbed.1 As a result, the skeleton becomes the body's primary source of calcium,4 with osteoclasts dissolving bone to raise serum calcium.7 These actions lead to osteomalacia, and they precipitate and exacerbate osteopenia and osteoporosis.4,7,8
Manifestations of Vitamin D Deficiency
Vitamin D deficiency causes bone to demineralize. In children, bones soften over time and become deformed, leading to growth retardation, enlargement of the epiphyses of the long bones, and leg deformities.9 Adults with osteomalacia may experience global bone discomfort and muscle aches, often leading to a misdiagnosis of fibromyalgia, chronic fatigue syndrome, or arthritis. Because vitamin D receptors are present in skeletal muscle, deficiency may also lead to proximal muscle weakness; an increased risk of falls; global bone discomfort, often elicited with pressure over the sternum or tibia; and low back pain (in older women).8,10 Common manifestations of vitamin D deficiency are listed in Table 3.1,4,8-10
| Bone discomfort or pain (often throbbing) in low back, pelvis, lower extremities |
| Increased risk of falls and impaired physical function |
| Muscle aches |
| Proximal muscle weakness |
| Symmetric low back pain in women |
Benefits of Vitamin D Supplementation
FALL PREVENTION
In a randomized controlled trial (RCT) of 184 nursing home residents, patients who received 800 IU of vitamin D daily had a 72 percent reduction in falls compared with the placebo group.12 Another trial involving 445 ambulatory participants 65 years and older demonstrated that women with adequate levels of vitamin D and calcium who received calcium citrate (500 mg per day) and vitamin D3 (700 IU per day) had a markedly lower fall rate compared with the placebo group (47 versus 60 percent, respectively). The number needed to treat to prevent one fall was seven, and the impact was noted primarily in less active women.13
FRACTURE PREVENTION
In adults 65 years and older, more than 90 percent of hip fractures are caused by falling, and the one-year mortality rate for persons with hip fractures is 20 percent.14,15 Daily vitamin D intake is crucial in the reduction of hip and nonvertebral fracture rates. Clinical research suggests that the optimal daily dosage for adults in this age group is approximately 700 to 800 IU.16-18
A meta-analysis of 12 RCTs followed more than 19,000 persons older than 60 years living in ambulatory and institutional settings.16 The study assessed the overall effectiveness of vitamin D supplementation in preventing hip fractures and nonvertebral fractures. A vitamin D dosage of 700 to 800 IU per day reduced the relative risk of hip fracture by 26 percent and the relative risk of nonvertebral fracture by 23 percent, compared with calcium supplementation alone or placebo. No significant benefit in fracture reduction was observed at a dosage of 400 IU per day.16
In an RCT of community-dwelling men and women 65 to 85 years of age, persons taking vitamin D had a statistically significant decrease in osteoporotic fractures, particularly in women.17 The dosage shown to decrease fractures was approximately 800 IU per day, whereas a lower dosage of 400 IU per day was ineffective.17 In another RCT, 445 ambulatory white adults 65 years and older were randomized to receive 500 mg of calcium with 700 IU vitamin D per day or placebo.18 After three years, there was a statistically significant increase in total bone mineral density in the treatment group compared with placebo (P <.001), as well as a reduction in nonvertebral fracture rates in the treated women not taking estrogen.18
Role of Vitamin D in Other Conditions
CARDIOVASCULAR DISEASE
Research suggests that suboptimal vitamin D levels are associated with increased risk of cardiovascular disease. One study found that 25-hydroxyvitamin D levels were inversely related to the following cardiovascular risk factors: blood pressure greater than 140/90 mm Hg, blood glucose level above 125 mg per dL (6.95 mmol per L), and body mass index of 30 kg per m2 or greater.19
A recent analysis of the Framingham Offspring Study cohort measured the 25-hydroxyvitamin D levels of participants with no known cardiovascular disease (n = 1,939).20 During a follow-up period of about five years, 120 participants experienced their first cardiovascular event (e.g., myocardial infarction, angina, stroke, heart failure). There was a 62 percent higher risk of cardiovascular events in patients with hypertension whose 25-hydroxyvitamin D level was less than 15 ng per mL (38 nmol per L), compared with those whose level was 15 ng per mL or greater. Clinical trials are needed to determine whether vitamin D supplementation has a role in preventing cardiovascular events.
COLON CANCER
Vitamin D receptors have a broad tissue distribution, which includes colorectal tissues. In vitro studies have reported that colon cancers are responsive to the antiproliferative effects of 1,25-dihydroxyvitamin D.2 However, results of clinical studies present conflicting data. Evidence from the Women's Health Initiative RCT suggests that a modest dosage of calcium (1,000 mg per day) and vitamin D (400 IU per day) does not affect the risk of colorectal cancer in healthy women at average risk.21 Conversely, a nested case-control study from the Nurses' Health Study reported that the risk of colon cancer was inversely related to serum levels of 25-hydroxyvitamin D.22
DEPRESSION
Diagnostic Evaluation
The best indicator of vitamin D status is 25-hydroxyvitamin D because it is the major circulating form of vitamin D; it reflects cutaneous and dietary contributions; and it is thought to be a precursor for 1,25-dihydroxyvitamin D, the most active vitamin D metabolite.7,25 The metabolite 1,25-dihydroxyvitamin D should not be used to measure vitamin D levels because levels can be increased by secondary hyperparathyroidism.1 Physicians should consider vitamin D testing in patients who present with unexplained symptoms (Table 31,4,8–10).
Prevention and Treatment
To prevent vitamin D deficiency in persons with inadequate sun exposure, the Institute of Medicine has recommended adequate intake (AI) based on levels needed to maintain optimal bone health in all members of a healthy population. The current daily AI is 200 IU for infants, children, and adults younger than 51 years; 400 IU for adults 51 to 70 years of age; and 600 IU for adults older than 70 years.8,26,27 However, recent research suggests that current AI recommendations for children and adults may be too low to maintain optimal levels (above 30 ng per mL) for calcium absorption and parathyroid hormone suppression.3,28 Based on these concerns, the American Academy of Pediatrics recently recommended doubling the minimum daily intake for children and adolescents to 400 IU (Table 429).
| Supplementation of 400 IU per day is recommended for: |
| All breastfed infants unless they are weaned to a minimum of 1 L per day (33.8 fl oz) of vitamin D–fortified formula or milk |
| All infants who are not breastfed and who are ingesting less than 1 L per day of vitamin D–fortified formula or milk |
| All children and adolescents who do not get regular sunlight exposure; who do not ingest a minimum of 1 L per day of vitamin D–fortified formula or milk; or who do not take a daily multivitamin supplement containing at least 400 IU of vitamin D |
Information from reference 29 .
Vitamin D is a fat-soluble vitamin, and there are concerns about toxicity from excessive supplementation. Widespread fortification of food and drink from the 1930s to 1950s in the United States and Europe led to reported cases of toxicity.4 Table 5 lists signs of vitamin D toxicity, and Table 6 lists contraindications to vitamin D supplementation.30 The U.S. Preventive Services Task Force states that dosages of vitamin D greatly exceeding the recommended AI should be taken with care.31 According to the National Academy of Sciences, there is little risk of toxicity at supplementation levels of up to 2,000 IU per day.3
| Headache |
| Metallic taste |
| Nephrocalcinosis or vascular calcinosis |
| Pancreatitis |
| Nausea |
| Vomiting |
| Granulomatous diseases (e.g., tuberculosis) |
| Metastatic bone disease |
| Sarcoidosis |
| Williams syndrome |
To replenish serum 25-hydroxyvitamin D levels in persons with vitamin D deficiency, one cost-effective regimen is oral ergocalciferol at 50,000 IU per week for eight weeks. The optimal time for rechecking the serum levels after repletion has not been clearly defined, but the goal is to achieve a minimum level of 30 ng per mL. Serum 25-hydroxyvitamin D levels should be measured again after completion of therapy, and if values have not reached or exceeded the minimum level, a second eight-week course of ergocalciferol should be prescribed. If the serum 25-hydroxyvitamin D levels still have not risen, the most likely cause is nonadherence to therapy or malabsorption. If malabsorption is suspected, consultation with a gastroenterologist should be considered. After vitamin D levels are replete, maintenance dosages of cholecalciferol should be instituted at 800 to 1,000 IU per day from dietary and supplemental sources.1,2,4