The population of patients older than 65 years is projected to increase substantially in the coming years, particularly in rural areas. Family physicians are essential providers of geriatric care, especially in rural areas, but need payment reform to improve their capacity to meet the needs of older patients.
The proportion of Americans who are 65 years and older is projected to increase from 12 percent in 2005 to 20 percent by 2030.1 Growth will be even higher in rural areas, which already have more older residents.2 Baby boomers may have more chronic disease and live longer than past generations.
A recent Institute of Medicine report called for improved geriatric competency of all health care professionals, better recruitment and retention of health professionals, and new models of care delivery.1 Some predict 36,000 geriatricians will be needed by 2030 to meet the needs of a growing population of older patients.3
Analysis of U.S. Census and American Medical Association Master File data (see accompanying figure) revealed there are substantially more family physicians than general internists in all areas except the most urban, and more family physicians than geriatricians in all areas, especially in rural areas, which have a higher percentage of older persons.4,5 For example, in the 670 most rural counties (rural-urban continuum code levels 8 and 9), older persons were more than 17 percent of the population, and there were 68 geriatricians compared with 1,394 family physicians in these frontier areas.
Figure. Number of Physicians per Older Person by Rural-Urban Continuum Code
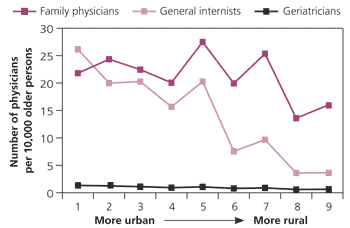
Office-based physicians per 10,000 older persons by rural-urban continuum code. Data from 2006.
Information from references 4 and 5.
Given the low numbers of geriatricians,3 current incentives for geriatric specialty practice, a small number of fellowship spots, and the decline of student interest in primary care and geriatrics, producing nearly 30,000 new geriatricians by 2030 is improbable. The training and distribution of family physicians makes them essential to providing care for older Americans. Any strategy to ensure high-quality geriatric care for all Americans now and in the future must include: enhanced geriatric training within primary care residencies; increased support for residency training in community- and rural-based programs; implementation of medical home models of care; and adequate payment to deliver and integrate increasingly complex care for older patients.

