Continuous electronic fetal monitoring was developed in the 1960s to assist in the diagnosis of fetal hypoxia during labor. Continuous electronic fetal monitoring has been shown to reduce the incidence of neonatal seizures, but there has been no beneficial effect in decreasing cerebral palsy or neonatal mortality. Intraobserver variability may play a major role in its interpretation. To provide a systematic approach to interpreting the electronic fetal monitor tracing, the National Institute of Child Health and Human Development convened a workshop in 2008 to revise the accepted definitions for electronic fetal monitor tracing. The key elements include assessment of baseline heart rate, presence or absence of variability, and interpretation of periodic changes. The workshop introduced a new classification scheme for decision making with regard to tracings. This system can be used in conjunction with the Advanced Life Support in Obstetrics course mnemonic, DR C BRAVADO, to assist in the systematic interpretation of fetal monitoring. DR C BRAVADO incorporates maternal and fetal risk factors (DR = determine risk), contractions (C), the fetal monitor strip (BRA = baseline rate, V = variability, A = accelerations, and D = decelerations), and interpretation (O = overall assessment).
Intrapartum fetal monitoring was developed in the 1960s to identify events that might result in hypoxic ischemic encephalopathy, cerebral palsy, or fetal death. Continuous electronic fetal monitoring (EFM), using external or internal transducers, became a part of routine maternity care during the 1970s; by 2002, about 85 percent of live births (3.4 million out of 4 million) were monitored by it.1 Continuous EFM has led to an increase in cesarean delivery and instrumental vaginal births; however, the incidences of neonatal mortality and cerebral palsy have not fallen, and a decrease in neonatal seizures is the only demonstrable benefit.2 The potential benefits and risks of continuous EFM and structured intermittent auscultation should be discussed during prenatal care and labor, and a decision reached by the pregnant woman and her physician, with the understanding that if intrapartum clinical situations warrant, continuous EFM may be recommended.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Compared with structured intermittent auscultation, continuous EFM showed no difference in overall neonatal death rate. Continuous EFM reduced neonatal seizures (NNT = 661), but not the occurrence of cerebral palsy. Continuous EFM increased cesarean delivery rates overall (NNH = 20) and instrumental vaginal births (NNH = 33). | A | 2 |
| Compared with structured intermittent auscultation, a period of EFM on maternity unit admission results in a lack of improved neonatal outcomes and increased interventions, including epidural analgesia (NNH = 19), continuous EFM (NNH = 7), and fetal blood scalp testing (NNH = 45). | A | 6 |
| Amnioinfusion for umbilical cord compression in the presence of decelerations reduced: fetal heart rate decelerations (NNT = 3); cesarean delivery overall (NNT = 8); Apgar score < 7 at five minutes (NNT = 33); low cord arterial pH (< 7.20; NNT = 8); neonatal hospital stay > three days (NNT = 5); and maternal hospital stay > three days (NNT = 7). | A | 22 |
| Compared with EFM alone, the addition of fetal electrocardiography analysis results in a reduction in operative vaginal deliveries (NNT = 50) and fetal scalp sampling (NNT = 33). | A | 25–28 |
| Fetal pulse oximetry has not shown a reduction in cesarean delivery rates. | A | 31 |
EFM = electronic fetal monitoring; NNH = number needed to harm; NNT = number needed to treat.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Selection of FHR Monitoring Method
There are several considerations when choosing a method of intrapartum fetal monitoring. Structured intermittent auscultation is a technique that employs the systematic use of a Doppler assessment of fetal heart rate (FHR) during labor at defined timed intervals (Table 1).4 It is equivalent to continuous EFM in screening for fetal compromise in low-risk patients.2,3,5 Safety in using structured intermittent auscultation is based on a nurse-to-patient ratio of 1:1 and an established technique for intermittent auscultation for each institution.4 Continuous EFM should be used when there are abnormalities in structured intermittent auscultation or for high-risk patients (Table 2).4 An admission tracing of electronic FHR in low-risk pregnancy increases intervention without improved neonatal outcomes, and routine admission tracings should not be used to determine monitoring technique.6
Table 1. Structured Intermittent Auscultation
| Frequency |
| Every 15 to 30 minutes in active phase of first stage of labor; every 5 minutes in second stage of labor with pushing |
| Indications |
| Assess FHR before: initiation of labor-enhancing procedure; ambulation of patient; administration of medications; or initiation of analgesia or anesthesia |
| Assess FHR after: admission of patient; artificial or spontaneous rupture of membranes; vaginal examination; abnormal uterine activity; or evaluation of analgesia or anesthesia |
| Procedure |
| 1. Palpate the abdomen to determine the position of the fetus (Leopold maneuvers) |
| 2. Place the Doppler over the area of maximal intensity of fetal heart tones |
| 3. Differentiate maternal pulse from fetal pulse |
| 4. Palpate for uterine contraction during period of FHR auscultation to determine relationship |
| 5. Count FHR between contractions for ≥ 60 seconds to determine average baseline rate |
| 6. Count FHR after uterine contraction for 60 seconds (at 5-second intervals) to identify fetal response to active labor (this may be subject to local protocols) |
FHR = fetal heart rate.
Information from reference 4.
Table 2. Maternal and Fetal High-Risk Factors That Indicate Use of Continuous Electronic Fetal Monitoring
| Occurrence | Risk factors |
|---|---|
| Antenatal | |
| Fetal | Abnormal umbilical artery Doppler velocimetry |
| Breech presentation | |
| Intrauterine growth restriction | |
| Multiple pregnancies | |
| Oligohydramnios | |
| Rh isoimmunization | |
| Maternal | Anemia |
| Antepartum hemorrhage | |
| Cardiac disease | |
| Diabetes | |
| Hypertension (preeclampsia or eclampsia) | |
| Hyperthyroidism | |
| Maternal motor vehicle collision or trauma | |
| Morbid obesity | |
| Renal disease | |
| Vascular disease | |
| Intrapartum | |
| Fetal | Abnormal fetal heart rate on auscultation or admission |
| tracing (20-minute strip)* | |
| Meconium-stained amniotic fluid | |
| Maternal | Hypertonic uterus |
| Induced or augmented labor | |
| Intrauterine infection or chorioamnionitis | |
| Post-term pregnancy (> 42 weeks' gestation) | |
| Preterm labor (< 32 weeks' gestation) | |
| Previous cesarean delivery | |
| Prolonged membrane rupture > 24 hours at term | |
| Regional analgesia, particularly after initial bolus and after top-ups (continuous electronic fetal monitoring is not required with mobile or continuous-infusion epidurals) | |
| Vaginal bleeding in labor | |
*— Although this continues to be widely accepted, randomized controlled trials have shown that electronic fetal monitoring performed at admission does not change outcomes.
Adapted with permission from Liston R, Sawchuck D, Young D, for the Society of Obstetrics and Gynaecologists of Canada, and the British Columbia Perinatal Health Program. Fetal health surveillance: antepartum and intrapartum consensus guideline. No. 197 (replaces No. 90 and No. 112) [published correction appears in J Obstet Gynaecol Can. 2007;29(11):909]. J Obstet Gynaecol Can. 2007;29(9 suppl 4):S33.
Continuous EFM may adversely affect the labor process and maternal satisfaction by decreasing maternal mobility, physical contact with her partner, and time with the labor nurse compared with structured intermittent auscultation.7 However, continuous EFM is used routinely in North American hospitals, despite a lack of evidence of benefit. The perception that structured intermittent auscultation increases medicolegal risk, the lack of hospital staff trained in structured intermittent auscultation, and the economic benefit of continuous EFM from decreased use of nursing staff may promote the use of continuous EFM.8 Online Table A lists considerations in developing an institutional strategy for fetal surveillance.
Online Table A. Considerations for Developing an Institutional Fetal Surveillance Strategy
| Determine staff availability and level of comfort Assess personnel available on the labor floor Train nurses on fetal surveillance techniques and institutional protocols Periodically update skills and knowledge Provide patients with the same level of care, regardless of fetal monitoring technique Discuss monitoring technique with the patient Completely inform patients of the evidence regarding fetal surveillanceInitiate discussion during prenatal visit before labor starts Obtain patient preferences and communicate physician concerns clearly Determine risk of mother and fetus Know the indications for continuous electronic fetal monitoring based on risk factors listed in Table 2 Update risk factors regularly before and during labor Establish institutional protocols for clear lines of communication about when to change monitoring technique based on change in risk |
Information from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Interpretation of FHR Tracings
A concern with continuous EFM is the lack of standardization in the FHR tracing interpretation.5,8–11 Studies demonstrate poor inter-rater reliability of experts, even in controlled research settings.12,13 A National Institute of Child Health and Human Development (NICHD) research planning workshop was convened in 1997 to standardize definitions for interpretation of EFM tracing.14 These definitions were adopted by the American College of Obstetricians and Gynecologists (ACOG) in 2002,5 and revisions were made in a 2008 workshop sponsored by NICHD, ACOG, and the Society for Maternal-Fetal Medicine.11 The Advanced Life Support in Obstetrics (ALSO) curriculum developed the mnemonic DR C BRAVADO (Table 3) to teach a systematic, structured approach to continuous EFM interpretation that incorporates the NICHD definitions.9,11
Table 3. DR C BRAVADO Mnemonic for Interpretation of Continuous Electronic Fetal Monitoring
| Mnemonic parts | Notes |
|---|---|
| DR: Determine risk | High, medium, or low risk (i.e., risk in terms of the clinical situation) |
| C: Contractions | Rate, rhythm, frequency, duration, intensity, and resting tone |
| BRA: Baseline rate | Bradycardia (< 110 bpm), normal (110 to 160 bpm), or tachycardia (> 160 bpm); rising baseline |
| V: Variability | Reflects central nervous system activity: absent, minimal, moderate, or marked |
| A: Accelerations | Spontaneous; stimulated; none |
| Rises from the baseline of ≥ 15 bpm, lasting ≥ 15 seconds | |
| Preterm: ≥ 10 bpm, lasting ≥ 10 seconds | |
| D: Decelerations | Absent, early, variable, late, or prolonged |
| O: Overall assessment and written plan | Stoplight algorithm (Figure 1) or National Institute of Child Health and Human Development categorization11 |
| Assessment includes implementing an appropriate management plan |
bpm = beats per minute.
DR C BRAVADO
Determine Risk (DR). The clinical risk status (low, medium, or high) of each fetus is assessed in conjunction with the interpretation of the continuous EFM tracing. A term, low-risk baby may have higher reserves than a fetus that is preterm, growth restricted, or exposed to uteroplacental insufficiency because of preeclampsia. An increase in risk status during labor, such as the diagnosis of chorioamnionitis, may necessitate a change in monitoring from structured intermittent auscultation to continuous EFM.
Contractions (C). It is important to review the pressure tracing before assessing the fetal tracing to accurately interpret decelerations. The electronic fetal monitor uses an external pressure transducer or an intrauterine pressure catheter (IUPC) to measure amplitude and frequency of contractions. However, the strength of contractions cannot always be accurately assessed from an external transducer and should be determined with an IUPC, if necessary. Contractions are classified as normal (no more than five contractions in a 10-minute period) or tachysystole (more than five contractions in a 10-minute period, averaged over a 30-minute window).11 Tachysystole is qualified by the presence or absence of decelerations, and it applies to spontaneous and stimulated labor. The term “hyperstimulation” is no longer accepted, and this terminology should be abandoned.11
Baseline Rate (BRA; Online Table B). The normal range for baseline FHR is defined by NICHD as 110 to 160 beats per minute (bpm; Online Figure A). A change in baseline FHR is said to occur when the change persists for 10 minutes or longer. A baseline of less than 110 bpm is defined as bradycardia.11 Mild bradycardia (100 to 110 bpm) is associated with post-term infants and occipitoposterior position.15 Rates of less than 100 bpm may be seen in fetuses with congenital heart disease or myocardial conduction defects.15 A baseline greater than 160 bpm is defined as tachycardia11 (Online Figure B). This is associated with certain maternal and fetal conditions, such as chorioamnionitis, fever, dehydration, and tachyarrhythmias.
Online Table B. Fetal Heart Rate Characteristics
| Characteristic | Definition | |
|---|---|---|
| Accelerations | Visually apparent, abrupt (onset to peak < 30 seconds) increase in FHR from the most recently calculated baseline | |
| Peak ≥ 15 bpm above baseline, duration ≥ 15 seconds, but < 2 minutes from onset to return to baseline; before 32 weeks’ gestation: peak ≥ 10 bpm above baseline, duration ≥ 10 seconds | ||
| Baseline FHR | Approximate mean FHR rounded to increments of 5 bpm during a 10-minute segment, excluding periodic or episodic changes, periods of marked variability, and segments of baseline that differ by > 25 bpm | |
| In any 10-minute window, the minimum baseline duration must be ≥ 2 minutes, or the baseline for that period is indeterminate (refer to the previous 10-minute segment for determination of baseline) | ||
| Bradycardia | Baseline rate: < 110 bpm | |
| Decelerations | ||
| Early | The nadir of the deceleration occurs at the same time as the peak of the contraction | |
| Late | The nadir of the deceleration occurs after the peak of the contraction | |
| Variable | Abrupt decrease in FHR; if the nadir of the deceleration is ≥ 30 seconds, it cannot be considered a variable deceleration | |
| Tachycardia | Baseline rate: > 160 bpm | |
| Variability | ||
| Absent | Amplitude range: undetectable | |
| Minimal | Amplitude range: detectable, but ≤ 5 bpm | |
| Moderate | Amplitude range: 6 to 25 bpm | |
| Marked | Amplitude range: > 25 bpm | |
bpm = beats per minute; FHR = fetal heart rate.
Information from Macones GA, Hankins GD, Spong CY, Hauth J, Moore T. The 2008 National Institute of Child Health and Human Development workshop report on electronic fetal monitoring: update on definitions, interpretation, and research guidelines. Obstet Gynecol. 2008;112(3):661-666.
Online Figure A.
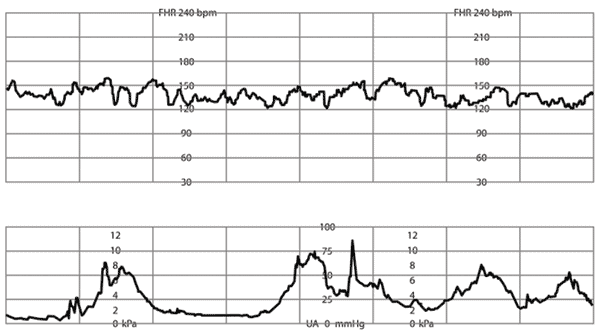
Normal baseline fetal heart rate (FHR), shown at 135 beats per minute (bpm). Normal baseline rate ranges from 110 to 160 bpm for a 10-minute segment and duration ≥ 2 minutes. Excludes periodic and episodic changes, marked variability, and segments differing by ≥ 25 bpm.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Online Figure B.
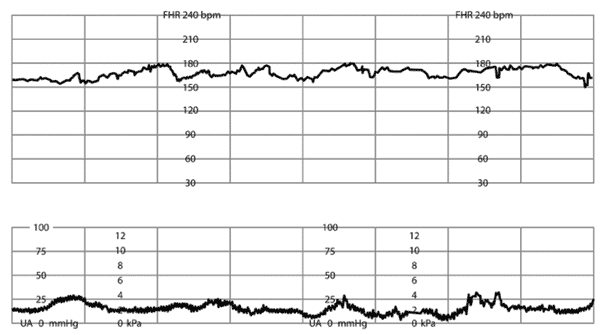
Tachycardia of fetal heart rate (FHR), shown at 170 beats per minute (bpm). Baseline rate with tachycardia is > 160 bpm.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Variability (V; Online Table B). The FHR normally exhibits variability, with an average change of 6 to 25 bpm of the baseline rate, and is linked to the fetal central nervous system. Therefore, it is a vital clue in determining the overall fetal condition. Detection is most accurate with a direct fetal scalp electrode, although newer external transducers have improved the ability to detect variability. The NICHD has stated that it is no longer useful to distinguish between short-term and long-term variability and has categorized variability into the following classifications, depending on the amplitude of the FHR tracing: absent (Online Figure C), minimal (Online Figure D), moderate (Online Figure E), and marked (Online Figure F).11
Online Figure C.
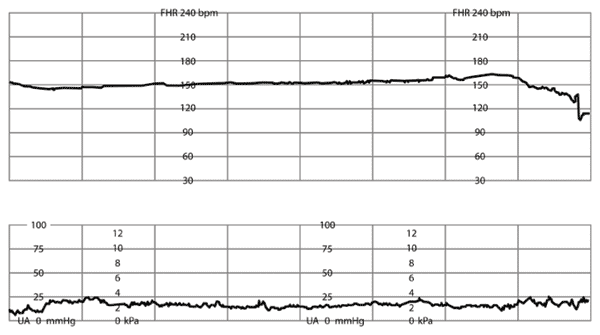
Minimal variability of fetal heart rate (FHR). Amplitude range of FHR tracing is undetectable.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Online Figure D.
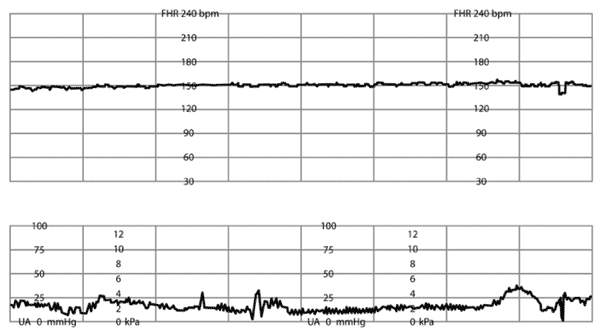
Minimal variability of fetal heart rate (FHR). Amplitude range of FHR tracing ≤ 5 beats per minute.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Online Figure E.
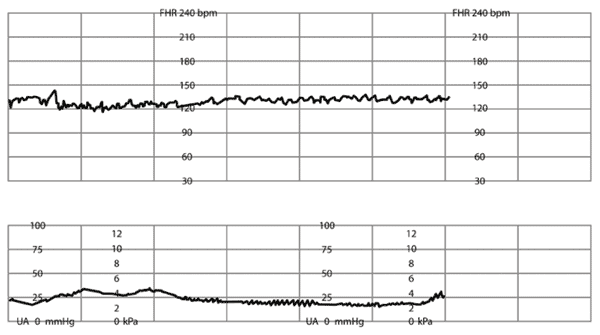
Moderate variability of fetal heart rate (FHR). Amplitude range of FHR tracing is 6 to 25 beats per minute.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Online Figure F.
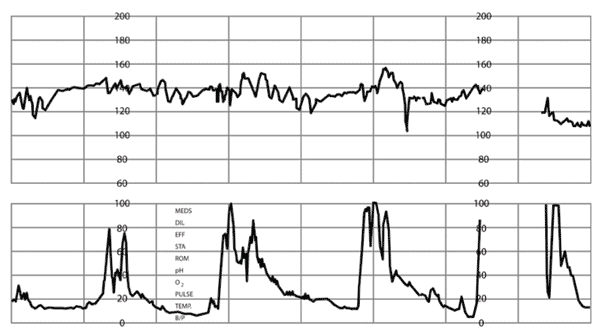
Marked variability of fetal heart rate (FHR). Amplitude range of FHR tracing > 25 beats per minute.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Sleep cycles of 20 to 40 minutes or longer may cause a normal decrease in FHR variability, as can certain medications, including analgesics, anesthetics, barbiturates, and magnesium sulfate.15 Loss of variability, accompanied by late or variable decelerations, increases the possibility of fetal acidosis if uncorrected.15
Sinusoidal pattern is a smooth, undulating sine wave pattern defined by an amplitude of 10 bpm with three to five cycles per minute, lasting at least 20 minutes.11 This uncommon pattern is associated with severe fetal anemia and hydrops, and it usually requires rapid intervention in these settings.15 Similar appearing benign tracings occasionally occur because of “fetal thumb sucking” or maternal narcotic administration, and generally these will persist for less than 10 minutes.15
Accelerations (A). Abrupt increases in the FHR are associated with fetal movement or stimulation and are indicative of fetal well-being11 (Online Table B, Online Figure G).
Online Figure G.
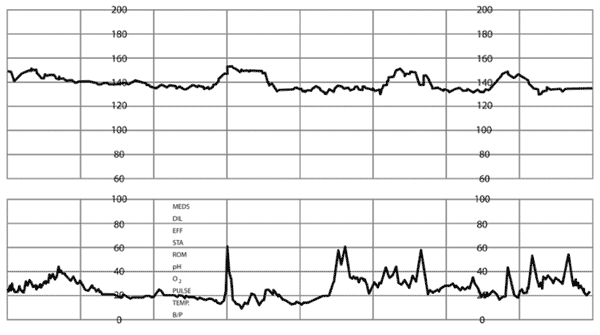
Acceleration of fetal heart rate (FHR). Visually apparent, abrupt (onset to peak < 30 seconds) increase in FHR from the most recently calculated baseline. Peak ≥ 15 beats per minute (bpm) above the baseline, and duration ≥ 15 seconds, but < 2 minutes from onset of the acceleration to return to baseline. Before 32 weeks’ gestation, peak ≥ 10 bpm above baseline, duration ≥ 10 seconds.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Decelerations (D). Periodic changes in FHR, as they relate to uterine contractions, are decelerations that are classified as recurrent if they occur with 50 percent or more of contractions in a 20-minute period, and intermittent if they occur with less than 50 percent of contractions.11 The decrease in FHR is calculated from the onset to the nadir of the deceleration. A gradual decrease is defined as at least 30 seconds from the onset of the deceleration to the FHR nadir, whereas an abrupt decrease is defined as less than 30 seconds from the onset of the deceleration to the beginning of the FHR nadir.11
Early decelerations (Online Figure H) are transient, gradual decreases in FHR that are visually apparent and usually symmetric.11 They occur with and mirror the uterine contraction and seldom go below 100 bpm.11 The nadir of the deceleration occurs at the same time as the peak of the contraction. The onset, nadir, and recovery of the deceleration usually coincide with the beginning, peak, and ending of the contraction, respectively.11 Early decelerations are nearly always benign and probably indicate head compression, which is a normal part of labor.15
Online Figure H.
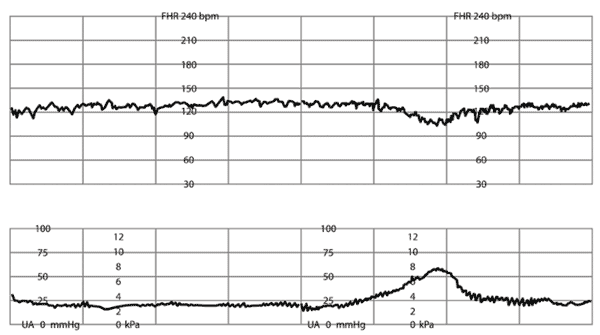
Early deceleration of fetal heart rate (FHR). Gradual decrease and return of FHR is associated with a uterine contraction. In most cases, the onset of the deceleration, nadir, and recovery coincide with the beginning, peak, and ending of the contraction, respectively (FHR mirrors the contraction).
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Variable decelerations (Online Figure I), as the name implies, vary in terms of shape, depth, and timing in relationship to uterine contractions, but they are visually apparent, abrupt decreases in FHR.11 The decrease in FHR is at least 15 bpm and has a duration of at least 15 seconds to less than two minutes.11 Characteristics of variable decelerations include rapid descent and recovery, good baseline variability, and accelerations at the onset and at the end of the contraction (i.e., “shoulders”).11 When they are associated with uterine contractions, their onset, depth, and duration commonly vary with successive uterine contractions.11 Overall, variable decelerations are usually benign, and their physiologic basis is usually related to cord compression, with subsequent changes in peripheral vascular resistance or oxygenation.15 They occur especially in the second stage of labor, when cord compression is most common.15 Atypical variable decelerations may indicate fetal hypoxemia, with characteristic features that include late onset (in relation to contractions), loss of shoulders, and slow recovery.15
Online Figure I.
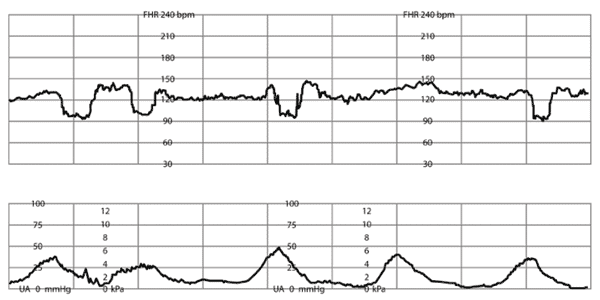
Variable deceleration of fetal heart rate (FHR). Abrupt decrease in FHR < 30 seconds from the beginning of the deceleration to the nadir. The decrease in FHR (measured at the nadir) is ≥ 15 beats per minute, with a duration ≥ 15 seconds, but < 2 minutes.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Late decelerations (Online Figure J) are visually apparent, usually symmetric, and have the characteristic feature of onset of the deceleration after the onset of the uterine contraction.11 The timing of the deceleration is delayed, with the nadir of the deceleration occurring after the peak of the contraction.11 The onset, nadir, and recovery of the deceleration usually occur after the beginning, peak, and ending of the contraction, respectively. The physiology behind late deceleration is uteroplacental insufficiency.16,17 Transient late deceleration patterns may be seen with maternal hypotension or uterine hyperstimulation. Subtle, shallow late decelerations can be difficult to visualize, but can be detected by holding a straight edge along the baseline.
Online Figure J.
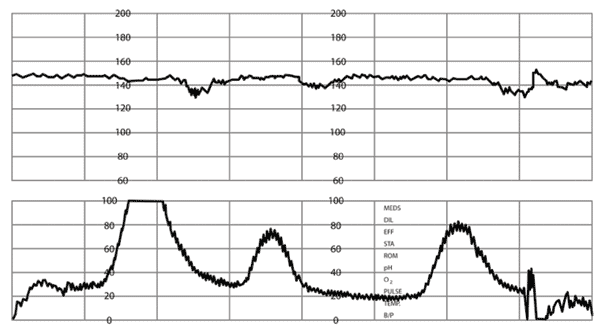
Repetitive late deceleration of fetal heart rate (FHR). National Institute of Child Health and Human Development Category II: repetitive late deceleration with minimal variability.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Prolonged decelerations (Online Figures K and L) last longer than two minutes, but less than 10 minutes.11 They may be caused by a number of factors, including head compression (rapid fetal descent), cord compression, or uteroplacental insufficiency. Management depends on the clinical picture and presence of other FHR characteristics.18
Online Figure K.
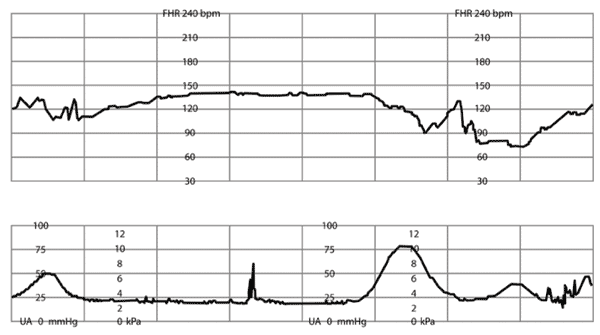
Prolonged deceleration of fetal heart rate (FHR) with slow recovery. National Institute of Child Health and Human Development Category II: prolonged deceleration ≥ 2 minutes and < 10 minutes.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Online Figure L.
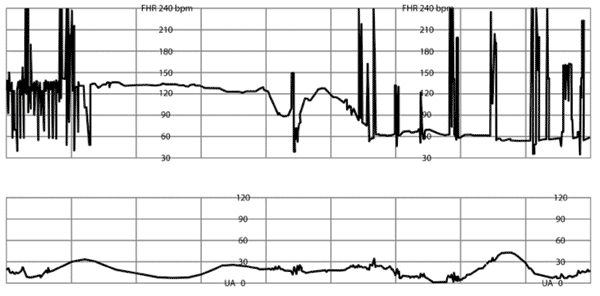
Prolonged deceleration of fetal heart rate (FHR) without recovery. National Institute of Child Health and Human Development Category III: absent variability and bradycardia.
Online Figures A through L adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Overall Assessment (O). The recommendations for the overall management of FHR tracings by NICHD, the International Federation of Gynecology and Obstetrics, and ACOG agree that interpretation is reproducible at the extreme ends of the fetal monitor strip spectrum.10 For example, the presence of a normal baseline rate with FHR accelerations or moderate variability predicts the absence of fetal acidemia.10,11 Bradycardia, absence of variability and accelerations, and presence of recurrent late or variable decelerations may predict current or impending fetal asphyxia.10,11 However, more than 50 percent of fetal strips fall between these two extremes, in which overall recommendations cannot be made reliably.10 In the 2008 revision of the NICHD tracing definitions, a three-category system was adopted: normal (category I), indeterminate (category II), and abnormal (category III).11 Category III tracings need intervention to resolve the abnormal tracing or to move toward expeditious delivery.11 In the ALSO course, using the DR C BRAVADO approach, the FHR tracing may be classified using the “stoplight” algorithm (Figure 19), which corresponds to the NICHD categories.9,11 Interventions are determined by placing the FHR tracing in the context of the specific clinical situation and corresponding NICHD category, fetal reserve, and imminence of delivery (Table 4).9,11
Figure 1. Continuous Electronic Fetal Monitoring Stoplight

Stoplight algorithm for intrapartum surveillance of fetal heat rate (FHR). (NICHD = National Institute of Child Health and Human Development.)
*— See Table 4 for further information on the management of continuous electronic fetal monitoring findings by NICHD category.
†— General measures include vaginal examination, checking maternal vital signs, giving oxygen, changing maternal position, administering intravenous fluids, and assessing fetal pH with acoustic or fetal scalp stimulation.
Adapted from Bailey RE. Intrapartum fetal surveillance. In: Leeman L, ed. Advanced Life Support in Obstetrics Program: Provider Course Syllabus. Leawood, Kan.: American Academy of Family Physicians; 2009.
Table 4. Interpretation and Management of Continuous EFM Findings
| Continuous EFM findings | Significance | Management |
|---|---|---|
| NICHD Category I: Normal | ||
| Moderate baseline FHR variability, late or variable decelerations absent, accelerations present or absent, and normal baseline FHR (110 to 160 bpm) | Normal pH and fetal well-being | Continue current monitoring method (SIA or continuous EFM) |
| NICHD Category II: Indeterminate* | ||
| Baseline FHR changes (bradycardia [< 110 bpm] not accompanied by absent baseline variability, or tachycardia [> 160 bpm]) | Tachycardia: medication, maternal anxiety, infection, fever | General measures† |
| Bradycardia: rupture of membranes, occipitoposterior position, post-term pregnancy, congenital anomalies | Consider expedited delivery if abnormalities persist‡ | |
| Change in FHR variability (absent and not accompanied by decelerations; minimal; or marked) | Medications; sleep cycle; change in monitoring technique; possible fetal hypoxia or acidemia | General measures† |
| Change monitoring method (internal monitoring if doing continuous EFM, or EFM if doing SIA) | ||
| Consider expedited delivery if abnormalities persist‡ | ||
| No FHR accelerations after fetal stimulation | Possible fetal hypoxia or acidemia | General measures† Discontinue oxytocin (Pitocin) Consider expedited delivery if abnormalities persist‡ |
| FHR decelerations without absent variability | Variable: cord entrapment or prolapse | General measures† Amnioinfusion (for recurrent decelerations) |
| Late: possible uteroplacental insufficiency; epidural hypotension; tachysystole | General measures† Discontinue oxytocin Consider expedited delivery if abnormalities persist‡ | |
| NICHD Category III: Abnormal | ||
| Absent baseline FHR variability with recurrent decelerations (variable or late) and/or bradycardia | Uteroplacental insufficiency; fetal hypoxia or acidemia | General measures† |
| Sinusoidal FHR pattern | Discontinue oxytocin | |
| Expedite delivery ‡ | ||
bpm = beats per minute; EFM = electronic fetal monitoring; FHR = fetal heart rate; NICHD = National Institute of Child Health and Human Development; SIA = structured intermittent auscultation.
*— Category II FHR tracings may represent an appreciable fraction of those encountered in clinical care, and include all FHR tracings not categorized as category I or III.
†— General measures include vaginal examination, checking maternal vital signs, giving oxygen, changing maternal position, administering intravenous fluids, and assessing fetal pH with acoustic or fetal scalp stimulation.
‡— Expedite with operative vaginal or cesarean delivery.
If the FHR tracing is normal, structured intermittent auscultation or continuous EFM techniques can be employed in a low-risk patient, although reconsideration may be necessary as labor progresses.2 If the FHR tracing is abnormal, interventions such as position changes, maternal oxygenation, and intravenous fluid administration may be used. When continuous EFM tracing is indeterminate, fetal scalp pH sampling or fetal stimulation may be used to assess for the possible presence of fetal acidemia.5 Fetal scalp pH testing is no longer commonly performed in the United States and has been replaced with fetal stimulation or immediate delivery (by operative vaginal delivery or cesarean delivery). A meta-analysis showed that if there is absent or minimal variability without spontaneous accelerations, the presence of an acceleration after scalp stimulation or fetal acoustic stimulation indicates that the fetal pH is at least 7.20.19
If the FHR tracing remains abnormal, these tests may need to be performed periodically, and consideration of emergent cesarean or operative vaginal delivery is usually recommended.15 Measurements of cord blood gases are generally recommended after any delivery for abnormal FHR tracing because evidence of metabolic acidosis (cord pH less than 7.00 or base deficit greater than 12 mmol per L) is one of the four essential criteria for determining an acute intrapartum hypoxic event sufficient to cause cerebral palsy.20
When using continuous EFM, tracings should be reviewed by physicians and labor and delivery nurses on a regular basis during labor. The periodic review includes ensuring that a good quality tracing is present and that abnormalities are appropriately communicated. Adequate documentation is necessary, and many institutions are now employing flow sheets (e.g., partograms), clinical pathways, or FHR tracing archival processes (in electronic records). Any written information on the tracing (e.g., emergent situations during labor) should coincide with these automated processes to minimize litigation risk.21
Intrauterine Resuscitation
Table 5 lists intrauterine resuscitation interventions for abnormal EFM tracings.9 Management will depend on assessment of the risk of hypoxia and the ability to effect a rapid delivery, when necessary. If delivery is imminent, even severe decelerations are less significant than in the earlier stages of labor. The use of amnioinfusion for recurrent deep variable decelerations demonstrated reductions in decelerations and cesarean delivery overall. Additionally, an Apgar score of less than 7 at five minutes, low cord arterial pH (less than 7.20), and neonatal and maternal hospital stays greater than three days were reduced.22
Table 5. Interventions for Abnormal Electronic Fetal Monitoring
| 1. Change maternal position |
| 2. Assess maternal vital signs (temperature, blood pressure, pulse) |
| 3. Discontinue oxytocin (Pitocin) infusion, if in use |
| 4. Initiate oxygen at 6 to 10 L per minute |
| 5. Perform a vaginal examination (check for cord prolapse, rapid descent of the head, or vaginal bleeding suggestive of placental abruption) |
| 6. Give intravenous fluids if not already administered; consider bolus |
| 7. Assess fetal pH (fetal scalp stimulation, scalp pH, or acoustic stimulation) |
| 8. Give amnioinfusion for recurrent, moderate to severe variable decelerations |
| 9. Consider need for expedited delivery (operative vaginal delivery or cesarean delivery) |
Information from reference 9.
Tocolytic agents such as terbutaline (formerly Brethine) may be used to transiently stop contractions, with the understanding that administration of these agents improved FHR tracings compared with untreated control groups, but there were no improvements in neonatal outcomes.23 A recent study showed a significant effect of maternal oxygen on increasing fetal oxygen in abnormal FHR patterns.24
Areas for Future Development
Although continuous EFM remains the preferred method for fetal monitoring, the following methodologies are active areas of research in enhancing continuous EFM or developing newer methodologies for fetal well-being during labor.
Fetal hypoxemia results in biphasic changes in the ST segment of the fetal electrocardiography (FECG) waveform and an increase in the T:QRS ratio.15 The ST-segment automated analysis (STAN) software from Noventa Medical can record the frequency of ST events and, combined with changes in continuous EFM, can be used to determine if intervention during the labor process is indicated.15 Several studies have evaluated FECG analysis, documenting its effectiveness at reducing operative vaginal deliveries, fetal scalp sampling, neonatal encephalopathy, and fetal acidosis (pH < 7.05).25–28 One drawback to this technology is that it requires rupture of the membranes and internal fetal scalp monitoring.
Another area of interest is the use of computer analysis for key components of the fetal tracing,29 or decision analysis for the interpretation of the EFM tracing.30 These have not been demonstrated to improve clinical outcomes.29,30 Fetal pulse oximetry was developed to continuously monitor fetal oxygenation during labor by using an internal monitor, requiring rupture of membranes.31 Trials have not demonstrated a reduction in cesarean delivery rates or interventions with the use of fetal pulse oximetry.31

